Abstract
Purpose
The purpose of this study was to investigate whether the genetic risk factors of age-related macular degeneration (AMD) are associated with the development of choroidal neovascularization (CNV) in highly myopic eyes of elderly Japanese.
Methods
Highly myopic elderly Japanese patients with and without CNV were genotyped for three AMD-associated single nucleotide polymorphisms (SNPs), namely rs10490924 (A69S) of ARMS2, rs11200638 of HTRA1, and rs1061170 (Y402H) of complement factor H (CFH), with the TaqMan SNP assay. One hundred and eighty-three unrelated highly myopic (axial lengths >26.00 mm or refractive errors >−6.0 diopters) Japanese patients with CNV who were ⩾50 years of age (mean age±standard deviation of 62.7±6.3 years) and 170 highly myopic patients without CNV who were ⩾50 years old (62.3±7.1 years) were studied. The differences in the genotypic distributions for the three SNPs between the two groups were tested with the Trend χ2 test, and logistic regression analyses were performed for age and gender adjustment.
Results
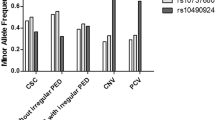
No significant difference was detected in the distribution of the three SNPs, rs10490924 (P>0.1), rs11200638 (P>0.1), and rs1061170 (P>0.5), between the two groups even after adjustments for age and gender differences.
Conclusion
The genetic risk factors of AMD related to these SNPs do not contribute significantly to the development of CNV in a highly myopic elderly Japanese population.
Similar content being viewed by others
Introduction
Choroidal neovascularization (CNV) is one of the most vision-threatening complications in highly myopic eyes. The pathogenesis of CNV in high myopia has not been fully determined. One important causative factor of CNV in highly myopic eyes is related to the excessive axial elongation of the eye, which results in the rupture of the Bruch membrane and atrophy of the choirocapillaries.1 Patchy chorioretinal atrophy and lacquer cracks are important predisposing findings for the development of CNV in highly myopic eyes.2 However, there are many highly myopic patients with these ocular predisposing findings who never develop CNV throughout life. This suggests that factors other than excessive axial elongation may also contribute to the development of CNV in these highly myopic eyes.
CNV is a complication common to high myopia and age-related macular degeneration (AMD).3 High myopia is the most common cause of CNV in patients younger than 50 years of age, whereas CNV can also develop in highly myopic eyes of the elderly population.4 In the elderly population, the most frequent cause of CNV is AMD; this raises a hypothesis that the processes involved in the aetiology of AMD may contribute to the development of CNV in highly myopic patients over the age of 50. AMD is caused by interactions of environmental and genetic factors, and it is believed that genetic factors contribute strongly to AMD.5, 6, 7 Thus, AMD-associated genetic factors may also be associated with the development of CNV in highly myopic eyes of elderly patients.
Among the genetic factors of AMD investigated, a single nucleotide polymorphism (SNP) rs1061170, which is also known as Y402H, of the complement factor H (CFH) gene on chromosome 1q32 has been shown in many studies to be a major AMD-associated polymorphism.8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19 More recently, two SNPs in the ARMS2(LOC387715)/HTRA1 region on chromosome 10q26, that is rs10490924 (also known as A69S) and rs11200638, were found in many studies to be strongly associated with AMD.14, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33 Fernandez-Robredo et al hypothesized that CNV associated with AMD and CNV associated with high myopia share a common genetic origin.34 This group analysed a possible association between two AMD-associated SNPs (rs1061170 and rs10490924) and CNV associated with high myopia in a Spanish population, and they did not find a significant association. However, the possible association in Asian populations remains to be elucidated.
To investigate the possible contribution of AMD genetic risk factors to CNV in elderly highly myopic Japanese, we analysed the association of these AMD-associated SNPs, namely rs10490924 (A69S) of ARMS2/LOC387715, rs11200638 of HTRA1, and rs1061170 (Y402H) of CFH, with the development of CNV in elderly Japanese patients with high myopia.
