Abstract
Diverse death phenotypes of cancer cells can be induced by Photofrin-mediated photodynamic therapy (PDT), which has a decisive role in eliciting a tumor-specific immunity for long-term tumor control. However, the mechanism(s) underlying this diversity remain elusive. Caspase-3 is a critical factor in determining cell death phenotypes in many physiological settings. Here, we report that Photofrin-PDT can modify and inactivate procaspase-3 in cancer cells. In cells exposed to an external apoptotic trigger, high-dose Photofrin-PDT pretreatment blocked the proteolytic activation of procaspase-3 by its upstream caspase. We generated and purified recombinant procaspase-3-D3A (a mutant without autolysis/autoactivation activity) to explore the underlying mechanism(s). Photofrin could bind directly to procaspase-3-D3A, and Photofrin-PDT-triggered inactivation and modification of procaspase-3-D3A was seen in vitro. Mass spectrometry-based quantitative analysis for post-translational modifications using both 16O/18O- and 14N/15N-labeling strategies revealed that Photofrin-PDT triggered a significant oxidation of procaspase-3-D3A (mainly on Met-27, -39 and -44) in a Photofrin dose-dependent manner, whereas the active site Cys-163 remained largely unmodified. Site-directed mutagenesis experiments further showed that Met-44 has an important role in procaspase-3 activation. Collectively, our results reveal that Met oxidation is a novel mechanism for the Photofrin-PDT-mediated inactivation of procaspase-3, potentially explaining at least some of the complicated cell death phenotypes triggered by PDT.
Similar content being viewed by others
Main
Photodynamic therapy (PDT) has a direct effect on cancer cells, triggering cell death by autophagy, apoptosis and/or necrosis.1, 2, 3 It was initially believed that PDT killed cells via necrosis, but in 1991, Oleinick and colleagues4 demonstrated that PDT could trigger apoptosis of mouse lymphoma cells. Numerous subsequent studies (including ours) documented that different cell death phenotypes can be induced by PDT, depending on the cell type, the photosensitizer and its subcellular location, the overall dose and the incubation protocol.5, 6, 7, 8, 9 Several reports have shown that Photofrin-PDT can have complicated effects on tumor cells, where either apoptosis or necrosis has been observed.5 However, although many reports have documented the complicated cell death phenotypes induced by PDT, less attention has been paid to the effect of PDT on the modification and regulation of caspase-3 activity, which is a critical factor in determining cell death phenotypes.
Caspase-3, an important executioner in apoptosis, exists in cells as an inactive zymogen and can be activated by proteolysis through either the intrinsic mitochondria-mediated pathway or the extrinsic death-receptor-mediated pathway.10 Owing to its critical role in apoptosis, numerous reports have investigated the regulation of caspase-3 activity by different post-translational modifications, such as nitrosylation, glutathionylation and phosphorylation, all of which inhibited caspase-3 activity.11, 12, 13 However, it is currently unknown whether caspase-3 could be affected and modified by other reactive oxygen species (ROS), such as the singlet oxygen elicited by clinically approved PDT.
Some studies have shown that caspase-3 was activated by PDT, whereas others found that PDT-induced necrosis occurred without caspase-3 activation.3, 14, 15 In this study, we detected significant inhibition of caspase-3 activation exposed to higher (but not lower) doses of Photofrin-PDT, and which could dose-dependently induce covalent modification of procaspase-3 in human cells. We generated and purified recombinant procaspase-3 to confirm the direct inactivation and modification of procaspase-3 by high-dose Photofrin-PDT in vitro. In addition, we used 16O/18O- and 14N/15N-labeling methods coupled with liquid chromatography-electrospray tandem mass spectrometry (LC-MS/MS) to quantitatively analyze procaspase-3, and found that methionine oxidation was the major modification mode caused by Photofrin-PDT. Finally, we observed that Met-44, one of the major modification sites, has an important role in the activation of procaspase-3.
Results
Photofrin-PDT elicits a bell-shape, dose-dependent activation of caspase-3 in human cancer cell lines
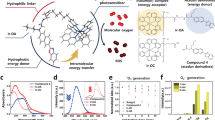
Caspase activation has critical roles in determining the cell death phenotype in PDT treatment, but conflicting reports existed regarding the effects of PDT on the cell death phenotype.14, 15, 16 Here, we performed caspase-3 activity assays in cells treated with different doses of Photofrin followed by PDT. We found that Photofrin-PDT elicited a bell-shape, dose-dependent activation of caspase-3 in both A431 and Jurkat T cells (Figures 1a and d). Caspase-3 activity increased following PDT of cells that received Photofrin doses of 7–14 μg/ml, but decreased drastically when the Photofrin dose was ≥28 μg/ml. We also found that staurosporine, a well-known apoptotic trigger for many cell types,17 could further activate caspase-3 in cells pretreated with Photofrin-PDT. However, the extent of further activation by staurosporine was significantly lower in cells receiving PDT at higher doses (28–112 μg/ml) of Photofrin (Figures 1a and d, compare the gray and white bars). The death phenotypes of both cells treated with different doses of Photofrin-PDT were evaluated by annexin V and propidium iodide staining. The results showed that although apoptosis could be slightly and moderately triggered in A431 and Jurkat T cells, respectively, by lower doses (7–14 μg/ml) of Photofrin-PDT, necrotic-like cell death represented the major death phenotype in both cells that received higher doses (28–112 μg/ml) of Photofrin-PDT (Figures 1b and e). We additionally examined the effect of Photofrin-PDT on the TRAIL or FasL-mediated apoptotic cell death in Jurkat T cells and found that PDT with 28 μg/ml of Photofrin could significantly attenuate the anti-Fas antibody- and TRAIL-mediated caspase-3 activation (Supplementary Figure 1). This finding indicates that high-dose Photofrin-PDT can impair the caspase-3 activation elicited by an apoptotic trigger in both A431 and Jurkat T cells.
