Abstract
Purpose/Method To determine the patterns of referral, the hospital-based management and the subjective degree of visual success achieved by keratoconics attending the Corneal Service at Sunderland Eye Infirmary, England, a specifically designed anonymous questionnaire was mailed to 160 keratoconus subjects.
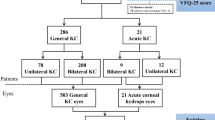
Results The following responses were obtained from 97 (61%) respondents: mean age of first referral (22.88 ± 8.36 years); gender (male:female ratio 3:1); source of initial referral (optometrists 90%); visual symptoms experienced before referral (46% complained of blurred/distorted vision); and the type of visual correction before referral (70% wore a refractive correction: 72% spectacles, 28% contact lenses). Initial post-referral treatment included bilateral contact lens fitting (65%), monocular contact lens correction (26%), penetrating keratoplasty (8%) and no intervention (1%). Two-thirds of subjects were presently wearing contact lenses (67%), with the mean period of successful lens wear being 8.26 ± 7.92 years, and 31% had undergone penetrating keratoplasty (PK) since initial referral. A subjective evaluation of visual acuity with contact lenses was made by respondents using a visual analogue scale. The mean value was 86.86 ± 15.25 (range 50-100 mm), with 50 mm representing moderate visual acuity. Of those who underwent PK the mean subjective evaluation of the change in post-operative vision compared with pre-operatively was 82.41 ± 26.57 (range 1-100 mm), with 50 mm representing no visual change. The majority of subjects therefore noted a moderate to marked visual improvement following PK.
Conclusion In this fairly young group of patients, predominantly male, the majority wore a refractive correction for approximately 10 years before referral to the Hospital Eye Service (HES). Most referrals were initiated by optometrists. On initial HES assessment the treatment for two-thirds was bilateral contact lens fitting; only a quarter were fitted monocularly. However, by the time of this study only a tenth retained monocular contact lens correction, with the mean length of time from diagnosis to bilateral contact lens wearing being approximately 5½ years. The progressive nature of this disease is further evidenced by the large number of contact lens sets required by patients (approximately 5) and by the number of patients (n = 22) requiring PK, the mean length of time from diagnosis to corneal graft being approximately 8½ years.
Similar content being viewed by others
Article PDF
References
Zadnik K . Keratoconus. In: Bennett ES, Weissman BA, editors. Clinical contact lens practice. Philadelphia: Lippincott, 1993:1–10.
Carlson DW, Green RP . The career impact of keratoconus on Air Force aviators. Am J Ophthalmol 1991;112:557–61.
Kennedy RH, Bourne WM, Dyer JA . A 48 year clinical and epidemiologic study of keratoconus. Am J Ophthalmol 1986;101:267–73.
Rabinowitz YS, Nesburn AB, McDonnell PJ . Videokeratography of the fellow eye in unilateral keratoconus. Ophthalmology 1993;100:181–6.
McCormack HM, Home DJ, Sheather S . Clinical applications of visual analogue scales: a critical review. Psychol Med 1988;18:1007–19.
Ridley F . Eye rubbing and contact lenses. Br J Ophthalmol 1961;45:631.
Gretz DC, McDonnell PJ . Keratoconus and ocular massage. Am J Ophthalmol 1988;106:757–8.
Hall KGC . A comprehensive study of keratoconus. Br J Physiol Opt 1963;20:215–56.
Woodward EG . Contact lenses in abnormal ocular conditions. In: Stone J, Phillips AJ, editors. Contact lenses. London: Butterworth, 1989:748–57.
Woodward EG . Kerataconus: maternal age and social class. Br J Ophthalmol 1981;65:104–7.
Lee LR, Hirst LW, Readshaw G . Clinical detection of unilateral keratoconus. Aust NZ J Ophthalmol 1995;23:129–33.
Reinke AR . Keratoconus: a review of research and current fitting techniques: 1. Int Contact Lens Clin 1975;2:66–79.
Duke-Elder S . System of ophthalmology: disease of the outer eye. St Louis: CV Mosby, 1965:964–76.
Bennett ES . Keratoconus. In: Bennett ES, Grohe RM, editors. Rigid gas permeable contact lenses. New York: Professional Press Books, 1986:297–344.
Papas EB, Schultz BL . Repeatability and comparison of visual analogue and numerical rating scales in the assessment of visual quality. Ophthalmol Physiol Opt 1997;17:492–8.
Krachmer JH, Feder RS, Belin MW . Keratoconus and related noninflammatory corneal thinning disorders. Surv Ophthalmol 1984;28:293–322.
Burger DS . Keratoconus: etiology, diagnosis and management. Practical Optom 1991;4:121–9.
Baum J . On the location of the cone and the etiology of keratoconus. Cornea 1995;14:142–3.
Karseras AG, Ruben M . Aetiology of keratoconus. Br J Ophthalmol 1976;60:522–5.
