Abstract
In patients who were treated with exogenous BMP-2 to repair bone fractures or defects, the levels of the inflammatory cytokines such as TNF-α and IL-1β in sera are significantly elevated, which may affect the outcome of bone regeneration. Mitogen-activated protein kinase (MAPK) cascades such as extracellular signal-regulated kinase 1/2 (ERK1/2), p38, and c-Jun NH2-terminal kinase 1/2 (JNK1/2) have a crucial role in osteogenic differentiation and are activated by both BMP-2 and TNF-α/IL-1β. However, previous studies suggested that the effects of BMP-2 and TNF-α/IL-1β in osteoblastic differentiation are opposite. Here, we investigated the exact role of MAPKs in a BMP-2 and TNF-α/IL-1β co-existed condition. Treatment with TNF-α/IL-1β inhibited BMP-2-induced alkaline phosphatase activity, calcium deposition, osteogenic transcriptional factor Runx2, and the expression of osteogenic markers in C2C12 and MC3T3-E1 cells. This inhibitory effect was independent of the canonical BMP/Smad pathway, suggesting the presence of an alternate regulatory pathway for BMP-2-induced Runx2 activity and subsequent osteoblastic differentiation. We then confirmed that BMP-2, TNF-α, and IL-1β alone can activate p38, ERK1/2, and JNK1/2, respectively. However, only inhibition of p38 and ERK1/2 signaling were required to modulate BMP-2-induced Runx2 expression. Finally, we determined that TNF-α/IL-1β decreased BMP-2-induced Runx2 expression through the activation of p38 and ERK1/2 signaling. Furthermore, strong activation of p38 and ERK1/2 signaling by transfection with CA-MKK3 or CA-MEK1 inhibited BMP-2-induced Runx2 expression and osteoblastic differentiation in C2C12 and MC3T3-E1 cells. Based on these results, we conclude that TNF-α/IL-1β- and BMP-2-activated p38 and ERK1/2 signaling have opposing roles that converge on Runx2 to regulate osteoblastic differentiation. The elucidation of these mechanisms may hasten the development of new strategies and improve the osteoinductive efficacy of BMP-2 in the clinic to enhance osteoblastic differentiation and bone formation.
Similar content being viewed by others
Main
Bone morphogenetic protein-2 (BMP-2) is an important differentiation factor that is capable of inducing bone regeneration by promoting endochondral ossification via chemotaxis, migration, proliferation, and differentiation of mesenchymal stem cells (MSCs), making its potential as an agent to stimulate new bone growth in bone fracture and defect treatment.1 Currently, commercially available recombinant human BMP-2 (rhBMP-2) is impregnated in an absorbable collagen sponge (ACS), which is used to retain rhBMP-2 at wound sites and to permit a slow release into the extracellular milieu. The clinical use of rhBMP-2 was approved by the USA and European Union Food and Drug Administrations for the use in spinal fusions, open tibial factures, and oral maxillofacial reconstructions.2, 3 Early studies of BMP-2/ACS demonstrated its safety profile and relatively significant results in augmenting bone mass at the site of implantation.4 However, extended clinical use of BMP-2/ACS has revealed increasing concerns regarding inflammation-related adverse events such as soft-tissue swelling,5, 6 seroma,7, 8 bone resorption,9 and the low osteoinductive efficacy of BMP-2.4, 10, 11, 12 These complications have resulted in unsatisfactory long-term outcomes in clinical applications.4, 13, 14
The possible causes of the transient and low osteoinductive efficacy of BMP-2 in vivo still remain ambiguous. In the clinic, trauma,15 contamination,16 degradation of the ACS, and exogenous BMP-217, 18 can trigger an exaggerated inflammatory environment, which are characterized by the recruitment of inflammatory cells and stem cells to the implantation site and the secretion of various inflammatory cytokines in sera, such as TNF-α, IL-1β, IL-8, and IL-6.8 Recently, the use of anti-inflammatory drugs such as bone morphogenetic protein-binding peptide,19 triptolide-micelles,20 and corticosteroids21, 22 was proved to reduce the inflammatory response and subsequently enhance the osteoinductive capacity of BMP-2. These results indicate that the low osteoinductive efficacy of BMP-2 may be a result of the exaggerated inflammatory environment. We previously investigated the relationship between inflammation and the low osteoinductive efficacy of BMP-2 and demonstrated that an exaggerated inflammatory environment inhibited BMP-2-induced osteoblastic differentiation of MSCs in vitro and decreased BMP-2/ACS-induced bone mass in a rodent model.23 However, elucidating the mechanism responsible for these phenomena is complicated and requires a more detailed investigation.
BMP-2 modulates osteoblastic differentiation through the canonical BMP/Smad pathway and non-canonical BMP pathways.1, 24, 25 Generally, the activation of target cells by BMP-2 is initiated by type II BMP receptors. The activated BMP receptors subsequently propagate the BMP signals by phosphorylating BMP-specific Smad1/5/8. Finally, Smad1/5/8 binds Smad4, and the complex is transported to the nucleus to activate or repress the transcription of osteogenic genes.1 In addition to BMP/Smad signaling, MAPK cascades represent as an alternative, non-canonical pathway for BMP-2 signal transduction.25, 26, 27 MAPKs are a set of well-described ERK1/2, p38, and JNK1/2.28, 29 MAPKs control many cellular events, including cell proliferation, migration, terminal differentiation, and cell death.30, 31 In the non-canonical MAPK pathways, BMP-2 activates the p38, ERK1/2, and JNK1/2 signaling pathways to promote the expression and activation of an osteogenic-specific transcription factor runt-related transcription factor 2 (Runx2).32 Runx2 has an essential role in osteoblastic differentiation of stem cells and directly stimulates transcription of its important downstream target genes, including those encoding osteocalcin (OCN), type I collagen (COL1A1), and osteopontin (OPN), by binding to specific enhancer regions containing the core sequence.27, 33
TNF-α and IL-1β are two major cytokines that lead to a negative role in bone metabolism in many inflammatory diseases or pathological processes such as rheumatoid arthritis (RA), bone fractures, and ankylosing spondylitis (AS). Similar to BMP-2, TNF-α and IL-1β also simulate MAPK activation in inflammatory environments.30, 31 However, in contrast to the positive role of BMP-2 in bone metabolism, TNF-α and IL-1β have been proved to promote bone loss by activating osteoclastogenesis and decrease bone mineral density by inhibiting osteoblastic differentiation and bone formation.16, 34, 35, 36 Clinical and experimental observations have revealed that TNF-α and IL-1β are also significantly elevated in sera after the implantation of BMP-2/ACS,8, 37, 38, 39, 40 implicating these cytokines as the suspected cause of the low osteoinductive efficacy of BMP-2.23
These data suggest that BMP-2 and TNF-α/IL-1β might have opposite effects on osteoblastic differentiation. These conflicting results of in vitro studies emphasize the need to address the exact role of MAPKs and the mechanism by which they affect osteoblastic differentiation. To clarify the role of BMP-2- and TNF-α/IL-1β-activated MAPKs in osteoblastic differentiation, MC3T3-E1 and C2C12 cells were cultured in BMP-2- and/or TNF-α/IL-1β-supplemented media. We found that under such conditions, BMP-2 and TNF-α/IL-1β induced the activation of the p38 and ERK1/2 signaling pathways and played opposing roles in the regulation of Runx2 expression and osteoblastic differentiation. These opposing roles of BMP-2- and TNF-α/IL-1β-activated p38 and ERK1/2 signaling converged on Runx2 to regulate osteoblastic differentiation.