Effects of Photofrin-PDT on the activation and modification of procaspase-3. (a) A431 cells were treated with different doses of Photofrin-PDT, and then immediately treated with staurosporine (ST, 1 μM) for another 6 h. Cell lysates (100 μg) were analyzed for caspase-3 activity using Ac-DEVD-pNA as a substrate. PDT, cells were treated with PDT alone; PDT-ST, cells were treated with PDT and ST; Fur Act, the activity difference between PDT-ST and PDT, which denotes further activation by ST. (b) A431 cells were treated with different doses of Photofrin-PDT, and after PDT, the cells were incubated for another 6 h. The cells were then harvested for annexin V (AV)/propidium iodide (PI) staining and flow cytometry analysis. The percentage of positively (+) and negatively (−) stained cells for AV/PI in each condition were indicated. Cells treated with staurosporine (ST, 1 μM) for 6 h were used as control. (c) A431 cells were treated with or without different doses of Photofrin-PDT, and cell extracts (20 μg) were subjected to 10% SDS-PAGE followed by immunoblot analysis with an anti-caspase-3 antibody. C, untreated; L, laser alone for a total of 10 J with a fluence rate of 15 mW; P, 28 μg/ml Photofrin alone. Actin (lower panel) was detected as the internal control. (d–f) Jurkat T cells were treated and analyzed as described in (a–c), respectively. The resulting cell lysates (20 μg in the upper panel and 100 μg in the lower panel) were subjected to immunoblot analysis with an anti-caspase-3 antibody. (g) A431 cell extracts (100 μg) were left untreated (−), treated with 28 μg/ml of Photofrin followed by PDT (+), or treated with 28 μg/ml of Photofrin alone (P). Recombinant active caspase-8 (0.3 U) was then added, and the extracts were incubated at 37°C for 10–30 min in the dark. The reaction products were resolved by SDS-PAGE and analyzed by immunoblotting with an anti-caspase-3 antibody. (h) A431 cell lysates were pretreated without (−) or with (+) 5 mM NaN3, followed by treatment with or without PDT using 28 μg/ml of Photofrin. The cell lysates (100 μg) were then prepared and processed by caspase-8 for 30 min as described in (g)
To explore further, extracts of A431 cells treated with or without Photofrin-PDT were immunoblotted with an anti-caspase-3 antibody. To our surprise, in addition to the expected 32-kDa procaspase-3 protein, we also observed the Photofrin dose-dependent appearance of an unusual high molecular weight (HMW) species (>80 kDa) with immunoreactivity to the anti-caspase-3 antibody (Figure 1c), which could also be observed in Photofrin-PDT-treated Jurkat T cells (Figure 1f). The specificity of anti-caspase-3 antibody was further confirmed using extracts of MCF-7 cells lacking caspase-3 expression18 (Supplementary Figure 2). Consistent with our above findings, PDT with low doses (14 and 28 μg/ml) but not high doses (56–112 μg/ml) of Photofrin could activate caspase-3 in Jurkat T cells as evidenced by immunoblotting (Figure 1f, lower panel). Regarding A431 cells, the p17 subunit could not be detected clearly under the same assay condition (data not shown). Moreover, we found the selectivity of Photofrin-PDT to modify caspase-3 but not caspase-8 and -9 (Supplementary Figure 3). Collectively, these results show that Photofrin-PDT has a dose-dependent biphasic effect on caspase-3 activation, and also suggest that Photofrin-PDT may cause covalent modification of caspase-3 in cells.
High-dose Photofrin-PDT inhibits caspase-8-mediated cleavage/activation of caspase-3 in A431 cell lysates
On the basis of the above observations, we hypothesize that after PDT, procaspase-3 may lose its capability to be processed by upstream caspase-8,10 or its processed product(s) of caspase-3 might lose their enzyme activity via covalent modifications elicited by Photofrin-PDT. As expected, the endogenous procaspase-3 in the control lysates was efficiently processed by exogenous caspase-8 (Figure 1g, compare lanes 3, 5 and 7). However, the active subunits were barely detected in lysates pretreated with Photofrin-PDT (Figure 1g, lanes 4, 6 and 8). These results collectively suggest that Photofrin-PDT may modify procaspase-3 to a form that is not properly processed by caspase-8. The major effect of PDT is to generate ROS, and we found that in the presence of sodium azide (a potent ROS scavenger), Photofrin-PDT could no longer inhibit the caspase-8-mediated proteolytic activation of procaspase-3 (Figure 1h). This observation further indicated that Photofrin-PDT-generated ROS are required for caspase-3 modification(s).
Photofrin-PDT directly elicits the chemical modification and enzymatic inhibition of procaspase-3
To further investigate the mechanism responsible for this effect, we generated and purified recombinant procaspase-3 for further studies. Consistent with previous reports,19 the recombinant procaspase-3 produced in Escherichia coli degraded and quickly autoactivated during purification, producing processed/activated caspase-3 that was not suitable for the present study. We thus generated procaspase-3 mutant (procaspase-3-D3A),20 in which three Asp residues, Asp-9, -28 and -175, were substituted to Ala to prevent autocleavage/activation during purification (Figure 2a). When purified procaspase-3-D3A was treated by Photofrin-PDT, the formation of HMW species resembling those detected in cells was observed (Figure 2b, compare lanes 1 and 2), indicating that cross-linking occurred among the procaspase-3-D3A monomers. In addition to the formation of HMW species, PDT also caused a slight molecular weight shift of the 32-kDa procaspase-3-D3A, resulting in the formation of a clear doublet on the SDS gel (Figure 2b, lane 4); this suggests that PDT can cause complex modifications of procaspase-3-D3A. We also found that Photofrin-PDT suppressed the caspase-3 activity assayed by Ac-DEVD-pNA in a Photofrin dose-dependent manner (Figure 2c). Similar results were observed when we monitored polyADP-ribose polymerase (PARP) as an endogenous substrate (Figure 2d, compare lanes 1–3). Moreover, sodium azide pretreatment significantly attenuated the Photofrin-PDT-mediated suppression of caspase-3 activity (Figure 2d), again indicating that the ROS have a critical role in this effect.
