Abstract
Purpose: To compare colonoscopy screening/surveillance rates by level of risk for colorectal cancer based on age, personal history of adenomatous polyps or colorectal cancer, or family history of colorectal cancer.
Methods: Participants were aged 30–90 years, were seen within 5 years at Intermountain Healthcare, and had family history in the Utah Population Database. Colonoscopy rates were measured for those with/without risk factors.
Results: Among those aged 60–69 years, 48.4% had colonoscopy in the last 10 years, with rates declining after age 70 years. Percentages of those having had a colonoscopy in the last 10 years generally increased by risk level from 38.5% in those with a familial relative risk <1.0 to 47.6% in those with a familial relative risk >3.0. Compared with those with no family history, the odds ratio for being screened according to guidelines was higher for those with one first-degree relative diagnosed with colorectal cancer ≥ 60 years or two affected second-degree relatives (1.54, 95% confidence interval: 1.46–1.61) than those with one affected first-degree relative diagnosed <60 years or ≥2 affected first-degree relatives (1.25, 95% confidence interval: 1.14–1.37).
Conclusions: Compliance with colonoscopy guidelines was higher for those with familial risk but did not correspond with the degree of risk.
Similar content being viewed by others
Main
Colorectal cancer (CRC) is the second leading cause of cancer-related death in the United States. In 2010, it is estimated that 142,570 cases were diagnosed, and 51,370 deaths were caused by the disease.1 Having a positive family history such as a single affected first-degree relative essentially doubles an individual's risk for the disease.2–5 Other important risk factors for CRC include increasing age, and personal history of CRC, adenomatous polyps, or inflammatory bowel disease (IBD).1,6,7
CRC is often preventable through screening because precancerous polyps can be identified and removed.8,9 Findings from the National Polyp Study suggest that 76–90% of CRC occurrences could be prevented through periodic colonoscopy.2,10 Updated screening and surveillance guidelines were published in 2008–2009 by the US Preventive Services Task Force, the American College of Gastroenterology, the American Cancer Society, the Multi-Society Task Force on CRC, and the American College of Radiology.8,9,11,12 Although current guidelines support the use of fecal occult blood testing (FOBT) or flexible sigmoidoscopy as screening options for those at average risk, colonoscopy is considered to be more sensitive.13–15 Consequently, guidelines recommend colonoscopy as the screening/surveillance tool for those with significantly elevated risk arising from a personal history of adenomatous polyps, surgically resected CRC, IBD, or a family history of CRC. Based on the 2003 National Health Information Survey, percentages of men and women reporting colonoscopy (32.2% and 29.8%, respectively) were higher than those reporting FOBT (16.1% and 15.3%, respectively) or sigmoidoscopy (7.6% and 5.9%, respectively).16 Current practice trends confirm that physicians most frequently recommend colonoscopy rather than one of the other test options prescribed in the guidelines.17
Screening guidelines recommend that average-risk individuals begin screening at 50 years of age. According to data from the 2005 National Health Information Survey and the 2006 Behavioral Risk Factor Surveillance System, between 50% and 60% of adults aged 50 years or older reported having had an FOBT in the past year and/or endoscopy (colonoscopy or sigmoidoscopy) in the past 10 years.18,19 According to 2008 Behavioral Risk Factor Surveillance System data for the state of Utah where this study was conducted, 67.2% of individuals aged 50 years or older report having ever had endoscopy vs. 61.8% nationwide.20
Individuals who have undergone a surgical resection for CRC are at increased risk for a recurrence of CRC. Current surveillance guidelines recommend colonoscopy to be performed 1 year after resection based on reports of a high incidence of apparently metachronous second cancers (i.e., originating separately from the original cancer) within 2 years after resection.21 It has been reported that between 55% and 61.2% of patients have had ≥1 colonoscopy or other complete colon examination within 18 months after resection and between 52.4% and 73.6% have had ≥1 colonoscopy within 3 years after resection.22–25
For those with a family history of CRC or adenomatous polyps in first-degree relatives, it is recommended that screening start at age 40 years or 10 years before the earliest age of diagnosis of a family member diagnosed with CRC, whichever is younger, with follow-up screening every 5 years. Several studies have compared CRC screening rates (colonoscopy and/or FOBT) between persons with a positive family history and those without.26–31 In general, those with a positive family history of CRC were significantly more likely to be in compliance with screening recommendations compared with those without a family history. However, overall, the prevalence of screening was found to be low, and the majorities of both groups had not been screened. Limitations of these studies include small sample sizes, highly selected populations, self-reported family history, and most importantly, self-reported CRC screening. Only one study used an electronic medical record (EMR) for documentation of CRC screening.31 This study found that those with a positive family history were appropriately screened, based on risk-specific guidelines, less frequently than those with no family history of CRC. This may be due to the fact that screening guidelines are more stringent for those with a family history than those at average risk. Therefore, compliance rates among those at increased risk are lower than those at average risk because more screenings are recommended in shorter time frames, meaning that there are more opportunities to be out of compliance.
