Abstract
Parity has previously been reported to affect the difference in blood pressure (BP) measured in the office and at home, also known as the white-coat effect, during pregnancy. The objective of this study was to identify possible factors that cause the white-coat effect during pregnancy, focusing on parity. In total, 530 pregnant women (31.3±4.7 years old) who delivered at a maternal clinic were eligible for the study. The association between parity and the white-coat effect (clinic BP compared with home BP) was investigated for each trimester of pregnancy by multivariate analysis of covariance adjusted for age, body mass index, family history of hypertension and smoking habits. The magnitudes of the white-coat effect for systolic BP in the first, second and third trimesters were 4.1±9.8, 3.4±7.1 and 1.8±6.0 mm Hg, respectively and those for diastolic BP were 3.8±7.4, 1.6±5.8 and 2.4±4.9 mm Hg, respectively. Parity was significantly and negatively associated with the white-coat effect for systolic BP in the first trimester of pregnancy (nulliparous women: 5.07±0.61 mm Hg and multiparous women: 2.78±0.74 mm Hg, P=0.02) as well as for diastolic BP in the second and third trimesters of pregnancy. Age, body mass index, family history of hypertension and smoking were not significantly associated with the white-coat effect in any trimester of pregnancy. Parity may have an influence on the white-coat effect in pregnancy; however, the observed effect, on average 1–2 mm Hg, was small.
Similar content being viewed by others
Introduction
Hypertension in pregnancy is one of the major diseases of maternity and sometimes leads to severe outcomes such as stroke, premature delivery and/or low birth weight.1 To account for this situation, standardized antenatal care in Japan includes blood pressure (BP) monitoring at almost every antenatal care visit. Because the BP of pregnant women is usually only measured in clinics or hospitals, the white-coat effect, which is defined as ‘the increase of BP that occurs during an office visit,’2 cannot be excluded. The white-coat effect often causes hypertension in the office3 and is commonly observed among pregnant women.4, 5 To evaluate the white-coat effect, out-of-office BP measurements, including ambulatory BP monitoring or home BP measurements, are essential. In particular, the mean home BP values are stable and highly reproducible.6 Therefore, the American Heart Association and the American Society of Hypertension and Preventive Cardiovascular Nurses Association have recently recommended home BP measurement for pregnant women and consider home BP measurement during pregnancy to be theoretically ideal for monitoring BP trends during pregnancy.2
It has previously been observed that the systolic BP of nulliparous women measured in the clinic is higher than that of multiparous women in the first trimester, though there was no significant difference in systolic BP measured at home between the groups.7 Therefore, it is assumed that parity influences the white-coat effect during pregnancy. Furthermore, recognition of the factors affecting the white-coat effect might be helpful to consider in antenatal care. However, the factors that influence the white-coat effect among pregnant women are unknown. Thus, the present study investigated possible factors associated with the white-coat effect in pregnancy, especially focusing on parity.
