Abstract
Background/Objectives:
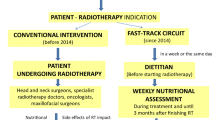
Since 2007, our institution has used validated guidelines for the insertion of proactive gastrostomy feeding tubes in patients with head and neck cancer. Helical intensity-modulated radiotherapy (H-IMRT) delivered by Tomotherapy, is an advanced radiotherapy technique introduced at our centre in 2010. This form of therapy reduces long-term treatment-related toxicity to normal tissues. The aim of this study is to compare weight change and need for tube feeding following H-IMRT (n=53) with patients that would have previously been treated with three-dimensional conformal radiotherapy (n=134).
Subjects/Methods:
Patients with head and neck cancer assessed as high nutritional risk with recommendation for proactive gastrostomy were identified from cohorts from 2007 to 2008 and 2010 to 2011. Retrospective data were collected on clinical factors, weight change from baseline to completion of treatment, incidence of severe weight loss (⩾10%) and tube feeding. Statistical analyses to compare outcomes between the two treatments included χ2-test, Fisher’s exact and two-sample Wilcoxon tests (P<0.05).
Results:
The H-IMRT cohort had higher proportions of patients with definitive chemoradiotherapy (P=0.032) and more advanced N stage (P<0.001). Nutrition outcomes were not significantly different between H-IMRT and conformal radiotherapy, respectively: need for proactive gastrostomy (n=49, 92% versus n=115, 86%, P=0.213), median percentage weight change (−7.2% versus −7.3%, P=0.573) and severe weight loss incidence (28% versus 27%, P=0.843).
Conclusions:
Both groups had median weight loss >5% and high incidences of tube feeding and severe weight loss. Nutrition intervention remains critical in this patient population, despite advances in radiotherapy techniques, and no changes to current management are recommended.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Brown TE, Spurgin AL, Ross L, Tripcony L, Keller J, Hughes BG et al. Validated swallowing and nutrition guidelines for patients with head and neck cancer: Identification of high-risk patients for proactive gastrostomy. Head Neck 2012; 35: 1385–1391.
Hughes BG, Jain VK, Brown T, Spurgin AL, Hartnett G, Keller J et al. Decreased hospital stay and significant cost savings after routine use of prophylactic gastrostomy for high-risk patients with head and neck cancer receiving chemoradiotherapy at a tertiary cancer institution. Head Neck 2012; 35: 436–442.
Brown T, Ross L, Jones L, Hughes B, Banks M . Nutrition outcomes following implementation of validated swallowing and nutrition guidelines for patients with head and neck cancer. Support Care Cancer 2014; 22: 2381–2391.
Nugent B, Lewis S, O'Sullivan JM . Enteral feeding methods for nutritional management in patients with head and neck cancers being treated with radiotherapy and/or chemotherapy. Cochrane Database Syst Rev (Online) 2013; 1: CD007904.
Tyldesley S, Sheehan F, Munk P, Tsang V, Skarsgard D, Bowman CA et al. The use of radiologically placed gastrostomy tubes in head and neck cancer patients receiving radiotherapy. Int J Radiat Oncol Biol Phys 1996; 36: 1205–1209.
Senft M, Fietkau R, Iro H, Sailer D, Sauer R . The influence of supportive nutritional therapy via percutaneous endoscopically guided gastrostomy on the quality of life of cancer patients. Support Care Cancer 1993; 1: 272–275.
Lee JH, Machtay M, Unger LD, Weinstein GS, Weber RS, Chalian AA et al. Prophylactic gastrostomy tubes in patients undergoing intensive irradiation for cancer of the head and neck. Arch Otolaryngol Head Neck Surg 1998; 124: 871–875.
Vergeer MR, Doornaert PA, Rietveld DH, Leemans CR, Slotman BJ, Langendijk JA . Intensity-modulated radiotherapy reduces radiation-induced morbidity and improves health-related quality of life: results of a nonrandomized prospective study using a standardized follow-up program. Int J Radiat Oncol Biol Phys 2009; 74: 1–8.