We previously reported a comprehensive set of familial relative risk estimates based on 2.3 million individuals in Utah with various constellations of first-, second-, and third-degree relatives affected with CRC.4 These estimates were produced using the Utah Population Database (UPDB), a population-based resource with a computerized genealogy linked to statewide cancer registry records. The UPDB was created in the early 1970s and contains genealogies for the original Utah pioneers (members of the Church of Jesus Christ of Latter-day Saints) and their modern-day descendants.32,33 A high proportion of Utah residents (approximately 60%) receive care through Intermountain Healthcare, an integrated healthcare system, and are represented in Intermountain electronic records. The UPDB resource and the linkage to Intermountain records have provided unprecedented opportunities for record-based research on cancer screening behavior in relationship to family history of cancer.
The objective of this study was to compare colonoscopy screening/surveillance rates among those with various levels of risk based on family history and other factors, in a large sample using electronic family history and EMR data. Using these risk factors linked to data on colonoscopy procedures performed, we measure the numbers in and out of compliance with adapted guidelines.
MATERIALS AND METHODS
The UPDB, described earlier, includes information for more than 7 million individuals, although not all have linked genealogical data.4,34 Cancer history information for these individuals is obtained from the Utah Cancer Registry (UCR; a National Cancer Institute Surveillance, Epidemiology, and End Results program registry since 1973) and death certificates. A linkage has been created between the UPDB and clinical records from Intermountain Healthcare; 3.2 million individuals have records in both sources.
Intermountain Healthcare is a community-owned, nonprofit healthcare system that serves the health needs of Utah and southeastern Idaho residents. Intermountain electronically integrates data for all aspects of care, including inpatient and outpatient clinical and administrative data for diagnoses, procedures, laboratory results, billing codes and information, and pathology reports.
The Resource for Genetic Epidemiology at the University of Utah governs access to the UPDB.35 The Resource for Genetic Epidemiology, University of Utah Institutional Review Board, and Intermountain Healthcare Institutional Review Board approvals were obtained to conduct this research.
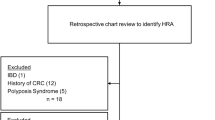
The individuals in this study were drawn from a pool of 357,208 CRC cases, matched controls (matched on age and sex), and relatives of cases and controls. Inclusion criteria for this study were (1) no record of death, (2) currently between the ages of 30 and 90 years, (3) part of ≥3 generations of Utah genealogy data and a descendant of original Utah pioneers, (4) seen as an inpatient or outpatient at Intermountain between December 2004 and December 2009, and (5) evidence of an Intermountain encounter 10 years previous to the most recent encounter. The encounter criteria help to exclude individuals who are not current Intermountain patients and those who have not been patients in the system long enough to adequately assess screening/surveillance compliance.
