Abstract
Familial benign hypocalciuric hypercalcaemia (FBHH) is a genetically heterogeneous disorder that consists of three designated types, FBHH1, FBHH2 and FBHH3, whose chromosomal locations are 3q21.1, 19p and 19q13, respectively. FBHH1 is caused by mutations of a calcium-sensing receptor (CaSR), but the abnormalities underlying FBHH2 and FBHH3 are unknown. FBHH3, also referred to as the Oklahoma variant (FBHHOk), has been mapped to a 12cM interval, flanked by D19S908 and D19S866. To refine the location of FBHH3, we pursued linkage studies using 24 polymorphic loci. Our results establish a linkage between FBHH3 and 17 of these loci, and indicate that FBHH3 is located in a 4.1 Mb region flanked centromerically by D19S112 and telomerically by rs245111, which in the syntenic region on mouse chromosome 7 contains four Casr-related sequences (Gprc2a-rss). However, human homologues of these Gprc2a-rss were not found and a comparative analysis of the 22.0 Mb human and 39.3 Mb mouse syntenic regions showed evolutionary conservation of two segments that were inverted with loss from the human genome of 11.6 Mb that contained the four Gprc2a-rss. Thus, FBHH3 cannot be attributed to Gprc2a-rss abnormalities. DNA sequence analysis of 12 other genes from the interval that were expressed in the parathyroids and/or kidneys did not detect any abnormalities, thereby indicating that these genes are unlikely to be the cause of FBHH3. The results of this study have refined the map location of FBHH3, which will facilitate the identification of another CaSR or a mediator of calcium homeostasis.
Similar content being viewed by others
Introduction
Familial benign hypocalciuric hypercalcaemia (FBHH), also referred to as familial hypocalciuric hypercalcaemia (FHH) or familial benign hypercalcaemia (FBH), is a heritable disorder of mineral homeostasis that is transmitted as an autosomal dominant trait with a high degree of penetrance.1, 2 FBHH is characterized biochemically by lifelong elevation of serum calcium concentrations and is associated with inappropriately low urinary calcium excretion and a normal or mildly elevated circulating parathyroid hormone (PTH) level.1, 2 Hypermagnesaemia is typically present. Individuals with FBHH are usually asymptomatic and the disorder is considered benign. However, chondrocalcinosis3 and pancreatitis4 occur in some adults, and some children suffer from neonatal severe hyperparathyroidism (NSHPT), which is a life-threatening disorder associated with severe hypercalcaemia, hypotonia, bone demineralization, fractures and respiratory distress.1, 5 FBHH and NSHPT in most families is caused by loss-of-function mutations of the gene encoding the calcium-sensing receptor (CaSR) located on chromosome 3q21.1.5, 6, 7 FBHH individuals are heterozygous for the CaSR mutations, and the NSHPT patients may either be homozygous or heterozygous for the CaSR mutations, or have de novo heterozygous CaSR mutations.1, 5
The human CaSR is a 1078 amino acid cell surface protein that is expressed predominantly in the parathyroids and kidneys, where it allows the regulation of PTH secretion and renal calcium reabsorption appropriate to the prevailing extracellular calcium ([Ca2+]o) concentration.1 The CaSR is a member of family C of the superfamily of G-protein-coupled receptors (GPCRs) that includes the metabotropic glutamate receptors, V2R vomeronasal pheromone receptors, TAS1R taste receptors, γ-amino butyric acid (GABA-B) receptors and the GPRC6A orphan receptor.8 Ligand binding by the CaSR results in Gq/11-protein-dependent stimulation of phospholipase C (PLC) activity, causing the accumulation of inositol 1,4,5-triphosphate (IP3) and the rapid release of calcium ions from intracellular stores ([Ca2+]i), followed by an influx of [Ca2+]0.9 These intracellular events mediate a decrease in the rate of PTH secretion from the parathyroid chief cell and a reduction in renal tubular calcium reabsorption. Thus, the CaSR has a key role in the regulation of [Ca2+]0 homeostasis, with inactivating mutations resulting in hypocalciuric hypercalcaemia and activating mutations resulting in the opposite manifestations of hypercalciuria with hypocalcaemia.1, 2, 10, 11 In addition, CaSR activation through the Gi-protein stimulates the extracellular signal-regulated kinase (ERK)1/2 and the mitogen-activated protein (MAP) kinase cascade.12 These pathways may have a role in regulating parathyroid cell proliferation and it is interesting to note that some CaSR-inactivating mutations may be associated with primary hyperparathyroidism.13 However, loss-of-function mutations involving the 3234 bp coding region of the CaSR gene have been found in approximately two-thirds of FBHH patients.14 Thus, it appears that other mutations involving the non-coding regions of the CaSR, or mutations involving other receptors and mediators of calcium regulation, may occur in FBHH patients.