Photofrin-PDT causes inactivation and modification of recombinant procaspase-3-D3A. (a) The amino-acid sequence of the recombinant human procaspase-3-D3A protein. The protein was Ala-mutated at Asp-9, Asp-28 and Asp-175 (underlined) and COOH-terminal tagged with six His residues. (b) Recombinant procaspase-3-D3A was left untreated (−) or treated with PDT (+) using 28 μg/ml of Photofrin, resolved by 10% SDS-PAGE, and then subjected to Coomassie brilliant blue staining (CBB) and immunoblotting with anti-His or anti-caspase-3 antibodies. (c) Recombinant procaspase-3-D3A (10 μg) was incubated with different doses of Photofrin in the dark for 10 min, left in the dark (P) or irradiated with laser (PDT), and then examined by the colorimetric caspase-3 activity assay as described. The experiments were repeated three times with reproducible results. (d) Recombinant procaspase-3-D3A (10 μg) was left untreated (−) or treated (+) with Photofrin-PDT in the absence (−) or presence (+) of 5 mM NaN3. After treatment, A431 cell lysates (100 μg) were mixed individually with the variously treated recombinant procaspase-3-D3A proteins and incubated at 37°C for 1 h in the dark. The reaction products were resolved by 10% SDS-PAGE and subjected to immunoblotting with an anti-PARP antibody. Actin (lower panel) was detected as an internal control. The positions of PARP and its p85 cleavage fragment are denoted by arrows, and the p85 signal was quantified by densitometry
We found that after PDT with 28 μg/ml Photofrin, the protein ratio of the HMW species to procaspase-3-D3A (32 kDa) was∼1/10 to 1/5, but the activity was only 40% of the control level (Figures 2b and c). This finding suggests that covalent modification(s) by small chemical group(s), which we believe cause the slight molecular weight shift of the 32-kDa procaspase-3-D3A, could have a major role in the Photofrin-PDT-mediated suppression of caspase-3 activity.
Direct interaction between procaspase-3-D3A and Photofrin
Photofrin-PDT can trigger the immediate production of ROS,21 which are directly involved in the modification and inactivation of procaspase-3 (Figure 2d). As ROS are highly reactive and have a short half-life, PDT-generated ROS would be likely to affect only components in the vicinity of their production (i.e., adjacent to the photosensitizer). This prompted us to test whether Photofrin can directly bind to procaspase-3-D3A by gel filtration. As shown in Figure 3a, procaspase-3-D3A yielded a minor peak (fraction 8) and a major peak (fraction 13) for optical density at 280 nm but barely emitted fluorescence at 630 nm, whereas Photofrin had a fluorescence peak (fraction 14) but showed very low absorption at 280 nm. However, when a mixture of Photofrin and procaspase-3-D3A was resolved, two prominent fluorescence peaks emerged at fractions 8 and 11 (Figure 3a, lower panel). Subsequent dot-blot analysis of these fractions (Figure 3b) showed that: (i) Photofrin alone did not bind significantly to the PVDF membrane; (ii) procaspase-3-D3A alone was distributed mainly in fractions 10–14 with a minor part in fraction 8, and did not emit a fluorescence signal; and (iii) when the mixture of Photofrin and procaspase-3-D3A was resolved, the signals for procaspase-3-D3A and Photofrin co-existed in fractions 8–15. These observations suggest that Photofrin can bind to and co-elute with procaspase-3-D3A during gel filtration. To explore further, other proteins (e.g., bovine serum albumin, ovalbumin and casein) were spotted in parallel as controls. We found that only the spots containing procaspase-3-D3A showed clear Photofrin signals above the background level (Figure 3c). These results collectively indicate that Photofrin can selectively and directly interact with procaspase-3-D3A.
Gel filtration analysis of the interaction between Photofrin and recombinant procaspase-3-D3A. Recombinant procaspase-3-D3A alone (1 mg), Photofrin alone (18.13 μg) or recombinant procaspase-3-D3A (1 mg) plus Photofrin (18.13 μg) (molar ratio 1 : 1) were applied to Superose 12 columns for gel filtration analysis, as described. (a) Each fraction was subjected to optical density measurement (280 nm) for procaspase-3-D3A proteins and fluorescence measurement (excitation 400 nm and emission 630 nm) for Photofrin. (b) Fractions were also directly spotted onto a PVDF membrane, and procaspase-3-D3A and Photofrin signals were detected by immunoblotting and fluorescence scanning (Typhoon 9400), respectively. (c) Procaspase-3-D3A, bovine serum albumin (BSA), ovalbumin, casein (10 μg of each protein) or Photofrin (5 μg) were spotted onto a PVDF membrane. The membrane was incubated with Photofrin-containing solution (100 μg in 10 ml distilled water) at room temperature in the dark for 3 h, washed thrice for 10 min with distilled water and thrice for 10 min with TTBS buffer (20 mM Tris-HCl, pH 7.4, 0.5 M NaCl, and 0.05% Tween 20). The washed membrane was air-dried and then scanned by a Typhoon 9400 fluorescence scanner
Analysis of Photofrin-PDT-elicited modification of procaspase-3-D3A using 16O/18O- and 14N/15N-labeling-based quantitative proteomics strategies
To examine possible modifications of procaspase-3-D3A and whether Photofrin is covalently linked to procaspase-3-D3A, we first used Fourier transform ion cyclotron resonance MS to measure the molecular mass of procaspase-3-D3A before and after Photofrin-PDT. The mass differences were found to be+16 Da and+32 Da (Supplementary Figure 4), strongly suggesting that Photofrin-PDT can elicit oxidation of procaspase-3-D3A by adding one or two oxygen atoms to the protein. This observation seems to preclude the possibility that porphyrin monomer(s) (580 Da for each monomer) were covalently incorporated into procaspase-3-D3A during Photofrin-PDT. It is well known that PDT can induce oxidation of some proteins such as GRP-78 and Bcl-2.22, 23 Our results also suggested that oxidation may represent the major type of procaspase-3-D3A modification elicited by Photofrin-PDT. We next used 16O/18O- and 14N/15N-labeling-based quantitative proteomics strategies in conjunction with the accurate mass and time tag approach to systemically identify and quantify the Photofrin-PDT-modified amino-acid residues of procaspase-3-D3A (Supplementary Figure 5–8).24 We obtained a list of possible modifications from the LC-MS/MS data and the relative abundance ratios of all identified pairs of 16O/18O-labeled peptides from the LC-MS data (Supplementary Table 1). Most of the detected peptide pairs had ratios of 0.79–1.5, and Table 1 lists 13 peptide pairs with relative abundance ratios ≥1.5. Notably, 12 out of the 13 had at least one