The following data were collected for study individuals (data source in parentheses): date of last colonoscopy (Intermountain inpatient and outpatient Current Procedural Terminology/Healthcare Common Procedure Coding System and International Classification of Diseases-9 procedure codes), diagnosis of CRC and surgical resection (Intermountain cancer registry), removal of an adenomatous polyp (contained in findings of pathology report), diagnosis of IBD (inpatient and outpatient International Classification of Diseases-9 codes and free text problem list entries), and dates of outpatient visits and inpatient hospital stays (Intermountain billing data). Numbers of first-, second-, and third-degree relatives affected with CRC were obtained from UPDB genealogy and UCR cancer data. Among individuals with cancer recorded in the UCR, 94% link to ≥1 records in the UPDB and 64.2% have family information. The type of relationship and age at diagnosis of affected relatives were also collected from the UPDB. The familial relative risk for each study individual was obtained by comparing their unique constellation of relatives affected with CRC, with familial relative risk estimates for various constellations previously published.4 An example of a family history constellation for a proband (considering CRC in the first- through third-degree relatives) is 0 affected first-degree relatives, one affected second-degree relative, and three affected third-degree relatives. Familial relative risk based on these extended constellations provides more quantitative and precise risk estimates than the guideline-based family history risk categories and is presented to provide an additional perspective on risk.
Although the total study population included individuals aged 30–90 years, we first evaluated the numbers of study individuals between 50 and 90 years of age who had evidence of colonoscopy in the past 10 years according to Intermountain data, stratified by age, risk factors, and also by familial relative risk level (e.g., <1.0, 1.0–1.99, 2.0–2.99, and >3.0). These numbers are irrespective of how long individuals have had risk factors or whether colonoscopies were for screening, surveillance, diagnostic, or treatment purposes because of the difficulty of distinguishing the reason for colonoscopy when using only coded data.
We also evaluated compliance with guidelines for those at normal risk or increased risk based on age, positive family history of CRC, a personal history of surgically resected CRC, or a personal history of adenomatous polyps.8 Study individuals aged 30–90 years with at least one risk factor were included. We used adapted guideline criteria (Table 1) to assign each individual to a status of compliant or not compliant with risk factor-specific CRC screening (age and family history) or surveillance (polyps or surgically resected CRC) guidelines using Intermountain colonoscopy data. Screening and surveillance guidelines from the American Cancer Society, the Multi-Society Task Force on CRC, and the American College of Radiology for individuals at high or increased risk were simplified based on authors' expert opinion to measure compliance in a practical way using available electronic sources of data. Additional time periods beyond those specified in the guidelines were provided to count colonoscopies that occurred shortly after the due date. For example, according to the guidelines those aged 50 years or older with no other risk factors are to be screened every 10 years. Eleven years were provided in our adaptation of the guideline to measure compliance to allow capture of procedures occurring within the 10th year. For those with a personal history of surgically resected CRC, only 1 year surveillance compliance (adapted as 18 months) was measured because of the complexity of screening intervals past the first postresection screening. Because of surgical resection data being available electronically before colonoscopy dates were available, individuals with resections earlier than 1994 were not included in the analysis. Compliance in those with IBD was also not assessed due to complexity; however, IBD diagnoses were used to exclude individuals from the group ≥50 years of age at “normal” risk (i.e., have no other risk factors considered in this analysis). Multivariate logistic regression was used to quantify the relative odds that individuals with each particular risk factor would be compliant with guidelines through colonoscopy, compared with those at normal risk, adjusting for age and sex.
RESULTS
Colonoscopy within the last 10 years among those aged 50–90 years
There were 71,446 individuals aged 50–90 years included in Table 2. Among other risk factors for CRC, 5836 (8.2%) had at least one adenoma documented and 2738 (3.8%) had a history of an advanced adenoma. Individuals with advanced adenoma (defined here as multiple adenomas, villous adenoma, or high-grade dysplasia) are a subset of those who are identified with an adenoma. Among those with ≥1 CRC affected first-degree relative, 8.7% had a first-degree relative diagnosed <50 years of age. There were 55,646 (77.9%) considered at normal risk, having no CRC, IBD, or adenoma and having 0 CRC affected first-degree relatives and ≤1 CRC affected second-degree relatives.
