Abstract
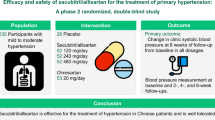
This 8-week, randomized, double-blind, parallel-group study compared the efficacy and safety of aliskiren with ramipril in Asian patients with mild to moderate hypertension. Following a 2- to 3-week placebo run-in period, patients with mean sitting diastolic blood pressure (msDBP) ⩾95 and <110 mm Hg were randomized to receive once daily dose of either aliskiren 75, 150, 300 mg or ramipril 5 mg for 8 weeks. Efficacy variables were the changes in msDBP and mean sitting systolic BP (msSBP) and BP control rates (<140/90 mm Hg). Safety was assessed by recording adverse events (AEs) and serious AEs (SAEs). Of 1316 randomized patients, 1160 (88.1%) completed the study. At the study endpoint, patients on aliskiren had greater mean BP reductions (14.39/11.63 mm Hg for 300 mg; 12.16/10.04 mm Hg for 150 mg; 12.24/10.66 mm Hg for 75 mg) than those on 5 mg ramipril (11.46/9.19 mm Hg). All aliskiren doses were statistically non-inferior (P<0.0001) to ramipril in reducing msDBP. The reduction in BP for aliskiren 300 mg was statistically superior vs. ramipril (P<0.002). Blood pressure control rates were higher for aliskiren (300 mg, 52.29%; 150 mg, 48.11%; 75 mg, 45.68%) than for ramipril (5 mg, 43.7%); the difference for aliskiren 300 mg vs. ramipril 5 mg was statistically significant (P<0.05). Aliskiren was well tolerated with a fourfold lower incidence of cough (0.6–1.2%) compared with ramipril (5.2%). SAEs were rare in this study (0.5%). Aliskiren produced greater BP reductions with a lower incidence of cough than ramipril in Asian patients with mild to moderate hypertension.
Similar content being viewed by others
Introduction
Despite advances in the diagnosis and treatment of hypertension, only about 5–33% of patients achieve blood pressure (BP) control (<140/90 mm Hg) globally. Blood pressure control rates for the Asian population range from 9.5 to 36.6%, and in China, the rates have been estimated to be as low as 9.5%. This is of particular concern because of the increasing prevalence of hypertension (15–35%) in the Asian populations.1, 2, 3, 4, 5, 6, 7 Of the many available antihypertensive drugs, angiotensin-converting enzyme inhibitors (ACEis) and angiotensin II receptor blockers that act on the renin angiotensin–aldosterone system form the mainstay of therapy today.2, 8 However, incomplete blockade of renin angiotensin–aldosterone system by these agents results in an increase in plasma renin activity and potentially limits the therapeutic benefits of these drugs.9 Moreover, ACE inhibition also results in suppression of kininase II, which may be followed by accumulation of the protussive mediators bradykinin and substance P in the upper respiratory tract or lungs. This results in undesirable adverse effects, such as dry cough, in susceptible individuals, leading to the discontinuation of therapy.10 Direct renin inhibitors, which act by inhibiting the activity of the enzyme renin, offer potential advantages over ACEis and angiotensin II receptor blockers. Aliskiren, the first in class of direct renin inhibitors, is approved for clinical use as an antihypertensive agent in the United States, Europe, Japan and China.11, 12 The efficacy, safety and tolerability of aliskiren have been well established in Caucasian and Japanese populations,11, 13, 14, 15, 16, 17, 18 but aliskiren has not been studied in Chinese hypertensive patients. Thus, the present study assessed the efficacy and safety of aliskiren compared with ramipril in a predominantly Chinese population with mild to moderate hypertension.
Methods
Study design
This was an 8-week, randomized, double-blind, active-controlled, parallel-group study conducted across multiple centers in China (25), Thailand (4) and India (7). The study included a 1-week washout period, a 2- to 3-week placebo run-in period and an 8-week, double-blind, active-controlled treatment period (Figure 1). Eligible patients were randomly allocated (1:1:1:1) to a once-daily treatment with one of the following regimens: 300, 150 and 75 mg aliskiren or 5 mg ramipril. Ramipril was selected as an active control because it is a widely used ACEi and has an established efficacy and safety profile.19 The ramipril dose (5 mg) used in the present study is the commonly prescribed dose for Chinese patients. The study was conducted according to good clinical practice guidelines and was in compliance with the Declaration of Helsinki (2002) Principles of the World Medical Association. The study protocol was reviewed by the appropriate institutional review board or ethical review committee for each study center, and all patients provided written informed consent before participating in the study.
