Abstract
CYBA (p22phox) is an integral constituent of the NADPH oxidases and is consequently a main component of oxidative stress, which is strongly associated with hypertension. This study investigates the contribution of CYBA polymorphisms toward the complex etiology of hypertension in two ethnically different populations, one located at a high altitude and the other at a low altitude. The significance of CYBA single nucleotide polymorphisms and their correlation with clinical and biochemical phenotypes were investigated in age- and ethnicity-matched unrelated permanent high-altitude residents (>3500 m) comprising 245 controls and 241 patients. The results were replicated in a second population comprising 935 controls and 545 patients who lived at a low altitude (<200 m). The analysis of covariance revealed that CYBA risk alleles and their haplotypes, rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C, were positively correlated with clinical parameters, for example, systolic blood pressure (SBP), diastolic blood pressure (DBP) and mean arterial pressure (MAP), and biochemical parameters, for example, 8-isoPGF2α level, and inversely correlated with catalase activity in patients compared with controls (P⩽0.01, each). Conversely, the protective alleles and their haplotype, rs8854G/rs9932581A/rs4873T, were inversely correlated with SBP, DBP, MAP and 8-isoPGF2α level, and positively correlated with catalase activity (P⩽0.001, each). Furthermore, correlation analysis between the clinical and biochemical parameters revealed a positive correlation of SBP, DBP and MAP with 8-isoPGF2α levels and a negative correlation with catalase activity in both populations (P<0.0001, each). CYBA (p22phox) variants influence the markers of oxidative stress and are associated with hypertension.
Similar content being viewed by others
Introduction
Reactive oxygen species (ROS)-induced oxidative stress (OS) plays a vital role in the pathophysiology of cardiovascular diseases including essential hypertension.1, 2 Several experimental models of hypertension and clinical hypertension have shown increased production of ROS3, 4, 5, 6, 7 with evidence of reduction in blood pressure (BP) when ROS scavenging molecules were used.8, 9, 10 ROS are produced by a variety of systems that involve several enzymes, such as xanthine oxidase, cyclooxygenases, lipoxygenases and NADPH oxidase.11 OS is associated with diminished antioxidants and the activation of vasoconstrictors.7 Among these vasoconstrictors, isoprostanes formed by the free radical-catalyzed peroxidation of arachidonic acid are potent vasoconstrictors.12 The metabolite 8-iso prostaglandin F2α (8-isoPGF2α) is considered to be a promising marker of oxidative injury in both animals and humans.13, 14 Conversely, catalase (CAT), an antioxidant enzyme, protects cells from oxidative damage.15 Notably, in most of the experimental hypertension models studied to date, higher ROS production coupled with decreased antioxidants is associated with increased BP.7, 16 Therefore, evaluating ROS production by assessing the 8-isoPGF2α levels along with the CAT activity can be crucial in hypertension management.
The biological regulation of BP, to a greater extent, is based on the complex interactions between environmental and genetic factors. Studies have revealed the role of the cytochrome b-245, alpha polypeptide (CYBA) gene in cellular redox homeostasis.17 Numerous genetic polymorphisms have been reported within the promoter and exonic regions of CYBA. A few of these polymorphisms are known to influence gene expression and NADPH oxidase activation, leading to elevated free radical formation along with antioxidant deficiency.18, 19 The genetic variants of CYBA have been associated with diverse cardiovascular diseases that share a similar pathology with hypertension.20, 21, 22, 23, 24, 25 The association of CYBA polymorphisms with hypertension has been studied in Asian and Caucasian populations but not without conflicting findings.18, 19, 26, 27, 28, 29 To our surprise, there is sparse literature on the role of CYBA in high-altitude (HA) hypertension; CYBA, being a vital marker of OS,18, 19 may also play a crucial role in the pathogenesis of hypertension at a HA (⩾3500 m). HA enhances a hypobaric hypoxia environment that tends to create OS.23 Although human adaptation to HA is understandably a result of advantageous genetic variations and selective pressure, a significant number of people may differ in their genetic make-up and as a consequence may fail to tolerate the extreme OS and become hypertensive. On the basis of these concepts, we hypothesized that CYBA variants may contribute to the clinical endpoints of hypertension in HA populations via oxidant and antioxidant redox imbalances and thus to essential hypertension pathophysiology. Notably, we replicated the study in a lowland population with a larger sample size and robust statistical power to ascertain the role of CYBA variants in the pathophysiology of hypertension. Furthermore, this study is the first of its type to show association of CYBA variants with essential hypertension in Indian populations at two diverse altitudes: one population at ⩾3500 m under hypobaric hypoxia environment and the other population living at ~250 m under normoxic environment. To test our hypothesis in a case–control design, we set forth three major objectives: first, to determine systolic BP (SBP), diastolic BP (DBP), mean arterial pressure (MAP), 8-isoPGF2α level and CAT activity; second, to screen genetic variants of CYBA individually and as haplotypes; and finally to correlate the genetic outcome with clinical and biochemical levels in age- and ethnicity-matched unrelated subjects of HA and lowland populations.