The identification of two other FBHH loci not at chromosome 3q21.1 indicates genetic heterogeneity and supports the possibility that there may be additional CaSRs or second messengers involved in calcium homeostasis. One of these FBHH loci has been mapped to chromosome 19p,15 and the other, which was identified in a kindred from Oklahoma and is referred to as the Oklahoma variant (FBHHOk),16 has been mapped to chromosome 19q13.17 These three genetically distinct types of FBHH have been designated as FBHH Type 1 (FBHH1, Mendelian Inheritance in Man (MIM) no. 145980), FBHH2 (MIM %145981) and FBHH3 (MIM %600740), with their chromosomal locations being 3q21.1, 19p and 19q13, respectively.6, 15, 17 The genes for FBHH2 and FBHH3 remain to be identified, and in the pursuit of this objective we have previously mapped FBHH3 (ie, FBHHOk) to an approximate 12 cM interval flanked centromerically by D19S908 and telomerically by D19S866 on chromosome 19q13.17 This interval is approximately 4.9 Mb in size and contains 179 genes.17 To identify the genetic defect causing FBHH3, we undertook three approaches: first, we aimed to delineate further the critical chromosome interval on 19q13 by the use of 24 polymorphic markers (17 microsatellite tandem repeats and 7 single-nucleotide polymorphisms, SNPs); second, we examined the critical interval and its syntenic region on mouse chromosome 7 for candidate genes; and third, we searched DNA sequence abnormalities in 12 candidate genes from the critical interval that were also expressed in the parathyroids and/or kidney.
Materials and methods
Patients
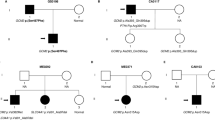
Forty members, from five generations, of the previously reported16, 17, 18 FBHHOk kindred were investigated. For these family members, the biochemical phenotype of FBHH was established16 by documenting hypercalcaemia associated with a low ratio (<0.01) of calcium clearance to creatinine clearance. Elevated concentrations of serum PTH had been observed in some affected individuals >30 years of age (II.2, II.4, II.6, II.9 and III.6, Figure 1). Three adults >40 years of age (II.4, II.9 and III.3) also showed evidence of osteomalacia. An individual taking anticonvulsants that may alter Ca2+ homeostasis, a man (IV.4) described previously16 as suffering from hypocalcaemia due to hypoparathyroidism, and five individuals who were normocalcaemic children of unaffected parents were excluded from the linkage study; the haplotypes of individual (IV.4) were determined but were not included for analysis at the FBHH3 locus. Thus, the 34 family members from five generations included for genetic analysis of the FBHH3 locus consisted of 19 affected members, 13 unaffected members and 2 unaffected spouses (Figure 1). Informed consent was obtained using protocols approved by the local and national ethics review committees.
