Abstract
The endothelial nitric oxide (NO) system may be damaged in preeclampsia; however, the involved mechanisms are unclear. In this study, we used primary human umbilical vein endothelial cells (HUVECs) to evaluate the endothelial NO system in preeclampsia and to determine the underlying mechanisms that are involved. We isolated and cultured HUVECs from normal and preeclamptic pregnancies and evaluated endothelial NO synthase enzyme (eNOS) expression and NO production. Whole-cell K+ currents and oxidative stress were also determined in normal and preeclamptic HUVECs. Compared with normal HUVECs, eNOS expression, NO production and whole-cell K+ currents in preeclamptic HUVECs were markedly decreased, whereas oxidative stress was significantly increased. The decreased K+ currents were associated with damaged Ca2+-activated K+ (KCa) channels, especially the large (BKCa) and small (SKCa) conductance KCa channels, and were involved in the downregulated eNOS expression in preeclamptic HUVECs. Moreover, the increased oxidative stress detected in preeclamptic HUVECs was mediated by NADPH (nicotinamide adenine dinucleotide phosphate) oxidase 2 (NOX2)-dependent reactive oxygen species overproduction that could downregulate whole-cell K+ currents, eNOS expression and NO production. Taken together, our study indicated that the increased oxidative stress in preeclamptic HUVECs could downregulate the NO system by suppressing BKCa and SKCa channels. Because the damaged NO system was closely related to endothelial dysfunction, this study provides important information to further understand the pathological process of endothelial cell dysfunction in preeclampsia.
Similar content being viewed by others
Introduction
Preeclampsia is a disorder of pregnancy characterized by hypertension and a large amount of protein in the urine, resulting in maternal mortality and prenatal deaths, preterm births and intrauterine growth restriction.1 The pathogenetic mechanism implicated in preeclampsia is unclear, but there is a consensus that endothelial dysfunction plays an important role in the pathogenesis of preeclampsia.2, 3, 4 Endothelial dysfunction can be broadly defined as an imbalance between vasodilator and vasoconstrictor substances produced from the endothelium.4, 5 Among many endothelium-derived vasoactive factors, nitric oxide (NO) is a critical vessel-relaxing molecule.6 As the key synthesis enzymes of NO, endothelial nitric oxide synthase enzyme (eNOS) is the focus of endothelial dysfunction in preeclampsia.7, 8, 9, 10, 11 Recent studies have shown that eNOS levels are significantly decreased in both preeclamptic maternal blood9 and placenta,10 indicating the NO system is damaged in preeclampsia.
Notably, the changes in membrane potential regulated by potassium channels have been proposed to be involved in regulating the release of endothelium-derived vasoactive factors.12, 13, 14, 15 Endothelial cells express several distinct types of potassium channels: Ca2+-activated K+ (KCa) channels (including large (BKCa), intermediate (IKCa) and small (SKCa) conductance KCa subfamilies), inward rectifier K+ channels and ATP-sensitive K+ channels.12 Among them, KCa channels play an important role in modulating the endothelial NO system.13, 14, 15 The simultaneous blockade of IKCa and SKCa channels not only abolishes membrane hyperpolarization but also attenuates NO production in endothelial cells from conduit vessels such as the human umbilical vein.15 The activities of KCa channels were considered to be regulated by the oxidative stress induced by reactive oxygen species (ROS) in vascular smooth muscle and endothelial cells.16, 17, 18, 19, 20 Oxidative stress could impair IKCa and SKCa channels in mesenteric arteries in diabetic rats.16 ROS also inhibited BKCa channels in porcine renal artery endothelium17 and impaired BKCa channel functions by altering cysteine-mediated calcium sensing.20 In hypertensive patients and rodents, oxidative stress was demonstrated to be increased, and the balance of oxidative status seems to be disrupted.21, 22, 23 Previous studies have shown that the increased oxidative stress detected in preeclampsia was involved in regulating endothelial KCa channels24 and was related to modulating endothelial vasoactive factors.25, 26, 27
In light of these findings, both KCa channels and oxidative stress could regulate endothelial NO levels. In addition, ROS were suggested to be an important regulator of KCa channels in various tissues, whereas altered oxidative stress and the NO system were confirmed in preeclampsia. An interesting question was then raised: is there any link among oxidative stress, KCa channels and NO system in endothelial cells? This study hypothesized that increased oxidative stress in preeclampsia may affect endothelial KCa channels and eventually damage the NO system.