Materials and methods
Study participants
The study protocol and consent form were approved by the human ethics committees of CSIR-Institute of Genomics and Integrative Biology (IGIB) Delhi, Govind Ballabh (GB) Pant hospital New Delhi and Sonam Norboo Memorial (SNM) Hospital, Leh, Jammu and Kashmir. Prior to written consent, subjects were informed of the objectives, study organization and implications of their participation. Age-, gender- and ethnicity-matched unrelated participants from two different populations were recruited. First, the HA population, that is, highlanders (HLs), residing at ⩾3500 m was recruited through the hypertension and general outpatient clinic of SNM hospital. This population comprised 241 hypertensive patients (HHLs) and 245 normotensive controls (NHLs). Second, the lowland North-Indian population, that is, lowlanders (LLs), residing at <200 m was recruited through the hypertension and general outpatient clinic of GB Pant hospital. This population comprised 545 hypertensive patients (HLLs) and 935 normotensive controls (NLLs). The clinicians administered a detailed questionnaire about environmental factors, life style, health, clinical history, residential region and hemodynamic parameters.
Inclusion and exclusion criteria and clinical assessment
The inclusion and clinical assessment criteria for both the populations were similar. Recruitment criteria for HHLs and HLLs included the following: age 25–60 years, SBP ⩾140 mm Hg and/or DBP ⩾90 mm Hg (JNC VII) and absence of antihypertensive medication. Recruitment criteria for NHLs and NLLs included the following: age 25–60 years, SBP <120 and DBP <80 mm Hg, absence of family history of hypertension and any medication. Participants with a history of coronary artery disease, cerebrovascular disease, stroke, secondary hypertension, diabetes mellitus and renal diseases were excluded. Moreover, a significant number of subjects were excluded for reasons such as a lack of consent for the study, medication use, and to maintain both the age limit and the male to female ratio.
All subjects rested for 5 min prior to BP measurement. The clinician recorded three BP measurements, with the subject in a supine position, using a calibrated mercury sphygmomanometer with the appropriate adult cuff size. The point at which the first of two or more Korotkoff sounds were heard was recorded as the SBP and the disappearance of the Korotkoff sound as the DBP. A venous blood sample (10 ml, and after overnight fasting) was taken from each subject; subjects were in a supine position during the procedure. Blood plasma was used for the estimation of biochemical parameters. Genomic DNA was isolated from peripheral blood leukocytes using a modified salting-out protocol.30 The isolated DNA and plasma samples were stored at −80 °C if not used immediately.
Biochemical parameters
The plasma 8-isoPGF2α levels were measured using a competitive ELISA kit (Assay Designs, Farmingdale, NY, USA). CAT enzymatic activity was quantified using spectrometry by measuring the rate of catalytic elimination of hydrogen peroxide. The rate of disintegration of hydrogen peroxide into water and oxygen by CAT is proportional to its catalytic activity. Estimations were performed in duplicate on a high-throughput SpectraMaxplus384 spectrophotometer (Molecular Devices, Sunnyvale, CA, USA). Routine biochemical parameters, for example, total cholesterol, triglycerides, glucose and uric acid, were estimated on an Autoanalyzer (Elecsys 2010, Roche, Germany). The intra- and inter-assay coefficient of variations were <10% for all the measurements.
Selection and genotyping of CYBA single nucleotide polymorphisms (SNPs)
SNPs were selected based on their location in the gene, clinical and functional relevance, and their tagging with other SNPs from the genotype data available in the international HapMap project (http://hapmap.ncbi.nlm.nih.gov). Three SNPs were eventually selected for this study. The SNPs rs8854G/A (−1442G/A) and rs9932581A/G (−930A/G) are located in the promoter region. The allele rs9932581G is known to increase the transcriptional activity of the promoter as it lies in a potential binding site for the C/EBP (CCAAT/enhancer-binding protein) transcription factor.19 The third SNP rs4673C/T (242C/T or H72Y), located on exon 4, changes the amino acid histidine to tyrosine in the potential heme-binding site resulting in the loss of oxidative function and superoxide production.19 The SNPs rs8854G/A, rs9932581A/G and rs4673C/T were genotyped using SNaPshot ddNTP primer extension PCR (Applied Biosystems, Foster City, CA, USA). Two observers independently read and confirmed all the genotypes; discrepancies, if any, were resolved by repeating PCR-RFLP and SNaPshot.
Linkage disequilibrium (LD) and haplotypes
The extent of association, that is, the Lewontin’s coefficient (D′) and squared correlation coefficient (r2) for pairwise LD was calculated by Haploview-v4.0.31 Haplotypes were estimated from genotypes using software PHASEv2.1.1.32 The order of SNPs in inferred haplotypes was based on their physical location, starting from SNPs at the upstream promoter region to downstream. A frequency cutoff of 2% was applied to both populations separately, and haplotypes with <2% frequency were excluded from the analysis. The distribution of each haplotype was compared using multivariate logistic regression analysis. Depending upon the P-value and odds ratio (OR), the haplotypes were categorized as significant risk and/or protective haplotypes.
Correlation analysis
First, the individual genetic variants and haplotypes of CYBA were correlated with clinical parameters, that is, SBP, DBP and MAP. Second, the genetic outcomes were correlated with the two biochemical parameters, that is, 8-isoPGF2α level and CAT activity in both the patients and controls of the two populations. Third, the correlation between the clinical and biochemical parameters was also performed to understand their synchronized effect.