Methods
Study design
This study was a part of the ‘Babies and Their Parents’ Longitudinal Observation in Suzuki Memorial Hospital in the Intrauterine Period (BOSHI) Study. The principal objective of the BOSHI study was to investigate the relationship between the home BP and lifestyle-related diseases. The target population of the study was pregnant women who expected to deliver at Suzuki Memorial Hospital in Sendai City, Miyagi prefecture, Japan. This center has specialists in obstetrics, gynecology and in vitro fertilization. All of the study protocols were approved by the Institutional Review Board of Tohoku University Graduate School of Medicine and the Review Board of Suzuki Memorial Hospital. The details of the BOSHI study have been described elsewhere.8, 9
Study participants
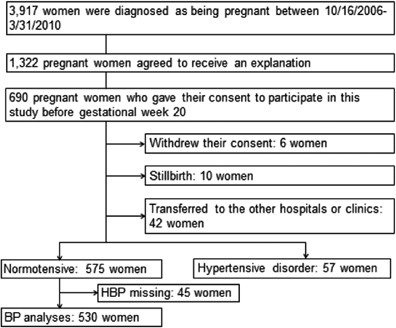
In the BOSHI study, a total of 3917 women were diagnosed as being pregnant between 1 October 2006 and 31 March 2010 and were scheduled to have their deliveries at the hospital. All of them were invited to participate in the BOSHI Study by poster advertising and a letter from the investigating staff. Among them, 1322 pregnant women agreed to receive an explanation about the BOSHI study from physicians, midwives or pharmacists, and 690 gave their consent to participate. Women who participated after week 20 of gestation did not describe details of their smoking or alcohol-drinking history, had missing BP data before gestational week 20, had hypertension before gestational week 20 or had multiple gestations were excluded. Figure 1 shows a flow diagram of the participants. A total of 690 healthy pregnant women before 20 weeks of gestation were enrolled for analysis. All of them had singleton pregnancies, and none had a history of hypertension. Data on the individual characteristics and BP before gestational week 20 were available for all of these participants. Six women withdrew their consent and ten women were excluded from the study because of fetal death during pregnancy. Another 27 women were transferred to other hospitals due to threatened premature delivery (four women), premature membrane rupture (three women), diabetes (six women), placenta previa (five women), choledochal cyst (one woman), obesity and small myoma (one woman), follow-up for lumbar fracture (one woman), anxiety neurosis (one woman) and deafness (one woman), as well as due to fetal problems, including intrauterine growth retardation (two women), suspected tetralogy of Fallot (one woman) and fetal ovarian cyst (one woman). Fifteen women were also excluded due to their transfer to the nearest midwifery clinic. During the follow-up period, 57 women developed gestational hypertension or preeclampsia. Of the remaining 575 healthy pregnant women, 45 did not measure their home BP during pregnancy and were excluded from the analysis.
Clinic BP measurement
Clinic BP was measured using a HEM705IT instrument (Omron Healthcare, Kyoto, Japan) based on the cuff-oscillometric method; this device generates a digital display of both systolic and diastolic BP and is equivalent to the Omron T9P, which is validated for pregnant women.10 When pregnant women visited the hospital, their BP was measured twice in a seated position after 1–2 min of rest. All antenatal care visits were booked between 0900 and 1500 h.
Home BP measurement
Home BP was measured using a HEM747IC or HEM7080IC semiautomatic device (Omron Healthcare) based on the cuff-oscillometric method; this device generates a digital display of both systolic and diastolic BP and is equivalent to the HEM705IT. After enrollment, the pregnant women received instruction about home BP measurement from physicians, midwives or pharmacists. Home BP measurements were based on the Japanese Society of Hypertension guidelines for self-monitoring BP at home.11 The pregnant women were asked to measure their BP at their upper arm every morning with the following guidelines: within 1 h of waking, after micturition, before breakfast, while seated and after resting for more than 1 min. They were also asked to keep recording their home BP until 1 month after delivery.
Data collection and statistical analysis
Background information and antenatal care records, including clinic BP data, were collected from the medical charts of the pregnant women. Characteristics of the participants were assessed by the mean and standard deviation (s.d.) or by numbers and percentages.
Participants had their BP measured twice at each antenatal care visit. The mean clinic BP value at each visit was calculated. Furthermore, it is standard practice in Japan for pregnant women to visit antenatal care clinics or hospitals once every 4 weeks until gestational week 23, once every 2 weeks from gestational weeks 24–35 and once a week after gestational week 36. At gestational week 40, the clinic BP measurement was taken one or more time during each antenatal care visit. Because of the irregular BP measurements, individual mean clinic BP values were estimated in the first, second and third trimesters using the individual mean clinic BP value at each visit. The first trimester of pregnancy was defined as gestational weeks 12–15, the second trimester was defined as gestational weeks 16–27 and the third trimester was defined as gestational weeks 28–40. The magnitude of the white-coat effect was calculated for each trimester as the mean clinic BP minus the mean home BP.