Pedigree of family segregating for FBHHOk and chromosome 19q13 loci. The pedigree has been truncated, and the numerals identifying individuals have been altered from the original descriptions16, 18 to indicate those family members who yielded information for the localization of FBHHOk. In addition, the affected individuals IV.16 and V.1, who have become available for study since the previous report,17 are included. Squares indicate males, and circles indicate females. Unblackened symbols indicate unaffected individuals, and blackened symbols indicate affected individuals. The hatched square indicates an individual (IV.4) with idiopathic hypoparathyroidism who was excluded from the linkage analysis. The paternal haplotypes are on the left, and the maternal haplotypes are on the right. Deduced haplotypes are within parentheses. FBHHOK is segregating with the haplotype [3,5,3,3,7,6,3,4,5,3,3,6,3,1], defined by the loci listed to the left of the haplotypes of individual I.1 (eg, in the 16 affected individuals, II.4, II.6, II.9, III.6, III.9, III.13, III.17, III.18, IV.8, IV.10, IV.11, IV.13, IV.14, IV.15, IV.16 and V.1). Blackened bars indicate affected haplotypes, and unblackened bars indicate unaffected haplotypes. Recombinants (indicated by an asterisk – *) between FBHHOk and the loci listed were observed in individuals II.2, III.3 and III.4. The stippled region of the haplotype in individual III.4 indicates that the exact boundary of the recombinant could not be determined as the mother II.2 was homozygous at the loci (D19S745 and D19S412) involved. The region containing the FBHHOk gene is indicated between the arrows.
Genetic markers
Leukocyte DNA was prepared from venous blood samples by standard methods from 35 members (19 affected and 16 unaffected) of the five-generation FBHHOk kindred (Figure 1). Polymorphisms in 17 microsatellite tandem repeats were detected as previously described17, 18 using either fluorescently labelled primers (for the loci DM, D19S112, D19S745, gaat-p8371, D19S412, D19S219, D19S606, D19S902, D19S879 and D19S604) or radioactively (γ-ATP32) end-labelled primers (for the loci SULT2A1 (sulfotransferase family, cytosolic, 2A, dehydroepiandrosterone (DHEA)-preferring, member 1), GYS1 (glycogen synthase 1), HRC (histidine-rich calcium-binding protein), Rras, D19S317, D19S246 and KLK1 (kallikrein 1)).19, 20, 21, 22, 23 Seven SNPs (rs17660300, rs10411262, rs12611226, rs12463216, rs11667229, rs24511 and rs3097342) were detected by PCR and restriction endonuclease analysis in a subset of individuals, as previously reported.24 The order and genetic distances of these 24 polymorphic loci were deduced from published genetic maps19, 20, 21 and the order of loci was taken as 19cen – D19S219 – DM – D19S112 – D19S745 – rs17660300 – D19S412 – rs10411262 – D19S606 – SULT2A1 – D19S902 – rs12611226 – rs12463216 – GYS1 – rs11667229 – D19S879 – HRC – D19S604 – Rras – rs245111 – rs3097342 – D19S317 – D19S246 – KLK1 – gaatp8371 – 19qter.
Linkage analysis
The data from this and the previously reported study17 were pooled for linkage studies. The affected individuals IV.16 and V.I (Figure 1) have been recently ascertained and not previously reported.17 Conventional two-point LOD scores were calculated using the LINKAGE computer programs,17, 18 with the frequency and penetrance of FBHHOk set at 10−4 and 90%, respectively,17, 18 and a variation of these values had no significant effects on the results of the linkage analysis.
DNA sequence analysis
DNA from an FBHHOk-affected member and an unaffected unrelated individual was used with gene-specific primers (details available on request) for PCR amplification, as described.17 The DNA sequences of the PCR products were determined using methods as previously described.17 Reverse transcriptase-PCR (RT-PCR) using gene-specific primers was used to exclude any splicing abnormalities, using total RNA extracted from an Epstein–Barr virus-transformed lymphoblastoid cell line from one affected and one unrelated normal individual, as previously described.25
Comparative genome analysis
Searches were undertaken of the National Center for Biotechnology Information23 and Ensembl Bioinformatic databases.22 A database search with nucleotide sequence was performed using the BLAST algorithm. A comparative genome analysis of the FBHH3 candidate region on human chromosome 19q13 and syntenic region on mouse chromosome 7 was undertaken.