Materials and methods
Sample collection
Written consent was obtained from all participants. Umbilical cords were from normal (NP, N=43) and preeclamptic pregnancies (PE, N=32) at local hospitals in Suzhou, China. All procedures of the study were approved by the Ethics and Research Committee of the participating hospital. Healthy pregnant participants were defined as those with a blood pressure <140/90 mm Hg and no clinically significant complications. Preeclamptic pregnant participants were defined as those with a blood pressure >140/90 mm Hg and significant proteinuria after 20 weeks of pregnancy.28 The clinical characteristics of all participants are summarized in Table 1.
Endothelial cell isolation and culture
Umbilical cords (∼20 cm in length) were excised from the placenta immediately after delivery and were placed into cold sterile phosphate-buffered saline. All preparations were performed under sterile conditions in a laminar airflow bench. Endothelial cells were isolated from umbilical veins as described previously29 and then cultured in M199 (Sigma-Aldrich, St Louis, MO, USA) containing 1% endothelial cell growth factor supplement and 20% fetal bovine serum at 37 °C with 5% CO2 and 95% air humidified incubator.
Real-time PCR and western blotting
Total RNA from human umbilical vein endothelial cells (HUVECs) was isolated using Trizol reagent (Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s protocol and was then reversed transcribed using the first-strand cDNA Synthesis Kit (Toyobo (Shanghai) Biotech, Shanghai, China). Real-time quantitative PCR was performed using the SYBR Green Supermix Taq Kit (Takara Biotechnology Co., Ltd., Dalian, China) and was analyzed using the Real-Time PCR Detection System (Bio-Rad Laboratories, Inc., Hercules, CA, USA). The primer sequences are listed in Table 2. Whole-cell proteins were separated by sodium dodecyl sulfate–polyacrylamide gel electrophoresis and were immunoblotted with primary antibodies against eNOS (rabbit polyclonal, 1:200 dilution), SK3 (rabbit polyclonal, 1:200 dilution), KCNMA1 (rabbit polyclonal, 1:200 dilution), KCNMB1 (mouse monoclonal, 1:500 dilution) or NOX2 (mouse monoclonal, 1:1000 dilution) followed by incubation with the appropriate secondary antibodies. All antibodies were purchased from Santa Cruz Biotechnology, Inc. (Santa Cruz, CA, USA). All experiments were repeated three times with independently prepared tissue lysates. Real-time quantitative PCR and western blot analyses were performed as previously described.30
Measurement of NO production and superoxide generation
In cells, NO is transient and volatile, making it unsuitable for most convenient detection methods. Two end products of NO, nitrite and nitrate, can be easily detected by photometric means. NO production in cultured HUVECs was determined using the Nitrate/Nitrite Assay Kit (Beyotime Biotechnology, Nantong, China). Superoxide (O2−) is one of the major ROS. Superoxide production by HUVECs was detected by staining with fluorescently labeled dihydroethidium (Sigma-Aldrich). In the presence of O2−, dihydroethidium reacts with O2− to form fluorescent ethidium that intercalates with DNA and produces fluorescence. The cultured adherent HUVECs (usually 6 to 7 days after isolation from umbilical cords) were incubated with dihydroethidium (20 μM) in a light-protected humidified chamber at 37 °C for 60 min, and then the cells were washed three times with phosphate-buffered saline and fixed with 4% paraformaldehyde for 10 min. Images were acquired with a microscope system, and superoxide generation was quantitatively calculated using Image-Pro Plus 6.0 (Media Cybernetics, Rockville, MD, USA).
Electrophysiological measurements
Whole-cell K+ currents were recorded on single endothelial cells using the whole-cell patch-clamp technique.29 The adherent primary HUVECs (cultured 6–7 days after isolation from umbilical cords) were washed three times with phosphate-buffered saline and were then digested with 0.25% trypsin. Whole-cell K+ currents were measured on single endothelial cells using an Axon Multiclamp 700B (Axon Instruments, Foster City, CA, USA) with Clampex 10.1 as previously described.29, 31 Before cell K+ currents were monitored, HUVECs were cultured with iberiotoxin (IBTX, a selective BKCa blocker, 10−7 mol l−1), apamin (a selective SKCa blocker, 10−6 mol l−1) or apocynin (a NADPH oxidase inhibitor, 10−7 mol l−1) as previously described.31, 32, 33 All patch-clamp experiments were carried out at 22°C. The drugs were from Sigma-Aldrich.