Multivariate analysis of covariance adjusted for age, parity, body mass index, family history of hypertension and smoking habits was used to detect possible factors affecting the white-coat effect for each trimester. Smoking habits were only analyzed in the first trimester of pregnancy. The variables listed above were reported as factors that might affect the white-coat effect in previous studies.2, 4, 12, 13, 14 Statistical significance was defined as P<0.05. All statistical analyses were carried out using the SAS package (version 9.3, SAS Institute, Cary, NC, USA).
Results
A final total of 530 healthy pregnant women were eligible for BP analysis. None of the 530 normotensive pregnant women analyzed had proteinuria >2+ by dipstick on at least two consecutive antenatal care visits. Characteristics of the participants are summarized in Table 1. The mean age of the participants was 31.3±4.7 years. Approximately 60% of the participants were nulliparous women. The mean body mass index was 21.5±3.4 kg m−2, 34.2% of the participants had a family history of hypertension and 4.0% of the participants continued to smoke even after discovering they were pregnant.
The mean frequency of BP measurements in the clinic was 1.1±0.3 in the first trimester, 3.6±1.1 in the second trimester, and 7.2±1.6 in the third trimester. The mean frequency of BP measurements at home was 10.4±6.8 in the first trimester, 40.9±23.6 in the second trimester and 40.1±24.7 in the third trimester. The maximum values of the white-coat effect were 4.1 mm Hg for systolic BP and 3.8 mm Hg for diastolic BP, both in the first trimester of pregnancy (Table 2). The minimum values of the white-coat effect were 1.8 mm Hg for systolic BP in the third trimester and 1.6 mm Hg for diastolic BP in the second trimester of pregnancy (Table 2).
Multivariate analysis of covariance for possible factors affecting the white-coat effect in each trimester of pregnancy is shown in Tables 3 and 4. Parity was significantly and negatively associated with the white-coat effect for systolic BP in the first trimester of pregnancy (nulliparous women: 5.07±0.61 mm Hg and multiparous women: 2.78±0.74 mm Hg, P=0.02 adjusted for age, body mass index, family history of hypertension and smoking), as well as for diastolic BP in the second and third trimesters of pregnancy. The average clinic and home systolic BPs of nulliparous women were 108.9 and 103.8 mm Hg in the first trimester, respectively, 107.4 and 103.5 mm Hg in the second trimester, respectively, and 107.8 and 105.6 mm Hg in the third trimester, respectively. The average clinic and home systolic BPs of multiparous women were 106.6 and 103.8 mm Hg in the first trimester, respectively, 106.2 and 103.4 mm Hg in the second trimester, respectively, and 106.7 and 105.0 mm Hg in the third trimester, respectively. The average clinic and home diastolic BPs of nulliparous women were 66.6 and 62.3 mm Hg in the first trimester, respectively, 63.3 and 61.2 mm Hg in the second trimester, respectively, and 66.0 and 63.0 mm Hg in the third trimester, respectively. The average clinic and home systolic BPs of multiparous women were 64.7 and 61.7 mm Hg in the first trimester, respectively, 61.8 and 60.9 mm Hg in the second trimester, respectively, and 64.0 and 62.5 mm Hg in the third trimester, respectively. Age, body mass index and family history of hypertension were not significantly associated with the white-coat effect throughout pregnancy. There was also no significant association between smoking and the white-coat effect in the first trimester of pregnancy.
Discussion
The present study found that parity was associated with the white-coat effect during pregnancy. In a previous study comparing clinic BP behavior throughout pregnancy with home BP behavior in groups of nulliparous and multiparous women, parity was assumed to influence the white-coat effect during pregnancy. The findings of the present study, which considered individual differences in BP between clinic BP and home BP measurements, supported the present hypothesis that parity is significantly associated with the white-coat effect during pregnancy. This is the first study to attempt to identify possible factors affecting the white-coat effect in each trimester of pregnancy.