Results
TNF-α/IL-1β alone suppresses BMP-2-induced osteoblastic differentiation
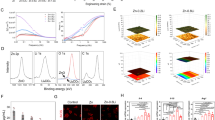
We previously demonstrated that an inflammatory environment inhibits BMP-2-induced bone mass in vivo and osteoblastic differentiation of BMSCs in vitro through inflammatory cytokines, including TNF-α and IL-1β.23 However, the mechanism responsible for this phenomenon is complicated and unclear. Therefore, we examined the effect of TNF-α/IL-1β on BMP-2-induced osteoblastic differentiation. We cultured the multipotent C2C12 cells or preosteoblastic MC3T3-E1 cells in BMP-2- and/or TNF-α/IL-1β-supplemented medium for several days to study the effects of these inflammatory cytokines on BMP-2-induced osteoblastic differentiation. After 7 days of co-culture, alkaline phosphatase (ALP) staining (Figure 1a) demonstrated that presence of TNF-α or IL-1β inhibited BMP-2-induced ALP expression in C2C12 cells. Furthermore, quantitation of ALP activity revealed a dose-dependent inhibitory effect of TNF-α/IL-1β on BMP-2-induced ALP expression (Figure 1b). Consistent with the effects observed for the early marker ALP, Alizarin red staining and quantification were also decreased in the TNF-α/IL-1β-treated MC3T3-E1 cells (Figures 1c–d). We also quantified ALP activity in MC3T3-E1 cells after BMP-2 and/or TNF-α/IL-1β treatment and found that the level of ALP activity in MC3T3-E1 cells was reduced and was similar to that observed in C2C12 cells (Figure 1e). These results demonstrate that TNF-α/IL-1β alone inhibits BMP-2-induced osteoblastic differentiation and mineralization.
TNF-α/IL-1β alone suppresses BMP-2-induced osteoblastic differentiation. (a) C2C12 cells were treated with BMP-2 (200 ng/ml) in the presence or absence of TNF-α (50 ng/mL) or IL-1β (20 ng/ml). The ALP staining assay of ALPase activity on day 7. (b) C2C12 cells were treated with BMP-2 in the presence or absence of TNF-α/IL-1β in a dose-dependent experiment. Quantification assay of ALPase activity on day 3, normalized with the untreated cells. (c–e) MC3T3-E1 cells were treated with BMP-2 (200 ng/ml) in the presence or absence of TNF-α (50 ng/ml) or IL-1β (20 ng/ml). An Alizarin red staining assay of calcium deposition on day 21 (c), quantitative analysis of the Alizarin red staining on day 21 (d), and quantification assay of ALPase activity on day 3 (e), compared with the untreated wells. (f–h) C2C12 cells were treated with BMP-2 in the presence or absence of TNF-α or IL-1β for 48 h. Real-time PCR and relative quantification of COL1A1 (f), OCN (g), and OPN (h), normalized versus GAPDH. Each bar represents the mean±S.D. of three independent experiments. *P<0.05 and **P<0.01 compared with the untreated cells
To further verify these findings, we quantified the transcription levels of the osteogenic genes such as COL1A1 (Figure 1f), OCN (Figure 1g), and OPN (Figure 1h) in C2C12 cells by real-time PCR. BMP-2 increased the transcriptional levels of these genes, but TNF-α/IL-1β alone attenuated this effect. Taken together, these data indicate that TNF-α/IL-1β alone has a crucial role in the inflammation-mediated suppression of BMP-2-induced osteogenesis.
TNF-α/IL-1β alone inhibits BMP-2-induced Runx2 expression via a BMP/Smad-independent pathway
BMP-2 is a potent osteoblastic differentiation factor that signals though Smads. To determine whether TNF-α/IL-1β exerts an inhibitory effect on BMP-2-induced osteoblastic differentiation through crosstalk with the canonical BMP/Smad signaling, C2C12 cells were treated with BMP-2 in the presence or absence of TNF-α/IL-1β. We then analyzed the time- and dose-dependent changes in Smad1/5/8 and Runx2. First, we treated C2C12 cells with BMP-2 in the presence or absence of TNF-α/IL-1β for 0, 4, 8, 12, 24, and 48 h. When cells were stimulated with BMP-2 alone, Smad1/5/8 phosphorylation and Runx2 expression were significantly increased. The maximum Smad1/5/8 signal occurred at 2 h posttreatment, and the maximum Runx2 expression occurred at 48 h posttreatment (Figure 2a, left panel). Consequently, the presence of TNF-α/IL-1β effectively blocked BMP-2-induced Runx2 expression until 48 h later but did not change the phosphorylation of Smad1/5/8 (Figure 2a, middle and right panels). Based on the results of the time-course study, we next treated the cells with BMP-2 in the presence or absence of TNF-α/IL-1β at different concentrations for 2 h to measure the phosphorylation level of Smad1/5/8 and for 48 h to measure the expression level of Runx2 by immunoblotting. Treatment with TNF-α/IL-1β alone for 2 h did not affect the BMP-2-induced phosphorylation of smad1/5/8, but the expression of Runx2 was decreased in a dose-dependent manner after treatment with TNF-α/IL-1β alone for 48 h (Figure 2b).
TNF-α/IL-1β alone inhibits BMP-2-induced Runx2 expression via a BMP/Smad-independent pathway. (a) C2C12 cells were treated with BMP-2 in the presence or absence of TNF-α or IL-1β for 0, 2, 4, 12, 24, and 48 h. Immunoblotting analysis of phosphorylated Smad1/5/8 and Runx2, normalized versus GAPDH. (b) C2C12 cells were treated with BMP-2 in the presence or absence of TNF-α or IL-1β. Immunoblotting analysis of phosphorylated Smad1/5/8 after 2 h; immunoblotting analysis of Runx2 after 48 h, normalized versus GAPDH. (c and d) C2C12 cells were transiently transfected with pSBE-Luc (c) or p6XOSE2-Luc (d) along with pRL-TK-Luc for 24 h. Subsequently, the cells were treated as previously described for 48 h, and luciferase activity assays of the cell lysates were performed, normalized against pRL-TK-Luciferase activity. (e) MC3T3-E1 cells were treated with TNF-α or IL-1β for 1 h, then the cells were treated with BMP-2 for an additional hour, and immunofluorescence analysis of the Smad1 protein was performed. Original magnification, × 200. The results are representative of three independent experiments. Each bar represents the mean±S.D. **P<0.01 compared with the untreated cells or the indicated groups
We next examined whether the BMP-2-induced activation of the BMP/Smad signaling and the transcriptional activity of Runx2 are affected by TNF-α/IL-1β treatment. We performed luciferase reporter assays with the pSBE-Luc vector to monitor the activation of BMP/Smad signaling and with the p6XOSE2-Luc vector to monitor the transcriptional activity of Runx2. BMP-2 treatment alone enhanced Smad1/5/8- and Runx2-induced luciferase activity simultaneously. Notably, the presence of TNF-α or IL-1β significantly suppressed the transcriptional activity of Runx2 but did not affect the phosphorylation of Smad1/5/8 (Figures 2c and d). These data indicate that TNF-α/IL-1β alone inhibits BMP-2-induced Runx2 expression and activation but does not affect the BMP/Smad signaling.