Materials and methods
All procedures used in this study conform to the tenets of the Declaration of Helsinki. The Institutional Review Board and the Ethics Committee of each institution approved the protocols used in this study. All of the patients were fully informed of the purpose and procedures, and a written consent was obtained from each patient.
Patients and controls
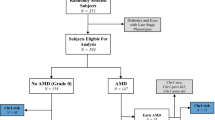
One hundred and eighty-three unrelated highly myopic Japanese patients with CNV (HM-CNV group) who were ⩾50 years of age (mean age±standard deviation (SD), 62.7±6.3 years; men:women, 23.5:76.5%) were recruited from Kyoto University Hospital, Tokyo Medical and Dental University Hospital, and Fukushima Medical University Hospital. The inclusion criteria were (1) axial lengths >26.00 mm or refractive errors >−6.0 diopters (D) in both eyes, (2) clinical presentation and angiographic manifestations of macular CNV in at least one eye, and (3) age ⩾50 years at their first visit with CNV to our institutes. Among the patients, 141 patients (77%) had monocular CNV and 42 patients (23%) had binocular CNV (an old CNV was present in the fellow eye). All of the patients underwent detailed ophthalmologic examinations, including dilated indirect and contact lens slit-lamp biomicroscopy, automatic objective refraction, measurement of the axial length by A-scan ultrasound (UD-6000, Tomey, Nagoya, Japan) or partial coherence interferometry (IOLMaster, Carl Zeiss Meditec, Dublin, CA, USA), colour fundus photography, optical coherence tomography, and fluorescein angiography. Individuals with a history of ocular surgery, with the exception of cataract surgery, were excluded. Patients with secondary choroidal neovascular diseases, such as angioid streaks, presumed ocular histoplasmosis syndrome, and ocular trauma, were also excluded. Even if patients with CNV had soft drusen in each of their eyes, they were not excluded from this study. However, there was only one highly myopic patient with CNV who also had soft drusen.
For control, 170 highly myopic (axial lengths >26.00 mm or refractive errors >−6.0 D in both eyes) Japanese cases who were ⩾50 years of age (62.3±7.1 years; men:women, 31.2:68.8%) without CNV were recruited from the same institutions (HM-control group). Subjects with soft drusen were excluded from the HM-control group.
For a population-based control (PB-control) group, 374 Japanese subjects (39.2±9.6 years; men:women, 50.8:49.2%) were randomly selected from the Pharma SNP Consortium. This healthy, population-based cohort had been recruited for earlier genomic studies and was considered to be representative of the general Japanese population.35 None of the subjects in this group had a history of any ocular diseases.
Genotyping
To investigate a possible association between CNV in highly myopic elderly patients and the genetic risk factors of AMD, we genotyped the three AMD-associated SNPs, namely rs10490924 (A69S) of ARMS2/LOC387715, rs11200638 of HTRA1, and rs1061170 (Y402H) of CFH, which have repeatedly been shown to be significantly associated with AMD.
Genomic DNA was prepared from the leucocytes of the peripheral blood using a DNA extraction kit (QuickGene-610L, Fujifilm, Minato, Tokyo, Japan). The public dbSNP database build 128 was used to extract the genotyping information for the SNPs. All of the SNPs were genotyped using Taqman SNP assays with the ABI PRISM 7700 system (Applied Biosystems, Foster City, CA, USA) according to the manufacturer's instructions.
Statistical analyses
The Hardy–Weinberg equilibrium (HWE) for the genotypic distribution was evaluated using the HWE-exact test for each group. Differences in the demographic features between the HM-CNV group and the HM-control group or the PB-control group were tested for statistical significance by the χ2 test for dichotomous data and by the Wilcoxon rank sum test for continuous data. Differences in the observed genotypic distribution between the HM-CNV group and the HM-control group were tested by the Trend χ2 test. Logistic regression analysis was performed for age and gender adjustments. These statistical analyses were performed using software R (http://www.r-project.org/).