Patients
Patients aged ⩾18 years with uncomplicated essential hypertension who fulfilled the following criteria were included in the study: (1) mean sitting diastolic BP (msDBP) ⩾90 and <110 mm Hg at the visit immediately before randomization; (2) msDBP ⩾95 and <110 mm Hg at the time of randomization; and (3) absolute difference of ⩽10 mm Hg in msDBP after the initial 2 weeks of single-blind placebo run-in period to the time of randomization. Patients with severe hypertension (msDBP ⩾110 mm Hg and/or msSBP ⩾180 mm Hg), history or evidence of secondary hypertension, known Keith–Wagener grade III or IV hypertensive retinopathy, hypertensive encephalopathy or cerebrovascular accident, transient ischemic cerebral attack within 12 months, severe cardiovascular disease including myocardial infarction, coronary bypass surgery, any percutaneous coronary intervention, Type 1 or Type 2 diabetes mellitus with glycosylated hemoglobin (HbA1c) >8% at washout period, or any surgical or medical condition that could alter the kinetics and bioavailability of the study drug were excluded from the study. Pregnant or nursing women were also excluded.
Efficacy assessments
The primary efficacy variable was the change in msDBP from baseline to week 8 endpoint. Secondary efficacy variables were the change in msSBP from baseline to week 8 endpoint, the proportion of patients achieving BP control (<140/90 mm Hg) and the proportion of patients achieving BP response (msDBP <90 mm Hg or reduction of ⩾10 mm Hg from baseline in msDBP). Post hoc analyses of the following efficacy variables were also performed: change in the pulse pressure (PP: msSBP−msDBP) and change in mean arterial pressure, MAP: (2 × msDBP + msSBP)/3 from baseline to week 8 endpoint.
Blood pressure measurements
Clinic BP measurements were recorded at all study visits (weeks 0, 2, 4 and 8) using a standard sphygmomanometer and appropriate arm cuff size in accordance with the 1988 American Heart Association Committee Report on Blood Pressure Determination. Sitting BP was measured at trough (24±3 h post dose) from the arm in which the highest sitting DBP was found at the first study visit. After the patient had been sitting for 5 min, three measurements of systolic and diastolic BP were taken at 1- to 2-min intervals, and the average of these was recorded as the mean value for that visit.
Safety assessments
Safety assessments consisted of monitoring and recording of all adverse events (AEs), serious AEs (SAEs) and laboratory tests and vital signs.
Statistical analysis
The primary efficacy variable (change in msDBP from baseline to week 8 endpoint) was used to demonstrate that aliskiren was non-inferior to ramipril. A sample size of 267 completed patients per treatment group was estimated, assuming a 10% dropout rate and a s.d. of 8 mm Hg. This would provide 90% power to detect (one-sided significance level of 0.025) a non-inferiority margin of 2.25 mm Hg between aliskiren and ramipril. If non-inferiority was established, the data was assessed for treatment superiority. The efficacy analyses were performed on the intent-to-treat population. In the case of missing data, the last measurement in the double-blind period was carried forward. Comparisons were made between aliskiren and ramipril for changes in msDBP and msSBP from baseline to week 8 endpoint using a one-way analysis of covariance model with treatment group and region as factors and baseline as a covariate. The proportion of patients achieving BP response and BP control were each compared using a logistic regression model with baseline msDBP as a covariate and treatment and region as factors. A post hoc analysis was performed on the intent-to-treat population to evaluate the treatment effect of aliskiren vs. ramipril on PP and MAP. Comparisons were made between aliskiren and ramipril for changes in PP and MAP from baseline to week 8 endpoint using a one-way analysis of covariance model with treatment group and region as factors and baseline as a covariate. The safety assessments were based primarily on the frequency of AEs, laboratory abnormalities and SAEs suspected to be study drug related.