Results
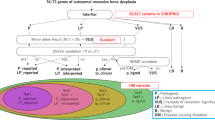
Fourteen of the 17 polymorphic microsatellite markers, whose order in the 12 cM region on chromosome 19q13 has been established as 19 cen – D19S219 – DM – D19S112 – D19S745 – D19S412 – D19S606 – D19S902 – D19S879 – HRC – D19S604 – Rras – D19S317 – D19S246 – gaatp 8371 – 19qter,19, 20, 21 proved to be informative in the FBHHOk family. Linkage between FBHHOk and 10 of the 14 polymorphic loci (Table 1) from chromosome 19q13 was established with the highest peak LOD score of 6.92, at 0% recombination, being observed between D19S606 and FBHHOk. These results confirm the previous localization of FBHHOk to this region.17 Analysis of individual recombinants (Figure 1) helped to refine the region containing the FBHHOk locus. The pedigree in Figure 1 shows 46 members (44 surviving and 2 deceased), from 5 generations, with data from 14 chromosome 19q13 microsatellite polymorphic loci. The haplotype of individual I.1, a deceased father, was ascertained by the examination of his four affected children (II.2, II.4, II.6 and II.9) and one unaffected son (II.7). His affected daughter, II.2, has inherited a recombinant haplotype that locates FBHHOk centromeric to D19S317, and this is confirmed further by the similar recombinants in her affected daughter, III.3. The affected son, III.4, has inherited a recombinant haplotype that locates FBHHOk telomeric to D19S112. The combined observations of the recombinants observed in II.2, III.3 and III.4, locate FBHHOk within the <10 cM interval flanked centromerically by D19S112 and telomerically by D19S317. A further analysis using seven SNPs located within this critical region in 11 key family members (Figure 2) revealed recombinants in individuals II.2, III.3 and III.4 that helped to map FBHHOk centromeric to rs245111. Thus, the FBHH3 was mapped to an interval flanked centromerically by D19S112 and telomerically by rs245111. This interval was found to be 4.1 Mb in size and to contain 135 protein-coding genes and 24 predicted genes.21, 22, 23 This human 19q13 region is syntenic to a region of mouse chromosome 7 that contains four GPCRs that have been referred to as Casr-related sequences as they have >30% identity and >50% homology at the amino-acid level to the human CaSR.26 These four Casr-related sequences,26 also known as Gprc2a-rs1, Gprc2a-rs2, Gprc2a-rs3 and Gprc2a-rs5, belong to family C of the GPCR genes and encode putative vomeronasal pheromone receptors.27 On the basis of the high degree of identity and homology with the human CaSR, these represented highly likely candidate genes for FBHH3. However, a bioinformatic (BLAST) analysis of the human 19q13 region did not identify the human, or primate, homologues of the Gprc2a-rs genes, thereby precluding their mutational analysis for FBHH3. The basis for the absence of these Gprc2a-rs genes in man was revealed by a comparative analysis of the human chromosome 19q13 and syntenic regions on mouse chromosome 7. This showed that although both regions had close homologies, they also had several differences, as follows (Figure 3). First, the centromeric-to-telomeric orientation of human chromosome 19q13 was reversed on mouse chromosome 7, as previously described.28 In addition, an 11.6 Mb region on mouse chromosome 7 that contains 35 murine genes including the four Gprc2a-rs was not present in the human genome (Figure 3). In mouse, this 11.6 Mb region lies within a 39.3 Mb segment in which the centromeric 25.1 Mb, situated between the Lig1 and Pop4 genes, and the telomeric 2.6 Mb, situated between the Siglec5 and Emp3 genes, are otherwise evolutionarily conserved. However, the mouse 25.1 Mb centromeric and 2.6 Mb telomeric portions are inverted in man. Thus, the syntenic region in man is 22.0 Mb in size and is situated between the POP4 and SIGLEC5 genes (Figure 3). The 4.1 Mb FBHH3 candidate interval is located within this 22.0 Mb region.