In the canonical BMP/Smad signaling, the phosphorylated Smad proteins are translocated to the nucleus, where they bind specific motifs in promoter regions, recruit Runx2, and regulate the transcription of target genes. To further confirm whether the inhibitory effect of TNF-α/IL-1β on BMP-2-induced osteoblastic differentiation was mediated by BMP/Smad signaling, we examined the nuclear translocation of Smad1 by immunofluorescence staining. As shown in Figure 2e, BMP-2 induced strong nuclear accumulation of Smad1. However, pretreatment with TNF-α/IL-1β did not affect the nuclear translocation of Smad1. Collectively, these data indicate that the inhibitory effect of TNF-α/IL-1β on BMP-2-induced Runx2 expression and activation is independent of the BMP/Smad signaling.
TNF-α, IL-1β, and BMP-2 could activate p38, ERK1/2, and JNK1/2 signaling, respectively
MAPK signaling exerts a wide range of functions and controls of proliferation, migration, terminal differentiation, and cell death.30, 31 There is evidence suggesting that inflammatory cytokines, including TNF-α and IL-1β, activate the MAPK signaling pathway in various cell types. In this study, we observed that the addition of TNF-α/IL-1β to the culture medium induced a rapid and strong activation of MAPK signaling, including p38, ERK1/2, and JNK1/2, in C2C12 cells (Figures 3a and b). The addition of BMP-2 similarly led to the phosphorylation of p38, ERK1/2, and JNK1/2 in C2C12 cells (Figure 3c).
TNF-α, IL-1β, and BMP-2 could activate p38, ERK1/2, and JNK1/2 signaling, respectively. (a–c) C2C12 cells were treated with BMP-2 (a), TNF-α (b), or IL-1 (c) alone for 0, 0.5, 1, 2, 4, 8, 12, and 24 h, and immunoblotting analysis was performed of phosphorylated p38, ERK1/2, and JNK1/2, respectively, normalized versus total p38, ERK1/2, and JNK1/2 protein, respectively. The immunoblotting results are representative of three independent experiments
p38 and ERK1/2 signaling are required in BMP-2-induced Runx2 expression
To determine whether BMP-2-activated MAPK signaling induces Runx2 expression, C2C12 cells were treated with specific inhibitors of the BMP/Smad, p38, ERK1/2, and JNK1/2 signaling pathways. Because of the positive role of BMP/Smad signaling in regulating Runx2 expression,25 we pretreated C2C12 cells with a specific Smad1 inhibitor DMH141, 42 to neutralize BMP-2-induced Runx2 expression and activation. We then examined the changes in Runx2 levels or p6XOSE2-luciferase activity, both of which could be affected by MAPKs. Before stimulation, C2C12 cells expressed a basal level of Runx2 protein, pSBE-Luciferase activity, and p6XOSE2-Luciferase activity. After a 1-h pretreatment with DMH1, the BMP-2-induced phosphorylation of Smad1/5/8 (Figure 4a lane 4) and the upregulation of pSBE-Luciferase activity (Figure 4e) were significantly suppressed to basal levels. However, the protein and mRNA levels of Runx2 (Figures 4a, lane 4 and 4b) as well as p6XOSE2-Luciferase activity (Figure 4f) were significantly lower in DMH1-pretreated cells than in BMP-2-treated cells. Nevertheless, the levels of Runx2 expression and p6XOSE2-Luciferase activity remained above basal level, suggesting the involvement of other signals in regulating Runx2 expression and activation.
p38 and ERK1/2 signaling are required for BMP-2-induced Runx2 expression. (a and b) C2C12 cells were pretreated with the Smad1 inhibitor DMH1 and/or MAPK inhibitors (SB203580, PD98059, or SP600125) for 1 h, and the cells were treated with BMP-2. Immunoblotting analysis of p38, ERK1/2, JNK1/2, and Smad1/5/8 (a) after 2 h; immunoblotting (a) and real-time PCR (b) analysis of Runx2 after 48 h, normalized versus total p38, ERK1/2, JNK1/2, or GAPDH. (c and d) C2C12 cells were transfected with plasmids containing Smad1 siRNA and/or pretreated with MAPK inhibitors (SB203580, PD98059, or SP600125) for 1 h, and the cells were treated with BMP-2. Immunoblotting analysis of Smad1/5/8 (c) after 2 h; immunoblotting (c) and real-time PCR (d) analysis of Runx2 after 48 h, normalized versus GAPDH. (e and f) C2C12 cells were transiently transfected with pSBE-Luc (e) or p6XOSE2-Luc (f) with pRL-TK-Luc for 24 h. Subsequently, the cells were treated as previously described for another 48 h, luciferase activity assays of the cell lysates were performed, normalized against pRL-TK-Luciferase activity. The results are representative of three independent experiments. Each bar represents the mean±S.D. *P<0.05 and **P<0.01 compared with the untreated cells or the indicated groups
We next blocked the different MAPK signaling pathways with the p38-specific inhibitor SB203580, the ERK1/2-specific inhibitor PD98059, and the JNK1/2-specific inhibitor SP600125 in the culture medium. SB203580 or PD98059 displayed synergistic effects with DMH1 to inhibit the BMP-2-induced Runx2 protein and mRNA levels (Figures 4a lane 5, lane 6, and 4b) to the basal levels. By contrast, SP600125 had no significant effect on Runx2 expression (Figures 4a lane 7 and 4b). To investigate the potential role of MAPKs in the regulation of the transcriptional activity of Runx2, p6XOSE2-Luciferase activity was measured in cells after inhibitor and BMP-2 treatment. The p6XOSE2-Luciferase activity was significantly decreased by the pretreatment of cells with SB203580 or PD98059 compared with treatment with BMP-2 only, whereas the p6XOSE2-Luciferase activity was not affected by SP600125 inhibition (Figure 4f). We also used Smad1 siRNA to silence expression of Smad1 in C2C12 cells and then block BMP-2-activated BMP/Smad signaling in this study. The expression of Runx2 in mRNA and protein level were similar to that after DMH1 pretreatment (Figures 4c and d). These results suggest that p38 and ERK1/2 signaling are required in BMP-2-induced Runx2 expression and activation.
TNF-α/IL-1β decreases BMP-2-induced Runx2 expression through the activation of p38 and ERK1/2 signaling
To examine the effect of the TNF-α/IL-1β-activated p38 and ERK1/2 pathways on Runx2 expression and activation, C2C12 cells were treated with BMP-2 and TNF-α/IL-1β in the presence or absence of p38 and ERK1/2 inhibitors. First, we pretreated C2C12 cells with TNF-α for 1 h and then stimulated with BMP-2 for 2 h. We observed that p38 and ERK1/2 signaling were activated at 2 h, whereas the expression of Runx2 protein and p6XOSE2-Luciferase activity were significantly decreased 48 h later (Figures 5a lane 4 and 5b). These results indicate that the activation of p38 and ERK1/2 signaling in these cells suppresses Runx2 expression and activation. Thus, TNF-α-activated p38 and ERK1/2 signaling opposes BMP-2-activated p38 and ERK1/2 signaling in controlling Runx2 expression and activation. To further investigate these opposing roles, we blocked p38 and ERK1/2 signaling with SB203580 and PD98059, respectively. Blocking of p38 and ERK1/2 signaling restored Runx2 protein levels and p6XOSE2-Luciferase activity but did not affect Smad1/5/8 phosphorylation (Figures 5a lane 8, lane 12, and 5b).