Data analysis and statistics
The data were analyzed with GraphPad Prism 5 software (GraphPad Software, La Jolla, CA, USA) and were expressed as means±s.e.m. Statistical analysis was performed with t-test or two-way analysis of variance followed by Bonferroni’s test. Curve fitting was also performed with GraphPad Software. Differences were only considered statistically significant at P<0.05.
Results
eNOS expression and NO production
Compared with the NP group, NO production was decreased in preeclamptic HUVECs (11.56±4.845 vs. 5.89±3.338 μmol l−1, NP vs. PE, P<0.05; Figure 1a). The mRNA and protein levels of eNOS were also significantly downregulated in preeclamptic HUVECs (Figures 1b and c).
eNOS expression and NO production in normal and preeclamptic HUVECs. (a) NO production in HUVECs (N=15 for NP; N=15 for PE). (b, c) mRNA and protein levels of eNOS in HUVECs (N=28 for NP; N=27 for PE). eNOS, endothelial nitric oxide synthase enzyme; HUVEC, human umbilical vein endothelial cell; N, number of participants; NO, nitric oxide; NP, normal pregnancy; PE, preeclampsia. Error bars denote s.e.m. *P<0.05.
Whole-cell K+ currents in HUVECs
Because potassium channels were related to eNOS expression and NO production,14, 15 we determined whole-cell K+ currents in HUVECs. The whole-cell K+ currents of HUVECs in the PE group were significantly lower than those in the NP group (NP vs. PE: 12.28±1.25 vs. 5.45±0.51 pA pF−1; TP=+60 mV, P<0.05; Figures 2a and b). To determine whether BKCa or SKCa channels were involved in the decreasing whole-cell K+ currents in preeclamptic HUVECs, HUVECs were cultured with IBTX (a selective BKCa blocker) and/or apamin (a selective SKCa blocker). Whole-cell K+ currents in normal HUVECs were significantly decreased by blocking BKCa (from 12.08±1.16 pA pF−1 at baseline to 7.24±0.80 pA pF−1, TP=+60 mV, P<0.05; Figure 2c) or SKCa (from 12.16±1.22 pA pF−1 at baseline to 8.65±0.72 pA pF−1, TP=+60 mV, P<0.05; Figure 2d), whereas there were no significant changes in preeclamptic HUVECs (P>0.05; Figures 2c and d). Simultaneous blockade of BKCa and SKCa showed a further inhibitory effect on the whole-cell K+ current (NP: from 12.26±1.21 pA pF−1 at baseline to 4.34±0.48 pA pF−1, TP=+60 mV, P<0.05; PE: from 5.36±0.61 pA pF−1 at baseline to 3.64±0.42 pA pF−1, TP=+60 mV, P<0.05; Figure 2e).
Whole-cell K+ currents in normal and preeclamptic HUVECs. (a) Representative images of whole-cell K+ currents in HUVECs. (b) Current density in normal and preeclamptic HUVECs. N=23, n=48 for NP; N=24, n=52 for PE. (c–e) The effect of BKCa and/or SKCa blocker on whole-cell K+ currents in normal and preeclamptic HUVECs. N=20, n=41 for NP; N=21, n=38 for PE. Apamin, a selective SKCa blocker; HUVEC, human umbilical vein endothelial cell; IBTX, a selective BKCa blocker; N, number of participants; n, number of cells; NP, normal pregnancy; PE, preeclampsia. Error bars denote s.e.m. *P<0.05; **P<0.01; #P>0.05.
Expression of KCa channel subunit genes
KCa channels are divided into the BKCa, IKCa and SKCa conductance KCa subfamily that respectively include KCNMA1, KCNMB1 (KCa1.1 and BKβ1), SK4 (KCa3.1) and SK1, SK2, SK3 (KCa2.1, KCa2.2 and KCa2.3) subunits.18 As shown in Figures 3a–d, the mRNA and protein levels of KCNMB1 and SK3 were significantly lower in preeclamptic HUVECs than in the NP group, whereas there were no significant differences in the expression of KCNMA1, SK1, SK2 and SK4 between normal and preeclamptic HUVECs.