Evidence of colonoscopy in the last 10 years was found for 34.1% of individuals at normal risk and 57.8% of those with one or more risk factors. By age group, the percentage of individuals with colonoscopy within 10 years was highest in the 60–69 years age range (48.4%) and lowest in the 80–90 years age range (28.5%). Colonoscopy within the last 10 years was detected for most individuals with a history of CRC (65.7%), adenoma (83.9%), or advanced adenoma (93.9%). Regardless of risk defined by familial relative risk, the 60–69 years age group remained the group with the highest colonoscopy rates.
We evaluated evidence of colonoscopy in the last 10 years in this same sample aged 50–90 years according to familial relative risk level (Table 3). The most common risk category was familial relative risk <1.0 (77.2%). There were 16.9% with a familial relative risk between 1.0 and 1.99, 4.6% with a familial relative risk between 2.0 and 2.99, and 1.3% with a familial relative risk ≥3.0. Colonoscopy rates generally increased by risk level, from 38.5% in those with a familial relative risk <1.0 to 47.6% in those with a familial relative risk ≥3.0.
Screening/surveillance compliance rates using colonoscopy according to adapted guidelines
We summarized colonoscopy screening compliance (Table 4) in a sample at normal or increased risk according to criteria presented in Table 1. A total of 73,912 individuals aged 30 years or older with ≥1 risk factor were included in this analysis. Among 55,646 considered at normal risk, 35.0% underwent colonoscopy within the last 11 years. There were 529 with a history of a surgical resection for CRC ≥18 and ≤191 months ago, and among these, 40.1% had undergone colonoscopy within 18 months after the resection date. Among 1273 individuals with a history of adenoma documented ≥6 years ago, 58.4% had colonoscopy within 6 years after polypectomy. The higher set of criteria for increased risk based on a positive family history of CRC is “1 affected first-degree relative diagnosed <60 years or ≥2 first-degree relatives of any age.” For comparison with the view of risk presented in Table 3, individuals with ≥1 affected first-degree relative diagnosed <60 years of age would have a familial relative risk of 2.69 (95% confidence interval [CI]: 2.43–2.96), and for those with two first-degree relatives of any age, the familial relative risk is 3.01 (95% CI: 2.66–3.38). In the 2518 individuals aged 40 years or older meeting the criteria, 38.6% were compliant with the guideline within the last 6 years. For those younger than 40 years who met the criteria, 33.3% underwent colonoscopy within the last 6 years. The lower set of criteria for increased risk based on family history of CRC is “1 affected first-degree relative diagnosed ≥60 years or 2 affected second-degree relatives.” Once again, for comparison with Table 3, for those with ≥1 affected first-degree relative diagnosed ≥60 years, the familial relative risk is 1.99 (95% CI: 1.90–2.09), and for those with two affected second-degree relatives (in the absence of any affected first-degree relatives), the familial relative risk is 1.20 (95% CI: 1.05–1.38). Among the 9002 who met the increased risk criteria and who were also aged 40 years or older, 42.4% underwent colonoscopy within the last 10 years.
We estimated the relative odds that individuals with a particular risk factor would be compliant with guidelines specific to their risk level, compared with compliance in those at normal risk with their appropriate guidelines, taking into account age and sex (Table 4). The highest odds ratio (OR) was observed for those with a history of adenoma ≥6 years ago (2.57, 95% CI: 2.29–2.89), and the lowest was observed in those meeting the higher familial risk criteria (one CRC affected first-degree relative diagnosed <60 years or ≥2 first-degree relatives affected at any age; OR = 1.25, 95% CI: 1.14–1.37). All groups at higher risk had significant improvement in screening/surveillance compared with the referent group.