The D' for pairwise linkage disequilibrium (LD) index between rs10490924 and rs11200638, both on chromosome 10q26, was calculated. Differences in the inferred haplotype frequencies between the HM-CNV group and the HM-control group were also examined by the χ2 test, and multiple testing correction for the P-value (Pc) was performed by the permutation test (number of iterations=10 000).36 Haplotype analyses were performed using the Haploview version 4.0.37
The single SNP analyses and the haplotype analyses between the HM-CNV group and the PB-control group were performed in the same way. The level of statistical significance was set at P<0.05 and Pc<0.05.
Results
The demographics of the study population are shown in Table 1. The HM-CNV group and the HM-control group were not age or gender matched, and the HM-control group was younger and had a higher male-to-female ratio than the HM-CNV group. However, these differences were not significant (P>0.1 for age and P>0.1 for gender). Both the HM-CNV group and the HM-control group were significantly older than the population-based control group because highly myopic patients ⩾50 years old were recruited and had lower male-to-female ratios because high myopia is a phenotype seen more frequently in women than in men.
The genotype counts, associations, and odds ratio (OR) for rs10490924, rs11200638, and rs1061170 in the HM-CNV group and the HM-control group are shown in Table 2. The distributions of the genotypes for the three SNPs were all in HWE (P>0.1). The differences in the genotypic distributions for the three SNPs between the HM-CNV group and the HM-control group were not statistically significant (P>0.1). After correcting for gender and age differences based on a logistic regression model by assuming an additive effect of each of the three SNPs, no new significant differences were found between the two groups. We performed a subset analysis on the 141 highly myopic cases with monocular CNV. Again, no significant differences were found in the genotypic distribution for these subjects (data not shown). To examine the effects of different age inclusion criteria, we also performed subset analyses on much older HM-CNV and HM control (⩾55, ⩾60, and ⩾65 years of age). However, no new significant differences were found in this study (data not shown).
In this study population, rs11200638 and rs10490924 were in strong LD (D'=0.97). The inferred haplotype frequencies in the HM-CNV group and the HM-control group are shown in Table 3. The haplotype frequencies were not significantly different between the HM-CNV group and the HM-control group after the multiple testing corrections. Haplotype analyses using the subset of cases with monocular CNV also did not show any significant differences even before the multiple testing correction (data not shown).
Single SNP analyses and haplotype analyses between the HM-CNV group and PB-control group for the three SNPs also showed no significant associations (data not shown).
We analysed the genotypic distributions for rs10490924, rs11200638, and rs1061170 in the pooled highly myopic cases (HM-CNV group+HM-control group) and compared them with the PB-control group to check for a possible difference in the genetic background for the three AMD-associated SNPs in the highly myopic population. The results are shown in Table 4. The distributions of the genotypes were all in HWE (P>0.1). There were no significant differences even after gender and age adjustment between the pooled highly myopic cases and the PB-control group.
Discussion
The results of this study showed that the genotypic distribution of three AMD-associated SNPs, rs11200638, rs10490924 and rs1061170, in highly myopic elderly Japanese patients with CNV did not differ significantly from that in highly myopic elderly Japanese without CNV. All of the highly myopic patients with binocular CNV in our study had an old CNV in the fellow eye at their first visit, suggesting that some of the patients might have had a CNV long before their first visit, that is they might have had a CNV before reaching 50 years of age. Thus, we analysed a subset of the HM-CNV group with monocular CNV, but still no significant differences were found in the distribution of the three SNPs. These results indicated that the molecular or cellular events that are related to these AMD-associated SNPs have little, or small if any, contribution to the development of CNV in highly myopic eyes of the elderly Japanese population.