Sanguineti G, Gunn GB, Parker BC, Endres EJ, Zeng J, Fiorino C . Weekly dose-volume parameters of mucosa and constrictor muscles predict the use of percutaneous endoscopic gastrostomy during exclusive intensity-modulated radiotherapy for oropharyngeal cancer. Int J Radiat Oncol Biol Phys 2011; 79: 52–59.
Romesser PB, Romanyshyn JC, Schupak KD, Setton J, Riaz N, Wolden SL et al. Percutaneous endoscopic gastrostomy in oropharyngeal cancer patients treated with intensity-modulated radiotherapy with concurrent chemotherapy. Cancer 2012; 118: 6072–6078.
Corry J, Poon W, McPhee N, Milner AD, Cruickshank D, Porceddu SV et al. Randomized study of percutaneous endoscopic gastrostomy versus nasogastric tubes for enteral feeding in head and neck cancer patients treated with (chemo)radiation. J Med Imaging Radiat Oncol 2008; 52: 503–510.
Mekhail TM, Adelstein DJ, Rybicki LA, Larto MA, Saxton JP, Lavertu P . Enteral nutrition during the treatment of head and neck carcinoma: is a percutaneous endoscopic gastrostomy tube preferable to a nasogastric tube? Cancer 2001; 91: 1785–1790.
Kramer S, Newcomb M, Hessler J, Siddiqui F . Prophylactic versus reactive PEG tube placement in head and neck cancer. Otolaryngol Head Neck Surg 2014; 150: 407–412.
Amin N, Reddy K, Westerly D, Raben D, DeWitt P, Chen C . Sparing the larynx and esophageal inlet expedites feeding tube removal in patients with stage III-IV oropharyngeal squamous cell carcinoma treated with intensity-modulated radiotherapy. Laryngoscope 2012; 122: 2736–2742.
Rusthoven KE, Raben D, Ballonoff A, Kane M, Song JI, Chen C . Effect of radiation techniques in treatment of oropharynx cancer. Laryngoscope 2008; 118: 635–639.
de Arruda FF, Puri DR, Zhung J, Narayana A, Wolden S, Hunt M et al. Intensity-modulated radiation therapy for the treatment of oropharyngeal carcinoma: the Memorial Sloan-Kettering Cancer Center experience. Int J Radiat Oncol Biol Phys 2006; 64: 363–373.
Ruchala KJ, Olivera GH, Schloesser EA, Mackie TR., Megavoltage CT . on a tomotherapy system. Phys Med Biol 1999; 44: 2597–2621.
Fiorino C, Dell'Oca I, Pierelli A, Broggi S, De Martin E, Di Muzio N et al. Significant improvement in normal tissue sparing and target coverage for head and neck cancer by means of helical tomotherapy. Radiother Oncol 2006; 78: 276–282.
Sheng K, Molloy JA, Read PW . Intensity-modulated radiation therapy (IMRT) dosimetry of the head and neck: a comparison of treatment plans using linear accelerator-based IMRT and helical tomotherapy. Int J Radiat Oncol Biol Phys 2006; 65: 917–923.
Lee TF, Fang FM, Chao PJ, Su TJ, Wang LK, Leung SW . Dosimetric comparisons of helical tomotherapy and step-and-shoot intensity-modulated radiotherapy in nasopharyngeal carcinoma. Radiother Oncol 2008; 89: 89–96.
Ferguson ML, Bauer J, Gallagher B, Capra S, Christie DR, Mason BR . Validation of a malnutrition screening tool for patients receiving radiotherapy. Australas Radiol 1999; 43: 325–327.
Isenring E, Zabel R, Bannister M, Brown T, Findlay M, Kiss N et al. Updated evidence-based practice guidelines for the nutritional management of patients receiving radiation therapy and/or chemotherapy. Nutr Diet 2013; 70: 312–324.