DISCUSSION
We report an analysis of colonoscopy rates in those with, and without, specific risk factors for CRC. Colonoscopy rates in the last 10 years in a sample of individuals aged 50–90 years are reported (Table 2). Almost half of individuals aged 60–69 years had evidence of colonoscopy in the last 10 years, which is consistent with national self-reported screening behavior statistics.18,19 Colonoscopy rates declined in those older than 70 years. Comparisons between differences in 10-year colonoscopy rates in those with and without risk factors in Table 2 should be interpreted with caution as some colonoscopies may be for surveillance (in those with surgically resected CRC or adenoma), others for screening, and others as part of diagnostic or treatment processes. Based on data presented in Table 3, it is clear that colonoscopy rates increase and then decline with age, peaking in the 60–69 years age range. Published guidelines recommend that individuals with a positive family history have more frequent screening, compared with those with no familial risk.8,11,12 Our analysis shows that although rates generally increase with familial relative risk level, indicating that a positive family history has some effect on screening behavior in this population, the increase does not reflect the increased frequency recommended by the guidelines. For example, <40% of those with one affected first-degree relative diagnosed <60 years or ≥2 first-degree relatives of any age had evidence of colonoscopy within the last 6 years. In those with one affected first-degree relative diagnosed ≥60 years or two affected second-degree relatives, the percentage with evidence of colonoscopy within the last 11 years was just >40%. Screening tests perform better in populations where the prior probability of having disease is higher. It would be expected that failure to comply with screening guidelines in populations at increased risk would have a disproportionate negative effect on CRC prevention. If higher priority were assigned to high-risk individuals out of compliance with screening, the impact on prevention could be increased with a more efficient outlay of scarce resources.
Colonoscopy rates are reported for a sample of individuals aged 30–90 years according to risk factor-specific screening recommendations adapted from well-accepted guidelines (Table 4). The rate of colonoscopies within 18 months after CRC surgical resection (40.1%) and accompanying OR for surveillance compliance compared with those at normal risk (1.27, 95% CI: 1.06–1.53) are lower than ideal. However, some patients with stage III and stage IV CRC may not have further surveillance after resection because cancer care is a higher priority. The colonoscopy rate within 6 years for those with polypectomy (58.4%) and the accompanying OR (2.57, 95% CI: 2.29–2.89) are higher but still leave room for improvement. Considering the influence of family history, the OR for the lower level of familial risk (1.54, 95% CI: 1.46–1.61) is higher than the OR for the higher level of risk (1.25, 95% CI: 1.14–1.37). Based on a logistic regression model comparing the higher level of family risk to the lower family risk and adjusting for age and sex, P = 0.025. This difference contradicts the assumption that those at higher risk would be screened more frequently. A central finding is that the highest levels of risk based on family history are not being screened according to the frequency specified by guidelines, and it is particularly concerning. Some studies have suggested that increased compliance with family history is observed, but in this large dataset, the opposite is observed. There does not seem to be a study design reason to explain this finding, and we believe it may well be real and should have impact on how physicians and others view family history in gaining screening compliance.
What could potentially explain why colonoscopy rates are not higher in those with risk factors, particularly a positive family history? First, although a systematic review found specificity for self-reported family history to be consistently high (>90%), sensitivity was lower and more variable (40–90%) depending on the cancer site.36 In addition, reporting accuracy was not as high with respect to extended relatives compared with the first degree. Second, at present, there are no standardized system-wide efforts within Intermountain to obtain and analyze family history and communicate risk to providers or patients. This lack of awareness of risk would interfere with appropriate application of risk-based screening guidelines. At least one study has shown an inverse correlation between the number of affected relatives and the accurate documentation of family history in the medical record by the provider.37 The implication is that a large family history requires more time to collect taking up an unacceptable amount of the visit. Finally, there may be a lack of provider awareness about the enhanced screening recommendations for those at high risk. Our study was unable to analyze the causes. In summary, colonoscopy rates within the last 10 years in those with risk factors for CRC, such as a previous diagnosis of CRC, adenoma, or a positive family history, were higher than those without these risk factors. Although colonoscopy rates in those with risk factors according to guidelines were higher compared with rates for those without the risk factors, efforts to improve compliance are still warranted.