CNV is a complication common to both high myopia and AMD.3 It can be difficult or impossible to distinguish between the CNV that is attributable to excessive axial elongation and the CNV that is attributable to the aetiology of the wet-type AMD in highly myopic eyes of the elderly.1 The important phenotypic hallmarks of AMD are soft drusen and pigment abnormalities in the macular area.38, 39, 40 In the highly myopic eyes of elderly patients, other characteristic changes typical of pathological myopia, for example chorioretinal atrophy, lacquer cracks, or posterior staphyloma, are often present.41 These degenerative changes make it difficult to determine, using ophthalmoscopic examinations, whether the hallmarks of AMD are present. Thus, we hypothesized that highly myopic patients who develop CNV after 50 years of age may have some contribution from the same genetic factors associated with AMD.
Recently, Fernandez-Robredo et al34 investigated a possible contribution of the two AMD-associated SNPs, rs1061170 (Y402H) and rs10490924 (A69S), to CNV associated with high myopia in a Spanish population >30 years of age. This group studied 100 patients with CNV associated with high myopia and 96 age-matched highly myopic controls without CNV. They did not find a significant difference in the genotypic distribution between the two groups for these AMD-associated SNPs. In this study, we focused on more elderly patients, that is ⩾50 years of age, with CNV in highly myopic eyes to maximize the detection power based on the hypothesis that the contribution by these AMD-associated SNPs to the development of CNV may be stronger in older patients. Our study in elderly myopic patients (183 HM-CNV cases and 170 HM controls) has an 80% power at an α-error of 0.05 for detection of an OR >1.88 when the risk allele frequency is 0.35 in the controls (rs10490924 and rs11200638) and an OR >3.19 when the control risk allele frequency is 0.05 (rs1061170). However, we did not find any significant differences.
Some case–control studies in the elderly and population-based epidemiological studies have reported that hypermetropia is one of the risk factors for early age-related maculopathy (early ARM) and/or late ARM (ie AMD).42, 43, 44, 45, 46, 47, 48 From the results of the Beijing Eye Study, Xu et al49 reported that the prevalence of both early and late ARM was significantly lower in the highly myopic group. We also analysed the differences in the genotypic distributions for the AMD-associated SNPs by the Trend χ2 test between the pooled elderly (⩾50 years old) highly myopic cases (HM-CNV group+HM-control group) and the PB-control group. The difference between the two groups was not significant. Although the recruitment of the highly myopic cases in our study was not population –based, but hospital based, these results suggest that the low prevalence of AMD in highly myopic cases cannot be explained simply by the difference of genetic background on the AMD-associated locus between highly myopic cases and the general population.
This study has some limitations. First, the age of the HM-CNV patients was recorded at the first visit. We did not know the exact time of the onset of the CNV, and there might have been an interval between the development of CNV and the examinations in some cases. This possibility is important in the cases with binocular CNV at their first consultation because old CNV was present in their fellow eyes. To reduce this bias, we performed a subset analysis on monocular CNV cases only. However, the results did not change. Second, the HM-CNV group and HM-control group were not age and gender matched. To minimize the possible influence of these differences, we performed age and gender adjustments using the logistic regression analysis and found no new significant associations. Third, the age range of the population-based control group in this study was significantly younger than that in the high myopia groups. Some of these young controls may develop axial elongation and may become ‘highly myopic’ in the future. Therefore, the case–control association analyses using these subjects tend to be statistically conservative. To circumvent the shortcomings, it will be important to perform a replication analysis using age-matched population-based controls.
In summary, our results show that the genotypic distribution of three AMD-associated SNPs (rs10490924 (A69S) of ARMS2/LOC387715, rs11200638 of HTRA1, and rs1061170 (Y402H) of CFH) in highly myopic elderly Japanese patients with CNV was not significantly different from that in highly myopic Japanese patients without CNV. These results indicate that these SNPs do not contribute significantly to the development of CNV in highly myopic eyes of the elderly Japanese population.