The expression of KCa channel subunit genes in normal and preeclamptic HUVECs. (a, c) mRNA and protein levels of KCNMA1 and KCNMB1 in HUVECs (N=19 for NP; N=20 for PE). (b) mRNA levels of SK1, SK2, SK3 and SK4 in HUVECs (N=19 for NP; N=20 for PE). (d) Protein levels of SK3 in HUVECs (N=3 for NP; N=3 for PE). Error bars denote s.e.m. *P<0.05; **P<0.01. HUVEC, human umbilical vein endothelial cell; N, number of participants; NP, normal pregnancy; PE, preeclampsia.
Effect of BKCa and/or SKCa blocker on eNOS expression
To determine whether the decreased BKCa and SKCa was associated with downregulated eNOS expression, HUVECs were cultured with IBTX and/or apamin. As shown in Figures 4a and b, eNOS expression was downregulated by blocking BKCa and SKCa in normal HUVECs, whereas no significant differences were noted in preeclamptic HUVECs, suggesting that the downregulated eNOS expression observed in preeclamptic HUVECs was linked to damaged BKCa and SKCa.
Superoxide production and NADPH oxidase (NOX) expression
Superoxide is the main component of ROS, and hence we measured superoxide production in HUVECs with superoxide-mediated dihydroethidium fluorescence. Figures 5a and b showed that superoxide production was significantly increased in preeclamptic HUVECs compared with that in the NP group. Moreover, the expression of the NOX catalytic subunit NOX2, but not NOX1 and NOX4, was significantly upregulated in preeclamptic HUVECs (Figures 5c and d).
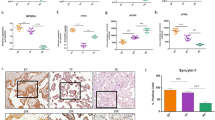
Superoxide production and NOX expression in normal and preeclamptic HUVECs. (a, b) Fluorescence microscopic images and fluorescence intensity of cultured HUVECs after incubation with DHE for 60 min. (c) mRNA levels of NOX1, NOX2 and NOX4 in HUVECs (N=25 for NP; N=24 for PE). (d) Protein levels of NOX2 in HUVECs (N=3 for NP; N=3 for PE). Error bars denote s.e.m. **P<0.01. DHE, dihydroethidium; HUVEC, human umbilical vein endothelial cell; N, number of participants; NOX, NADPH (nicotinamide adenine dinucleotide phosphate) oxidase; NP, normal pregnancy; PE, preeclampsia. A full color version of this figure is available at the Hypertension Research journal online.
Effect of a NOX inhibitor on K+ currents and the NO system
To further determine whether oxidative stress was involved in regulating K+ currents and NO system, preeclamptic HUVECs were cultured with apocynin (an NADPH oxidase inhibitor). After pretreatment with apocynin, whole-cell K+ currents were significantly increased in preeclamptic HUVECs (from 5.56±0.45 pA pF−1 at baseline to 9.98±0.76 pA pF−1; TP=+60 mV, P<0.05; Figure 6a). Pretreated preeclamptic HUVECs with apocynin partially rescued KCNMB1, SK3 and eNOS expression (Figures 6b–e). Moreover, NO production was also increased in preeclamptic HUVECs after pretreatment with apocynin (Figure 6f).
The effect of apocynin (NOX inhibitor) on the K+ current, KCNMB1, SK3 and eNOS expression and NO production in preeclamptic HUVECs. (a) Effect of NOX inhibitor on whole-cell K+ currents in HUVECs (N=19, n=33 for NP; N=17, n=40 for PE). (b, c) Effect of NOX inhibitor on mRNA and protein levels of KCNMB1 and SK3 in HUVECs (N=17 for NP; N=17 for PE). (d, e) mRNA and protein levels of eNOS in HUVECs (N=17 for PE). (f) NO production in HUVECs (N=15 for PE). Error bars denote s.e.m. *P<0.05; **P<0.01. eNOS, endothelial nitric oxide synthase enzyme; HUVEC, human umbilical vein endothelial cell; N, number of participants; n, number of cells; NO, nitric oxide; NOX, NADPH (nicotinamide adenine dinucleotide phosphate) oxidase; NP, normal pregnancy; PE, preeclampsia.