An important limitation of this analysis is that we are unable to ascertain colonoscopies that were performed outside the Intermountain system, which may have led to underestimating screening rates by colonoscopy. The study attempted to mitigate this by identifying individuals who had been seen in the system recently and who also had evidence of being long-term users of the Intermountain system; however, this does not guarantee that all colonoscopies were performed within the system. Despite this limitation, the numbers of individuals in this study were sufficiently large that the results are nonetheless meaningful. Although overall screening rates may have been improved by considering other screening tests such as FOBT or sigmoidoscopy, our analysis focused exclusively on colonoscopy, as is recommended by the majority of the guidelines we used. Considering current practice trends and the fact that those with the risk factors considered in this study are more likely to undergo this procedure for screening/surveillance than other tests such as FOBT, we believe this is justified. In addition, we had concerns about completeness of FOBT and sigmoidoscopy data based on the fact that they are often performed in the outpatient setting and may not be as reliably documented electronically at Intermountain as colonoscopies. As previously noted, it was difficult to distinguish underlying reasons for colonoscopy. In terms of the potential for bias, this would tend to overstate compliance rates with guidelines. Screening and surveillance guidelines provide a recommendation for each risk factor separately, and this is how compliance was measured. Therefore, individuals with more than one risk factor (e.g., a family history of CRC and a personal history of the disease and resection) would be represented in more than one category in the analysis. Also, individuals with hereditary forms of the CRC such as Lynch syndrome have not been excluded from our dataset because it is difficult to reliably identify them. In a previous UPDB study, the number of individuals meeting the Amsterdam I criteria was estimated to be small (65/9458 cases or 0.7% of the cases), and none had colonic polyposis consistent with the familial adenomatous polyposis syndrome.38
This analysis of screening and surveillance behavior through colonoscopy addresses the limitations of similar studies including small sample sizes, highly selective populations, and self-reported family history and CRC screening. The quality and depth of electronically available data on colonoscopy and risk factors, and particularly the integration of electronic family history data and cancer registry data in this study are particular advantages contributing to this area of research.
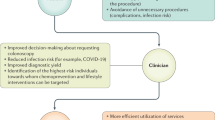
This study demonstrates the feasibility to use data from EMRs in combination with coded family history information to assess risk. This has the potential to provide point-of-care clinical decision support and “just in time” education to patients and providers. Future efforts are being directed to create a CRC family history risk algorithm within a patient-entered family history tool deployed in our electronic patient portal. Once deployed, this could allow combination of personal and family history risk factors and facilitate the delivery of individualized risk-based screening recommendations to both patients and providers, and the impact on compliance with recommended screening could be assessed.
REFERENCES
Jemal A, Siegel R, Xu J, Ward E . Cancer statistics, 2010. CA Cancer J Clin 2010; 60: 277–300.
Winawer S, Fletcher R, Rex D, et al. Colorectal cancer screening and surveillance: clinical guidelines and rationale—update based on new evidence. Gastroenterology 2003; 124: 544–560.
Lynch HT, de la Chapelle A . Hereditary colorectal cancer. N Engl J Med 2003; 348: 919–932.
Taylor DP, Burt RW, Williams MS, Haug PJ, Cannon-Albright LA . Population-based family history-specific risks for colorectal cancer: a constellation approach. Gastroenterology 2010; 138: 877–885.
Fuchs CS, Giovannucci EL, Colditz GA, Hunter DJ, Speizer FE, Willett WC . A prospective study of family history and the risk of colorectal cancer. N Engl J Med 1994; 331: 1669–1674.
Schatzkin A, Freedman LS, Dawsey SM, Lanza E . Interpreting precursor studies: what polyp trials tell us about large-bowel cancer. J Natl Cancer Inst 1994; 86: 1053–1057.
Bernstein CN, Blanchard JF, Kliewer E, Wajda A . Cancer risk in patients with inflammatory bowel disease: a population-based study. Cancer 2001; 91: 854–862.
Levin B, Lieberman DA, McFarland B, et al. Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US Multi-Society Task Force on Colorectal Cancer, and the American College of Radiology. Gastroenterology 2008; 134: 1570–1595.
Whitlock EP, Lin JS, Liles E, Beil TL, Fu R . Screening for colorectal cancer: a targeted, updated systematic review for the U.S. Preventive Services Task Force. Ann Intern Med 2008; 149: 638–658.