TNF-α/IL-1β decreases BMP-2-induced Runx2 expression via activation of p38 and ERK1/2 signaling. (a and c) C2C12 cells were pretreated with a MAPK inhibitor (SB203580 or PD98059) for 1 h, followed by treatment with BMP-2 in the presence or absence of TNF-α/IL-1β. Immunoblotting analysis of p38, ERK1/2, and Smad1/5/8 at 2 h later; immunoblotting analysis of Runx2 after 48 h, normalized versus total p38, ERK1/2, or GAPDH. (b and d) C2C12 cells were transiently transfected with p6XOSE2-Luc along with pRL-TK-Luc for 24 h. Subsequently, the cells were treated as previously described for 48 h, luciferase activity assays in the cell lysates were performed, normalized against pRL-TK-Luciferase activity. The results are representative of three independent experiments. Each bar represents the mean±S.D. **P<0.01 compared with the untreated cells or the indicated groups
Similar results were also observed in C2C12 cells stimulated with BMP-2 and IL-1β (Figures 5c and d). These results indicated that the BMP-2- and TNF-α/IL-1β-activated p38 and ERK1/2 signaling pathways may have an opposing roles in the regulation of Runx2 expression and activation.
Constitutive activation of p38 and ERK1/2 signaling attenuates BMP-2-induced Runx2 activity and osteoblastic differentiation
To further elucidate the role of p38 and ERK1/2 signaling in BMP-2-induced Runx2 activity in an inflammatory environment, we ectopically induced p38 and ERK1/2 signaling activation before exposure to BMP-2 by transfection with CA-MKK3 or CA-MEK1, respectively. Transfection with CA-MKK3 or CA-MEK1 induced strong expression and phosphorylation of p38 and ERK1/2 signaling, respectively, in C2C12 cells without BMP-2 or TNF-α/IL-1β treatment (Figure 6a lane 3 and lane 5). However, overexpression of p38 and ERK1/2 significantly decreased BMP-2-induced Runx2 expression (Figure 6a lane 4 and lane 6) and p6XOSE2-Luciferase activity (Figure 6b), indicating that strong activation of p38 and ERK1/2 signaling has a negative role in Runx2 expression and activation.
Constitutively activation of p38 and ERK1/2 signaling attenuates BMP-2-induced Runx2 expression and osteoblastic differentiation. (a) C2C12 cells were transiently transfected with CA-MKK3 or CA-MEK1 for 24 h. The cells were then treated with BMP-2. Immunoblotting analysis of p38, ERK1/2, and Smad1/5/8 after 2 h; immunoblotting analysis of Runx2 after 48 h, normalized versus total p38, ERK1/2, or GAPDH. (b) C2C12 cells were transiently transfected with CA-MKK3, CA-MEK1, or p6XOSE2-Luc for 24 h. Subsequently, the cells were treated as previously described for 48 h, luciferase activity assay of the cell lysates were performed, normalized against pRL-TK-Luciferase activity. (c and d) C2C12 cells were transiently transfected with CA-MKK3 or CA-MEK1 for 24 h, followed by treatment with BMP-2, quantified assays of ALPase activity on day 3 (d), and ALP staining assays of ALPase on day 7 (c). (e and f) MC3T3-E1 cells were transfected and treated as previously described, real-time PCR (e) and immunofluorescence (f) analysis of OCN on day 2 were performed, normalized versus GAPDH. Original magnification, × 200. Each bar represents the mean±S.D. of three independent experiments. *P<0.05 and **P<0.01 compared with the untreated cells
To further investigate whether the activation of p38 and ERK1/2 signaling have any effect in BMP-2-induced osteoblastic differentiation, we measured changes in the early osteogenic marker ALP in C2C12 cells and the later osteogenic marker OCN in MC3T3-E1 cells. Consistent with Runx2, transfection with CA-MKK3 or CA-MEK1 also significantly decreased the expression of ALP (Figures 6c and d) and OCN (Figures 6e and f). Therefore, these data suggest that strong activation of p38 or ERK1/2 signaling has an inhibitory effect on BMP-2-induced Runx2 expression and osteoblastic differentiation.
Discussion
Increasing exaggerated inflammatory responses and related complications continue to occur after BMP-2/ACS implantation in the clinic and are strongly suspected for the low osteoinductive efficacy of BMP-2. The differentiation factor BMP-2 and the inflammatory cytokines such as TNF-α and IL-1β are proved to have opposing roles in osteoblastic differentiation. However, the exact role of TNF-α/IL-1β in BMP-2-induced osteoblastic differentiation and the underlying mechanism have remained unclear. Herein, we first demonstrated that TNF-α/IL-1β inhibits BMP-2-induced Runx2 expression and activation and subsequent osteoblastic differentiation independent of BMP/Smad signaling. Then, we found that TNF-α, IL-1β, and BMP-2 alone all could activate p38, ERK1/2, and JNK1/2 signaling, respectively. However, TNF-α/IL-1β and BMP-2 has opposing roles on Runx2 expression and activation. Moreover, the presence of TNF-α/IL-1β was found to diminish BMP-2-induced Runx2 activity through the activation of p38 and ERK1/2 signaling. Finally, we confirmed that strong activation of p38 and ERK1/2 signaling by transfection with CA-MKK3 or CA-MEK1 significantly attenuated BMP-2-induced Runx2 expression and osteoblastic differentiation, even without stimulation of TNF-α/IL-1β. Taken together, these data suggest that the TNF-α/IL-1β- and BMP-2-activated p38 and ERK1/2 signaling have opposing roles and converge on Runx2 to regulate BMP-2-induced osteoblastic differentiation.
The study of the interplay between the inflammatory environment and BMP-2 in osteoblastic differentiation is challenging and complicated by at least two issues: (1) the expression profile of inflammatory cytokines in vivo is complicated, and these cytokines have multiple roles in osteoblastic differentiation;8, 16, 34, 35, 36, 37, 38, 39, 40 and (2) BMP-2-induced pathways engage in crosstalk with inflammatory cytokine-induced pathways.23 Clinical and experimental observations have demonstrated that inflammatory cytokines such as TNF-α, IL-1β, IL-8, and IL-6 are significantly elevated in sera after BMP-2/ACS implantation or in supernatant after LPS stimulation.8, 37, 38, 39, 40 Among these elevated inflammatory cytokines, TNF-α and IL-1β can be produced by osteoblasts, surrounding stromal or inflammatory cells.43 The roles of TNF-α and IL-1β in the osteogenic differentiation of progenitor cells and bone metabolism are complicated and biphasic.34, 43, 44, 45, 46 In this study, the presence of TNF-α/IL-1β alone could decrease ALP activity and the expression of osteogenic genes in BMP-2-treated C2C12 cells and MC3T3-E1 cells. These results suggest that TNF-α/IL-1β have negative roles in BMP-2-induced osteoblastic differentiation. Although TNF-α has been shown to inhibit BMP-2-induced osteoblastic differentiation in different cell types,47, 48, 49, 50, 51 the effects of IL-1β on BMP-2-induced osteoblastic differentiation were not investigated in these previous studies, and the underlying mechanisms responsible for this inhibition are unknown.