Pedigree of 11 individuals from the family segregating for FBHHOk, and chromosome 19q13 SNP loci. Symbols and identification codes by generation and location within the pedigree are as described in Figure 1. The paternal haplotypes are on the left, and the maternal haplotypes are on the right. Deduced haplotypes are within parentheses. FBHHOK is segregating with the haplotype [T,C,G,T,T,C,G]; eg, in four affected individuals I.1, II3, II.4 and II.5). Blackened bars indicate affected haplotypes, and unblackened bars indicate unaffected haplotypes. Recombinants (indicated by an asterisk – *) between FBHHOk and the loci listed were observed in individuals II.2 and III.3.
Comparison of the FBHH3 candidate interval on human chromosome 19q13.3 with the syntenic regions on mouse chromosome 7. Horizontal solid lines represent syntenic regions between the two species. Horizontal dashed lines indicate non-syntenic regions. Vertical arrows indicate the position of markers flanking the FBHH3 candidate region. Chromosomal locations of candidate genes for FBHH3 are shown (asterisked), as well as their mouse homologues. Genes at chromosomal break points are also indicated (†).
The absence of the four Gprc2a-rs genes from the human 19q13 region initiated a search for other candidate genes for FBHH3. Twelve of these were selected on the basis of their renal and/or parathyroid expression, as well as of a known or likely influence on GPCR-mediated signal transduction (Table 2), for prioritized DNA sequence analysis. These 12 genes encoded the following: a PTH-related protein known as PTH2;29 a prostacyclin GPCR known as PTGIR;30 a G-protein γ-subunit known as GNG8; an epithelial membrane protein known as EMP3 that has increased expression in parathyroid adenomas;31 a lipid kinase known as SPHK2 that inhibits cell growth and is activated by ERK1/2 phosphorylation;32 a Gq/11-protein-stimulated intracellular second messenger known as TULP2;33 a protein known as NUCB1 that binds to the Gi-protein and maintains a Ca2+ storage pool in the golgi;34 a protein known as HRC that has a key role in sarcoplasmic reticulum Ca2+ cycling;35 a putative cytosolic Ca2+-binding protein known as RCN3;36 a guanine nucleotide exchange factor known as CYTH2 that has a role in CaSR-induced cytoskeletal reorganization during chemotaxis;37 and a GTPase known as R-RAS that is activated by cyclic AMP and signals through nuclear factor-κB to modulate cell growth.38 DNA sequence analysis of the coding region and intron–exon boundaries of these 12 genes, from an individual affected with FBHHOk and from an unrelated normal individual, did not detect any abnormalities. In addition, RT-PCR excluded any splicing abnormalities, thereby indicating that these genes were unlikely to be responsible for FBHHOk.
Discussion
Our localization of the FBHH3 gene to a <10 cM region between D19S112 and rs245111 advances the search for this regulator of calcium homeostasis. The <10 cM interval containing FBHH3 is 4.1 Mbp in size, and contains 159 genes.21, 22, 23 This large number of genes is consistent with chromosome 19 having a higher gene density than any other human chromosome.21 The FBHH3 gene possibly encodes another CaSR or a mediator in the CaSR pathway. The report of four Gprc2a-rs located within the mouse syntenic region on chromosome 7,26 suggested that these were likely candidate genes for FBHH3. However, a BLAST analysis of the human 4.1 Mb critical region revealed that it did not contain any of these four Gprc2a-rs. The absence of these four Gprc2a-rs in the human chromosome 19q13 was explained by a comparative genome analysis of the human and mouse syntenic regions. This revealed that the FBHH3 candidate interval on chromosome 19q13 is located in a region that had undergone chromosomal rearrangements during evolution following the divergence of primate and rodent species. Of the 39.3 Mb mouse region, a total of 27.7 Mb, comprising a 2.6 Mb telomeric and 25.1 Mb centromeric region, was evolutionarily conserved in man (Figure 3). However, a murine 11.6 