- NEWS AND VIEWS
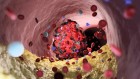
Checkpoint for gut microbes after birth
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 560, 436-438 (2018)
doi: https://doi.org/10.1038/d41586-018-05861-z
References
Fulde, M. et al. Nature 560, 489–493 (2018).
Dominguez-Bello, M. G. et al. Proc. Natl Acad. Sci. USA 107, 11971–11975 (2010).
Yatsunenko, T. et al. Nature 486, 222–227 (2012).
Macpherson, A. J., Gomez de Agüero, M. & Ganal-Vonarburg, S. C. Nature Rev. Immunol. 17, 508–517 (2017).
Rogier, E. W. et al. Proc. Natl Acad. Sci. USA 111, 3074–3079 (2014).
Koch, M. A. et al. Cell 165, 827–841 (2016).
Gensollen, T., Iyer, S. S., Kasper, D. L. & Blumberg, R. S. Science 352, 539–544 (2016).
Olszak, T. et al. Science 336, 489–493 (2012).
Gomez de Agüero, M. et al. Science 351, 1296–1302 (2016).
Vijay-Kumar, M. et al. Science 328, 228–231 (2010).
Chassaing, B., Ley, R. E. & Gewirtz, A. T. Gastroenterology 147, 1363–1377 (2014).
Carvalho, F. A. et al. Cell Host Microbe 12, 139–152 (2012).
Ubeda, C. et al. J. Exp. Med. 209, 1445–1456 (2012).

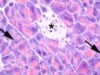 Read the paper: Neonatal selection by Toll-like receptor 5 influences long-term gut microbiota composition
Read the paper: Neonatal selection by Toll-like receptor 5 influences long-term gut microbiota composition
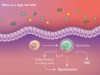 A high-pressure situation for bacteria
A high-pressure situation for bacteria
 Probiotic prevents infections in newborns
Probiotic prevents infections in newborns