Rivadeneira DE, Evoy D, Fahey TJ, Lieberman MD, Daly JM . Nutritional support of the cancer patient. CA Cancer J Clin 1998; 48: 69–80.
Attar A, Malka D, Sabate JM, Bonnetain F, Lecomte T, Aparicio T et al. Malnutrition is high and underestimated during chemotherapy in gastrointestinal cancer: an AGEO prospective cross-sectional multicenter study. Nutr Cancer 2012; 64: 535–542.
Langius JA, van Dijk AM, Doornaert P, Kruizenga HM, Langendijk JA, Leemans CR et al. More than 10% weight loss in head and neck cancer patients during radiotherapy is independently associated with deterioration in quality of life. Nutr Cancer 2013; 65: 76–83.
Langius JA, Bakker S, Rietveld DH, Kruizenga HM, Langendijk JA, Weijs PJ et al. Critical weight loss is a major prognostic indicator for disease-specific survival in patients with head and neck cancer receiving radiotherapy. Br J Cancer 2013; 109: 1093–1099.
Martin L, Senesse P, Gioulbasanis I, Antoun S, Bozzetti F, Deans C et al. Diagnostic criteria for the classification of cancer-associated weight loss. J Clin Oncol. 2015; 33: 90–99.
Hocking JS, Stein A, Conway EL, Regan D, Grulich A, Law M et al. Head and neck cancer in Australia between 1982 and 2005 show increasing incidence of potentially HPV-associated oropharyngeal cancers. Br J Cancer 2011; 104: 886–891.
Chatterjee S, Mott JH, Smyth G, Dickson S, Dobrowsky W, Kelly CG . Clinical challenges in the implementation of a tomotherapy service for head and neck cancer patients in a regional UK radiotherapy centre. Br J Radiol 2011; 84: 358–366.
Caudell JJ, Schaner PE, Desmond RA, Meredith RF, Spencer SA, Bonner JA . Dosimetric factors associated with long-term dysphagia after definitive radiotherapy for squamous cell carcinoma of the head and neck. Int J Radiat Oncol Biol Phys 2010; 76: 403–409.
Gunn GB, Endres EJ, Parker B, Sormani MP, Sanguineti G . A phase I/II study of altered fractionated IMRT alone for intermediate T-stage oropharyngeal carcinoma. Strahlenther Onkol 2010; 186: 489–495.
Studer G, Peponi E, Kloeck S, Dossenbach T, Huber G, Glanzmann C . Surviving hypopharynx-larynx carcinoma in the era of IMRT. Int J Radiat Oncol Biol Phys 2010; 77: 1391–1396.
van den Berg MG, Rasmussen-Conrad EL, van Nispen L, van Binsbergen JJ, Merkx MA . A prospective study on malnutrition and quality of life in patients with head and neck cancer. Oral Oncol 2008; 44: 830–837.
Capuano G, Grosso A, Gentile PC, Battista M, Bianciardi F, Di Palma A et al. Influence of weight loss on outcomes in patients with head and neck cancer undergoing concomitant chemoradiotherapy. Head Neck 2008; 30: 503–508.
Capelle L, Mackenzie M, Field C, Parliament M, Ghosh S, Scrimger R . Adaptive radiotherapy using helical tomotherapy for head and neck cancer in definitive and postoperative settings: initial results. Clin Oncol 2012; 24: 208–215.
You SH, Kim SY, Lee CG, Keum KC, Kim JH, Lee IJ et al. Is there a clinical benefit to adaptive planning during tomotherapy in patients with head and neck cancer at risk for xerostomia? Am J Clin Oncol 2012; 35: 261–266.
Duma MN, Kampfer S, Schuster T, Winkler C, Geinitz H . Adaptive radiotherapy for soft tissue changes during helical tomotherapy for head and neck cancer. Strahlenther Onkol 2012; 188: 243–247.