Results
Patient demographics and baseline characteristics
A total of 1613 patients were enrolled for the study, of which 1316 (81.6%) completed the single-blind placebo run-in period, and were randomized to receive either aliskiren 300 mg (n=331), 150 mg (n=323), 75 mg (n=332) or ramipril 5 mg (n=330) (Figure 2). Of the randomized patients, 1160 (88.1%) completed the study. The main reasons for discontinuation were withdrawal of consent (n=62), AEs (n=47), unsatisfactory therapeutic effect (n=17), lost to follow-up (n=19), protocol deviation (n=7) and administrative problems (n=4) (Figure 2). Patient demographic and baseline characteristics were generally comparable across treatment groups, except for the duration of hypertension that varied from 7.9 to 9.4 years in the aliskiren-treated groups compared with the ramipril group (8.0 years). Patients were predominantly Chinese (87.2%), with a mean age of 53.2 years, a mean duration of hypertension of 8.6 years, a baseline msDBP of 98.8 mm Hg and a baseline msSBP of 147.9 mm Hg (Table 1).
Efficacy results
For the primary endpoint, the reductions in msDBP were greater in the aliskiren-treated groups than in the ramipril group at each time point (Figure 3a). The mean reductions in BP were evident by week 2, with further reductions at week 4, which were maintained until the end of the study (week 8). The least square mean reductions in msDBP from baseline to week 8 endpoint were 11.63, 10.04 and 10.66 mm Hg for aliskiren at doses of 300, 150 and 75 mg, respectively, vs. 5 mg ramipril (9.19 mm Hg). Pairwise comparisons showed that all doses of aliskiren were statistically non-inferior (P<0.0001) to ramipril (between-treatment difference: −2.44 (95% confidence interval: −3.63, −1.25); −0.86 (95% confidence interval: −2.06, 0.34); and −1.48 (95% confidence interval: −2.67, −0.28) for 300, 150 and 75 mg aliskiren, respectively) in reducing msDBP from baseline. Mean SBP reductions were greater in the aliskiren-treated groups than in the ramipril group at the week 8 endpoint (Figure 3b); however, only the between-treatment comparison between aliskiren 300 mg and ramipril 5 mg showed statistical significance. Aliskiren (300 mg) was statistically superior to 5 mg ramipril in reducing both msDBP (P<0.0001) and msSBP (P=0.0014) from baseline to week 8 endpoint. At the week 8 endpoint, the proportion of patients who had their BP controlled to <140/90 mm Hg was higher in all three aliskiren-treatment groups (300 mg, 52.29%; 150 mg, 48.11%; and 75 mg, 45.68%) compared with the 5 mg ramipril treatment group, 43.65% (Figure 4). The difference between aliskiren 300 mg and ramipril 5 mg was statistically significant (P=0.0177). Similarly, the BP responder rate was higher for each of the aliskiren doses (300 mg, 67.89%; 150 mg, 59.75%; and 75 mg, 59.57%) than for ramipril (53.87%), with the difference between aliskiren 300 mg and ramipril 5 mg being significant (P<0.0001). The least square mean changes in PP from baseline to week 8 endpoint were −2.69, −1.95 and −1.66 mm Hg for aliskiren 300, 150 and 75 mg, respectively, vs. ramipril (−2.19 mm Hg). The between treatment difference for changes from baseline in PP were −0.49, 0.25 and 0.53 mm Hg for 300, 150 and 75 mg aliskiren vs. ramipril, respectively.
The decrease in MAP was greater in the aliskiren treatment groups compared with ramipril treatment group. The least square mean changes in MAP from baseline to week 8 endpoint were −12.62, −10.74 and −11.12 mm Hg for 300, 150 and 75 mg aliskiren, respectively, (vs. −9.9 mm Hg for ramipril). Pairwise comparisons showed that the least square mean difference was significantly greater with aliskiren 300 mg compared with ramipril, but were comparable with 150 and 75 mg doses of aliskiren. Between treatment differences for all the three doses of aliskiren vs. ramipril were −2.63 (P<0.0001), −0.76 and −1.13 mm Hg for aliskiren 300, 150 and 75 mg, respectively.