Winawer SJ, Zauber AG, Ho MN, et al. Prevention of colorectal cancer by colonoscopic polypectomy. The National Polyp Study Workgroup. N Engl J Med 1993; 329: 1977–1981.
U.S. Preventive Services Task Force. Screening for colorectal cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med 2008; 149: 627–637.
Rex DK, Johnson DA, Anderson JC, Schoenfeld PS, Burke CA, Inadomi JM . American College of Gastroenterology guidelines for colorectal cancer screening 2009 [corrected]. Am J Gastroenterol 2009; 104: 739–750.
Rockey DC, Paulson E, Niedzwiecki D, et al. Analysis of air contrast barium enema, computed tomographic colonography, and colonoscopy: prospective comparison. Lancet 2005; 365: 305–311.
Lieberman DA, Weiss DG, Bond JH, Ahnen DJ, Garewal H, Chejfec G . Use of colonoscopy to screen asymptomatic adults for colorectal cancer. Veterans Affairs Cooperative Study Group 380. N Engl J Med 2000; 343: 162–168.
Schoenfeld P, Cash B, Flood A, et al. Colonoscopic screening of average-risk women for colorectal neoplasia. N Engl J Med 2005; 352: 2061–2068.
Meissner HI, Breen N, Klabunde CN, Vernon SW . Patterns of colorectal cancer screening uptake among men and women in the United States. Cancer Epidemiol Biomarkers Prev 2006; 15: 389–394.
Klabunde CN, Lanier D, Nadel MR, McLeod C, Yuan G, Vernon SW . Colorectal cancer screening by primary care physicians: recommendations and practices, 2006–2007. Am J Prev Med 2009; 37: 8–16.
Shapiro JA, Seeff LC, Thompson TD, Nadel MR, Klabunde CN, Vernon SW . Colorectal cancer test use from the 2005 National Health Interview Survey. Cancer Epidemiol Biomarkers Prev 2008; 17: 1623–1630.
(CDC) CfDCaP. Use of colorectal cancer tests—United States, 2002, 2004, and 2006. MMWR Morb Mortal Wkly Rep 2008; 57: 253–258.
(CDC) CfDCaP. Behavioral risk factor surveillance system survey data. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2010.
Rex DK, Kahi CJ, Levin B, et al. Guidelines for colonoscopy surveillance after cancer resection: a consensus update by the American Cancer Society and the US Multi-Society Task Force on Colorectal Cancer. Gastroenterology 2006; 130: 1865–1871.
Elston Lafata J, Cole Johnson C, Ben-Menachem T, Morlock RJ . Sociodemographic differences in the receipt of colorectal cancer surveillance care following treatment with curative intent. Med Care 2001; 39: 361–372.
Elston Lafata J, Simpkins J, Schultz L, et al. Routine surveillance care after cancer treatment with curative intent. Med Care 2005; 43: 592–599.
Cooper GS, Yuan Z, Chak A, Rimm AA . Geographic and patient variation among Medicare beneficiaries in the use of follow-up testing after surgery for nonmetastatic colorectal carcinoma. Cancer 1999; 85: 2124–2131.
Cooper GS, Kou TD, Reynolds HL Jr . Receipt of guideline-recommended follow-up in older colorectal cancer survivors: a population-based analysis. Cancer 2008; 113: 2029–2037.
Clavel-Chapelon F, Joseph R, Goulard H . Surveillance behavior of women with a reported family history of colorectal cancer. Prev Med 1999; 28: 174–178.
Thrasher JF, Cummings KM, Michalek AM, Mahoney MC, Moysich KB, Pillittere DM . Colorectal cancer screening among individuals with and without a family history. J Public Health Manag Pract 2002; 8: 1–9.
Seeff LC, Nadel MR, Klabunde CN, et al. Patterns and predictors of colorectal cancer test use in the adult U.S. population. Cancer 2004; 100: 2093–2103.
Longacre AV, Cramer LD, Gross CP . Screening colonoscopy use among individuals at higher colorectal cancer risk. J Clin Gastroenterol 2006; 40: 490–496.