Discussion
This study was the first to determine associations among the endothelial NO system, potassium channels and oxidative stress in the placental–umbilical circulation and revealed the mechanism of the frail NO system in preeclampsia. The main findings include the following. (1) Compared with normal HUVECs, eNOS expression, NO production and whole-cell K+ currents were markedly decreased in preeclamptic HUVECs, whereas oxidative stress was significantly increased. (2) In preeclamptic HUVECs, the decreased whole-cell K+ currents were closely linked to the damaged KCa channels, especially BKCa and SKCa. Compared with preeclamptic HUVECs, the blockade of BKCa and/or SKCa in normal HUVECs had a significant inhibitory effect on eNOS expression. (3) The overproduction of NOX2-dependent ROS contributed to the increased oxidative stress detected in preeclamptic endothelial cells. Meanwhile, the NOX inhibitor showed a rescue effect on whole-cell K+ currents, eNOS expression and NO production in preeclamptic HUVECs. These results suggest that NOX2-derived ROS could damage the endothelial NO system via the suppression of BKCa and SKCa.
Previous studies on the NO system in preeclampsia showed various results.9, 10, 11, 34 For example, in maternal serum, there was no statistically significant difference in the eNOS levels between normal and preeclamptic pregnancies,34 whereas significantly lower eNOS levels in women with severe preeclampsia were reported in another study.9 In the placenta and/or umbilical cord, eNOS expression was also changed in preeclampsia.10, 11 Previous studies measured the NO system using only maternal serum or the placenta that may not directly reflect the endothelial NO systems in preeclampsia. Umbilical vein endothelial cells provide a classic model to study the endothelial NO system under normal and preeclamptic conditions. This study isolated and cultured normal and preeclamptic HUVECs in vitro and found that both eNOS expression and NO production were significantly reduced in preeclamptic HUVECs. This was the first report to demonstrate that the endothelial NO system was damaged in preeclampsia via directly measuring eNOS expression and NO production in isolated endothelial cells from the placenta–umbilical cord system.
Whole-cell K+ currents were also markedly decreased in the preeclamptic HUVECs. In the electrophysiological experiments, the reduction in K+ currents in normal HUVECs that were subtracted from the baseline by a selective BKCa blocker (IBTX) and/or a selective SKCa blocker (apamin) was greater than that in preeclamptic HUVECs. These results indicated that BKCa and SKCa channels were damaged in preeclamptic HUVECs and could be a major contributor to decreased whole-cell K+ currents. Molecular assays showed that the mRNA and protein levels of KCNMB1 (BKβ1 subunit) and SK3 were significantly downregulated in preeclamptic HUVECs, suggesting that the decreased cell K+ currents in preeclamptic HUVECs were associated with the downregulated expression of the BKβ1 subunit and SK3. KCa channels play important roles in the control of endothelial NO production.12, 13, 14, 15 Among KCa channels, BKCa and SKCa were demonstrated to influence NO production in cultured endothelial cells.14, 15 In this study, blockade of BKCa and SKCa in normal HUVECs not only declined K+ currents to similar levels as those in preeclamptic HUVECs but also significantly downregulated eNOS expression. These results demonstrated that the downregulated eNOS expression was closely related to BKCa and SKCa in preeclamptic HUVECs. To the best of our knowledge, this was the first study to report the influence of preeclampsia on membrane electro-activities linked to KCa channels in endothelial cells from human placental–umbilical circulation. This finding also provided new information on the possible influence of ion channels on the endothelial NO system in preeclampsia, raising the question regarding why cellular K+ channels as well as subunit expression levels were altered in preeclamptic endothelial cells.