References
Soubrane G . Choroidal neovascularization in pathologic myopia: recent developments in diagnosis and treatment. Surv Ophthalmol 2008; 53: 121–138.
Ohno-Matsui K, Yoshida T, Futagami S, Yasuzumi K, Shimada N, Kojima A et al. Patchy atrophy and lacquer cracks predispose to the development of choroidal neovascularisation in pathological myopia. Br J Ophthalmol 2003; 87: 570–573.
Grossniklaus HE, Green WR . Choroidal neovascularization. Am J Ophthalmol 2004; 137: 496–503.
Cohen SY, Laroche A, Leguen Y, Soubrane G, Coscas GJ . Etiology of choroidal neovascularization in young patients. Ophthalmology 1996; 103: 1241–1244.
Haddad S, Chen CA, Santangelo SL, Seddon JM . The genetics of age-related macular degeneration: a review of progress to date. Surv Ophthalmol 2006; 51: 316–363.
Gorin MB . A clinician's view of the molecular genetics of age-related maculopathy. Arch Ophthalmol 2007; 125: 21–29.
Swaroop A, Branham KE, Chen W, Abecasis G . Genetic susceptibility to age-related macular degeneration: a paradigm for dissecting complex disease traits. Hum Mol Genet 2007; 16 (Spec No. 2): R174–R182.
Edwards AO, Ritter 3rd R, Abel KJ, Manning A, Panhuysen C, Farrer LA . Complement factor H polymorphism and age-related macular degeneration. Science 2005; 308: 421–424.
Hageman GS, Anderson DH, Johnson LV, Hancox LS, Taiber AJ, Hardisty LI et al. A common haplotype in the complement regulatory gene factor H (HF1/CFH) predisposes individuals to age-related macular degeneration. Proc Natl Acad Sci USA 2005; 102: 7227–7232.
Haines JL, Hauser MA, Schmidt S, Scott WK, Olson LM, Gallins P et al. Complement factor H variant increases the risk of age-related macular degeneration. Science 2005; 308: 419–421.
Klein RJ, Zeiss C, Chew EY, Tsai JY, Sackler RS, Haynes C et al. Complement factor H polymorphism in age-related macular degeneration. Science 2005; 308: 385–389.
Zareparsi S, Branham KE, Li M, Shah S, Klein RJ, Ott J et al. Strong association of the Y402H variant in complement factor H at 1q32 with susceptibility to age-related macular degeneration. Am J Hum Genet 2005; 77: 149–153.
Baird PN, Islam FM, Richardson AJ, Cain M, Hunt N, Guymer R . Analysis of the Y402H variant of the complement factor H gene in age-related macular degeneration. Invest Ophthalmol Vis Sci 2006; 47: 4194–4198.
Conley YP, Jakobsdottir J, Mah T, Weeks DE, Klein R, Kuller L et al. CFH, ELOVL4, PLEKHA1 and LOC387715 genes and susceptibility to age-related maculopathy: AREDS and CHS cohorts and meta-analyses. Hum Mol Genet 2006; 15: 3206–3218.
Lau LI, Chen SJ, Cheng CY, Yen MY, Lee FL, Lin MW et al. Association of the Y402H polymorphism in complement factor H gene and neovascular age-related macular degeneration in Chinese patients. Invest Ophthalmol Vis Sci 2006; 47: 3242–3246.
Magnusson KP, Duan S, Sigurdsson H, Petursson H, Yang Z, Zhao Y et al. CFH Y402H confers similar risk of soft drusen and both forms of advanced AMD. PLoS Med 2006; 3: e5.
Maller J, George S, Purcell S, Fagerness J, Altshuler D, Daly MJ et al. Common variation in three genes, including a noncoding variant in CFH, strongly influences risk of age-related macular degeneration. Nat Genet 2006; 38: 1055–1059.