oxidized methionine (oxiMet) residue. In fact, 8 of the 10 Met residues in procaspase-3-D3A (Met-27, -39, -44, -100, -182, -222, -233 and -268) showed increased oxidation (≥1.5-fold) after PDT. We further used a more accurate 15N-labeling-based quantitative proteomics strategy (labeling at protein level) to analyze the PDT-elicited Met oxidation of procaspase-3-D3A at different Photofrin doses (Supplementary Figure 8). The quantitation results for all of the detected peptides are shown in Supplementary Table 2. We first analyzed the amounts of unmodified precursor peptides remaining after PDT with four different Photofrin doses. PDT with higher doses of Photofrin (28 and 56 μg/ml) caused significant decreases in the precursor peptides; the N-terminal region (a.a. 1–53) and internal region (a.a. 165–186) showed the most drastic reductions (30–40%) (Figure 4a). We then calculated the oxidized peptide yields after PDT; 7 out of the 10 Met residues (Met-27, -39, -44, -100, -182, -233 and -268) of procaspase-3-D3A showed Photofrin dose-dependent increases of oxidized peptide yields after PDT (Table 2). Figure 4b shows the oxidized peptide yields of all identified peptides following PDT with different Photofrin doses. It is interesting to note that two peptides, 20IIHGSESMASGISLDNSY38K (containing oxiMet-27) and 39MDYPEMGLCIIINN53K (containing oxiMet-39 and oxiMet-44) showed drastic increases in the oxidized peptide yield after PDT; their oxidized yields could reach 40.81 and 75.06% after 56 μg/ml Photofrin-PDT, respectively (Table 2). This suggests that Met-27, -39 and -44 may represent the most vulnerable residues for PDT. Moreover, the oxidized forms of 39MDYPEMGLCIIINN53K could together account for as much as 75.06% of the total detected forms of this peptide, and this value is similar to the extent of caspase-3 activity decrease seen after PDT with 56 μg/ml of Photofrin (Figure 2c). Notably, no oxidized peptide pairs for 157LFIIQAC164R were detected in both 16O/18O and 14N/15N-labeling analysis, suggesting that the catalytic site Cys-163 might not be modified by PDT. Taken together, these results suggest that PDT-induced methionine oxidation might represent the major event leading to the inhibition of procaspase-3-D3A.
Quantitative analysis of Met oxidation of procaspase-3-D3A at different doses of Photofrin-PDT, as assessed using 15N-labeling. (a) Precursor peptides remaining after PDT with different doses of Photofrin. After LC-MS/MS analysis, the amounts of precursor peptides that remained for each detected peptide were calculated from the extracted ion chromatograms derived from the MSQuant results. The PDT versus control (14N/15N) ratios of precursor peptides derived from untreated samples (i.e., dosed with 0 μg/ml of Photofrin) were taken as 100%. (b) Oxidized peptide yields after PDT with different doses of Photofrin. The oxidized peptide yield for each detected peptide was determined from the extracted ion chromatograms as the proportion of oxidized peptide versus that of all possible forms of that particular peptide: oxidized peptide/(oxidized peptide+unmodified precursor peptide+peptides with other modifications). The oxidized peptide yield represented the summation of all kind of oxidations such as single and dual methionine oxidation, cystine trioxidation and so on (see ‘Supplementary Materials and Methods’). This calculation assumed that all possible modifications were identified
Substitution of Met-44 by Leu significantly attenuates the proteolytic maturation of caspase-3
We next questioned whether these Met residues have critical roles in caspase-3 activity regulation. However, there is no available method for creating targeted and site-specific Met oxidations in a protein. Thus, we studied the role of the three Met residues by substituting each of them with leucine, which has a high stereo-structural similarity to methionine. We generated M27L, M39L and M44L mutants of procaspase-3-D3A, respectively, and assayed the purified mutants for caspase-3 activity before and after PDT. Before PDT, the D3A-M27L and D3A-M39L mutants displayed activities comparable to that of procaspase-3-D3A. In contrast, the activity of the D3A-M44L mutant was drastically lower (∼50%) than that of procaspase-3-D3A (Figure 5a), indicating that Met-44 may have an important role in regulating caspase-3 activity regardless of PDT. After PDT, activity losses were seen in all three mutants (20–50%) as compared with their respective original activities without PDT (Figure 5a). Similar results were observed for PARP cleavage assays in total cell lysates (Figure 5b). These observations suggest that oxidation of multiple Met residues could contribute to the Photofrin-PDT-mediated oxidative regulation of caspase-3 activity. We then generated a M44L mutant of wild-type procaspase-3 to further evaluate the role of Met-44 in caspase-3 activity regulation. When wild-type procaspase-3 was expressed in E. coli, induction triggered its autoprocessing in 1–1.5 h. In contrast, the M44L mutant maturated after induction for 2 h (Figure 5c), indicating that substituting Met-44 with Leu slowed the autoprocessing of procaspase-3. Furthermore, we expressed all the procaspase-3 constructs in MCF-7 cells. In addition, we also generated a prodomain deletion mutant (ΔN) and its M44L mutant (ΔN-M44L) to test whether this Met-to-Leu mutation had any effect on procaspase-3 processing at Asp-175 (Figure 5d), as it has been well established that during activation, procaspase-3 is first cut at Asp-175 between the large and small subunits, and then at Asp-28 between the prodomain and the large subunit.25 MCF-7 cells transiently transfected with these expression plasmids were challenged by UV irradiation to trigger caspase-3 activation. All procaspase-3 variants were ectopically expressed in MCF-7 cells at levels similar to that of the wild-type (Figure 5e, upper panel). They could respond to UV irradiation, as evidenced by the detection of active caspase-3 fragments (Figure 5e, middle panel) and increased casapase-3 activity (Figure 5f). The ΔN mutant was activated more strongly (∼2-fold) by UV stress than the wild-type (Figure 5f), which is consistent with a previous report that the prodomain of procaspase-3 may have autoinhibitory effects.26 The M44L mutant and the corresponding prodomain deletion mutant (ΔN-M44L), but not M27L and M39L, inhibited casapase-3 activation as compared with the activations of the wild-type and ΔN mutant, respectively (Figures 5e and f). These results collectively indicate that the Met-44 residue has an important role in regulating Asp-175 cleavage during caspase-3 maturation.