Thalasselis A . Thalesselis syndrome and genetic theories on keratoconus. J Am Optom Assoc 1995;66:495–9.
Gonzalez V, McDonnell PJ . Computer-assisted corneal topography in parents of patients with keratoconus. Arch Ophthalmol 1992;110:1413–4.
Salabert D, Cochener B, Mage F, Colin J . Keratoconus and familial topographic corneal anomalies. J Fr Ophtalmol 1994;17:646–56.
Rabinowitz YS, Maumenee IH, Lundergan MK, et al. Molecular genetic analysis in autosomal dominant keratoconus. Cornea 1992;11:302–8.
Rabinowitz YS, Garbus J, McDonnell PJ . Computer-assisted corneal topography in family members of patients with keratoconus. Arch Ophthalmol 1990;108:365–71.
Rahi A, Davies P, Ruben M, et al. Keratoconus and coexisting atopic disease. Br J Ophthalmol 1977;61:761–4.
Gasset AR, Hinson WA, Frias JL . Keratoconus and atopic diseases. Ann Ophthalmol 1978;10:991–4.
Gasset AR, Houde WL, Garcia-Bengochea M . Hard contact lens wear as an environmental risk in keratoconus. Am J Ophthalmol 1978;85:339–42.
Nauheim JS, Perry HD . A clinicopathologic study of contact lens related keratoconus. Am J Ophthalmol 1985;100:543–6.
Mascai MS, Varley GA, Krachmer JH . Development of keratoconus after contact lens wear: patient characteristics. Arch Ophthalmol 1990;108:534–8.
Shovlin JP . Keratoconus in patients wearing rigid contact lenses. 1. A causal relationship. Int Contact Lens Clin 1990;17:302–3.
Edrington TB, Zadnik K, Barr JT . Keratoconus. Optorn Clin 1995;4:65–73.
Crews MJ, Driebe WT, Stern GA . The clinical management of keratoconus: a 6 year retrospective study. CLAO J 1994;20:194–7.
Tuft SJ, Moodaley LC, Gregory WM, et al. Prognostic factors for the progression of keratoconus. Ophthalmology 1994;101:439–47.
Leger F, Ndiaye PA, Williamson W, et al. Indications of penetrating keratoplasty from a histopathological study of 1129 corneal buttons. J Fr Ophtalmol 1995;18:331–7.
Sayegh FN, Ehlers N, Faran I . Evaluation of penetrating keratoplasty in keratoconus: nine years' follow up. Acta Ophthalmol (Copenh) 1988;66:400.
Sharif KW, Casey TA . Changing indications for penetrating keratoplasty, 1971-1990. Eye 1993;7:485–8.
The Australian Corneal Graft Registry 1990 to 1992 report. Aust NZ J Ophthalmol 1993;21:1–48.
Smiddy WE, Hamburg TR, Kracher GP, Stark WJ . Keratoconus: contact lens or keratoplasty? Ophthalmology 1988;95:487–92.
Dana MR, Putz JL, Viana MA, et al. Contact lens failure in keratoconus management. Ophthalmology 1992;99:1187.
Williams KA, Muehlberg SM, Lewis RF, Coster DJ . How successful is corneal transplantation? A report from the Australian Corneal Graft Registry. Eye 1995;9:219–27.
Vail A, Gore SM, Bradley BA, et al. Corneal graft survival and visual outcome: a multicentre study. Corneal transplant follow-up study collaborators. Ophthalmology 1994;101:120–7.
Bechrakis N, Blom ML, Stark WJ, Green WR . Recurrent keratoconus. Cornea 1994;13:73–7.
Mamalis N, Anderson CW, Kreisler KR, et al. Changing trends in the indications for penetrating keratoplasy. Arch Ophthalmol 1992;110:1409–11.
Author information
Authors and Affiliations
Additional information
We thank Bausch and Lomb (UK) for their financial support
Rights and permissions
About this article
Cite this article
Weed, K., McGhee, C. Referral patterns, treatment management and visual outcome in keratoconus. Eye 12, 663–668 (1998). https://doi.org/10.1038/eye.1998.165
Issue Date:
DOI: https://doi.org/10.1038/eye.1998.165
Keywords
This article is cited by
-
Comparing the ocular surface temperature and dry eye condition of keratoconus with normal eyes using infrared thermal imaging
International Ophthalmology (2023)
-
Complications of accelerated corneal collagen cross-linking: review of 2025 eyes
International Ophthalmology (2020)
-
Validation of rs2956540:G>C and rs3735520:G>A association with keratoconus in a population of European descent
European Journal of Human Genetics (2015)
-
Cost effectiveness of collagen crosslinking for progressive keratoconus in the UK NHS
Eye (2015)
-
The Dundee University Scottish Keratoconus study: demographics, corneal signs, associated diseases, and eye rubbing
Eye (2008)