Postel EA, Agarwal A, Caldwell J, Gallins P, Toth C, Schmidt S et al. Complement factor H increases risk for atrophic age-related macular degeneration. Ophthalmology 2006; 113: 1504–1507.
Seddon JM, Francis PJ, George S, Schultz DW, Rosner B, Klein ML . Association of CFH Y402H and LOC387715 A69S with progression of age-related macular degeneration. JAMA 2007; 297: 1793–1800.
Jakobsdottir J, Conley YP, Weeks DE, Mah TS, Ferrell RE, Gorin MB . Susceptibility genes for age-related maculopathy on chromosome 10q26. Am J Hum Genet 2005; 77: 389–407.
Rivera A, Fisher SA, Fritsche LG, Keilhauer CN, Lichtner P, Meitinger T et al. Hypothetical LOC387715 is a second major susceptibility gene for age-related macular degeneration, contributing independently of complement factor H to disease risk. Hum Mol Genet 2005; 14: 3227–3236.
Dewan A, Liu M, Hartman S, Zhang SS, Liu DT, Zhao C et al. HTRA1 promoter polymorphism in wet age-related macular degeneration. Science 2006; 314: 989–992.
Yang Z, Camp NJ, Sun H, Tong Z, Gibbs D, Cameron DJ et al. A variant of the HTRA1 gene increases susceptibility to age-related macular degeneration. Science 2006; 314: 992–993.
Cameron DJ, Yang Z, Gibbs D, Chen H, Kaminoh Y, Jorgensen A et al. HTRA1 variant confers similar risks to geographic atrophy and neovascular age-related macular degeneration. Cell Cycle 2007; 6: 1122–1125.
Fisher SA, Rivera A, Fritsche LG, Babadjanova G, Petrov S, Weber BH . Assessment of the contribution of CFH and chromosome 10q26 AMD susceptibility loci in a Russian population isolate. Br J Ophthalmol 2007; 91: 576–578.
Kanda A, Chen W, Othman M, Branham KE, Brooks M, Khanna R et al. A variant of mitochondrial protein LOC387715/ARMS2, not HTRA1, is strongly associated with age-related macular degeneration. Proc Natl Acad Sci USA 2007; 104: 16227–16232.
Kondo N, Honda S, Ishibashi K, Tsukahara Y, Negi A . LOC387715/HTRA1 variants in polypoidal choroidal vasculopathy and age-related macular degeneration in a Japanese population. Am J Ophthalmol 2007; 144: 608–612.
Leveziel N, Souied EH, Richard F, Barbu V, Zourdani A, Morineau G et al. PLEKHA1-LOC387715-HTRA1 polymorphisms and exudative age-related macular degeneration in the French population. Mol Vis 2007; 13: 2153–2159.
Lu F, Hu J, Zhao P, Lin Y, Yang Y, Liu X et al. HTRA1 variant increases risk to neovascular age-related macular degeneration in Chinese population. Vision Res 2007; 47: 3120–3123.
Mori K, Horie-Inoue K, Kohda M, Kawasaki I, Gehlbach PL, Awata T et al. Association of the HTRA1 gene variant with age-related macular degeneration in the Japanese population. J Hum Genet 2007; 52: 636–641.
Ross RJ, Bojanowski CM, Wang JJ, Chew EY, Rochtchina E, Ferris 3rd FL et al. The LOC387715 polymorphism and age-related macular degeneration: replication in three case-control samples. Invest Ophthalmol Vis Sci 2007; 48: 1128–1132.
Tanimoto S, Tamura H, Ue T, Yamane K, Maruyama H, Kawakami H et al. A polymorphism of LOC387715 gene is associated with age-related macular degeneration in the Japanese population. Neurosci Lett 2007; 414: 71–74.
Yoshida T, DeWan A, Zhang H, Sakamoto R, Okamoto H, Minami M et al. HTRA1 promoter polymorphism predisposes Japanese to age-related macular degeneration. Mol Vis 2007; 13: 545–548.