In the well-documented BMP/Smad signaling pathway, BMP-2 activates Runx2 via the BMP/Smad signaling and subsequently modulates the processes of osteoblastic differentiation. Our data suggested that the presence of TNF-α/IL-1β decreased BMP-2-induced Runx2 expression and activation independent of BMP/Smad signaling. Our finding is further supported by one report demonstrating that TNF-α decrease the expression of Runx2 and the transcription of osteogenic genes by interfering with the DNA binding of Smad proteins instead of inhibiting phosphorylation of Smad1/5/8 or nuclear translocation of the Smad1/Smad4 complex.51 However, several reports have demonstrated that BMP/Smad signaling is required for TNF-α-inhibited osteoblastic differentiation through suppressing Smad1/5/8 phosphorylation and translocation.47, 48, 49, 50 We suspected the discrepancy between these studies, and our approaches are contributed to the cell types and the differentiation stages of the starting cells used. Therefore, these data suggest the existence of another pathway besides BMP/Smad signaling to regulate BMP-2-induced Runx2 expression and activation.
MAPK pathways can be activated by several extracellular stimuli. In our system, we confirmed that TNF-α, IL-1β, and BMP-2 alone all can activate the p38, ERK1/2, and JNK1/2 signaling in C2C12 cells. In previous studies, MAPK pathways can be activated by inflammatory cytokines, particularly TNF-α or IL-1β, to inhibit osteoblastic differentiation.52, 53, 54, 55 Conversely, MAPKs are also required for the induction of an osteoblastic phenotype by BMP-2, leading to mineral deposition in vitro.33, 56, 57 These paradoxical phenomena seem to support the idea that BMP-2- and TNF-α/IL-1β-activated MAPKs have opposing roles in modulating osteoblastic differentiation and have raised a new question: what is the exact role of MAPKs in osteoblast biology in an environment in which inflammatory cytokines and exogenous BMP-2 treatment co-exist simultaneously?
To address this issue, we should first clarify the role of each MAPK cascade on osteoblastic differentiation following BMP-2 treatment. Although the roles of p38, ERK1/2, and JNK1/2 on BMP-2-induced osteoblastic differentiation in various cell types have been well studied, details remain controversial. For example, BMP-2 activates p38 and ERK1/2 but not JNK1/2 to induce osteoblastic differentiation in C2C12 cells.58 However, JNK is required for the BMP-2-induced osteoblastic differentiation of MC3T3-E1-clone 24 cells.33 In this study, BMP-2-induced Runx2 expression and activation were significantly suppressed by the inhibition of BMP/Smad signaling synergistically with p38 or ERK1/2 signaling but not with JNK1/2 signaling. Taken together, our data suggest that p38 and ERK1/2 signaling are required for BMP-2-induced Runx2 expression and activation.
In the clinic, elevated inflammatory cytokines and high concentrations of exogenous BMP-2 unavoidably co-exist in the surrounding of the BMP-2/ACS implant.8 Therefore, we treated C2C12 cells with BMP-2 and TNF-α/IL-1β simultaneously to mimic the clinical model and investigate the exact role of p38 and ERK1/2 signaling in vivo. Our observations suggested that TNF-α/IL-1β inhibited BMP-2-induced Runx2 expression and activation, and p38 and ERK1/2 signaling, not JNK1/2 signaling, were required for this inhibitory effect. These observations are contrary to at least one previous report that TNF-α inhibits BMP-2-induced osteoblastic differentiation by activating SAPK/JNK signaling in C2C12 cells.50 This discrepancy suggests that when C2C12 cells are treated with BMP-2 alone, BMP-2-acvativated p38 and ERK1/2 signaling act as non-canonical pathways and have a weak inductive role in the upregulation of Runx2 expression and activation. However, the addition of TNF-α/IL-1β causes strong p38 and ERK1/2 signaling activation, which has a role in downregulation of Runx2 expression and activation. To further prove this hypothesis, we transfected C2C12 and MCT3C3-E1 cells with CA-MKK3 and CA-MEK1 to strongly induce the ectopic activation of p38 and ERK1/2 signaling before BMP-2 treatment. Under these conditions, independently of the presence of TNF-α/IL-1β, constitutively activated p38 and ERK1/2 signaling significantly attenuated BMP-2-induced Runx2 activation and osteoblastic differentiation. These data suggest that strong activation of p38 and ERK1/2 signaling by inflammatory cytokines, not only TNF-α or IL-1β, decreases BMP-2-induced Runx2 activation and inhibits the osteoblastic differentiation of osteoprogenitor cells in an inflammatory environment.
This study, concerning the opposing roles of TNF-α/IL-1β and BMP-2 in regulation of osteoblastic differentiation in clinical condition, has got several significant conclusions. First, inflammatory cytokines TNF-α and IL-1β inhibited BMP-2-induced osteoblastic differentiation. This result provides an alternate interpretation for the low osteoinductive efficacy of BMP-2 under clinical conditions. Second, BMP-2, TNF-α, and IL-1β alone can activate the p38 and ERK1/2 signaling but have an opposing roles in regulating Runx2 expression and activation (Figures 7a and b). Finally, when exogenous BMP-2 and inflammatory cytokines such as TNF-α and IL-1β are all present, p38 and ERK1/2 signaling are strongly activated, resulting in a significant decrease in BMP-2-induced Runx2 activation and osteoblastic differentiation (Figure 7c). Our study highlights the negative effects of an inflammatory environment on BMP-2-induced osteogenic differentiation and may facilitate the development of new strategies to improve the osteoinductive efficacy of BMP-2 and to enhance bone formation in a clinical setting.
Opposing TNF-α/IL-1β- and BMP-2-activated MAPK signaling pathways converge on Runx2 to regulate BMP-2-induced osteoblastic differentiation. (a) BMP-2 activates the canonical BMP/Smad signaling pathway and non-canonical MAPK pathways to regulate osteoblastic differentiation of osteoprogenitor cells. In the activated MAPK pathways, only p38 and ERK1/2 signaling are required to regulate the expression and activation of Runx2. (b) TNF-α and IL-1β also activate p38, ERK1/2, and JNK1/2 signaling, but they act to oppose the effects of BMP-2 on Runx2 expression and osteoblastic differentiation. (c) Without the positive influence of BMP/Smad signaling, both ERK1/2 and JNK1/2 signaling are activated, but BMP-2-induced Runx2 activity is inhibited, resulting in the suppression of osteoblastic differentiation
Materials and Methods
Cell culture
The murine multipotent mesenchymal progenitor cell line C2C12 and the preosteoblastic cell line MC3T3-E1 were purchased from American Type Culture Collection (ATCC, Manassas, VA, USA). C2C12 cells were grown in Dulbecco’s modified Eagle’s medium (DMEM), and MC3T3-E1 cells were maintained in ascorbic acid-free α-MEM. Both media were supplemented with 10% fetal bovine serum, 100 U/ml penicillin, 100 mg/ml streptomycin, and 0.25 mg/ml amphotericin B (cell culture reagents were obtained from Invitrogen, Carlsbad, CA, USA). For osteogenic differentiation, the medium was replaced with serum-free DMEM or α-MEM containing 200 ng/ml rhBMP2 in the presence or absence of TNF-α (50 ng/ml)/IL-1β (20 ng/ml) (cytokines were obtained from PeproTech, Rocky Hill, NJ, USA). For inhibitor treatment, cells were pretreated with 25 mM Smad1 inhibitor DMH1 (Sigma, St. Louis, MO, USA), 25 mM p38 inhibitor SB203580, 50 mM ERK1/2 inhibitor PD98059, or 25 mM JNK1/2 inhibitor SP600125 (MAPK inhibitors were obtained from Selleck, Shanghai, China) for the indicated times before BMP-2 stimulation.