Substitution of Met-44 by Leu attenuates the proteolytic maturation of caspase-3 in E. coli and MCF-7 cells. (a and b) Purified recombinant procaspase-3-D3A and its Met-to-Leu mutants (Met-27, Met-39 and Met-44) were treated with PDT using 28 μg/ml of Photofrin, followed by caspase-3 activity assays using Ac-DEVD-pNA (a) or endogenous PARP from A431 cell lysates (b). In (b), A431 cell lysates (100 μg) were digested with procaspase-3-D3A and its mutants at 37°C for 1 h, resolved by 10% SDS-PAGE, and subjected to immunoblotting with an anti-PARP antibody. ‘Act Casp3’ denotes the recombinant active form of caspase-3 purified from E. coli. (c) Wild-type procaspase-3 and its Met-to-Leu mutants were cloned into the pET23a vector, expressed in E. coli BL-21(DE3) cells via IPTG induction for different time periods, and analyzed by immunoblotting with an anti-caspase-3 antibody. FL, full-length form of procaspase-3; Ac, activated form of caspase-3. (d) Schematic representation of the structures of EGFP-tagged full-length procaspase-3, prodomain-deleted (ΔN) procaspase-3 and the Met-to-Leu mutants (Met-27, Met-39 and Met-44). The lower panel denotes the predicted MWs of the unprocessed and possible proteolytic forms of caspase-3 found in MCF-7 cells after the application of UV irradiation to trigger apoptosis. (e and f) Vectors encoding EGFP-tagged full-length procaspase-3, ΔN-procaspase-3 or the Met-to-Leu mutants were individually transfected to MCF-7 cells, and the transfected cells were selected with G418 (800 μg/ml) for 2 weeks. The stably selected cells were left untreated or irradiated with UV light (200 J/m2). Cell lysates were collected at 4, 8 and 24 h and subjected to 15% SDS-PAGE, followed by immunoblot analysis using antibodies against GFP, cleaved caspase-3 (D175) or actin (e), or by caspase-3 activity assay using Ac-DEVD-pNA (f). The experiments were repeated three times with reproducible results
Discussion
PDT-induced cell apoptosis or necrosis may occur through complicated mechanisms,27 and PDT-induced inflammatory responses to necrotic tumor cells can elicit a tumor-specific immunity that can have a decisive role in attaining long-term tumor control.28, 29 However, no previous study has investigated whether caspase-3 itself is subject to direct regulation by covalent modification in PDT-treated cells. Here, we report that Photofrin-PDT can directly modify procaspase-3, impair its enzyme activity, and decrease its activation by the upstream activator, caspase-8 (Figures 1 and 2). These findings could explain why higher doses of Photofrin-PDT failed to trigger significant caspase-3 activation in the tested cells (Figure 1). Several studies have reported that the death phenotype can be switched from apoptosis to necrosis-like death by inhibition of caspase-3.30, 31, 32 Our present findings appear to provide a new and important mechanism through which the fate of Photofrin-PDT-treated tumor cells may be determined.
Using two different MS-based quantitative approaches and purified recombinant procaspase-3-D3A, we systemically explored the Photofrin-PDT-triggered modifications of procaspase-3. The results from both strategies showed that Met oxidation represented the major modification of procaspase-3-D3A peptides (Tables 1 and 2). The oxidations of Met-27, Met-39 and Met-44 were determined to be the three most prominent modifications. Surprisingly, the modification ratio of the active site (Cys-163)-containing peptide did not change following PDT in both experiments, indicating that either the active site was not modified, or the modification was too minor to be detected by MS. Mapping the susceptible Met residues in the 3D structure of procaspase-3 (PDB code: 1I3O, a.a. 32–174 and 176–277)33 shows that Met-39 and Met-44 cluster together at the surface of each monomer (Figure 6). In contrast, the active site Cys-163 is located at the interface of the two monomers. This analysis supports the notion that amino-acid residues located at the surface of caspase-3 are more susceptible to Photofrin-PDT-mediated oxidation, and may also explain why we didn’t detect oxidation of the active site Cys-163 (i.e., Photofrin could not reach it). Although Met-61 and Met-182 were also exposed on the outside of the dimeric structure, their oxidations were not significant (Tables 1 and 2, and Supplementary Table 1 and 2). This observation further suggests that Photofrin-PDT-mediated Met oxidation shows selectivity. Collectively, we identify the N-terminal region of procaspase-3 that is highly susceptible to Photofrin-PDT-mediated oxidative stress by quantitative proteomics approaches.