Fernandez-Robredo P, Maestre SR, Zarranz-Ventura J, Mulero HH, Salinas-Alaman A, Garcia-Layana A . Myopic choroidal neovascularization genetics. Ophthalmology 2008; 115: 1632, 1632 e1.
Gushima H . Pharma SNP Consortium (PSC). Research on Pharmacokinetics related Genetic Polymorphism among Japanese Population. Xenobiotic Metab and Dispos 2001; 16: 340–345.
Pesarin F . Multivariate Permutation Tests: With Applications in Biostatistics. Wiley-Blackwell: Chichester, UK, 2001.
Barrett JC, Fry B, Maller J, Daly MJ . Haploview: analysis and visualization of LD and haplotype maps. Bioinformatics 2005; 21: 263–265.
Bird AC, Bressler NM, Bressler SB, Chisholm IH, Coscas G, Davis MD et al. An international classification and grading system for age-related maculopathy and age-related macular degeneration. The International ARM Epidemiological Study Group. Surv Ophthalmol 1995; 39: 367–374.
Age-Related Eye Disease Study Research Group. The Age-Related Eye Disease Study system for classifying age-related macular degeneration from stereoscopic color fundus photographs: the Age-Related Eye Disease Study Report Number 6. Am J Ophthalmol 2001; 132: 668–681.
Klein R, Peto T, Bird A, Vannewkirk MR . The epidemiology of age-related macular degeneration. Am J Ophthalmol 2004; 137: 486–495.
Curtin BJ, Karlin DB . Axial length measurements and fundus changes of the myopic eye. I. The posterior fundus. Trans Am Ophthalmol Soc 1970; 68: 312–334.
The Eye Disease Case-Control Study Group. Risk factors for neovascular age-related macular degeneration. Arch Ophthalmol 1992; 110: 1701–1708.
Sandberg MA, Tolentino MJ, Miller S, Berson EL, Gaudio AR . Hyperopia and neovascularization in age-related macular degeneration. Ophthalmology 1993; 100: 1009–1013.
Chaine G, Hullo A, Sahel J, Soubrane G, Espinasse-Berrod MA, Schutz D et al. Case-control study of the risk factors for age related macular degeneration. France-DMLA Study Group. Br J Ophthalmol 1998; 82: 996–1002.
Wang JJ, Mitchell P, Smith W . Refractive error and age-related maculopathy: the Blue Mountains Eye Study. Invest Ophthalmol Vis Sci 1998; 39: 2167–2171.
Age-Related Eye Disease Study Research Group. Risk factors associated with age-related macular degeneration. A case-control study in the age-related eye disease study: Age-Related Eye Disease Study Report Number 3. Ophthalmology 2000; 107: 2224–2232.
Ikram MK, van Leeuwen R, Vingerling JR, Hofman A, de Jong PT . Relationship between refraction and prevalent as well as incident age-related maculopathy: the Rotterdam Study. Invest Ophthalmol Vis Sci 2003; 44: 3778–3782.
Xu L, Li Y, Zheng Y, Jonas JB . Associated factors for age related maculopathy in the adult population in China: the Beijing eye study. Br J Ophthalmol 2006; 90: 1087–1090.
Xu L, Li Y, Wang S, Wang Y, Wang Y, Jonas JB . Characteristics of highly myopic eyes: the Beijing Eye Study. Ophthalmology 2007; 114: 121–126.
Acknowledgements
The study was supported in part by the Ministry of Education, Culture, Sports, Science ,and Technology of Japan and by the Japanese National Society for the Prevention of Blindness.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Nakanishi, H., Gotoh, N., Yamada, R. et al. ARMS2/HTRA1 and CFH polymorphisms are not associated with choroidal neovascularization in highly myopic eyes of the elderly Japanese population. Eye 24, 1078–1084 (2010). https://doi.org/10.1038/eye.2009.215
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2009.215