Statistical analysis
Unpaired Student's t-test was performed to compare the differences in baseline characteristics and demographic features between the two groups. A goodness-of-fit test was used for testing the Hardy–Weinberg Equilibrium, and a χ2 test compared the genotype and allele frequencies of CYBA polymorphisms between the controls and patients in the two populations. Risk prediction for hypertension was estimated by OR at 95% confidence interval using multivariate logistic regression by SPSS-12 (SPSS, Chicago, IL, USA). Haplotype distribution was compared by multiple regression analysis based on the frequency of each individual haplotype vs. all combined in each population. Furthermore, the clinical characteristics and biochemical parameters were tested for normal distribution using the Shapiro-Wilk test and expressed as the mean±s.d. The 8-isoPGF2α levels were log-transformed before analysis to follow a normal distribution. The categorical and continuous variables between patients and controls of the two populations were analyzed with a general linear model. The power of the sample size to detect the association at α=0.05 was calculated using SPSS-12. A P-value of <0.05 after adjustment for confounding factors and Bonferroni’s correction for multiple testing was considered statistically significant. As the total number of SNPs was three, the P-value was therefore multiplied by three for Bonferroni’s correction test.
Results
Demographic and phenotypic profiles
The main characteristics of the two study populations are presented in Table 1. In HHLs and HLLs, the SBP, DBP and MAP and 8-isoPGF2α levels were significantly higher, whereas CAT activity was significantly lower compared with NHLs and NLLs (P<0.0001, each). The distribution of the clinical and biochemical parameters followed a normal distribution in both the groups (P>0.05).
Single-locus association analyses
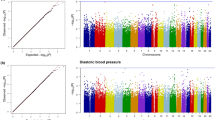
The allele and genotype frequencies of the three studied polymorphisms were in Hardy–Weinberg Equilibrium (P>0.05) for the controls and patients in both populations. When checked for tagging with other SNPs, the three SNPs were observed as singleton in all the HapMap populations. HHLs, in a comparative allele frequency analysis, revealed a similar allelic distribution pattern for the studied CYBA SNPs with HapMap Han Chinese (Beijing, China, CHB) and Japanese (Tokyo, Japan, JPT) (P>0.05; Supplementary Figure 1a); whereas HLLs were closer to HapMap Northern and Western European ancestry (CEU), Gujarati Indians (Houston, Texas, GIH) and Mexican ancestry (Los Angeles, California, MEX) (P>0.05; Supplementary Figure 1b). The results of the single-locus analyses are shown in Table 2. The multiple-logistic regression analysis, after adjustment for potential confounding factors, revealed overrepresentation of the CYBA genotypes rs9932581GG+GA and rs4873CC+TC in HHLs compared with NHLs (P=0.034 and P=0.135, respectively). As a consequence, the rs9932581G and rs4873C alleles were significantly prevalent in HHLs and were associated with an increased risk of hypertension (P=0.047, OR=1.30; P=0.024, OR=1.47). Similarly, the genotypes rs8854AA+GA, rs9932581GG+GA and rs4873CC+TC were overrepresented in HLLs compared with NLLs (P=0.012, P<0.001 and P=0.001, respectively). As a consequence, the rs8854A, rs9932581G and rs4873C alleles were significantly prevalent in HLLs and were associated with an increased risk of hypertension (P=0.004, OR=1.43; P<0.001, OR=1.38; P<0.001, OR=1.42).
LD and haplotype analysis
To understand the extent of involvement and the relationship among the CYBA SNPs, pairwise LD was assessed by D′ and r2. The pairwise LD was similar for both patients and controls of the two populations. The haplotype analysis was also performed in both populations. A total of five haplotypes were identified after an overall cutoff frequency of >2% (Table 3). However, the logistic regression analysis and Bonferroni’s correction for multiple testing after adjustment for seven confounding factors, that is, age, gender, BMI, alcohol, smoking, TG and cholesterol, revealed two haplotypes rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C as risk conferring in both HLs (OR=2.3, OR=1.2, respectively) and LLs (OR=1.6 and OR=1.3, respectively). Conversely, a single haplotype, rs8854G/rs9932581A/rs4873T, was significantly prevalent in NHLs and NLLs and appeared to be protective haplotypes (OR⩽0.7, P=0.001 each). The omnibus global test for the haplotypes also showed a significant association with hypertension in both populations (P<0.0001, each).
Correlation analyses
Single locus vs. clinical parameters
In HHLs, the general linear model revealed that the rs9932581G risk allele was correlated with an increase of 3.6 mm Hg SBP (P=0.040), and rs4873C was correlated with an increase of 4.8 mm Hg SBP and 3.5 mm Hg MAP (P⩽0.038, Figure 1a). In NHLs, however, rs9932581G was correlated with an increase of 1.3 mm Hg SBP and rs4873C was correlated with an increase of 2.0 mm Hg DBP (P=0.021, Supplementary Figure 2a). Similarly, in HLLs, rs9932581G and rs4873C were correlated with an increase of 2.4 and 4.0 mm Hg SBP (P=0.005; P=5.21E-6), 1.1 and 1.8 mm Hg DBP (P=0.006; P=2.01E-5) and 1.6 and 2.5 mm Hg MAP (P=0.001; P=3.41E-7), respectively; another risk allele, rs8854A, was also correlated with an increase of 1 mm Hg MAP (P=0.006, Figure 1b). In NLLs, however, the three risk alleles, that is, rs8854A, rs9932581G and rs4873C correlated with increased SBP, DBP and MAP but did not reach significance (P>0.05), Supplementary Figure 2b.