Parity
Parity was negatively associated with the white-coat effect for systolic BP in the first trimester of pregnancy. A wide difference was previously found in systolic BP measured in the clinic between nulliparous and multiparous women in the first trimester.7 However, no significant difference was found in systolic BP measured at home between nulliparous and multiparous women.7 Therefore, it was expected that nulliparous women tend to have the white-coat effect more than multiparous women during pregnancy. It is possible that, compared with multiparous women, nulliparous women are more nervous or emotionally unstable due to their first pregnancies and antenatal care, which they have never experienced before.15 Sympathetic tone is one possible mechanism for the white-coat effect.16 However, heart rate data were not collected during antenatal care visits, so it remains unclear whether the sympathetic tone was a cause of the white-coat effect in the present study. The significant difference between systolic clinic BP and home BP in the first trimester might be partially explained by an increased response to the medical environment among nulliparous women.
As for diastolic BP, parity was negatively associated with the white-coat effect in the second and third trimesters of pregnancy. It has also previously been reported that nulliparous women tend to have higher clinic diastolic BP than multiparous women.7 The significant difference between diastolic but not systolic clinic BP and home BP in the second and third trimesters might have been caused by a decrease in the total peripheral vascular resistance caused by vasodilatation in early gestation, as well as by an increase in insulin resistance in later pregnancy, especially in nulliparous women. However, the mechanism of this phenomenon was not addressed in the present analysis. The mechanism of the white-coat effect on diastolic BP during pregnancy will be investigated in a future study.
Age
Aging has been reported to decrease the white-coat effect for systolic BP in the general population12 and in hypertensive patients.17, 18 A previous study also reported that white-coat hypertension is common among young women of childbearing age.19 However, in the present study, the previously identified associations between age and the white-coat effect for both systolic and diastolic BP were not identified throughout pregnancy. The reason for this difference might be that the age distribution was not very wide in the present study population (mean±s.d., 31.3±4.7 years old; minimum to maximum, 17.5–45.8 years old).
Body mass index
Obesity is a well-known risk factor for hypertension in pregnancy.20, 21, 22 Obesity acts through increased sympathetic activity or insulin resistance,21 which is considered to be a possible mechanism for the development of white-coat hypertension.19 In contrast, it remains uncertain whether body mass index is a factor contributing to the white-coat effect in pregnancy. Although the pregnant women whose pre-pregnancy body mass index was more than 22 kg m−2 tended to have the white-coat effect, the pre-pregnancy body mass index was not identified to be associated with white-coat effect. It is possible that the pre-pregnancy body mass indices of the study participants were mostly normal (normal weight) and that the body mass index distribution was not wide enough to show evidence of an association between obesity and the white-coat effect.
Family history of hypertension
Some previous studies have reported that a family history of cardiovascular disease is associated with the white-coat effect.14, 23 The present study considered a family history of hypertension to be a family history of cardiovascular disease because data for family history of cardiovascular disease were not available. Using this definition, no association between a family history of hypertension and the white-coat effect was observed in this study. Previous studies have found a significant association between a family history of cardiovascular diseases and the white-coat effect in patients with suspected and treated hypertension (mean age, 57–58 years; male, approximately 50%).14, 23 Therefore, it should be clarified that a family history of hypertension was not associated with the white-coat effect in pregnant women.
Smoking
Previous studies found that smokers have the white-coat effect less than non-smokers in adulthood.12, 13 The present study showed that smoking was not associated with the white-coat effect in early pregnancy. The association between smoking and the white-coat effect in middle and late pregnancy could not be investigated because data for smoking habits in middle and late pregnancy were not collected. Bakker et al.24 reported that continued smoking is associated with a steeper increase in both systolic and diastolic BP throughout pregnancy. Whether smoking affects the white-coat effect or is associated with true hypertension in middle and late pregnancy will be addressed in a future study.
