Abstract
Background/Objectives:
High body mass index (BMI) is associated with increased incident atrial fibrillation (AF) and mortality rate. In patients presenting with nonvalvular AF (NVAF), the prognostic relevance of BMI remains unclear.
Subjects/Methods:
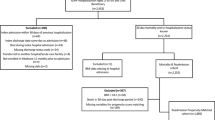
In this prospective observational study, a total of 1759 patients with NVAF (69.9±12.9 years old, 47.9% male) were divided into three clinical settings according to estimated stroke risks (CHADS2 score ⩽1 (low), =2 (moderate) and ⩾3 (high)). The primary outcome was all-cause mortality, and the secondary outcomes included thromboembolism and major bleeding. Cox-proportional hazard models were used to estimate the association between BMI levels and clinical outcomes.
Results:
During a mean follow-up of 1 year representing 1974 patient-years at risk, 256 patients died, 142 suffered from thromboembolism and 17 developed major bleeding. Multivariate adjusted Cox analysis indicated that a BMI of 24.0–27.9 kg/m2 was independently associated with improved survival among all patients (hazard ratio (HR) 0.689, 95% confidence interval (CI) 0.512–0.928; P=0.018) and patients at high stroke risk (HR 0.622, 95% CI 0.410–0.943; P=0.024), but not among those at low or moderate stroke risks. No associations were observed between BMI levels and the incidence of thromboembolic events in various clinical settings.
Conclusions:
A paradoxical BMI–all-cause mortality risk association was observed in Chinese patients with NVAF, and this association was pronounced among patients at high stroke risk rather than in those at low stroke risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Sumeray M, Steiner M, Sutton P, Treasure T . Age and obesity as risk factors in perioperative atrial fibrillation. Lancet 1988; 2: 448.
Wang TJ, Parise H, Levy D, D'Agostino RS, Wolf PA, Vasan RS et al. Obesity and the risk of new-onset atrial fibrillation. JAMA 2004; 292: 2471–2477.
Kokubo Y, Watanabe M, Higashiyama A, Nakao YM, Kobayashi T, Watanabe T et al. Interaction of Blood Pressure and Body Mass Index With Risk of Incident Atrial Fibrillation in a Japanese Urban Cohort: The Suita Study. Am J Hypertens 2015; 28: 1355–1361.
Tedrow UB, Conen D, Ridker PM, Cook NR, Koplan BA, Manson JE et al. The long- and short-term impact of elevated body mass index on the risk of new atrial fibrillation the WHS (women's health study). J Am Coll Cardiol 2010; 55: 2319–2327.
Wilson PW, D'Agostino RB, Sullivan L, Parise H, Kannel WB . Overweight and obesity as determinants of cardiovascular risk: the Framingham experience. Arch Intern Med 2002; 162: 1867–1872.
Kodama S, Horikawa C, Fujihara K, Heianza Y, Hirasawa R, Yachi Y et al. Comparisons of the strength of associations with future type 2 diabetes risk among anthropometric obesity indicators, including waist-to-height ratio: a meta-analysis. Am J Epidemiol 2012; 176: 959–969.
Gupta PP, Fonarow GC, Horwich TB . Obesity and the obesity paradox in heart failure. Can J Cardiol 2015; 31: 195–202.
Kenchaiah S, Evans JC, Levy D, Wilson PWF, Benjamin EJ, Larson MGôK . Obesity and the risk of heart failure. N Engl J Med 2002; 347: 305–313.
Gage BF, Waterman AD, Shannon W, Boechler M, Rich MW, Radford MJ . Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA 2001; 285: 2864–2870.
Jousilahti P, Tuomilehto J, Vartiainen E, Pekkanen J, Puska P . Body weight, cardiovascular risk factors, and coronary mortality. 15-year follow-up of middle-aged men and women in eastern Finland. Circulation 1996; 93: 1372–1379.
Abdullah A, Wolfe R, Stoelwinder JU, de Courten M, Stevenson C, Walls HL et al. The number of years lived with obesity and the risk of all-cause and cause-specific mortality. Int J Epidemiol 2011; 40: 985–996.
Winter JE, MacInnis RJ, Wattanapenpaiboon N, Nowson CA . BMI and all-cause mortality in older adults: a meta-analysis. Am J Clin Nutr 2014; 99: 875–990.