Safety results
The overall incidence of AEs was similar among the treatment groups (Table 2). The majority of AEs were mild to moderate in severity. Overall, 8.9% of AEs were suspected to be study drug related, with a higher incidence in the ramipril treatment group (12.5%) than in the aliskiren-treated groups (6–8.7%). Dizziness (4.0%), headache (2.8%) and cough (2.0%) were the most commonly reported AEs. No incidence of hypotension (<100/60 mm Hg) was reported in the aliskiren-treatment groups, and only one patient in the ramipril group developed hypotension (0.3%). The incidence of cough was ∼fourfold higher (5.2%) in the ramipril (5 mg) group compared with the three aliskiren groups (0.6 to 1.2%). The overall rate of discontinuation because of AEs was 3.6%. Headache and dizziness were the most frequently reported AEs that led to discontinuation and were more frequently reported for patients treated with aliskiren. Cough led to discontinuation from the study, most frequently in the ramipril group. Cough-related discontinuations in the ramipril group were 1.2%, compared with 0.3% in each of the aliskiren groups (300 and 150 mg), and were more frequent in female (0.85%) than in male (0.14%) patients. No deaths were reported during the study, and only 0.5% (n=7) of patients experienced SAEs. All SAEs occurred in ⩽1 patient each: head injury and drug eruption occurred in aliskiren, 150 mg; chest pain, cerebral hemorrhage and medical device complication occurred in aliskiren 75 mg, varicose vein occurred in aliskiren 300 mg and hypertension in ramipril 5 mg group. Of the above SAE's, only the case of drug eruption (dermatitis medicamentosa) in the aliskiren 150 mg group was considered to be related to study medication.
Discussion
This study is the first to compare the antihypertensive efficacy and safety of the direct renin inhibitor aliskiren with that of the ACEi ramipril in Asian patients (predominantly Chinese) with essential hypertension. Aliskiren demonstrated greater reductions in BP with good tolerability compared with ramipril. Results from this study demonstrate that the reduction in msDBP was statistically non-inferior to ramipril for all doses of aliskiren, with numerically greater BP reductions for each of the doses. Aliskiren (300 mg) was statistically superior to ramipril in reducing both msDBP and msSBP from baseline to the week 8 endpoint. The proportions of patients achieving overall BP control (<140/90 mm Hg) and those responding to treatment were also greater in the aliskiren-treated groups than in the ramipril-treated group.
The mean BP reductions observed with the 300 and 150 mg doses of aliskiren in the present study are consistent with findings from previous studies conducted in the Caucasian and Japanese populations.11, 20, 21 The BP control rates and response to treatment showed a similar trend to that seen in Caucasian and Japanese patients,11, 16 suggesting that the response to aliskiren treatment does not differ significantly among racial/ethnic groups.
Interestingly, in the present study, the mean baseline systolic BP (147.6 mm Hg) was lower compared with that reported in previous studies performed in Caucasians and Japanese patients (systolic BP >151.0 mm Hg),11, 16, 20, 21 and the body mass index was lower (∼26.2 kg m−2) compared with that of Caucasians (∼30.3 kg m−2),16, 20 but similar to that of Japanese patients (25.5 kg m−2).11 However, these differences in baseline characteristics did not affect the BP response to treatment with aliskiren or BP control.
Despite the superior BP reductions observed with aliskiren 300 mg vs. ramipril 5 mg, the main limitation of the present study is the planned allocation of the study drugs wherein all three doses of aliskiren (300, 150 and 75 mg) are compared with only ramipril. In the present study, 5 mg ramipril was selected in the Asian (predominantly Chinese) population because it is the commonly prescribed dose in Chinese patients for treatment of essential hypertension. Furthermore, it was also reported that the incidence of dry cough due to ACEi's higher in Chinese patients.22, 23 The observed changes in PP and MAP indicate reductions in all treatment groups, but no significant treatment difference between aliskiren and ramipril, except in the case of aliskiren 300 mg for reduction in MAP where the difference compared with ramipril was superior.
Safety and tolerability are also key factors for the successful treatment of patients with essential hypertension. Overall, the tolerability seen in this study was consistent with the known profiles of the two drugs studied and was similar to that reported in previous studies conducted in Caucasian and Japanese patients.11, 15 Treatment with aliskiren was well tolerated, and the incidence of AEs was similar between the treatment groups. The use of ACEis is known to produce persistent dry cough in at least 5–35% of treated patients overall,10 but is even more prevalent in Chinese patients (44%) due to their genetic susceptibility.22, 23 Bradykinin-induced sensitization of airway sensory nerves is a potential mechanism of ACEi-induced cough.24 Results from this study show that the incidence of cough was fourfold lower with the maximum dose of aliskiren compared with ramipril, which can be attributed to the fact that treatment with aliskiren does not inhibit bradykinin degradation.