Endothelial dysfunction under the conditions of preeclampsia has been closely related to oxidative stress.25, 26, 27 Recently, several studies have shown that ROS could impair KCa channels in the vasculature.20, 24 ROS are produced intracellularly through multiple mechanisms depending on the cell and tissue type.35 In the vasculature, NOX complexes (seven distinct isoforms) are the major sources of ROS generation. Among the seven isoforms of the NOX family, NOX1, NOX2 and NOX4 were predominantly expressed in vascular endothelial cells; specifically, NOX2 was closely associated with endothelial cell dysfunction.36, 37 In this study, both the intracellular ROS concentration and NOX2 expression were significantly increased in preeclamptic HUVECs, indicating an increased oxidative stress in preeclamptic HUVECs that was probably mediated by the overproduction of NOX2-dependent ROS. In addition, our study showed that the suppression of NOX activity with an NADPH oxidase inhibitor (apocynin) in preeclamptic HUVECs could partially rescue the altered KCNMB1, SK3 and whole-cell K+ currents. The inhibition of NOX activity also rescued eNOS expression and NO production in preeclamptic HUVECs. Together, these results indicate that heightened NOX2-mediated ROS production is involved in regulating KCa channels, modulating eNOS expression and producing NO in endothelial cells. The finding also provides new opportunities to further investigate underlying signal pathways for ROS-induced alterations in endothelial ion channels.
It is known that NO-mediated vasodilatation is one of the major functions of vascular endothelial cells. According our study, the frail endothelial NO system in preeclampsia may initiate placenta–umbilical cord vascular dysfunction, eventually leading to intrauterine fetal ischemia and developmental retardation. Thus, this study not only offers new information regarding the control of NO system in the placental–umbilical circulation but also contributes to a better understanding of the pathological process of vascular dysfunction complicated by preeclampsia.
References
Leeman L, Fontaine P . Hypertensive disorders of pregnancy. Am Fam Physician 2008; 78: 93–100.
Ducat A, Doridot L, Calicchio R, Méhats C, Vilotte JL, Castille J, Barbaux S, Couderc B, Jacques S, Letourneur F, Buffat C, Le Grand F, Laissue P, Miralles F, Vaiman D . Endothelial cell dysfunction and cardiac hypertrophy in the STOX1 model of preeclampsia. Sci Rep 2016; 6: 19196.
Tuzcu ZB, Asicioglu E, Sunbul M, Ozben B, Arikan H, Koc M . Circulating endothelial cell number and markers of endothelial dysfunction in previously preeclamptic women. Am J Obstet Gynecol 2015; 213: 533.
Roberts JM, Taylor RN, Musci TJ, Rodgers GM, Hubel CA, McLaughlin MK . Preeclampsia: an endothelial cell disorder. Am J Obstet Gynecol 1989; 161: 1200–1204.
Orabona R, Sciatti E, Vizzardi E, Bonadei I, Valcamonico A, Metra M, Frusca T . Endothelial dysfunction and vascular stiffness in women with a previous pregnancy complicated by early or late pre-eclampsia. Ultrasound Obstet Gynecol, (e-pub ahead of print 26 February 2016; doi:10.1002/uog.15893).
Nyberg M, Jensen LG, Thaning P, Hellsten Y, Mortensen SP . Role of nitric oxide and prostanoids in the regulation of leg blood flow and blood pressure in humans with essential hypertension: effect of high-intensity aerobic training. J Physiol 2012; 590: 1481–1494.
Wang Y, Gu Y, Zhang Y, Lewis DF . Evidence of endothelial dysfunction in preeclampsia: decreased endothelial nitric oxide synthase expression is associated with increased cell permeability in endothelial cells from preeclampsia. Am J Obstet Gynecol 2004; 190: 817–824.
Sakar MN, Atay AE, Demir S, Bakir VL, Demir B, Balsak D, Akay E, Ulusoy AI, Verit FF . Association of endothelial nitric oxide synthase gene G894T polymorphism and serum nitric oxide levels in patients with preeclampsia and gestational hypertension. J Matern Fetal Neonatal Med 2015; 28: 1907–1911.
Zawiejska A, Wender-Ozegowska E, Iciek R, Brazert J . Concentrations of endothelial nitric oxide synthase, angiotensin-converting enzyme, vascular endothelial growth factor and placental growth factor in maternal blood and maternal metabolic status in pregnancy complicated by hypertensive disorders. J Hum Hypertens 2014; 28: 670–676.
Du L, He F, Kuang L, Tang W, Li Y, Chen D . eNOS/iNOS and endoplasmic reticulum stress-induced apoptosis in the placentas of patients with preeclampsia. J Hum Hypertens 2017; 31: 49–55.
Bhavina K, Radhika J, Pandian SS . VEGF and eNOS expression in umbilical cord from pregnancy complicated by hypertensive disorder with different severity. Biomed Res Int 2014; 2014: 982159.