Study limitations
The present study has some limitations. First, only five factors (age, parity, body mass index, family history of hypertension and smoking habit) that might affect the white-coat effect2, 4, 12, 13, 14 were addressed because the number of participants was not high enough to analyze other possible factors for the white-coat effect in pregnancy. Second, the participants did not always measure home BP on the same day that the clinic BP was measured, so BP differences were not calculated from measurements taken on the same day. Instead, the mean BP values were used to analyze the differences between clinic BP and home BP in each trimester of pregnancy. As antenatal care visits are scheduled during the daytime, clinic BP measurements are limited during pregnancy. Therefore, the timing of clinic BP measurements was more varied compared with home BP measurements. Thus, clinic BP measurements might have been affected by the diurnal BP rhythm. In addition, participants were asked to measure their home BP in the morning, based on the above-mentioned guidelines; thus, diurnal rhythms could not be confirmed, and diurnal variation was not characterized. In addition, it is difficult to estimate the day-to-day BP variation of pregnant women because of the unique changes in BP that occur during pregnancy. During pregnancy, BP decreases from the first trimester to the second trimester and reaches its lowest level around gestational week 20; after that, BP increases until delivery.8, 25 The present analysis was performed with the mean BP values for each trimester, which resulted in the inclusion of diurnal and day-to-day variations in the analysis; this variation was not corrected for in the results. The present study was not designed to monitor the changes in BP between the clinic and the home; rather, this study concerned the difference between the average clinic and home BP. Further study is necessary to investigate the day-to-day variation of BP during pregnancy. Finally, the final participants were only a fraction of the patients who were invited to take part in the study. A number of women either did not enroll or dropped out of the study because they felt it was difficult to continuously take home BP measurements. This may have led to participant selection bias. However, the mean age and prevalence of complications in the present participants were comparable to those among pregnant women in a nationwide survey previously conducted in Japan.26 Moreover, the rate of normotensive pregnant women who were eligible for the analysis was similar to that of the other study.27
In conclusion, the present study found that there is a small white-coat effect on both systolic and diastolic BP in pregnancy and that parity might be associated with the causes of the white-coat effect in pregnancy. Antenatal caregivers must consider and perhaps confirm the existence of the white-coat effect, especially in nulliparous women with mild hypertension measured in the clinic, to prevent unnecessary treatment.
References
Owens PE, Lyons SP, Rodriguez SA, O'Brien ET . Is elevation of clinic blood pressure in patients with white coat hypertension who have normal ambulatory blood pressure associated with target organ changes? J Hum Hypertens 1998; 12: 743–748.
Pickering TG, Miller NH, Ogedegbe G, Krakoff LR, Artinian NT, Goff D . American Heart Association; American Society of Hypertension; Preventive Cardiovascular Nurses Association: Call to action on use and reimbursement for home BP monitoring: a joint scientific statement from the American Heart Association, American Society of Hypertension and Preventive Cardiovascular Nurses Association. Hypertension 2008; 52: 1–9.
Pickering TG, Coats A, Mallion JM, Mancia G, Verdecchia P . Blood Pressure Monitoring. Task force V: White-coat hypertension. Blood Press Monit 1999; 4: 333–341.
Broughton Pipkin F, Sharif J, Lal S . Predicting high blood pressure in pregnancy: a multivariate approach. J Hypertens 1998; 16: 221–229.
Biswas A, Choolani MA, Anandakumar C, Arulkumaran S . Ambulatory blood pressure monitoring in pregnancy induced hypertension. Acta Obstet Gynecol Scand 1997; 76: 829–833.
Imai Y, Obara T, Asamaya K, Ohkubo T . The reason why home blood pressure measurements are preferred over clinic or ambulatory blood pressure in Japan. Hypertens Res 2013; 36: 661–672.