Murff HJ, Peterson NB, Greevy RA, Shrubsole MJ, Zheng W . Early initiation of colorectal cancer screening in individuals with affected first-degree relatives. J Gen Intern Med 2007; 22: 121–126.
Palmer RC, Emmons KM, Fletcher RH, et al. Familial risk and colorectal cancer screening health beliefs and attitudes in an insured population. Prev Med 2007; 45: 336–341.
Skolnick MH The Utah genealogical data base: a resource for genetic epidemiology. In: Cairns J, Lyon JL, Skolnick MH, editor, Banbury report no. 4: cancer incidence in defined populations. Cold Spring Harbor, NY: Cold Spring Harbor Laboratory, 1980; 285–297.
Skolnick MH . Prospects for population oncogenetics. In: Mulvihill JJ, Miller RW, Fraumeni JF, editors. Genetics of human cancer. New York: Raven Press, 1977; 19–25.
Cannon Albright LA . Utah family-based analysis: past, present and future. Hum Hered 2008; 65: 209–220.
Wylie JE, Mineau GP . Biomedical databases: protecting privacy and promoting research. Trends Biotechnol 2003; 21: 113–116.
Qureshi N, Wilson B, Santaguida P, et al. Family history and improving health. Evid Rep Technol Assess (Full Rep) 2009; 1–135.
Grover S, Stoffel EM, Bussone L, Tschoegl E, Syngal S . Physician assessment of family cancer history and referral for genetic evaluation in colorectal cancer patients. Clin Gastroenterol Hepatol 2004; 2: 813–819.
Maul JS, Warner NR, Kuwada SK, Burt RW, Cannon-Albright LA . Extracolonic cancers associated with hereditary nonpolyposis colorectal cancer in the Utah Population Database. Am J Gastroenterol 2006; 101: 1591–1596.
Acknowledgements
This research was supported by the Utah Cancer Registry, which is funded by contract N01-PC-35141 from the National Cancer Institute's Surveillance, Epidemiology, and End Results program with additional support from the Utah State Department of Health and the University of Utah. Partial support for all datasets within the Utah Population Database was provided by the University of Utah Huntsman Cancer Institute and the Huntsman Cancer Institute Cancer Center Support Grant, P30 CA42014 from the National Cancer Institute. Additional support was from R01, National Library of Medicine Grant LM009331 and the Huntsman Cancer Foundation (L.A.C.-A.), National Cancer Institute Grants R01-CA40641 and PO1-CA73992 (R.W.B.), and an Intermountain Healthcare, Homer Warner Center for Informatics Research Fellowship (D.P.T.).
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure: The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Taylor, D., Cannon-Albright, L., Sweeney, C. et al. Comparison of compliance for colorectal cancer screening and surveillance by colonoscopy based on risk. Genet Med 13, 737–743 (2011). https://doi.org/10.1097/GIM.0b013e3182180c71
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1097/GIM.0b013e3182180c71
Keywords
This article is cited by
-
Very-low-dose aspirin and surveillance colonoscopy is cost-effective in secondary prevention of colorectal cancer in individuals with advanced adenomas: network meta-analysis and cost-effectiveness analysis
BMC Gastroenterology (2021)
-
Imaging alternatives to colonoscopy: CT colonography and colon capsule. European Society of Gastrointestinal Endoscopy (ESGE) and European Society of Gastrointestinal and Abdominal Radiology (ESGAR) Guideline – Update 2020
European Radiology (2021)
-
Early detection of colorectal cancer based on presence of methylated syndecan-2 (SDC2) in stool DNA
Clinical Epigenetics (2019)
-
LC-MS-based lipid profile in colorectal cancer patients: TAGs are the main disturbed lipid markers of colorectal cancer progression
Analytical and Bioanalytical Chemistry (2019)
-
Clinical utility of a blood-based protein assay to increase screening of elevated-risk patients for colorectal cancer in the primary care setting
Journal of Cancer Research and Clinical Oncology (2017)