Coleman HA, Tare M, Parkington HC . Endothelial potassium channels, endothelium-dependent hyperpolarization and the regulation of vascular tone in health and disease. Clin Exp Pharmacol Physiol 2004; 31: 641–649.
Tanaka Y, Koike K, Toro L . MaxiK channel roles in blood vessel relaxations induced by endothelium-derived relaxing factors and their molecular mechanisms. J Smooth Muscle Res 2004; 40: 125–153.
Climent B, Schubert R, Stankevicius E, García-Sacristán A, Simonsen U, Rivera L . Large conductance Ca2+-activated K+ channels modulate endothelial cell outward currents and nitric oxide release in the intact rat superior mesenteric artery. Biochem Biophys Res Commun 2012; 417: 1007–1013.
Sheng JZ, Braun AP . Small- and intermediate-conductance Ca2+-activated K+ channels directly control agonist-evoked nitric oxide synthesis in human vascular endothelial cells. Am J Physiol Cell Physiol 2007; 293: C458–C467.
Zhao L, Wang Y, Ma X, Wang Y, Deng X . Oxidative stress impairs IKCa- and SKCa-mediated vasodilatation in mesenteric arteries from diabetic rats. Nan Fang Yi Ke Da Xue Xue Bao 2013; 33: 939–944.
Brakemeier S, Eichler I, Knorr A, Fassheber T, Köhler R, Hoyer J . Modulation of Ca2+-activated K+ channel in renal artery endothelium in situ by nitric oxide and reactive oxygen species. Kidney Int 2003; 64: 199–207.
Soto MA, González C, Lissi E, Vergara C, Latorre R . Ca(2+-activated K+ channel inhibition by reactive oxygen species. Am J Physiol Cell Physiol 2002; 282: C461–C471.
Park WS, Ko EA, Jung ID, Son YK, Kim HK, Kim N, Park SY, Hong KW, Park YM, Choi TH, Han J . APE1/Ref-1 promotes the effect of angiotensin II on Ca2+ -activated K+ channel in human endothelial cells via suppression of NADPH oxidase. Arch Pharm Res 2008; 31: 1291–1301.
Tang XD, Garcia ML, Heinemann SH, Hoshi T . Reactive oxygen species impair Slo1 BK channel function by altering cysteine-mediated calcium sensing. Nat Struct Mol Biol 2004; 11: 171–178.
Llurba E, Gratacós E, Martín-Gallán P, Cabero L, Dominguez C . A comprehensive study of oxidative stress and antioxidant status in preeclampsia and normal pregnancy. Free Radic Biol Med 2004; 37: 557–570.
Al-Magableh MR, Kemp-Harper BK, Hart JL . Hydrogen sulfide treatment reduces blood pressure and oxidative stress in angiotensin II-induced hypertensive mice. Hypertens Res 2015; 38: 13–20.
Horvathova M, Zitnanova I, Kralovicova Z, Balis P, Puzserova A, Muchova J, Kluknavsky M, Durackova Z, Bernatova I . Sex differences in the blood antioxidant defense system in juvenile rats with various genetic predispositions to hypertension. Hypertens Res 2016; 39: 64–69.
Choi S, Kim JA, Na HY, Kim JE, Park S, Han KH, Kim YJ, Suh SH . NADPH oxidase 2-derived superoxide downregulates endothelial KCa3.1 in preeclampsia. Free Radic Biol Med 2013; 57: 10–21.
Pottecher J, Huet O, Degos V, Bonnet MP, Gaussem P, Duranteau J, Ozier Y, Mignon A, Tsatsaris V . In vitro plasma-induced endothelial oxidative stress and circulating markers of endothelial dysfunction in preeclampsia: an observational study. Hypertens Pregnancy 2009; 28: 212–223.
Sánchez-Aranguren LC, Prada CE, Riaño-Medina CE, Lopez M . Endothelial dysfunction and preeclampsia: role of oxidative stress. Front Physiol 2014; 59: 372.
Matsubara K, Higaki T, Matsubara Y, Nawa A . Nitric oxide and reactive oxygen species in the pathogenesis of preeclampsia. Int J Mol Sci 2015; 16: 4600–4614.