In conclusion, aliskiren demonstrated comparable or superior antihypertensive efficacy with a good tolerability profile compared with ramipril, making it an attractive treatment option for Asian patients with essential hypertension. The much lower incidence of cough with aliskiren treatment represents a potential added advantage in Asian patients, who are more susceptible to ACEi-induced cough.
References
Singh RB, Suh IL, Singh VP, Chaithiraphan S, Laothavorn P, Sy RG, Babilonia NA, Rahman AR, Sheikh S, Tomlinson B, Sarraf-Zadigan N . Hypertension and stroke in Asia: prevalence, control and strategies in developing countries for prevention. J Hum Hypertens 2000; 14: 749–763.
Brenner BM, Cooper ME, de Zeeuw D, Keane WF, Mitch WE, Parving HH, Remuzzi G, Snapinn SM, Zhang Z, Shahinfar S . Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: 861–869.
Whelton PK . Hypertension curriculum review: epidemiology and the prevention of hypertension. J Clin Hypertens (Greenwich) 2004; 6: 636–642.
Ong KL, Cheung BM, Man YB, Lau CP, Lam KS . Prevalence, awareness, treatment, and control of hypertension among United States adults 1999–2004. Hypertension 2007; 49: 69–75.
Writing group of 2010 Chinese Guidelines for the Management of Hypertension. 2010 Chinese guidelines for the management of hypertension. Chin J Cardiol 2011; 39: 579–616. [Article in Chinese].
Fujita T, Wu Z, Park J-B, Chen M-F . Briefings on JHS, CHS, KHS and THS guidelines and their difference from JNC VII and ESC/ESH. Int J Clin Pract 2006; 60 (Suppl 150): 3–7.
Aekplakorn W, Abbott-Klafter J, Khonputsa P, Tatsanavivat P, Chongsuvivatwong V, Chariyalertsak S, Sangwatanarojg S, Tiptaradolh S, Limb SS . Prevalence and management of prehypertension and hypertension by geographic regions of Thailand: the Third National Health Examination Survey, 2004. J Hypertens 2008; 26: 191–198.
Yusuf S, Sleight P, Pogue J, Bosch J, Davies R, Dagenais G . Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. N Engl J Med 2000; 342: 145–153.
Fleming I . Signaling by the angiotensin-converting enzyme. Circ Res 2006; 98: 887–896.
Dicpinigaitis PV . Angiotensin-converting enzyme inhibitor-induced cough: ACCP evidence-based clinical practice guidelines. Chest 2006; 129: 169S–173S.
Kushiro T, Itakura H, Abo Y, Gotou H, Terao S, Keefe DL . Aliskiren, a novel oral renin inhibitor, provides dose-dependent efficacy and placebo-like tolerability in Japanese patients with hypertension. Hypertens Res 2006; 29: 997–1005.
Chrysant SG . Aliskiren-hydrochlorothiazide combination for the treatment of hypertension. Expert Rev Cardiovasc Ther 2008; 6: 305–314.
Nussberger J, Wuerzner G, Jensen C, Brunner HR . Angiotensin II suppression in humans by the orally active renin inhibitor Aliskiren (SPP100): comparison with enalapril. Hypertension 2002; 39: E1–E8.
Stanton A, Jensen C, Nussberger J, O’Brien E . Blood pressure lowering in essential hypertension with an oral renin inhibitor, aliskiren. Hypertension 2003; 42: 1137–1143.
Gradman AH, Schmieder RE, Lins RL, Nussberger J, Chiang Y, Bedigian MP . Aliskiren, a novel orally effective renin inhibitor, provides dose-dependent antihypertensive efficacy and placebo-like tolerability in hypertensive patients. Circulation 2005; 111: 1012–1018.
Oh BH, Mitchell J, Herron JR, Chung J, Khan M Keefe DL . Aliskiren, an oral renin inhibitor, provides dose-dependent efficacy and sustained 24-h blood pressure control in patients with hypertension. J Am Coll Cardiol 2007; 49: 1157–1163.