Correlation analyses for CYBA SNPs with clinical parameters SBP, DBP and MAP in (a) HHLs (b) HLLs and for CYBA haplotypes with clinical parameters SBP, DBP and MAP in (c) HHLs (d) HLLs. The x axis represents (a) and (b) individual CYBA SNPs and the respective alleles embedded in the bars and, (c) and (d) individual CYBA haplotypes. The y axis represents clinical data as the mean±s.d. The general linear model was used to calculate significance level (P) after adjustment for age, gender, smoking, alcohol, triglyceride, cholesterol and Bonferroni’s correction test. The numerator and denominator represent (a) and (b) frequency of protective and risk allele, respectively and, (c) and (d) frequency of remaining haplotypes (R) and studied haplotype (H), respectively. A full color version of this figure is available at Hypertension Research.
Single locus vs. biochemical parameters
In HHLs, the general linear model revealed that the risk alleles rs9932581G and rs4873C were correlated with a decrease of 1.8 and 2.8 U ml−1 CAT activity (P⩽4.37E-07, Figure 2a) and an increase of 0.9 and 0.6 pg ml−1 8-isoPGF2α level, respectively (P=2.39E-14 and P=8.46E-05, respectively, Figure 2a). Similarly, in HLLs, the risk allele rs4873C was correlated with a decrease of 2.3 U ml−1 CAT activity (P=0.001, Figure 2b), whereas the rs8854A, rs9932581G and rs4873C risk alleles were correlated with an increase of 0.3–0.5 U ml−1 8-isoPGF2α level (P=6.21E-06, P=1.22E-08 and P=8.98E-19, respectively, Figure 2b). In the NHLs and NLLs, the risk alleles were correlated with marginal decrease in CAT activity and an increase in 8-isoPGF2α level (Supplementary Figure 3a and b).
Correlation analyses for CYBA SNPs with biochemical parameters catalase activity and 8-isoPGF2α level (pg ml−1) (U ml−1) in (a) HHLs and (b) HLLs and for CYBA haplotypes with biochemical parameters catalase activity and 8-isoPGF2α level (pg ml−1) (U ml−1) in (c) HHLs and (d) HLLs. The x axis represents (a) and (b) individual CYBA SNPs and the respective alleles embedded in the bars and, (c) and (d) individual CYBA haplotypes. The y axis represents biochemical data as the mean±s.d. The general linear model was used to calculate significance level (P) after adjustment for age, gender, smoking, alcohol, triglyceride, cholesterol and Bonferroni’s correction test. The numerator and denominator represent (a) and (b) frequency of protective and risk allele, respectively and, (c) and (d) frequency of remaining haplotypes (R) and studied haplotype (H), respectively. A full color version of this figure is available at Hypertension Research online.
Haplotypes vs. clinical parameters
In HHLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with an increase of 6.7 and 3.5 mm Hg SBP, 5.6 and 0.6 mm Hg DBP, and 5.9 and 1.5 mm Hg MAP, respectively (Figure 1c). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was marginally correlated with a decrease of 4.2 mm Hg SBP, 2.7 mm Hg DBP and 3.2 mm Hg MAP (Figure 1c). In NHLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with an increase of 0.5 and 1.7 mm Hg SBP, 5.6 and 0.9 mm Hg DBP, and 3.9 and 1.2 mm Hg MAP, respectively (Supplementary Figure 2c). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with a decrease of 3.3 mm Hg SBP, 3.4 mm Hg DBP and 3.4 mm Hg MAP, (P⩽0.0009, Supplementary Figure 2c).
In HLLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with an increase of 7.0 and 3.9 mm Hg SBP, 2.4 and 1.9 mm Hg DBP, and 3.9 and 2.5 mm Hg MAP, respectively, (P⩽6.7E-05, Figure 1d). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with a decrease of 5.4 mm Hg SBP, 3.1 mm Hg DBP and 3.9 mm Hg MAP (P⩽1.1E-0.6, Figure 1d). In NLLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with an increase of 2.8 and 0.8 mm Hg SBP (P⩽0.02), 1.0 and 0.3 mm Hg DBP, and 1.6 and 0.5 mm Hg MAP (P⩽0.05, respectively, Supplementary Figure 2d). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with a decrease of 3.3 mm Hg SBP, 3.4 mm Hg DBP and 3.4 mm Hg MAP (P⩽0.0008, Supplementary Figure 2d).
Haplotypes vs. biochemical parameters
In HHLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with a decrease of 2.9 and 1.6 U ml−1 CAT activity, respectively (P⩽0.007, Figure 2c) and an increase of 1.8 and 0.5 pg ml−1 8-isoPGF2α level (P⩽1.46E-5, Figure 2c), respectively. Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with an increase of 1.6 U ml−1 CAT activity (P⩽0.0009, Figure 2c) and a decrease of 1.9 pg ml−1 8-isoPGF2α level (P⩽2.24E-17, Figure 2c). In NHLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were marginally correlated with a decrease of 0.9 and 1.6 U ml−1 CAT activity, respectively, and an increase of 0.1 and 0.2 pg ml−1 8-isoPGF2α level, respectively; (Supplementary Figure 3c). Conversely, the protective haplotype rs8854G/rs9932581A/rs4873T was correlated with an increase of 3.7 U ml−1 CAT activity (P⩽0.001, Supplementary Figure 3c) and a decrease of 0.3 pg ml−1 8-isoPGF2α level (P⩽0.01, Supplementary Figure 3c).
In HLLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with a decrease of 3.9 and 1.8 U ml−1 CAT activity, respectively (P⩽0.02, Figure 2d), and an increase of 1.3 and 0.2 pg ml−1 8-isoPGF2α level, respectively (P⩽0.001, Figure 2d). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with an increase of 4.2 U ml−1 CAT activity (P⩽1.35E-8, Figure 2d) and a decrease of 1.3 pg ml−1 8-isoPGF2α level (P⩽3.89E-105, Figure 2d). In NLLs, the rs8854A/rs9932581G/rs4873C and rs8854G/rs9932581G/rs4873C risk haplotypes were correlated with a decrease of 1.2 and 0.1 U ml−1 CAT activity, respectively, and an increase of 0.2 and 0.1 pg ml−1 8-isoPGF2α level, respectively (P⩽1.66E-6, Supplementary Figure 3d). Conversely, the rs8854G/rs9932581A/rs4873T protective haplotype was correlated with an increase of 1.3 U ml−1 CAT activity (P⩽0.04, Supplementary Figure 3d) and a decrease of 0.2 pg ml−1 8-isoPGF2α level (P⩽2.95E-7, Supplementary Figure 3d).
Correlation between clinical and biochemical parameters
As shown in Figures 3a and b, MAP showed a significant negative correlation with CAT activity in the highland groups, that is, HHLs (P=4.08E-09) and NHLs (P=1.59E-6), as well as in both the lowland groups, that is, HLLs (P=5.79E-16) and NLLs (P=6.46E-23). Furthermore, as shown in Figures 3c and d, MAP showed a significant positive correlation with 8-isoPGF2α in both the highland groups, that is, HHLs (P=1.19E-25) and NHLs (P=3.15E-7), as well as in both the lowland groups, that is, HLLs (P=3.00E-50) and NLLs (P=8.27E-74). Similarly, SBP and DBP showed significant negative correlation with CAT activity in the highland groups, that is, HHLs (P=1.61E-11 and P=0.015, respectively) and NHLs (P=2.21E-5 and P=2.61E-5, respectively), as well as in both the lowland groups, that is, HLLs (P=2.67E-20 and P=3.16E-07, respectively) and NLLs (P=6.69E-28 and P=4.76E-13, respectively). Furthermore, these parameters showed a significant positive correlation with 8-isoPGF2α in both the highland groups, that is, HHLs (P=3.75E-12 and P=4.01E-12, respectively) and NHLs (P=4.21E-4 and P=1.29E-6, respectively), as well as in both the lowland groups, that is, HLLs (P=1.16E-30 and P=7.87E-27, respectively) and NLLs (P=5.96E-39 and P=2.50E-10, respectively).
Correlation analyses between MAP and catalase activity in (a) HLs and (b) LLs and correlation analyses between MAP and 8-isoPGF2α level in (c) HLs and (d) LLs. The x axis represents (a) and (b) catalase activity (U ml−1) and, (c) and (d) 8-isoPGF2α level (pg ml−1). The y axis represents clinical data (mm Hg). The MAP is correlated with catalase activity in (a) HLs and (b) in LLs, respectively, in patients and controls. The MAP is correlated with 8-isoPGF2α level in (c) HLs and (d) LLs, respectively, in patients and controls. A two-tailed P-value of <0.05 after multiple Bonferroni’s correction test was considered statistically significant. R2 represents regression co-efficient and P represents significance level. A full color version of this figure is available at Hypertension Research online.
Discussion
This study was performed in two different populations residing in contrasting environmental conditions, and the findings supported our hypothesis. The analysis of covariance revealed that CYBA risk and protective alleles and their haplotypes were correlated differentially with clinical and biochemical parameters. Of interest, our results successfully revealed the potential role of CYBA polymorphisms in hypertension susceptibility in two ethnically diverse populations residing at two contrasting altitudes.
Single locus analysis revealed that the three SNPs followed goodness-of-fit test in both populations. The presence of alleles, that is, rs8854A, rs9932581G and rs4673C, was associated with a higher risk for hypertension in both populations even after adjustment for potential confounders. The same risk alleles, in other populations, have been shown to be associated with cardiovascular diseases including hypertension.18, 19, 20, 21, 22, 23, 24, 33 When compared with the HapMap populations for allele frequencies, the HLs exhibited similarity to CHB and JPT, whereas LLs exhibited similarity to CEU, GIH and MEX.
Hypertension, being a multigenic disorder, is not mediated by a single variation. Hence, haplotype analysis was performed to determine the combined effect of individual associations. The outcomes were encouraging as the two haplotypes, that is, rs8854A/rs9932581G/rs4673C and rs8854G/rs9932581G/rs4673C, were associated with the risk of hypertension and a single haplotype rs8854G/rs9932581A/rs4673T was associated with protection. The combined effect of SNPs compared with individual SNPs was more substantial with higher odds of hypertension susceptibility. The risk variants on the promoter and exonic regions seem to enhance the impairment of the redox balance and hence higher BP phenotypes.18, 19, 26, 27, 28, 29
The general linear model revealed the correlation of the risk alleles of CYBA with elevated clinical and biochemical parameters in both HLs and LLs; in accordance, the risk haplotypes were also significantly correlated with elevated BP and 8-isoPGF2α levels and reduced CAT activity. The correlation was more significant in hypertensive groups compared with normotensives. These results inferred that the risk alleles individually or in combination made an appreciable contribution to increased OS in the body, and thus to increased susceptibility to hypertension. A recent study in spontaneously hypertensive rats also demonstrated that increased CAT activity might cause higher total antioxidant stress and that lower hydrogen peroxide levels contribute to hypertension pathogenesis.34 Importantly, there was a proportional correlation between the clinical and biochemical parameters, which suggested a synergism among these parameters and the genetic markers in both a healthy state or a pathological condition.