Mb region was not present in man, and this region contained the four Gprc2a-rs genes together with 31 other genes that are not present in man. Moreover, human chromosome 19 is known to have the highest break point density when compared with other human chromosomes,39 and the pronounced molecular divergence from rodents may explain the loss of the Casr-related sequences from the human genome during evolution. The absence of Gprc2a-rs genes within the critical FBHH3 interval led us to consider the possible involvement of other mediators in the CaSR pathway. The CaSR pathway, which begins with ligand binding by the CaSR, involves G-protein-dependent stimulation of PLC activity that causes an accumulation of IP3 and a rapid release of [Ca2+]i from intracellular stores, followed by an influx of [Ca2+]o.9 The intermediaries between CaSR activation, the elevation of [Ca2+]i, and the physiological response of a decrease in the rate of PTH secretion from the parathyroid cell and a reduction in renal tubular calcium reabsorption are likely to involve GTP-binding proteins and calcium-binding proteins that may be either calcium-dependent enzymes or calcium-dependent modulating proteins, and alterations in cyclic AMP and the MAP kinase cascade. Database searches of the 4.1 Mb interval containing FBHH3 on chromosome 19q13 revealed 12 candidate genes for FBHH3 that were considered to be components of GPCR-mediated signal transduction, and that were also expressed in the kidneys and/or parathyroid glands (Table 2). The absence of DNA sequence abnormalities in an individual with FBHH3 indicated that these 12 genes are unlikely to be involved in the aetiology of this disorder. Hence, other candidate genes need to be considered and similarly analyzed.
In summary, our results, locating FBHH3 to a <10 cM region that is 4.1 Mbp in size on human chromosome 19q13,21, 22, 23 have further delineated the interval for this disorder of calcium homeostasis. Furthermore, we have shown by comparative analysis that this region has undergone complex rearrangements during evolution that include the inversion of two conserved regions and a deletion of a 11.6 Mb region that contains 35 murine genes, including four Gprc2a-rs genes.
References
Chattopadhyay N, Brown EM : Role of calcium-sensing receptor in mineral ion metabolism and inherited disorders of calcium-sensing. Mol Genet Metab 2006; 89: 189–202.
Thakker RV : Diseases associated with the extracellular calcium-sensing receptor. Cell Calcium 2004; 35: 275–282.
Heath 3rd H : Familial benign (hypocalciuric) hypercalcemia. A troublesome mimic of mild primary hyperparathyroidism. Endocrinol Metab Clin North Am 1989; 18: 723–740.
Pearce SH, Wooding C, Davies M et al: Calcium-sensing receptor mutations in familial hypocalciuric hypercalcaemia with recurrent pancreatitis. Clin Endocrinol (Oxf) 1996; 45: 675–680.
Pollak MR, Brown EM, Chou YH et al: Mutations in the human Ca(2+)-sensing receptor gene cause familial hypocalciuric hypercalcemia and neonatal severe hyperparathyroidism. Cell 1993; 75: 1297–1303.
Chou YH, Brown EM, Levi T et al: The gene responsible for familial hypocalciuric hypercalcemia maps to chromosome 3q in four unrelated families. Nat Genet 1992; 1: 295–300.
Pearce SH, Bai M, Quinn SJ et al: Functional characterization of calcium-sensing receptor mutations expressed in human embryonic kidney cells. J Clin Invest 1996; 98: 1860–1866.
Bjarnadottir TK, Fredriksson R, Schioth HB : The gene repertoire and the common evolutionary history of glutamate, pheromone (V2R), taste(1) and other related G protein-coupled receptors. Gene 2005; 362: 70–84.
Hofer AM, Brown EM : Extracellular calcium sensing and signalling. Nat Rev Mol Cell Biol 2003; 4: 530–538.
Pollak MR, Brown EM, Estep HL et al: Autosomal dominant hypocalcaemia caused by a Ca(2+)-sensing receptor gene mutation. Nat Genet 1994; 8: 303–307.
Pearce SH, Williamson C, Kifor O et al: A familial syndrome of hypocalcemia with hypercalciuria due to mutations in the calcium-sensing receptor. N Engl J Med 1996; 335: 1115–1122.