Allison DB, Gallagher D, Heo M, Pi-Sunyer FX, Heymsfield SB . Body mass index and all-cause mortality among people age 70 and over: the Longitudinal Study of Aging. Int J Obes Relat Metab Disord 1997; 21: 424–431.
Lavie CJ, Alpert MA, Arena R, Mehra MR, Milani RV, Ventura HO . Impact of obesity and the obesity paradox on prevalence and prognosis in heart failure. JACC Heart Fail 2013; 1: 93–102.
Shah R, Gayat E, Januzzi JJ, Sato N, Cohen-Solal A, DiSomma S et al. Body mass index and mortality in acutely decompensated heart failure across the world:a global obesity paradox. J Am Coll Cardiol 2014; 63: 778–785.
Uretsky S, Messerli FH, Bangalore S, Champion A, Cooper-Dehoff RM, Zhou Q et al. Obesity paradox in patients with hypertension and coronary artery disease. Am J Med 2007; 120: 863–870.
Zhao W, Katzmarzyk PT, Horswell R, Wang Y, Li W, Johnson J et al. Body mass index and the risk of all-cause mortality among patients with type 2 diabetes mellitus. Circulation 2014; 130: 2143–2151.
Doehner W, Schenkel J, Anker SD, Springer J, Audebert HJ . Overweight and obesity are associated with improved survival, functional outcome, and stroke recurrence after acute stroke or transient ischaemic attack: observations from the TEMPiS trial. Eur Heart J 2013; 34: 268–277.
Strazzullo P, D'Elia L, Cairella G, Garbagnati F, Cappuccio FP, Scalfi L . Excess body weight and incidence of stroke: meta-analysis of prospective studies with 2 million participants. Stroke 2010; 41: e418–e426.
Swedberg K, Cleland J, Dargie H, Drexler H, Follath F, Komajda M et al. Guidelines for the diagnosis and treatment of chronic heart failure: executive summary (update 2005): The Task Force for the Diagnosis and Treatment of Chronic Heart Failure of the European Society of Cardiology. Eur Heart J 2005 26: 1115–1140.
Fauchier L, Grimard C, Pierre B, Nonin E, Gorin L, Rauzy B et al. Comparison of beta blocker and digoxin alone and in combination for management of patients with atrial fibrillation and heart failure. Am J Cardiol 2009; 103: 248–254.
Chen C, Lu FC . The guidelines for prevention and control of overweight and obesity in Chinese adults. Biomed Environ Sci 2004; 17 (Suppl), 1–36.
Zhou BF . Effect of body mass index on all-cause mortality and incidence of cardiovascular diseases—report for meta-analysis of prospective studies open optimal cut-off points of body mass index in Chinese adults. Biomed Environ Sci 2002; 15: 245–252.
Overvad TF, Rasmussen LH, Skjoth F, Overvad K, Lip GY, Larsen TB . Body mass index and adverse events in patients with incident atrial fibrillation. Am J Med 2013; 126: 640.e9–17.
Wang J, Yang YM, Zhu J, Zhang H, Shao XH, Tian L et al. Overweight is associated with improved survival and outcomes in patients with atrial fibrillation. Clin Res Cardiol 2014; 103: 533–542.
Baldinger B, Schwarz C, Jaggy C . Cardiovascular risk factors, BMI and mortality in a cohort of Swiss males (1976–2001) with high-sum-assured life insurance cover. J Insur Med 2006; 38: 44–53.
Wang ZJ, Zhou YJ, Galper BZ, Gao F, Yeh RW, Mauri L . Association of body mass index with mortality and cardiovascular events for patients with coronary artery disease: a systematic review and meta-analysis. Heart 2015; 101: 1631–1638.
Zhang H, Yang Y, Zhu J, Shao X, Liu Y, Zhao L et al. Baseline characteristics and management of patients with atrial fibrillation/flutter in the emergency department: results of a prospective, multicentre registry in China. Intern Med J 2014; 44: 742–748.
Anker SD, Negassa A, Coats AJ, Afzal R, Poole-Wilson PA, Cohn JN et al. Prognostic importance of weight loss in chronic heart failure and the effect of treatment with angiotensin-converting-enzyme inhibitors: an observational study. Lancet 2003; 361: 1077–1083.