Loo H, Fairfoul J, Chakrabarti A, Dean JC, Benson RJ, Jefferies SJ et al. Tumour shrinkage and contour change during radiotherapy increase the dose to organs at risk but not the target volumes for head and neck cancer patients treated on the TomoTherapy HiArt system. Clin Oncol 2011; 23: 40–47.
Chao KS, Low DA, Perez CA, Purdy JA . Intensity-modulated radiation therapy in head and neck cancers: The Mallinckrodt experience. Int J Cancer 2000; 90: 92–103.
Silander E, Jacobsson I, Berteus-Forslund H, Hammerlid E . Energy intake and sources of nutritional support in patients with head and neck cancer—a randomised longitudinal study. Eur J Clin Nutr 2013; 67: 47–52.
Brown T, Banks M, Hughes B, Kenny L, Lin C, Bauer J . Protocol for a randomized controlled trial of early prophylactic feeding via gastrostomy versus standard care in high risk patients with head and neck cancer. BMC Nurs 2014; 13: 17.
Arends J, Bodoky G, Bozzetti F, Fearon K, Muscaritoli M, Selga G et al. ESPEN Guidelines on Enteral Nutrition: non-surgical oncology. Clin Nutr 2006; 25: 245–259.
Brown T, Crombie J, Spurgin AL, Tripcony L, Keller J, Hughes B et al. Improving guideline sensitivity and specificity for the identification of proactive gastrostomy placement in patients with head and neck cancer. Head Neck 35: 1385–1391. in press.
Bauer J, Capra S, Ferguson M . Use of the scored Patient-Generated Subjective Global Assessment (PG-SGA) as a nutrition assessment tool in patients with cancer. Eur J Clin Nutr 2002; 56: 779–785.
White JV, Guenter P, Jensen G, Malone A, Schofield M . Consensus statement: Academy of Nutrition and Dietetics and American Society for Parenteral and Enteral Nutrition: characteristics recommended for the identification and documentation of adult malnutrition (undernutrition). JPEN J Parenter Enteral Nutr 2012; 36: 275–283.
Acknowledgements
We thank Dr Tuan Ha and Vanessa Getliffe for their assistance in data collection, and the staff in medical records and the Combined Head and Neck Clinic at the Royal Brisbane and Women’s Hospital (RBWH) for their support. This study was supported by the Royal Brisbane and Women’s Hospital PhD Scholarship.
Author contributions
TB initiated the study concept. TB, JB, MB and BH contributed to study design. TB and CL participated in the acquisition of data. TB analysed the data and prepared the first draft of the manuscript. All the authors participated in the interpretation of the data, critical revision of the manuscript and the final approval of the submitted version. As corresponding author, TB has full access to all the data in the study and has final responsibility for the decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
TB received a Royal Brisbane and Women’s Hospital PhD Scholarship. The funding body were not involved in the study design, data collection, analysis and interpretation of results, writing of the report or the decision to submit the article for publication. All other authors have no conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Brown, T., Banks, M., Hughes, B. et al. New radiotherapy techniques do not reduce the need for nutrition intervention in patients with head and neck cancer. Eur J Clin Nutr 69, 1119–1124 (2015). https://doi.org/10.1038/ejcn.2015.141
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.141
This article is cited by
-
Nutritional parameters associated with hospital admissions in patients being treated for head and neck cancer
Supportive Care in Cancer (2020)
-
Randomised controlled trial of early prophylactic feeding vs standard care in patients with head and neck cancer
British Journal of Cancer (2017)
-
DARS: a phase III randomised multicentre study of dysphagia- optimised intensity- modulated radiotherapy (Do-IMRT) versus standard intensity- modulated radiotherapy (S-IMRT) in head and neck cancer
BMC Cancer (2016)
-
Validation of an updated evidence-based protocol for proactive gastrostomy tube insertion in patients with head and neck cancer
European Journal of Clinical Nutrition (2016)