- NEWS AND VIEWS
Diet boosts the effectiveness of a cancer drug
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 560, 439-440 (2018)
doi: https://doi.org/10.1038/d41586-018-05871-x
References
Hopkins, B. D. et al. Nature 560, 499–503 (2018).
Fruman, D. A. et al. Cell 170, 605–635 (2017).
Philippon, H., Brochier-Armanet, C. & Perrière, G. BMC Evol. Biol. 15, 226 (2015 ).
De Meyts, P. BioEssays 26, 1351–1362 (2004).
Gallagher, E. J. et al. Oncogene 31, 3213–3222 (2012).
Chi, M., Ye, Y., Zhang, X. D. & Chen, J. Drug Design Dev. Ther. 8, 255-262 (2014).
Blouin, M. J., Zhao, Y., Birman, E. & Pollak, M. Eur. J. Cancer 48 (Suppl. 5), S151 (2012).
Erickson, N., Boscheri, A., Linke, B. & Huebner, J. Med. Oncol. 34, 72 (2017).
Klil-Drori, A. J., Azoulay, L. & Pollak, M. N. Nature Rev. Clin. Oncol. 14, 85–99 (2017).
O’Brien, C. et al. Clin. Cancer Res. 16, 3670–3683 (2010).
Kanarek, N. et al. Nature 559, 632–636 (2018).

 Read the paper: Suppression of insulin feedback enhances the efficacy of PI3K inhibitors
Read the paper: Suppression of insulin feedback enhances the efficacy of PI3K inhibitors
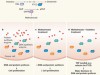 Histidine metabolism boosts cancer therapy
Histidine metabolism boosts cancer therapy
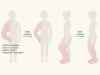 Lessons for cancer drug treatment from tackling a non-cancerous overgrowth syndrome
Lessons for cancer drug treatment from tackling a non-cancerous overgrowth syndrome