The crystal structure of caspase-3. Positions of the Met residues are denoted in the caspase-3 structure (PDB code: 1I3O33). To generate this structure, the active site (Cys-163) of recombinant procaspase-3 was mutated to Ala, and the protein was digested by granzyme and cocrystallized with XIAP. The N-terminal 1–31 residues were not resolved because of granzyme digestion at Asp-28. The orange and blue colors represent the dimeric caspase-3 molecules with their large and small subunits. Met-39, -44 and -222 are shown schematically as ball-and-stick atoms (gray, carbon; yellow, sulfur; and red, oxygen). The active site C163A is shown as a space-filling model. Met residues that did not show significant changes after Photofrin-PDT are indicated in green
Numerous studies have reported that Met oxidation can induce functional changes in proteins/peptides.34, 35 Fluorophore-assisted light inactivation treatment also triggers the formation of singlet oxygen, which can cause Met oxidation and inactivation of calmodulin.36 Modifications of sensitive residues located in a regulatory or catalytic region of the protein could have a profound effect on its function. Although we have shown that Met oxidation represents the major detectable covalent modification during the Photofrin-PDT-mediated inhibition of caspase-3, the role of Met oxidation in this observed inhibitory process still remains elusive. Our findings that (i) caspase-8-mediated cleavage of procaspase-3 at both Asp-175 and Asp-28 was drastically inhibited by Photofrin-PDT pretreatment (Figure 1), and (ii) the oxidized peptide yield of 39MDYPEMGLCIIINN53K correlated well with the caspase-3 activity loss after Photofrin-PDT (Figures 2 and 4) suggest that Photofrin-PDT-mediated Met-39/44 oxidation of procaspase-3 might interfere with the cleavage/activation process. During the maturation process, procaspase-3 is first cut at Asp-175 and forms the p20/p12 complex,37 which is catalytically active and can undergo autocleavage at Asp-28 to remove the prodomain and generate the mature p17/p12 caspase-3.25 Notably, mutation of Met-44 caused the prodomain cleavage without producing activity and inhibition of caspase-3 activation procedure by an apoptotic trigger (UV irradiation) (Figure 5). It is possible that Met-44 has a role in regulating caspase-3 cleavage/activation process, and oxidation of Met-44 may increase the hydrogen bonding to the surrounding amino-acid residues and alter the local structure, thereby affecting the proteolytic maturation of procaspase-3. Further experiments are needed to clarify the detailed mechanism.
PDT has been shown to damage several proteins/enzymes, leading to the loss of their biological activity,38, 39, 40 but little is known about how they are modified and whether they are the direct targets of Photofrin (i.e., Photofrin-binding proteins). We show here for the first time that Photofrin can directly bind to procaspase-3 (Figure 3), and provide evidence that this direct interaction could be the major driving force for the observed modification/inactivation of procaspase-3 during Photofrin-PDT. It is interesting to note that Zawacka-Pankau and colleagues40 has also reported direct interaction between Fhit and protoporphyrin IX (PpIX), which is the precursor for generating Photofrin. Fhit lost its hydrolase activity following PpIX-PDT in vitro, and the H98N mutation inhibits both the Fhit-PpIX interaction and Fhit’s tumor-suppressing ability, implying that H98 may be a vulnerable residue for PpIX-PDT and an important residue for Fhit hydrolase activity. These observations collectively suggest that the direct binding of photosensitizers to specific proteins may guide the selectivity of protein modification in PDT-treated cells.
In conclusion, we herein report for the first time that Photofrin-PDT can induce covalent modification of procaspase-3 and impair its activation in a ROS-dependent manner. Photofrin can directly bind to procaspase-3, the ROS formed immediately after laser irradiation can preferentially oxidize procaspase-3 on several Met residues (but not the active site Cys-163), and the Met-44 residue has a critical role in the proteolytic processing of procaspase-3 at Asp-28 and 175. Thus, the present study reveals a novel mechanism through which caspase-3 activity is regulated in tumor cells treated with Photofrin-PDT.
Materials and Methods
Cell culture and Photofrin-PDT
Human epidermoid carcinoma A431 and breast adenocarcinoma MCF-7 cells were cultured at 37°C in DMEM supplemented with 10% heat-inactivated fetal bovine serum, 100 U/ml penicillin, and 100 μg/ml streptomycin. Jurkat T cells were cultured at 37°C in RPMI-1640 supplemented with 10% heat-inactivated fetal bovine serum, 100 U/ml penicillin and 100 μg/ml streptomycin. Cells were incubated in media containing various concentrations of Photofrin (diluted from a 2.5 mg/ml stock solution in 5% dextrose) (Pinnacle Biologics, Inc., Bannockburn, IL, USA) in the dark at 37°C for 3 h, and then irradiated with a 632.8-nm He–Ne laser (Coherent, Santa Clara, CA, USA; fluence rate 15 mW, total energy 10 J/cm2). The cell culture plates were covered with aluminum foil, and all processes up to the SDS-PAGE step were performed in the dark to avoid unwanted light exposure. After PDT, the cells were washed twice with ice-cold PBS and lysed in lysis buffer (10 mM Tris-HCl, pH 7.4, 1 mM EDTA, 1 mM EGTA, 1% Triton X-100, 1 mM benzamidine, 1 mM phenylmethylsulfonyl fluoride, 50 mM sodium fluoride, 20 mM sodium pyrophosphate and 1 mM sodium orthovanadate) on ice for 15 min. The cell lysates were sonicated on ice and collected by centrifugation at 11 000 r.p.m. for 30 min at 4°C, and the protein concentrations were determined with a BCA protein assay reagent (Pierce, Rockford, IL, USA).
Anti-Fas antibody and TRAIL treatments
After PDT treatment, Jurkat T cells (5 × 106/ml) were treated with 500 ng Fas antibody (Clone CH.11, Millipore Upstate, Billerica, MA, USA) or TRAIL (PeproTech, Rocky Hill, NJ, USA) for 6 h. The cell lysates were then collected and analyzed by immunoblotting and caspase-3 activity assay.
Immunoblotting
Immunoblotting was carried out essentially as described.8 The monoclonal anti-CPP32/caspase-3 antibody was from Transduction Laboratories (Lexington, KY, USA); the anti-PARP, anticleaved caspase-3 (D175), anti-caspase-8 and anti-caspase-9 antibodies were from Cell Signaling Technology (Beverly, MA, USA); the anti-actin antibody was from Millipore (Billerica, MA, USA); and the anti-His antibody was from Santa Cruz Biotechnology (Santa Cruz, CA, USA). These antibodies were used to probe proteins transferred from SDS gels onto PVDF membranes, and the resulting signals were quantified by a densitometer (GE Healthcare Bio-Science, Uppsala, Sweden).