To further understand the downstream effect of genotypic alterations on the immediate phenotype, two biochemical markers of OS, for example, CAT and 8-isoPGF2α were investigated. CAT, an antioxidant enzyme with high specific activity, along with glutathione peroxidase protects hemoglobin from oxidative damage. CAT catalyzes the rapid decomposition of hydrogen peroxide that otherwise may contribute to higher levels of lipid peroxidation products, which includes 8-isoPGF2α.35 In tissues, 8-isoPGF2α is produced primarily from esterified arachidonic acid by non-enzymatic reactions catalyzed by free radicals and is known to be involved in the pathogenesis of various diseases.36 The depleted CAT activity may be responsible for excessive ROS production and the observed elevated 8-isoPGF2α levels in the patients. This condition along with the inflammatory process may create an ideal OS environment that enhances vascular damage.15, 35 Although ROS can be both beneficial and damaging in biological systems depending on the environment,16, 15, 16, 17 the oxidant–antioxidant imbalance in hypertensive patients in the present study revealed a shift towards oxidants suggesting its contribution to the pathophysiology of the disease.16, 17 Additionally, it has been reported that OS (as measured by high DNA damage and lower total antioxidant status) is significantly highest for the non-dipper hypertensive group followed by the dipper hypertensive group compared with the control group.37
It was apparent that the risk alleles in association with elevated BP and OS marker and reduced antioxidants led to vascular endothelial cell dysfunction. Such a change was reported to disturb the endothelium-derived relaxing factors such as nitric oxide, prostacyclin and endothelium-derived hyperpolarizing factor, or increased production of contracting factors such as endothelin-1 and thromboxane A2.12 It may also indicate that the increased activity of signaling pathways of vascular smooth muscle contraction such as Ca2+, protein kinase C, mitogen-activated protein kinase and Rho kinase may enhance vasoconstriction.38 In fact, in our studies we have consistently observed reduced levels of nitric oxide, a potent vasodilator, in hypertensive patients.39, 40, 41, 42
Overall, the assessment of the two populations the present study support the use of CYBA genetic variants as susceptible and/or predisposing hypertension markers. To bolster genetic association of low-sample-sized HLs, the results were replicated in LLs with a power of association of more than 80%. These genetic markers are associated with reduced antioxidant capability, elevated oxidant products and with differential BP phenotype, suggesting their role in susceptibility to hypertension. We are the first to demonstrate the association of CYBA variants with clinical and biochemical parameters in both diseased and normal state in a HA population and validated the findings in a low-altitude population. Despite the different environmental conditions, both populations complemented the genetic, clinical and biochemical findings.
The study can potentially provide a platform to elucidate the causative effect of CYBA genetic markers using in vivo and in vitro molecular studies. The genotype–phenotype correlations in two distinct populations substantially suggest the possibility of pharmacological interventions. In patients, the higher frequency of risk alleles and their significant association with increased oxidants and reduced antioxidant levels initiate the probable mechanisms of BP heritability and hypertension physiopathology. Similarly, in controls, the dominance of protective alleles and their significant association with decreased oxidants and increased antioxidant levels initiate the body’s vascular homeostasis maintenance mechanisms. This study contributed to the insight into hypertension genetics and to future translation of genetic findings into hypertension prophylaxis and treatment. Genotype–phenotype correlation results provide promising advancements in the understanding of hypertension pathogenesis, which provides new insights into BP control and a cure for hypertension. The understanding of the interactions of clinically and functionally relevant CYBA variants coupled with levels of catalase activity and 8-isoPGF2α in hypertension encourage better BP management protocols to help decrease the morbidity and mortality rates related to cardiovascular diseases. Nevertheless, the limitations of the study cannot be overlooked. Foremost is the smaller sample size of the HA population; similarly, the selection of few CYBA markers and the functional validation of the identified variants are limitations.
References
Paravicini TM, Touyz RM . Redox signaling in hypertension. Cardiovasc Res 2006; 71: 247–258.
Lu Q, Yang Y, Villar VA, Asico L, Jones JE, Yu P, Li H, Weinman EJ, Eisner GM, Jose PA . D5 dopamine receptor decreases NADPH oxidase, reactive oxygen species and blood pressure via heme oxygenase-1. Hypertens Res 2013; 36: 684–690.
Kerr S, Brosnan MJ, McIntyre M, Reid JL, Dominiczak AF, Hamilton CA . Superoxide anion production is increased in a model of genetic hypertension: role of the endothelium. Hypertension 1999; 33: 1353–1358.
Lerman LO, Nath KA, Rodriguez-Porcel M, Krier JD, Schwartz RS, Napoli C, Romero JC . Increased oxidative stress in experimental renovascular hypertension. Hypertension 2001; 37: 541–546.