ALP and Alizarin red staining
Before staining, cells were treated for the indicated times and washed with PBS and fixed with 4% paraformaldehyde for 30 min. For ALP staining, cells were stained with naphthol AS-BI alkaline solution for 45 min to visualize ALP activity. For Alizarin red, cells were stained with 40 mM Alizarin red S (Sigma) solution (pH 4.1) for 10 min to visualize matrix calcium deposition.
Qualification of ALP activity
Cells were exposed to BMP-2 and/or TNF-α/IL-1β at the indicated concentrations for 3 days. The cells were then lysed, and cellular ALPase activity was measured with an ALP detection kit (Nanjing Jiancheng Bioengineering Institute, Nanjing, China). The amount of ALP in the cells was normalized against the total protein content.
RNA extraction, RT-PCR, and quantitative real-time PCR analysis
Total RNAs was isolated from the BMP2-treated cells cultured in the presence and absence of TNF-α/IL-1β. Briefly, cells were washed with PBS and lysed with TRIzol reagent (Invitrogen), according to the manufacturer’s protocol. Then 2 μg of total RNA was used for reverse transcription, and the product was then used for real-time PCR. The quantification levels of osteogenic genes were quantified with an ABI 7500 Real-Time PCR System (Life Technologies, Foster, CA, USA). PCR primer pairs were designed based on the sequences of different exons of the corresponding genes (Table 1). All PCR amplifications were performed with an initial denaturation at 95 °C for 30 s, followed by 40 cycles at 95 °C for 5 s and 60 °C for 34 s, and melting curve analysis at 95 °C for 15 s and 60 °C for 60 s continuous.
Western blotting analysis
Proteins were extracted with RIPA lysis buffer containing 1 mM PMSF (Beyotime, Lianyungang, China). The protein samples were subjected to SDS-PAGE/immunoblotting analysis using anti-phospho-Smad1/5/8 antibody, anti-Runx2 antibody, anti-phospho- and anti-total ERK1/2 antibodies, anti-phospho- and anti-total p38 antibodies, anti-phospho- and anti-total JNK1/2 antibodies, and anti-GAPDH antibody (all from Cell Signaling, Danvers, MA, USA). The relative integrated density of each protein band was determined using an Odyssey infrared imaging system (LI-COR, Lincoln, NE, USA).
Immunofluorescence staining
After various treatments, the cells were fixed in 4% paraformaldehyde and then blocked with 5% goat serum. The cells were immunostained with anti-Smad1 antibody (Epitomics, Burlingame, CA, USA) or anti-OCN antibody (Cell Signaling) followed by a goat anti-rabbit Alexa Fluor-555- or Alexa Fluor-488-conjugated secondary antibody (Invitrogen). The cells were covered with an Anti-Fade Reagent (Cell Signaling).
Transient transfection and dual-luciferase assay
Transient transfections were performed using FuGENE HD (Promega, Madison, WI, USA). The total amounts of transfected plasmids in each group were equalized by the addition of an empty vector. For each transfection, C2C12 or MC3T3-E1 cells were separately co-transfected with Smad1 siRNA (Santa Cruz Biotechnology, Santa Cruz, CA, USA), CA-MKK3 (Cell Biolabs, San Diego, CA, USA), or CA-MEK1 (Cell Biolabs) and a luciferase reporter plasmid containing pSBE-Luc (Promega) or p6XOSE2-Luc (Sangon, Shanghai, China). A dual-luciferase assay was performed by using the Dual Luciferase Reporter Assay kit (Promega). The pSBE-Luciferase reporter plasmid was used to monitor BMP signaling, and the p6XOSE2-Luciferase reporter plasmid, which contained six tandem repeats of a Runx2 binding element in the promoter of the mouse OC gene,59 was used to monitor the transcriptional activity of Runx2.
Statistical analysis
All data are presented as the mean±S.D. of three independent experiments. Statistical evaluations were performed with the Student’s t-test. P-values<0.05 were considered statistically significant.
Abbreviations
- BMP-2:
-
bone morphogenetic protein-2
- MSC:
-
mesenchymal stem cell
- MAPK:
-
mitogen-activated protein kinase
- JNK1/2:
-
c-Jun NH2-terminal kinase 1/2
- ERK1/2:
-
extracellular signal-regulated kinase 1/2
- Runx2:
-
runt-related transcription factor 2
- ALP:
-
alkaline phosphatase
- ACS:
-
absorbable collagen sponge
- COL1A1:
-
type I collagen
References
Rosen V . BMP2 signaling in bone development and repair. Cytokine Growth Factor Rev 2009; 20: 475–480.
Benglis D, Wang MY, Levi AD . A comprehensive review of the safety profile of bone morphogenetic protein in spine surgery. Neurosurgery 2008; 62: ONS423–ONS431 discussion ONS431.
McKay WF, Peckham SM, Badura JM . A comprehensive clinical review of recombinant human bone morphogenetic protein-2 (INFUSE Bone Graft). Int Orthop 2007; 31: 729–734.
Carragee EJ, Hurwitz EL, Weiner BK . A critical review of recombinant human bone morphogenetic protein-2 trials in spinal surgery: emerging safety concerns and lessons learned. Spine J 2011; 11: 471–491.
Tumialan LM, Rodts GE . Adverse swelling associated with use of rh-BMP-2 in anterior cervical discectomy and fusion. Spine J 2007; 7: 509–510.
Smucker JD, Rhee JM, Singh K, Yoon ST, Heller JG . Increased swelling complications associated with off-label usage of rhBMP-2 in the anterior cervical spine. Spine (Phila Pa 1976) 2006; 31: 2813–2819.
Taher F, Lebl DR, Hughes AP, Girardi FP . Contralateral psoas seroma after transpsoas lumbar interbody fusion with bone morphogenetic protein-2 implantation. Spine J 2013; 13: e1–e5.
Robin BN, Chaput CD, Zeitouni S, Rahm MD, Zerris VA, Sampson HW . Cytokine-mediated inflammatory reaction following posterior cervical decompression and fusion associated with recombinant human bone morphogenetic protein-2: a case study. Spine (Phila Pa 1976) 2010; 35: E1350–E1354.
McClellan JW, Mulconrey DS, Forbes RJ, Fullmer N . Vertebral bone resorption after transforaminal lumbar interbody fusion with bone morphogenetic protein (rhBMP-2). J Spinal Disord Tech 2006; 19: 483–486.