Plasmid construction
The full-length human caspase-3 gene was amplified by PCR using cDNAs derived from human epidermoid carcinoma A431 cells as templates, and primers containing NdeI/XhoI sites (NdeI, 5'-GGAATTCCATATGGAGAACACTGAAAACTCAG-3'; XhoI, 5'-CCGCTCGAGGTGATAAAAATAGAGTTCTTTTGTG-3'). Purified PCR products were digested by NdeI and XhoI and cloned into the respective sites of a pET23a vector (Merck KGaA, Darmstadt, Germany) to generate the pET23a-caspase-3 expression plasmid. To produce the pET23a-caspase-3-D3A mutant, in which the cleavage sites at D9, -28 and -175 were substituted to alanines, we used the following forward and reverse primers: D9A-f, 5′-CATATGGAGAACACTGAAAACTCAGTGCTTCAAAATCC-3′; D9A-r, 5′-GGATATTCCAGAGGCCATTGATTCGCT-3′; D28A-f, 5′-GAATCAATGGCCTCTGGAATA-3′; D28A-r, 5’-AACACCACTGGCTGTCTCAAT-3′; D175A-f, 5′-GGCATTGAGACAGCCAGTGGTGTGAT-3′; D175A-r, 5′-TGTTAGCAGCCGGATCTCAGTGG-3′. We first amplified three fragments by paired primers: M1-D28 (fragment 1), D28-D175 (fragment 2) and D175-H285 (fragment 3). After PCR product purification, we used fragment 1 and 2 as templates, D9A-f and D28A-f as primers to generate fragment M1-D175 (fragment 1+2). At last, we used fragment 1+2 and fragment 3 as templates, D9A-f and D175A-r as primers to generate full-length caspase-3 contained D3A mutations. After PCR amplification, we used digestion and ligation to generate the pET23a-caspase-3-D3A mutant. To construct the Met-to-Leu mutants of caspase-3 and caspase-3-D3A, Met-27, -39 and -44 were substituted to Leu using a QuikChange site-directed mutagenesis kit (Stratagene, La Jolla, CA, USA) and specific primers (M27L, 5′-GGAATATCCCTGGACAACAGTTATAAACTGGATTATCCTGAG-3′; M39L, 5′-ACAACAGTTATAAAATGGATTATCCTGAGCTGGGTTTATGTATAATAATTAATAATAAG-3′; and M44L, 5′-CCAGTCGCTTTGTGCCCTGCTGAAACAGTATGC-3′). The resulting constructs were also subcloned into the pET23a-caspase-3, pET23a-caspase-3-D3A and pEGFP-C3 vectors (Clontech Laboratories Inc., Mountain View, CA, USA). To generate the prodomain deletion mutant, caspase-3-ΔN, we amplified pEGFP-C3-procaspase-3 with specific primers (ΔN-EcoRI-f, 5′-GAATTCCGTCTGGAATATCCCTGGACAAC-3′; KpnI-r, 5′-CGCGGTACCTTAGTGATAAAAATAGAGTTCTTTTG-3′), digested the amplified fragments and ligated them into the above-described vectors. Caspase-3-ΔN-M44L was also generated using a site-directed mutagenesis kit and the M44L primer. The DNA sequences of all constructs were confirmed by autosequencing.
Purification of recombinant caspase-3
E. coli BL21(DE3)-pLysS cells were transformed with pET23a-caspase-3, pET23a-caspase-3-D3A or the various methionine-to-leucine mutants. The transformed E. coli were grown and subjected to IPTG induction for 3 h, and the cultures were harvested and purified on His-Trap-FF columns (GE Healthcare Bio-Science, Piscataway, NJ, USA). The fractions containing recombinant proteins were concentrated and desalted with Amicon Centricon filters (5-kDa cutoff; Millipore), and the purified proteins were resuspended in distilled water or the caspase-3 activity assay buffer (see below).
Caspase-3 activity assay
Caspase-3 activity was determined using the Ac-DEVD-pNA colorimetric substrate (Merck KGaA). Briefly, cell lysates (100 μg) or recombinant caspase-3 (10 μg) were incubated in 0.1 ml caspase assay buffer (50 mM HEPES, pH 7.4, 0.1% CHAPS, 10 mM DTT, 0.1 mM EDTA, 100 mM NaCl and 10% glycerol) containing 0.2 mM Ac-DEVD-pNA at 37°C for 30–120 min, and the relative caspase-3 activities were determined by spectrophotometry at 405 nm. In some experiments, the relative activities of recombinant caspase-3 proteins were measured by their abilities to cleave the PARP protein to produce a 85 kDa fragment in cell lysates (100 μg), as detected by immunoblotting.
Annexin V and propidium iodide staining and flow cytometry
A431 and Jurkat T cells were treated with different doses of Photofrin-PDT. After 6 h incubation, cells were stained by FITC Annexin V Apoptosis Detection Kit (BD Biosciences, San Jose, CA, USA) and analyzed by FACSCalibur (BD Biosciences).
Gel filtration analysis
Recombinant procaspase-3-D3A alone (1 mg), Photofrin alone (18.13 μg) or procaspase-3-D3A (1 mg) plus Photofrin (18.13 μg) (molar ratio 1 : 1) were applied to Superose 12 HR 10/30 columns (GE Healthcare Bio-Science) pre-equilibrated with buffer A (0.05 M phosphate buffer with 0.15 M NaCl, pH 7.0). Fractions (1 ml) were collected and assessed by optical density measurement (280 nm) for procaspase-3-D3A proteins and by fluorescence measurement (excitation 400 nm and emission 630 nm) for Photofrin. Fractions were also directly spotted onto PVDF membranes, and procaspase-3-D3A and Photofrin signals were detected by immunoblotting and fluorescence scanning (Typhoon 9400; GE Healthcare), respectively.