Somers MJ, Mavromatis K, Galis ZS, Harrison DG . Vascular superoxide production and vasomotor function in hypertension induced by deoxycorticosterone acetate-salt. Circulation 2000; 101: 1722–1728.
Kopkan L, Cervenka L . Renal interactions of renin-angiotensin system, nitric oxide and superoxide anion: implications in the pathophysiology of salt-sensitivity and hypertension. Physiol Res 2009; 58: S55–S67.
Ponnuchamy B, Khalil RA . Cellular mediators of renal vascular dysfunction in hypertension. Am J Physiol Regul Integr Comp Physiol 2009; 296: R1001–R1018.
Ulker S, McKeown PP, Bayraktutan U . Vitamins reverse endothelial dysfunction through regulation of eNOS and NAD(P)H oxidase activities. Hypertension 2003; 41: 534–539.
Uehara Y, Kawabata Y, Hirawa N, Takada S, Nagata T, Numabe A, Iwai J, Sugimoto T . Possible radical scavenging properties of cicletanine and renal protection in Dahl salt sensitive rats. Am J Hypertens 1993; 6: 463–472.
Simonsen U, Christensen FH, Buus NH . The effect of tempol on endothelium-dependent vasodilatation and blood pressure. Pharmacol Ther 2009; 122: 109–124.
Mueller CF, Laude K, McNally JS, Harrison DG . ATVB in focus: redox mechanisms in blood vessels. Arterioscler Thromb Vasc Biol 2005; 25: 274–278.
Takahashi K, Nammour TM, Fukunaga M, Ebert J, Morrow JD, Roberts LJ 2nd, Hoover RL, Badr KF . Glomerular actions of a free radical-generated novel prostaglandin, 8-epi-prostaglandin F2 alpha, in the rat. Evidence for interaction with thromboxane A2 receptors. J Clin Invest 1992; 90: 136–141.
Morrow JD, Hill KE, Burk RF, Nammour TM, Badr KF, Roberts LJ . A series of prostaglandin F2-like compounds are produced in vivo in humans by a non-cyclooxygenase, free radical-catalyzed mechanism. Proc Natl Acad Sci U S A 1990; 87: 9383–9387.
Roberts LJ, Morrow JD . The generation and actions of isoprostanes. Biochim Biophys Acta 1997; 1345: 121–135.
Schriner SE, Linford NJ, Martin GM, Treuting P, Ogburn CE, Emond M, Coskun PE, Ladiges W, Wolf N, Van Remmen H, Wallace DC, Rabinovitch PS . Extension of murine life span by overexpression of catalase targeted to mitochondria. Science 2005; 308: 1909–1911.
Higashi Y, Sasaki S, Nakagawa K, Matsuura H, Oshima T, Chayama K . Endothelial function and oxidative stress in renovascular hypertension. N Engl J Med 2002; 346: 1954–1962.
Lee MY, Griendling KK . Redox signaling, vascular function, and hypertension. Antioxid Redox Signal 2008; 10: 1045–1059.
San JG, Moreno MU, Olivan S, Beloqui O, Fortuno A, Diez J, Zalba G . Functional effect of the p22phox -930A/G polymorphism on p22phox expression and NADPH oxidase activity in hypertension. Hypertension 2004; 44: 163–169.
Moreno MU, San JG, Fortuno A, Beloqui O, Diez J, Zalba G . The C242T CYBA polymorphism of NADPH oxidase is associated with essential hypertension. J Hypertens 2006; 24: 1299–1306.
Fang S, Wang L, Jia C . Association of p22phox gene C242T polymorphism with coronary artery disease: a meta-analysis. Thromb Res 2010; 125: e197–e201.
de Oliveira AR, Santos PC, Dias RG, Rodrigues MV, de Sa CR, Mill JG, Junior WN, Krieger JE, Pereira AC . Association between the C242T polymorphism in the p22phox gene with arterial stiffness in the Brazilian population. Physiol Genomics 2012; 44: 587–592.
Narne P, Ponnaluri KC, Singh S, Siraj M, Ishaq M . Relationship between NADPH oxidase p22phox C242T, PARP-1 Val762Ala polymorphisms, angiographically verified coronary artery disease and myocardial infarction in South Indian patients with type 2 diabetes mellitus. Thromb Res 2012; 130: e259–e265.
Mishra A, Ali Z, Vibhuti A, Kumar R, Alam P, Ram R, Thinlas T, Mohammad G, Qadar Pasha MA . CYBA and GSTP1 variants associate with oxidative stress under hypobaric hypoxia as observed in high-altitude pulmonary oedema. Clin Sci (Lond) 2012; 122: 299–309.
Moreno MU, Zalba G . CYBA gene variants as biomarkers for coronary artery disease. Drug News Perspect 2010; 23: 316–324.
Qi Y, Zhao H, Wang Y, Wang Y, Lu C, Xiao Y et al. Replication of the top 10 most significant polymorphisms from a large blood pressure genome-wide association study of northeastern Han Chinese East Asians. Hypertens Res 2014; 37: 134–138.
Kokubo Y, Iwai N, Tago N, Inamoto N, Okayama A, Yamawaki H, Naraba H, Tomoike H . Association analysis between hypertension and CYBA, CLCNKB, and KCNMB1 functional polymorphisms in the Japanese population—the Suita Study. Circ J 2005; 69: 138–142.
