Abstract
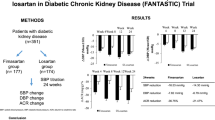
Efonidipine, a dihydropirydine calcium channel blocker, has been shown to dilate the efferent glomerular arterioles as effectively as the afferent arterioles. The present study compared the chronic effects of efonidipine and amlodipine on proteinuria in patients with chronic glomerulonephritis. The study subjects were 21 chronic glomerulonephritis patients presenting with spot proteinuria greater than 30 mg/dL and serum creatinine concentrations of ≤1.3 mg/dL in men or ≤1.1 mg/dL in women. All patients were receiving antihypertensive medication or had a blood pressure ≥130/85 mmHg. Efonidipine 20–60 mg twice daily and amlodipine 2.5–7.5 mg once daily were given for 4 months each in a random crossover manner. In both periods, calcium channel blockers were titrated when the BP exceeded 130/85 mmHg. Blood sampling and urinalysis were performed at the end of each treatment period. The average blood pressure was comparable between the efonidipine and the amlodipine periods (133±10/86±5 vs. 132±8/86±5 mmHg). Urinary protein excretion was significantly less in the efonidipine period than in the amlodipine period (1.7±1.5 vs. 2.0±1.6 g/g creatinine, p=0.04). Serum albumin was significantly higher in the efonidipine period than the amlodipine period (4.0±0.5 vs. 3.8±0.5 mEq/L, p=0.03). Glomerular filtration rate was not significantly different between the two periods. Plasma aldosterone was lower in the efonidipine period than in the amlodipine period (52±46 vs. 72±48 pg/mL, p=0.009). It may be concluded that efonidipine results in a greater reduction of plasma aldosterone and proteinuria than amlodipine, and that these effects occur by a mechanism independent of blood pressure reduction. A further large-scale clinical trial will be needed in order to apply the findings of this study to the treatment of patients with renal disease.
Similar content being viewed by others
Article PDF
References
Hostetter TH, Olson JL, Rennke HG, Venkatachalam MA, Brenner BM : Hyperfiltration in remnant nephrons: a potentially adverse response to renal ablation. Am J Physiol 1981; 241: F85–F93.
Brenner BM, Lawler EV, Mackenzie HS : The hyperfiltration theory: a paradigm shift in nephrology. Kidney Int 1996; 49: 1774–1777.
Remuzzi G, Perico N, Macia M, Ruggenenti P : The role of renin-angiotensin-aldosterone system in the progression of chronic kidney disease. Kidney Int Suppl 2005; 99: S57–S65.
Carmines PK, Mitchell KD, Navar LG : Effects of calcium antagonists on renal hemodynamics and glomerular function. Kidney Int Suppl 1992; 36: S43–S48.
Hayashi K, Ozawa Y, Fujiwara K, Wakino S, Kumagai H, Saruta T : Role of actions of calcium antagonists on efferent arterioles—with special references to glomerular hypertension. Am J Nephrol 2003; 23: 229–244.
Tanaka H, Shigenobu K : Pathophysiological significance of T-type Ca2+ channels: T-type Ca2+ channels and drug development. J Pharmacol Sci 2005; 99: 214–220.
Richard S : Vascular effects of calcium channel antagonists: new evidence. Drugs 2005; 65 ( Suppl 2): 1–10.
Sato A, Hayashi K, Saruta T : Antiproteinuric effects of mineralocorticoid receptor blockade in patients with chronic renal disease. Am J Hypertens 2005; 18: 44–49.
Imagawa K, Okayama S, Takaoka M, et al: Inhibitory effect of efonidipine on aldosterone synthesis and secretion in human adrenocarcinoma (H295R) cells. J Cardiovasc Pharmacol 2006; 47: 133–138.
Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The sixth report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Arch Intern Med 1997; 157: 2413–2446.
Cockcroft DW, Gault MH : Prediction of creatinine clearance from serum creatinine. Nephron 1976; 16: 31–41.
Peterson JC, Adler S, Burkart JM, et al: Blood pressure control, proteinuria, and the progression of renal disease. The Modification of Diet in Renal Disease Study. Ann Intern Med 1995; 123: 754–762.