Ishikuro M, Obara T, Metoki H, Ohkubo T, Yamamoto M, Akutsu K, Sakurai K, Iwama N, Katagiri M, Yagihashi K, Yaegashi N, Mori S, Suzuki M, Kuriyama S, Imai Y . Blood pressure measured in the clinic and at home during pregnancy among nulliparous and multiparous women: the BOSHI study. Am J Hypertens 2013; 26: 141–148.
Metoki H, Ohkubo T, Watanabe Y, Nishimura M, Sato Y, Kawaguchi M, Hara A, Hirose T, Obara T, Asayama K, Kikuya M, Yagihashi K, Matsubara Y, Okamura K, Mori S, Suzuki M, Imai Y, BOSHI Study Group. Seasonal trends of blood pressure during pregnancy in Japan: the Babies and their Parents' Longitudinal Observation in Suzuki Memorial Hospital in Intrauterine Period study. J Hypertens 2008; 26: 2406–2413.
Metoki H, Ohkubo T, Watanabe Y, Nishimura M, Sato Y, Kawaguchi M, Hara A, Hirose T, Obara T, Asayama K, Kikuya M, Yagihashi K, Matsubara Y, Okamura K, Mori S, Suzuki M, Imai Y, BOSHI Study Group. Daily serial hemodynamic data during pregnancy and seasonal variation: the BOSHI study. Clin Exp Hypertens 2012; 34: 290–296.
Brown MA, Roberts L, Davis G, Mangos G . Can we use the Omron T9P automated blood pressure monitor in pregnancy? Hypertens Pregnancy 2011; 30: 188–193.
Imai Y, Otsuka K, Kawano Y, Shimada K, Hayashi H, Tochikubo O, Miyakawa M, Fukiyama K . Japanese Society of Hypertension: Japanese society of hypertension (JSH) guidelines for self-monitoring of blood pressure at home. Hypertens Res 2003; 26: 771–782.
Hozawa A, Ohkubo T, Nagai K, Kikuya M, Matsubara M, Tsuji I, Ito S, Satoh H, Hisamichi S, Imai Y . Factors affecting the difference between screening and home blood pressure measurements: the Ohasama Study. J Hypertens 2001; 19: 13–19.
Manios ED, Koroboki EA, Tsivgoulis GK, Spengos KM, Spiliopoulou IK, Brodie FG, Vemmos KN, Zakopoulos NA . Factors influencing white-coat effect. Am J Hypertens 2008; 21: 153–158.
Yoon HJ, Ahn Y, Kim KH, Park JC, Park JB, Park CG, Youn HJ, Choi DJ, Shin JH, Kim DW, Rim SJ, Bae JH, Kim CW . Korean Hypertension Research Network: Can pulse pressure predict the white-coat effect in treated hypertensive patients? Clin Exp Hypertens 2012; 34: 555–560.
Fenwick J, Gamble J, Nathan E, Bayes S, Hauck Y . Pre- and postpartum levels of childbirth fear and the relationship to birth outcomes in a cohort of Australian women. J Clin Nurs 2009; 18: 667–677.
Fukuhara M, Arima H, Ninomiya T, Hata J, Hirakawa Y, Doi Y, Yonemoto K, Mukai N, Nagata M, Ikeda F, Matsumura K, Kitazono T, Kiyohara Y . White-coat and masked hypertension are associated with carotid atherosclerosis in a general population: the hisayama study. Stroke 2013; 44: 1512–1517.
Mallion JM, Clerson P, Bobrie G, Genes N, Vaisse B, Chatellier G . Predictive factors for masked hypertension within a population of controlled hypertensives. J Hypertens 2006; 24: 2365–2370.
Horikawa T, Obara T, Ohkubo T, Asayama K, Metoki H, Inoue R, Kikuya M, Hashimoto J, Totsune K, Imai Y, J-HOME Study Group. Difference between home and office blood pressures among treated hypertensive patients from the Japan Home versus Office Blood Pressure Measurement Evaluation (J-HOME) study. Hypertens Res 2008; 31: 1115–1123.