Hobson SA, Wright J, Lee F et al: Activation of the MAP kinase cascade by exogenous calcium-sensing receptor. Mol Cell Endocrinol 2003; 200: 189–198.
Hannan FM, Nesbit MA, Christie PT et al: Familial isolated primary hyperparathyroidism caused by mutations of the MEN1 gene. Nat Clin Pract Endocrinol Metab 2008; 4: 53–58.
D’Souza-Li L, Yang B, Canaff L et al: Identification and functional characterization of novel calcium-sensing receptor mutations in familial hypocalciuric hypercalcemia and autosomal dominant hypocalcemia. J Clin Endocrinol Metab 2002; 87: 1309–1318.
Heath 3rd H, Jackson CE, Otterud B et al: Genetic linkage analysis in familial benign (hypocalciuric) hypercalcemia: evidence for locus heterogeneity. Am J Hum Genet 1993; 53: 193–200.
McMurtry CT, Schranck FW, Walkenhorst DA et al: Significant developmental elevation in serum parathyroid hormone levels in a large kindred with familial benign (hypocalciuric) hypercalcemia. Am J Med 1992; 93: 247–258.
Lloyd SE, Pannett AA, Dixon PH et al: Localization of familial benign hypercalcemia, Oklahoma variant (FBHOk), to chromosome 19q13. Am J Hum Genet 1999; 64: 189–195.
Trump D, Whyte MP, Wooding C et al: Linkage studies in a kindred from Oklahoma, with familial benign (hypocalciuric) hypercalcaemia (FBH) and developmental elevations in serum parathyroid hormone levels, indicate a third locus for FBH. Hum Genet 1995; 96: 183–187.
Ashworth LK, Batzer MA, Brandriff B et al: An integrated metric physical map of human chromosome 19. Nat Genet 1995; 11: 422–427.
Gyapay G, Morissette J, Vignal A et al: The 1993–94 Genethon human genetic linkage map. Nat Genet 1994; 7: 246–339.
Grimwood J, Gordon LA, Olsen A et al: The DNA sequence and biology of human chromosome 19. Nature 2004; 428: 529–535.
Flicek P, Aken BL, Beal K et al: Ensembl 2008. Nucleic Acids Res 2008; 36: D707–D714.
Wheeler DL, Barrett T, Benson DA et al: Database resources of the National Center for Biotechnology Information. Nucleic Acids Res 2008; 36: D13–D21.
Bowl MR, Nesbit MA, Harding B et al: An interstitial deletion-insertion involving chromosomes 2p25.3 and Xq27.1, near SOX3, causes X-linked recessive hypoparathyroidism. J Clin Invest 2005; 115: 2822–2831.
Parkinson DB, Thakker RV : A donor splice site mutation in the parathyroid hormone gene is associated with autosomal recessive hypoparathyroidism. Nat Genet 1992; 1: 149–152.
Hinson TK, Damodaran TV, Chen J et al: Identification of putative transmembrane receptor sequences homologous to the calcium-sensing G-protein-coupled receptor. Genomics 1997; 45: 279–289.
Yang H, Shi P, Zhang YP et al: Composition and evolution of the V2r vomeronasal receptor gene repertoire in mice and rats. Genomics 2005; 86: 306–315.
Stubbs L, Carver EA, Shannon ME et al: Detailed comparative map of human chromosome 19q and related regions of the mouse genome. Genomics 1996; 35: 499–508.
Sugimura Y, Murase T, Ishizaki S et al: Centrally administered tuberoinfundibular peptide of 39 residues inhibits arginine vasopressin release in conscious rats. Endocrinology 2003; 144: 2791–2796.
Stitham J, Arehart EJ, Gleim S et al: Arginine (CGC) codon targeting in the human prostacyclin receptor gene (PTGIR) and G-protein coupled receptors (GPCR). Gene 2007; 396: 180–187.