Remuzzi G, Chiurchiu C, Ruggenenti P : Proteinuria predicting outcome in renal disease: nondiabetic nephropathies (REIN). Kidney Int Suppl 2004; 92: S90–S96.
de Zeeuw D, Remuzzi G, Parving HH, et al: Proteinuria, a target for renoprotection in patients with type 2 diabetic nephropathy: lessons from RENAAL. Kidney Int 2004; 65: 2309–2320.
Hunsicker LG, Atkins RC, Lewis JB, et al: Impact of irbesartan, blood pressure control, and proteinuria on renal outcomes in the Irbesartan Diabetic Nephropathy Trial. Kidney Int Suppl 2004; 92: S99–S101.
Abbate M, Benigni A, Bertani T, Remuzzi G : Nephrotoxicity of increased glomerular protein traffic. Nephrol Dial Transplant 1999; 14: 304–312.
Abbate M, Zoja C, Morigi M, et al: Transforming growth factor-beta1 is up-regulated by podocytes in response to excess intraglomerular passage of proteins: a central pathway in progressive glomerulosclerosis. Am J Pathol 2002; 161: 2179–2193.
Kannel WB, Stampfer MJ, Castelli WP, Verter J : The prognostic significance of proteinuria: the Framingham study. Am Heart J 1984; 108: 1347–1352.
Culleton BF, Larson MG, Parfrey PS, Kannel WB, Levy D : Proteinuria as a risk factor for cardiovascular disease and mortality in older people: a prospective study. Am J Med 2000; 109: 1–8.
Dykeman-Sharpe J : Proteinuria, a modifiable risk factor: angiotensin converting enzyme inhibitors (ACEIs) and angiotensin II receptor blockers (ARBs). CANNT J 2003; 13: 34–38.
Raij L : Recommendations for the management of special populations: renal disease in diabetes. Am J Hypertens 2003; 16: 46S–49S.
Ruggenenti P : Angiotensin-converting enzyme inhibition and angiotensin II antagonism in nondiabetic chronic nephropathies. Semin Nephrol 2004; 24: 158–167.
Okayama S, Imagawa K, Naya N, et al: Blocking T-type Ca2+ channels with efonidipine decreased plasma aldosterone concentration in healthy volunteers. Hypertens Res 2006; 29: 493–497.
Oshima T, Ozono R, Yano Y, et al: Beneficial effect of T-type calcium channel blockers on endothelial function in patients with essential hypertension. Hypertens Res 2005; 28: 889–894.
Ross R : Atherosclerosis—an inflammatory disease. N Engl J Med 1999; 340: 115–126.
Landmesser U, Hornig B, Drexler H : Endothelial function: a critical determinant in atherosclerosis? Circulation 2004; 109 ( Suppl 1): II27–II33.
Madamanchi NR, Vendrov A, Runge MS : Oxidative stress and vascular disease. Arterioscler Thromb Vasc Biol 2005; 25: 29–38.
Brewster UC, Setaro JF, Perazella MA : The renin-angiotensin-aldosterone system: cardiorenal effects and implications for renal and cardiovascular disease states. Am J Med Sci 2003; 326: 15–24.
Struthers AD, MacDonald TM : Review of aldosterone- and angiotensin II–induced target organ damage and prevention. Cardiovasc Res 2004; 61: 663–670.
Tonelli M, Wiebe N, Culleton B, et al: Chronic kidney disease and mortality risk: a systematic review. J Am Soc Nephrol 2006; 17: 2034–2047.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ishimitsu, T., Kameda, T., Akashiba, A. et al. Efonidipine Reduces Proteinuria and Plasma Aldosterone in Patients with Chronic Glomerulonephritis. Hypertens Res 30, 621–626 (2007). https://doi.org/10.1291/hypres.30.621
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.30.621
Keywords
This article is cited by
-
Ion-Channel modulator TH1177 reduces glomerular injury and serum creatinine in chronic mesangial proliferative disease in rats
BMC Nephrology (2020)
-
Blood pressure management in patients with type 2 diabetes mellitus
Hypertension Research (2017)
-
Clinical roles of calcium channel blockers in ischemic heart diseases
Hypertension Research (2017)
-
Dihydropyridine calcium channel blockers and renal disease
Hypertension Research (2017)
-
Chapter 5. Treatment with antihypertensive drugs
Hypertension Research (2014)