San JG, Fortuno A, Beloqui O, Diez J, Zalba G . NADPH oxidase CYBA polymorphisms, oxidative stress and cardiovascular diseases. Clin Sci (Lond) 2008; 114: 173–182.
Perianayagam MC, Liangos O, Kolyada AY, Wald R, MacKinnon RW, Li L, Rao M, Balakrishnan VS, Bonventre JV, Pereira BJ, Jaber BL . NADPH oxidase p22phox and catalase gene variants are associated with biomarkers of oxidative stress and adverse outcomes in acute renal failure. J Am Soc Nephrol 2007; 18: 255–263.
Zalba G, San JG, Moreno MU, Fortuno A, Diez J . NADPH oxidase-mediated oxidative stress: genetic studies of the p22(phox) gene in hypertension. Antioxid Redox Signal 2005; 7: 1327–1336.
Miller SA, Dykes DD, Polesky HF . A simple salting out procedure for extracting DNA from human nucleated cells. Nucleic Acids Res 1988; 16: 1215.
Barrett JC, Fry B, Maller J, Daly MJ . Haploview: analysis and visualization of LD and haplotype maps. Bioinformatics 2005; 21: 263–265.
Stephens M, Smith NJ, Donnelly P . A new statistical method for haplotype reconstruction from population data. Am J Hum Genet 2001; 68: 978–989.
Wu Z, Lou Y, Jin W, Liu Y, Lu L, Chen Q, Xie Y, Lu G . Relationship of the p22phox (CYBA Gene Polymorphism C242T with Risk of Coronary Artery Disease: A Meta-Analysis. PLoS One 2013; 8: e70885.
Sundaram A, Siew Keah L, Sirajudeen KN, Singh HJ . Upregulation of catalase and downregulation of glutathione peroxidase activity in the kidney precede the development of hypertension in pre-hypertensive SHR. Hypertens Res 2013; 36: 213–218.
Lardinois OM, Rouxhet PG . Peroxidatic degradation of azide by catalase and irreversible enzyme inactivation. Biochim Biophys Acta 1996; 1298: 180–190.
Pratico D, Rokach J, Lawson J, FitzGerald GA . F2-isoprostanes as indices of lipid peroxidation in inflammatory diseases. Chem Phys Lipids 2004; 128: 165–171.
Gur M, Elbasan Z, Yildiray SD, Yildiz KN, Seker T, Ozaltun B, Caylı M, Kocyigit A . DNA damage and oxidative status in newly diagnosed, untreated, dipper and non-dipper hypertensive patients. Hypertens Res 2013; 36: 166–171.
Cain AE, Khalil RA . Pathophysiology of essential hypertension: role of the pump, the vessel, and the kidney. Semin Nephrol 2002; 22: 3–16.
Nejatizadeh A, Kumar R, Stobdan T, Goyal AK, Sikdar S, Gupta M, Javed S, Qadar Pasha MA . Endothelial nitric oxide synthase gene haplotypes and circulating nitric oxide levels significantly associate with risk of essential hypertension. Free Radic Biol Med 2008; 44: 1912–1918.
Kumar R, Nejatizadeh A, Arif E, Akhtar S, Gupta M, Tyagi S, Goyal AK, Jain SK, Qadar Pasha MA . Multi-locus interactions of vascular homeostasis genes in essential hypertension: a gender-based study. Clin Chim Acta 2009; 405: 87–93.
Kumar R, Nejatizadeh A, Gupta M, Markan A, Tyagi S, Jain SK, Qadar Pasha MA . The epistasis between vascular homeostasis genes is apparent in essential Hypertension. Atherosclerosis 2012; 220: 418–424.
Kumar R, Kohli S, Mishra A, Garg R, Alam P, Stobdan T, Nejatizadeh A, Gupta M, Tyagi S, Pasha MA . Interaction between the genes of vasodilation pathways influence blood pressure and nitric oxide level in hypertension. Am J Hypertens 2014; 28: 239–247.
Acknowledgements
We highly appreciate the support and constant encouragement of Director, CSIR-Institute of Genomics and Integrative Biology, Delhi, and the staff at the Department of Cardiology, GB Pant Hospital, New Delhi, and SNM hospital, Leh, Jammu and Kashmir. The Council of Scientific and Industrial Research, India under the Taskforce BSC0122 supported this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on Hypertension Research website
Rights and permissions
About this article
Cite this article
Kumar, R., Kohli, S., Ali, Z. et al. CYBA (p22phox) variants associate with blood pressure and oxidative stress markers in hypertension: a replication study in populations of diverse altitudes. Hypertens Res 38, 498–506 (2015). https://doi.org/10.1038/hr.2015.31
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2015.31
Keywords
This article is cited by
-
Spatial transcriptomics reveals alterations in perivascular macrophage lipid metabolism in the onset of Wooden Breast myopathy in broiler chickens
Scientific Reports (2024)
-
Association between p22PHOX gene C242T polymorphism and hypertension in end-stage kidney disease patients
Journal of Human Hypertension (2021)
-
Associations of NADPH oxidase-related genes with blood pressure changes and incident hypertension: The GenSalt Study
Journal of Human Hypertension (2018)
-
Beneficial and harmful effects of exercise in hypertensive patients: the role of oxidative stress
Hypertension Research (2017)
-
Hypertension at high altitude: the interplay between genetic and biochemical factors in the setting of oxidative stress
Hypertension Research (2016)