Xu R, Bydon M, Sciubba DM, Witham TF, Wolinsky JP, Gokaslan ZL et al. Safety and efficacy of rhBMP2 in posterior cervical spinal fusion for subaxial degenerative spine disease: analysis of outcomes in 204 patients. Surg Neurol Int 2011; 2: 109.
Fu R, Selph S, McDonagh M, Peterson K, Tiwari A, Chou R et al. Effectiveness and harms of recombinant human bone morphogenetic protein-2 in spine fusion: a systematic review and meta-analysis. Ann Intern Med 2013; 158: 890–902.
Beidas OE, Deschamps-Braly JC, Morgan AM, Workman MC, Knotts CD, Denny AD et al. Safety and efficacy of recombinant human bone morphogenetic protein 2 on cranial defect closure in the pediatric population. J Craniofac Surg 2013; 24: 917–922.
Cahill KS, Chi JH, Day A, Claus EB . Prevalence, complications, and hospital charges associated with use of bone-morphogenetic proteins in spinal fusion procedures. JAMA 2009; 302: 58–66.
Hoffmann MF, Jones CB, Sietsema DL . Recombinant human Bone Morphogenetic Protein-2 (rhBMP-2) in posterolateral lumbar spine fusion: complications in the elderly. J Orthop Surg Res 2013; 8: 1.
Pape HC, Marcucio R, Humphrey C, Colnot C, Knobe M, Harvey EJ . Trauma-induced inflammation and fracture healing. J Orthop Trauma 2010; 24: 522–525.
Schett G . Effects of inflammatory and anti-inflammatory cytokines on the bone. Eur J Clin Invest 2011; 41: 1361–1366.
Ritting AW, Weber EW, Lee MC . Exaggerated inflammatory response and bony resorption from BMP-2 use in a pediatric forearm nonunion. J Hand Surg [Am] 2012; 37: 316–321.
MacDonald KM, Swanstrom MM, McCarthy JJ, Nemeth BA, Guliani TA, Noonan KJ . Exaggerated inflammatory response after use of recombinant bone morphogenetic protein in recurrent unicameral bone cysts. J Pediatr Orthop 2010; 30: 199–205.
Lee KB, Murray SS, Taghavi CE, Song KJ, Brochmann EJ, Johnson JS et al. Bone morphogenetic protein-binding peptide reduces the inflammatory response to recombinant human bone morphogenetic protein-2 and recombinant human bone morphogenetic protein-7 in a rodent model of soft-tissue inflammation. Spine J 2011; 11: 568–576.
Ratanavaraporn J, Furuya H, Tabata Y . Local suppression of pro-inflammatory cytokines and the effects in BMP-2-induced bone regeneration. Biomaterials 2012; 33: 304–316.
Tan Y, Montgomery SR, Aghdasi BG, Inoue H, Kaner T, Tian H et al. The effect of corticosteroid administration on soft-tissue inflammation associated with rhBMP-2 use in a rodent model of inflammation. Spine (Phila Pa 1976) 2013; 38: 806–813.
Xiong C, Daubs MD, Montgomery SR, Aghdasi B, Inoue H, Tian H et al. BMP-2 adverse reactions treated with human dose equivalent dexamethasone in a rodent model of soft-tissue inflammation. Spine (Phila Pa 1976) 2013; 38: 1640–1647.
Huang RL, Yuan Y, Zou GM, Liu G, Tu J, Li Q . LPS-stimulated inflammatory environment inhibits BMP-2-induced osteoblastic differentiation through crosstalk between TLR4/MyD88/NF-kappaB and BMP/Smad signaling. Stem Cells Dev 2014; 23: 277–289.
ten DP . Bone morphogenetic protein signal transduction in bone. Curr Med Res Opin 2006; 22 (Suppl 1): S7–11.
Chen G, Deng C, Li YP . TGF-beta and BMP signaling in osteoblast differentiation and bone formation. Int J Biol Sci 2012; 8: 272–288.
Huang YF, Lin JJ, Lin CH, Su Y, Hung SC . c-Jun N-terminal kinase 1 negatively regulates osteoblastic differentiation induced by BMP2 via phosphorylation of Runx2 at Ser104. J Bone Miner Res 2012; 27: 1093–1105.
Guo X, Wang XF . Signaling cross-talk between TGF-beta/BMP and other pathways. Cell Res 2009; 19: 71–88.
Chang L, Karin M . Mammalian MAP kinase signalling cascades. Nature 2001; 410: 37–40.
Johnson GL, Lapadat R . Mitogen-activated protein kinase pathways mediated by ERK, JNK, and p38 protein kinases. Science 2002; 298: 1911–1912.
Kyriakis JM, Avruch J . Mammalian MAPK signal transduction pathways activated by stress and inflammation: a 10-year update. Physiol Rev 2012; 92: 689–737.
Cargnello M, Roux PP . Activation and function of the MAPKs and their substrates, the MAPK-activated protein kinases. Microbiol Mol Biol Rev 2011; 75: 50–83.
Bokui N, Otani T, Igarashi K, Kaku J, Oda M, Nagaoka T et al. Involvement of MAPK signaling molecules and Runx2 in the NELL1-induced osteoblastic differentiation. FEBS Lett 2008; 582: 365–371.
Liu H, Liu Y, Viggeswarapu M, Zheng Z, Titus L, Boden SD . Activation of c-Jun NH(2)-terminal kinase 1 increases cellular responsiveness to BMP-2 and decreases binding of inhibitory Smad6 to the type 1 BMP receptor. J Bone Miner Res 2011; 26: 1122–1132.
Yang N, Wang G, Hu C, Shi Y, Liao L, Shi S et al. Tumor necrosis factor alpha suppresses the mesenchymal stem cell osteogenesis promoter miR-21 in estrogen deficiency-induced osteoporosis. J Bone Miner Res 2013; 28: 559–573.
Zhao B, Grimes SN, Li S, Hu X, Ivashkiv LB . TNF-induced osteoclastogenesis and inflammatory bone resorption are inhibited by transcription factor RBP-J. J Exp Med 2012; 209: 319–334.
Lacey DC, Simmons PJ, Graves SE, Hamilton JA . Proinflammatory cytokines inhibit osteogenic differentiation from stem cells: implications for bone repair during inflammation. Osteoarthritis Cartilage 2009; 17: 735–742.
Lee KB, Taghavi CE, Song KJ, Sintuu C, Yoo JH, Keorochana G et al. Inflammatory characteristics of rhBMP-2 in vitro and in an in vivo rodent model. Spine (Phila Pa 1976) 2011; 36: E149–E154.
Lee KB, Taghavi CE, Murray SS, Song KJ, Keorochana G, Wang JC . BMP induced inflammation: a comparison of rhBMP-7 and rhBMP-2. J Orthop Res 2012; 30: 1985–1994.
Bae HW, Strenge KB, Ashraf N, Badura JM, Peckham SM, McKay WF . Transient soft-tissue edema associated with implantation of increasing doses of rhBMP-2 on an absorbable collagen sponge in an ectopic rat model. J Bone Joint Surg Am 2012; 94: 1845–1852.
Hsu W, Polavarapu M, Riaz R, Larson A, Jared JD, Ghodasra J et al. Characterizing the host response to rhBMP-2 in a rat spinal arthrodesis model. Spine (Phila Pa 1976) 2013; 38: E691–E698.