Kushiro T, Itakura H, Abo Y, Gotou H, Terao S, Keefe DL . Long-term safety, tolerability, and antihypertensive efficacy of aliskiren, an oral direct renin inhibitor, in Japanese patients with hypertension. Hypertens Res 2009; 32: 169–175.
Schmieder RE, Philipp T, Guerediaga J, Gorostidi M, Smith B, Weissbach N, Maboudian M, Botha J, van Ingen H . Long-term antihypertensive efficacy and safety of the oral direct renin inhibitor aliskiren: a 12-month randomized, double-blind comparator trial with hydrochlorothiazide. Circulation 2009; 119: 417–425.
Wu N, Zhu J, Chen K . Tolerability of ramipril 10 mg/day in high-risk cardiovascular Chinese patients. Clin Drug Invest 2002; 22: 771–781.
Uresin Y, Taylor AA, Kilo C, Tschope D, Santonastaso M, Ibram GH, Fang H, Satlin A . Efficacy and safety of the direct renin inhibitor aliskiren and ramipril alone or in combination in patients with diabetes and hypertension. J Renin Angiotensin Aldosterone Syst 2007; 8: 190–198.
Andersen K, Weinberger MH, Egan B, Constance CM, Ali MA, Jin J, Keefe DL . Comparative efficacy and safety of aliskiren, an oral direct renin inhibitor, and ramipril in hypertension: a 6-month, randomized, double-blind trial. J Hypertens 2008; 26: 589–599.
Chan WK, Chan TY, Luk WK, Leung VK, Li TH, Critchley JA . A high incidence of cough in Chinese subjects treated with angiotensin converting enzyme inhibitors. Eur J Clin Pharmacol 1993; 44: 299–300.
Woo KS, Nicholls MG . High prevalence of persistent cough with angiotensin converting enzyme inhibitors in Chinese. Br J Clin Pharmacol 1995; 40: 141–144.
Mukae S, Aoki S, Itoh S, Iwata T, Ueda H, Katagiri T . Bradykinin B2 receptor gene polymorphism is associated with angiotensin-converting enzyme inhibitor-related cough. Hypertension 2000; 36: 127–131.
Acknowledgements
We thank the medical writers Lakshmi Deepa, PhD, and Ashish Agarwal, PhD (Novartis Healthcare India), for their assistance in drafting the manuscript and incorporating subsequent revisions. We also thank the clinical trial team for their expert collaboration as well as the staff of the centers involved in this work and the patients who participated in the study.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The content of this paper represents part of a registration study in China. The principal investigator, Professor Jun-Ren Zhu, was appointed independently by the regulatory authority SFDA, while the funding came from the sponsor, Novartis Pharma AG, Basel, Switzerland. The sponsor was involved in the design, analysis of the data and drafting of the manuscript. Professor Jun-Ren Zhu has received a research grant from Novartis Pharma AG, Basel, Switzerland. All authors analyzed the data reported here, and all authors contributed to and reviewed the final manuscript. Ruonan Wang and Ying-Mei Tu are employees of Beijing Novartis Pharma Co Ltd, Beijing, China. Shannon Ritter, and Deborah Keefe are employees of Novartis Pharmaceuticals Corporation, East Hanover, NJ, USA.
Appendix
Appendix
Trial investigators and sites

Rights and permissions
About this article
Cite this article
Zhu, JR., Sun, NL., Yang, K. et al. Efficacy and safety of aliskiren, a direct renin inhibitor, compared with ramipril in Asian patients with mild to moderate hypertension. Hypertens Res 35, 28–33 (2012). https://doi.org/10.1038/hr.2011.150
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2011.150
Keywords
This article is cited by
-
A randomized, double-blind, placebo-controlled, phase IIa, clinical study on investigating the efficacy and safety of SPH3127 tablet in patients with essential hypertension
Hypertension Research (2024)
-
The role of aliskiren in the management of hypertension and major cardiovascular outcomes: a systematic review and meta-analysis
Journal of Human Hypertension (2019)
-
Finding a place for aliskiren in the wide spectrum of blood pressure lowering agents
Hypertension Research (2012)