Forsberg L, Bjorck E, Hashemi J et al: Distinction in gene expression profiles demonstrated in parathyroid adenomas by high-density oligoarray technology. Eur J Endocrinol 2005; 152: 459–470.
Hait NC, Bellamy A, Milstien S et al: Sphingosine kinase type 2 activation by ERK-mediated phosphorylation. J Biol Chem 2007; 282: 12058–12065.
Carroll K, Gomez C, Shapiro L : Tubby proteins: the plot thickens. Nat Rev Mol Cell Biol 2004; 5: 55–63.
Lavoie C, Meerloo T, Lin P et al: Calnuc, an EF-hand Ca(2+)-binding protein, is stored and processed in the Golgi and secreted by the constitutive-like pathway in AtT20 cells. Mol Endocrinol 2002; 16: 2462–2474.
Arvanitis DA, Vafiadaki E, Fan GC et al: Histidine-rich Ca-binding protein interacts with sarcoplasmic reticulum Ca-ATPase. Am J Physiol Heart Circ Physiol 2007; 293: H1581–H1589.
Tsuji A, Kikuchi Y, Sato Y et al: A proteomic approach reveals transient association of reticulocalbin-3, a novel member of the CREC family, with the precursor of subtilisin-like proprotein convertase, PACE4. Biochem J 2006; 396: 51–59.
Bouschet T, Martin S, Kanamarlapudi V et al: The calcium-sensing receptor changes cell shape via a beta-arrestin-1 ARNO ARF6 ELMO protein network. J Cell Sci 2007; 120: 2489–2497.
Fan S, Meng Q, Laterra JJ et al: Ras effector pathways modulate scatter factor-stimulated NF-kappaB signaling and protection against DNA damage. Oncogene 2007; 26: 4774–4796.
Marques-Bonet T, Navarro A : Chromosomal rearrangements are associated with higher rates of molecular evolution in mammals. Gene 2005; 353: 147–154.
Acknowledgements
This work was supported by the Medical Research Council (MRC), United Kingdom (FMH, MAN, LC, JJOT, PTC and RVT); by the Leonardo Da Vinci Fellowship from the European Community (LC); and by grant 15958 from Shriners Hospitals for Children (MPW). We thank the MRC United Kingdom, Human Genome Mapping Project for computing facilities; the nursing and laboratory staff of the Center for Bone Disease and Molecular Metabolic Research, Shriners Hospital for Children, St Louis, for making this study possible. FMH and JJOT were MRC Clinical Research Training Fellows.
Author information
Authors and Affiliations
Corresponding author
Additional information
Electronic database information
Accession numbers and URLs for data in this article are as follows: Human Genome Map Viewer, Build 36.3: http://www.ncbi.nlm.nih.gov/mapview/(GenBank, http://www.ncbi.nlm.nih.gov/Web/GenBank/ (for map of human chromosome 19)); ENTREZ SNP database: http://www.ncbi.nlm.nih.gov/sites/entrez?db=snp; ENTREZ UniSTS database http://www.ncbi.nlm.nih.gov/sites/entrez?db=unists; BLAST: http://blast.ncbi.nlm.nih.gov/Blast.cgi; Online Mendelian Inheritance in Man (OMIM), http://www.ncbi.nlm.nih.gov/omim (for FBH (MIM no. 145980), FBH1 (MIM no. 145980), FBH2 (MIM %145981), FBH3 (MIM %600740).
Rights and permissions
About this article
Cite this article
Hannan, F., Nesbit, M., Turner, J. et al. Comparison of human chromosome 19q13 and syntenic region on mouse chromosome 7 reveals absence, in man, of 11.6 Mb containing four mouse calcium-sensing receptor-related sequences: relevance to familial benign hypocalciuric hypercalcaemia type 3. Eur J Hum Genet 18, 442–447 (2010). https://doi.org/10.1038/ejhg.2009.161
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejhg.2009.161
Keywords
This article is cited by
-
Sensing mechanisms involved in Ca2+ and Mg2+ homeostasis
Kidney International (2012)