Männistö T, Karumanchi SA, Pouta A, Vääräsmäki M, Mendola P, Miettola S, Surcel HM, Bloigu A, Ruokonen A, Järvelin MR, Hartikainen AL, Suvanto E . Preeclampsia, gestational hypertension and subsequent hypothyroidism. Pregnancy Hypertens 2013; 3: 21–27.
Watanapa WB, Theerathananon W, Akarasereenont P, Techatraisak K . Effects of preeclamptic plasma on potassium currents of human umbilical vein endothelial cells. Reprod Sci 2012; 19: 391–399.
Zhu X, Gao Q, Tu Q, Zhong Y, Zhu D, Mao C, Xu Z . Prenatal hypoxia enhanced angiotensin II-mediated vasoconstriction via increased oxidative signaling in fetal rats. Reprod Toxicol 2016; 60: 21–28.
Bo L, Jiang L, Zhou A, Wu C, Li J, Gao Q, Zhang P, Lv J, Li N, Gu X, Zhu Z, Mao C, Xu Z . Maternal high-salt diets affected pressor responses and microvasoconstriction via PKC/BK channel signaling pathways in rat offspring. Mol Nutr Food Res 2015; 59: 1190–1199.
Grgic I, Eichler I, Heinau P, Si H, Brakemeier S, Hoyer J, Köhler R . Selective blockade of the intermediate-conductance Ca2+-activated K+ channel suppresses proliferation of microvascular and macrovascular endothelial cells and angiogenesis in vivo. Arterioscler Thromb Vasc Biol 2005; 25: 704–709.
Haddad P, Dussault S, Groleau J, Turgeon J, Maingrette F, Rivard A . Nox2-derived reactive oxygen species contribute to hypercholesterolemia-induced inhibition of neovascularization: effects on endothelial progenitor cells and mature endothelial cells. Atherosclerosis 2011; 217: 340–349.
Wender-Ozegowska E, Zawiejska A, Iciek R, Brązert J . Concentrations of eNOS, VEGF, ACE and PlGF in maternal blood as predictors of impaired fetal growth in pregnancy complicated by gestational hypertension/preeclampsia. Hypertens Pregnancy 2015; 34: 17–23.
Muller F . The nature and mechanism of superoxide production by the electron transport chain: Its relevance to aging. J Am Aging Assoc 2000; 23: 227–253.
Sukumar P, Viswambharan H, Imrie H, Cubbon RM, Yuldasheva N, Gage M, Galloway S, Skromna A, Kandavelu P, Santos CX, Gatenby VK, Smith J, Beech DJ, Wheatcroft SB, Channon KM, Shah AM, Kearney MT . Nox2 NADPH oxidase has a critical role in insulin resistance-related endothelial cell dysfunction. Diabetes 2013; 62: 2130–2134.
Sukumar P, Viswambharan H, Imrie H, Cubbon RM, Yuldasheva N, Gage M, Galloway S, Skromna A, Kandavelu P, Santos CX, Gatenby VK, Smith J, Beech DJ, Wheatcroft SB, Channon KM, Shah AM, Kearney MT . Activin and NADPH-oxidase in preeclampsia: insights from in vitro and murine studies. Am J Obstet Gynecol 2015; 212: e1–12.
Acknowledgements
This study was supported partially by the NSFC (81320108006, 81370719 and 81401244), the Natural Science Foundation of Jiangsu Province (Grant No. BK20140292) and the Suzhou Natural Science Foundation SYS201451.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Chen, J., Gao, Q., Jiang, L. et al. The NOX2-derived reactive oxygen species damaged endothelial nitric oxide system via suppressed BKCa/SKCa in preeclampsia. Hypertens Res 40, 457–464 (2017). https://doi.org/10.1038/hr.2016.180
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.180
Keywords
This article is cited by
-
Higher prevalence of hypertensive disorders of pregnancy in women who smoke: the Japan environment and children’s study
Hypertension Research (2019)
-
Resveratrol improves endothelial cell markers impaired by plasma incubation from women who subsequently develop preeclampsia
Hypertension Research (2019)
-
ATP2B1 Gene Silencing Increases NO Production Under Basal Conditions Through the Ca2+/calmodulin/eNOS Signaling Pathway in Endothelial Cells
Hypertension Research (2018)