Ao A, Hao J, Hopkins CR, Hong CC . DMH1 a novel BMP small molecule inhibitor, increases cardiomyocyte progenitors and promotes cardiac differentiation in mouse embryonic stem cells. PLoS One 2012; 7: e41627.
Neely MD, Litt MJ, Tidball AM, Li GG, Aboud AA, Hopkins CR et al. DMH1, a highly selective small molecule BMP inhibitor promotes neurogenesis of hiPSCs: comparison of PAX6 and SOX1 expression during neural induction. ACS Chem Neurosci 2012; 3: 482–491.
Lin FH, Chang JB, McGuire MH, Yee JA, Brigman BE . Biphasic effects of interleukin-1beta on osteoblast differentiation in vitro. J Orthop Res 2010; 28: 958–964.
Gilbert L, He X, Farmer P, Boden S, Kozlowski M, Rubin J et al. Inhibition of osteoblast differentiation by tumor necrosis factor-alpha. Endocrinology 2000; 141: 3956–3964.
Hess K, Ushmorov A, Fiedler J, Brenner RE, Wirth T . TNFalpha promotes osteogenic differentiation of human mesenchymal stem cells by triggering the NF-kappaB signaling pathway. Bone 2009; 45: 367–376.
Glass GE, Chan JK, Freidin A, Feldmann M, Horwood NJ, Nanchahal J . TNF-alpha promotes fracture repair by augmenting the recruitment and differentiation of muscle-derived stromal cells. Proc Natl Acad Sci USA 2011; 108: 1585–1590.
Yamashita M, Otsuka F, Mukai T, Otani H, Inagaki K, Miyoshi T et al. Simvastatin antagonizes tumor necrosis factor-alpha inhibition of bone morphogenetic proteins-2-induced osteoblast differentiation by regulating Smad signaling and Ras/Rho-mitogen-activated protein kinase pathway. J Endocrinol 2008; 196: 601–613.
Matsumoto Y, Otsuka F, Takano M, Mukai T, Yamanaka R, Takeda M et al. Estrogen and glucocorticoid regulate osteoblast differentiation through the interaction of bone morphogenetic protein-2 and tumor necrosis factor-alpha in C2C12 cells. Mol Cell Endocrinol 2010; 325: 118–127.
Tang Y, Xie H, Chen J, Geng L, Chen H, Li X et al. Activated NF-κB in bone marrow mesenchymal stem cells from systemic lupus erythematosus patients inhibits osteogenic differentiation through downregulating Smad signaling. Stem Cells Dev 2013; 22: 668–678.
Mukai T, Otsuka F, Otani H, Yamashita M, Takasugi K, Inagaki K et al. TNF-alpha inhibits BMP-induced osteoblast differentiation through activating SAPK/JNK signaling. Biochem Biophys Res Commun 2007; 356: 1004–1010.
Yamazaki M, Fukushima H, Shin M, Katagiri T, Doi T, Takahashi T et al. Tumor necrosis factor alpha represses bone morphogenetic protein (BMP) signaling by interfering with the DNA binding of Smads through the activation of NF-kappaB. J Biol Chem 2009; 284: 35987–35995.
Eda H, Shimada H, Beidler DR, Monahan JB . Proinflammatory cytokines, IL-1beta and TNF-alpha, induce expression of interleukin-34 mRNA via JNK- and p44/42 MAPK-NF-kappaB pathway but not p38 pathway in osteoblasts. Rheumatol Int 2011; 31: 1525–1530.
Ferreira E, Porter RM, Wehling N, O'Sullivan RP, Liu F, Boskey A et al. Inflammatory cytokines induce a unique mineralizing phenotype in mesenchymal stem cells derived from human bone marrow. J Biol Chem 2013; 288: 29494–29505.
Greenblatt MB, Shim JH, Glimcher LH . Mitogen-activated protein kinase pathways in osteoblasts. Annu Rev Cell Dev Biol 2013; 29: 63–79.
Vincent C, Findlay DM, Welldon KJ, Wijenayaka AR, Zheng TS, Haynes DR et al. Pro-inflammatory cytokines TNF-related weak inducer of apoptosis (TWEAK) and TNFalpha induce the mitogen-activated protein kinase (MAPK)-dependent expression of sclerostin in human osteoblasts. J Bone Miner Res 2009; 24: 1434–1449.
Guicheux J, Lemonnier J, Ghayor C, Suzuki A, Palmer G, Caverzasio J . Activation of p38 mitogen-activated protein kinase and c-Jun-NH2-terminal kinase by BMP-2 and their implication in the stimulation of osteoblastic cell differentiation. J Bone Miner Res 2003; 18: 2060–2068.
Higuchi C, Myoui A, Hashimoto N, Kuriyama K, Yoshioka K, Yoshikawa H et al. Continuous inhibition of MAPK signaling promotes the early osteoblastic differentiation and mineralization of the extracellular matrix. J Bone Miner Res 2002; 17: 1785–1794.
Vinals F, Lopez-Rovira T, Rosa JL, Ventura F . Inhibition of PI3K/p70 S6K and p38 MAPK cascades increases osteoblastic differentiation induced by BMP-2. FEBS Lett 2002; 510: 99–104.
Jun JH, Yoon WJ, Seo SB, Woo KM, Kim GS, Ryoo HM et al. BMP2-activated Erk/MAP kinase stabilizes Runx2 by increasing p300 levels and histone acetyltransferase activity. J Biol Chem 2010; 285: 36410–36419.
Acknowledgements
This research was supported by a grant from the National Key Project of Scientific and Technical Supporting Programs Funded by Ministry of Science and Technology of China (No. 2012BAI11B03) and the National Natural Science Foundation of China (No. 81230042).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by A Stephanou
Rights and permissions
Cell Death and Disease is an open-access journal published by Nature Publishing Group. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Huang, RL., Yuan, Y., Tu, J. et al. Opposing TNF-α/IL-1β- and BMP-2-activated MAPK signaling pathways converge on Runx2 to regulate BMP-2-induced osteoblastic differentiation. Cell Death Dis 5, e1187 (2014). https://doi.org/10.1038/cddis.2014.101
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2014.101
Keywords
This article is cited by
-
Regulation of osteogenic differentiation by the pro-inflammatory cytokines IL-1β and TNF-α: current conclusions and controversies
Human Cell (2022)
-
Enhanced BMP-2/BMP-4 ratio in patients with peripheral spondyloarthritis and in cytokine- and stretch-stimulated mouse chondrocytes
Arthritis Research & Therapy (2020)
-
Lung gene expression signatures suggest pathogenic links and molecular markers for pulmonary tuberculosis, adenocarcinoma and sarcoidosis
Communications Biology (2020)
-
A small nuclear acidic protein (MTI-II, Zn2+-binding protein, parathymosin) attenuates TNF-α inhibition of BMP-induced osteogenesis by enhancing accessibility of the Smad4-NF-κB p65 complex to Smad binding element
Molecular and Cellular Biochemistry (2020)
-
Berberine Promotes Osteogenic Differentiation of Human Dental Pulp Stem Cells Through Activating EGFR-MAPK-Runx2 Pathways
Pathology & Oncology Research (2020)