Anker SD, Ponikowski P, Varney S, Chua TP, Clark AL, Webb-Peploe KM et al. Wasting as independent risk factor for mortality in chronic heart failure. Lancet 1997; 349: 1050–1053.
Coutinho T, Goel K, Correa DSD, Kragelund C, Kanaya AM, Zeller M et al. Central obesity and survival in subjects with coronary artery disease: a systematic review of the literature and collaborative analysis with individual subject data. J Am Coll Cardiol 2011; 57: 1877–1886.
Oreopoulos A, Ezekowitz JA, McAlister FA, Kalantar-Zadeh K, Fonarow GC, Norris CM et al. Association between direct measures of body composition and prognostic factors in chronic heart failure. Mayo Clin Proc 2010; 85: 609–617.
Wannamethee SG, Shaper AG, Whincup PH, Lennon L, Papacosta O, Sattar N . The obesity paradox in men with coronary heart disease and heart failure: the role of muscle mass and leptin. Int J Cardiol 2014; 171: 49–55.
Kasper EK, Hruban RH, Baughman KL . Cardiomyopathy of obesity: a clinicopathologic evaluation of 43 obese patients with heart failure. Am J Cardiol 1992; 70: 921–924.
Lavie CJ, Milani RV, Ventura HO . Obesity and cardiovascular disease: risk factor, paradox, and impact of weight loss. J Am Coll Cardiol 2009; 53: 1925–1932.
Preston SH, Stokes A . Obesity paradox: conditioning on disease enhances biases in estimating the mortality risks of obesity. Epidemiology 2014; 25: 454–461.
Hu G, Heymsfield SB . Is mortality risk reduced in overweight or obese diabetics? J Gen Intern Med 2014; 29: 3–4.
Lane DA, Lip GY . Use of the CHA(2)DS(2)-VASc and HAS-BLED scores to aid decision making for thromboprophylaxis in nonvalvular atrial fibrillation. Circulation 2012; 126: 860–865.
Acknowledgements
This work was supported by J Zhu and Y Yang, Fuwai Hospital, Beijing; C Li, Chaoyang Hospital, Beijing; X Bai, the First Hospital of China Medical University, Shenyang, Liaoning; F Zhang, Qingdao Municipal Hospital, Shandong; J Li, Bethune International Peace Hospital, Shijiazhuang, Hebei; Y Lu, Rujin Hospital, Shanghai; H Tang, the Central Hospital of Wuhan, Hubei; J Han, Wuhan Unin Hospital, Hubei; Q He, West China Hospital, Chengdu, Sichuan; H Zeng, Guangdong General Hospital, Guangzhou; J Lu, Guangzhou First Hospital, Guangdong; S Wang, the First Hospital of Qiqihaer, Heilongjiang; L Zhao, Fuxing Hospital, Beijing; P Yu, Pingdu People’s Hospital, Shandong; X Hui, Pudong Gongli Hospital, Shanghai; S Liu, Affiliated Hospital of North Sichuan Medical College, Nanchong, Sichuan; X Zhang, the First People’s Hospital of Yichang, Hubei; X Gu, the Sixth People’s Hospital of Chengdu, Sichuan; Z Zan, the Fourth Hospital of Langfang, Hebei; and H Zhang, Qingdao Municipal Hospital (East), Shandong, China.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on European Journal of Clinical Nutrition website
Supplementary information
Rights and permissions
About this article
Cite this article
Wan, H., Wu, S., Wang, J. et al. Body mass index and the risk of all-cause mortality among patients with nonvalvular atrial fibrillation: a multicenter prospective observational study in China. Eur J Clin Nutr 71, 494–499 (2017). https://doi.org/10.1038/ejcn.2016.183
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.183
This article is cited by
-
Association between Body Mass Index and Clinical Outcomes in Patients with Non-valvular Atrial Fibrillation Receiving Direct Oral Anticoagulants: A New Piece of Evidence on the Obesity Paradox from China
Cardiovascular Drugs and Therapy (2023)
-
Reply to ‘Body mass index and the risk of all-cause mortality among patients with nonvalvular atrial fibrillation: a multicenter prospective observational study in China; methodological issues’
European Journal of Clinical Nutrition (2017)
-
Body mass index and the risk of all-cause mortality among patients with nonvalvular atrial fibrillation: a multicenter prospective observational study in China; methodological issues
European Journal of Clinical Nutrition (2017)