Pickering TG, James GD, Boodie C, Harshfield GA, Blank S, Laragh JH . How common is white coat hypertension? JAMA 1988; 259: 225–228.
Tomoda S, Tamura T, Sudo Y, Ogita S . Effects of obesity on pregnant women: maternal hemodynamic change. Am J Perinatol 1996; 13: 73–78.
Thadhani R, Stampfer MJ, Hunter DJ, Manson JE, Solomon CG, Curhan GC . High body mass index and hypercholesterolemia: risk of hypertensive disorders of pregnancy. Obstet Gynecol 1999; 94: 543–550.
O’Brien TE, Ray JG, Chan WS . Maternal body mass index and the risk of preeclampsia: a systematic overview. Epidemiology 2003; 14: 368–374.
Lindbaek M, Sandvik E, Liodden K, Mjell J, Ravnsborg-Gjertsen K . Predictors for the white coat effect in general practice patients with suspected and treated hypertension. Br J Gen Pract 2003; 53: 790–793.
Bakker R, Steegers EA, Mackenbach JP, Hofman A, Jaddoe VW . Maternal smoking and blood pressure in different trimesters of pregnancy: the Generation R study. J Hypertens 2010; 28: 2210–2218.
Fujime M, Tomimatsu T, Okaue Y, Koyama S, Kanagawa T, Taniguchi T, Kimura T . Central aortic blood pressure and augmentation index during normal pregnancy. Hypertens Res 2012; 35: 633–638.
Ohkuchi A, Iwasaki R, Suzuki H, Hirashima C, Takahashi K, Usui R, Matsubara S, Minakami H, Suzuki M . Normal and high-normal blood pressures, but not body mass index, are risk factors for the subsequent occurrence of both preeclampsia and gestational hypertension: a retrospective cohort study. Hypertens Res 2006; 29: 161–167.
Mahendru AA, Everett TR, McEniery CM, Wilkinson IB, Lees CC . The feasibility of prospectively studying maternal cardiovascular changes from before conception. Hypertens Res 2013; 36: 698–704.
Acknowledgements
This work was supported by Grants for Scientific Research (Nos. 18590587, 18390192, 21390201, 22890017, 23590771, 23659347, 24689061 and 25670314) from the Ministry of Education, Culture, Sports, Science and Technology of Japan, a Grant-in-Aid (H21-Junkankitou[Seishuu]-Ippan-004) from the Ministry of Health, Labour and Welfare, Health and Labour Sciences Research Grants, Japan, a Grant-in-Aid for the Japan Society for the Promotion of Science (JSPS) fellows (19.7152, 20.7198, 20.7477 and 20.54043), and Grants from the Takeda Science Foundation; and Grants from the OTC Self-Medication Promotion Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Aside from the present study, HM is executing collaborative research with Omron Healthcare Ltd.
Rights and permissions
About this article
Cite this article
Ishikuro, M., Obara, T., Metoki, H. et al. Parity as a factor affecting the white-coat effect in pregnant women: the BOSHI study. Hypertens Res 38, 770–775 (2015). https://doi.org/10.1038/hr.2015.97
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2015.97
Keywords
This article is cited by
-
Hypertensive disorders of pregnancy: definition, management, and out-of-office blood pressure measurement
Hypertension Research (2022)
-
Association of maternal home blood pressure trajectory during pregnancy with infant birth weight: the BOSHI study
Hypertension Research (2020)
-
White coat hypertension in early pregnancy in women with pre-existing diabetes: prevalence and pregnancy outcomes
Diabetologia (2019)
-
Accumulation of evidence regarding home blood pressure during pregnancy is necessary
Hypertension Research (2017)
-
Monitoring and evaluation of out-of-office blood pressure during pregnancy
Hypertension Research (2017)