Plasmid transfection and UV treatment
MCF-7 cells were separately transfected with various caspase-3 mutant plasmids using Lipofectamine 2000 (Invitrogen, Carlsbad, CA, USA) according to the provided protocol. After 24 h expression, transfected cells were irradiated by UV light (200 J/m2) and the cell lysates were harvested after 4 or 8 h incubation for immunoblotting and caspase-3 activity assay.
Mass spectrometry data analysis
The intact protein measurement, 16O/18O labeling, 14N/15N labeling and mass spectrometry-related sample preparation and data analysis are detailed in the Supplementary Materials and Methods.
Abbreviations
- HMW:
-
high molecular weight
- LC-MS/MS:
-
liquid chromatography-electrospray tandem mass spectrometry
- PDT:
-
photodynamic therapy
- PARP:
-
polyADP-ribose polymerase
- ROS:
-
reactive oxygen species
References
Oleinick NL, Morris RL, Belichenko I . The role of apoptosis in response to photodynamic therapy: what, where, why, and how. Photochem Photobiol Sci 2002; 1: 1–21.
Kessel D, Vicente MG, Reiners JJ . Initiation of apoptosis and autophagy by photodynamic therapy. Autophagy 2006; 2: 289–290.
Marchal S, Fadloun A, Maugain E, D'Hallewin MA, Guillemin F, Bezdetnaya L . Necrotic and apoptotic features of cell death in response to Foscan photosensitization of HT29 monolayer and multicell spheroids. Biochem Pharmacol 2005; 69: 1167–1176.
Agarwal ML, Clay ME, Harvey EJ, Evans HH, Antunez AR, Oleinick NL . Photodynamic therapy induces rapid cell death by apoptosis in L5178Y mouse lymphoma cells. Cancer Res 1991; 51: 5993–5996.
Dellinger M . Apoptosis or necrosis following Photofrin photosensitization: influence of the incubation protocol. Photochem Photobiol 1996; 64: 182–187.
Peng Q, Moan J, Nesland JM . Correlation of subcellular and intratumoral photosensitizer localization with ultrastructural features after photodynamic therapy. Ultrastruct Pathol 1996; 20: 109–129.
Hsieh YJ, Wu CC, Chang CJ, Yu JS . Subcellular localization of Photofrin determines the death phenotype of human epidermoid carcinoma A431 cells triggered by photodynamic therapy: when plasma membranes are the main targets. J Cell Physiol 2003; 194: 363–375.
Hsieh YJ, Yu JS, Lyu PC . Characterization of photodynamic therapy responses elicited in A431 cells containing intracellular organelle-localized photofrin. J Cell Biochem 2010; 111: 821–833.
Wyld L, Reed MW, Brown NJ . Differential cell death response to photodynamic therapy is dependent on dose and cell type. Br J Cancer 2001; 84: 1384–1386.
Boatright KM, Salvesen GS . Mechanisms of caspase activation. Curr Opin Cell Biol 2003; 15: 725–731.
Mannick JB, Hausladen A, Liu L, Hess DT, Zeng M, Miao QX et al. Fas-induced caspase denitrosylation. Science 1999; 284: 651–654.
Huang Z, Pinto JT, Deng H, Richie JP . Inhibition of caspase-3 activity and activation by protein glutathionylation. Biochem Pharmacol 2008; 75: 2234–2244.
Alvarado-Kristensson M, Melander F, Leandersson K, Ronnstrand L, Wernstedt C, Andersson T . p38-MAPK signals survival by phosphorylation of caspase-8 and caspase-3 in human neutrophils. J Exp Med 2004; 199: 449–458.
Mikes J, Kleban J, Sackova V, Horvath V, Jamborova E, Vaculova A et al. Necrosis predominates in the cell death of human colon adenocarcinoma HT-29 cells treated under variable conditions of photodynamic therapy with hypericin. Photochem Photobiol Sci 2007; 6: 758–766.
Furre IE, Moller MT, Shahzidi S, Nesland JM, Peng Q . Involvement of both caspase-dependent and -independent pathways in apoptotic induction by hexaminolevulinate-mediated photodynamic therapy in human lymphoma cells. Apoptosis 2006; 11: 2031–2042.
Chen Y, Zheng W, Li Y, Zhong J, Ji J, Shen P . Apoptosis induced by methylene-blue-mediated photodynamic therapy in melanomas and the involvement of mitochondrial dysfunction revealed by proteomics. Cancer Sci 2008; 99: 2019–2027.
Bertrand R, Solary E, O'Connor P, Kohn KW, Pommier Y . Induction of a common pathway of apoptosis by staurosporine. Exp Cell Res 1994; 211: 314–321.
Janicke RU, Sprengart ML, Wati MR, Porter AG . Caspase-3 is required for DNA fragmentation and morphological changes associated with apoptosis. J Biol Chem 1998; 273: 9357–9360.
Denault JB, Salvesen GS . Expression, purification, and characterization of caspases. Curr Protoc Protein Sci 2003; Chapter 21: Unit 21 13.
Bose K, Pop C, Feeney B, Clark AC . An uncleavable procaspase-3 mutant has a lower catalytic efficiency but an active site similar to that of mature caspase-3. Biochemistry 2003; 42: 12298–12310.
Moan J, Berg K . The photodegradation of porphyrins in cells can be used to estimate the lifetime of singlet oxygen. Photochem Photobiol 1991; 53: 549–553.
Kessel D, Castelli M, Reiners JJ . Ruthenium red-mediated suppression of Bcl-2 loss and Ca(2+) release initiated by photodamage to the endoplasmic reticulum: scavenging of reactive oxygen species. Cell Death Differ 2005; 12: 502–511.
Magi B, Ettorre A, Liberatori S, Bini L, Andreassi M, Frosali S et al. Selectivity of protein carbonylation in the apoptotic response to oxidative stress associated with photodynamic therapy: a cell biochemical and proteomic investigation. Cell Death Differ 2004; 11: 842–852.
Qian WJ, Monroe ME, Liu T, Jacobs JM, Anderson GA, Shen Y et al. Quantitative proteome analysis of human plasma following in vivo lipopolysaccharide administration using 16O/18O labeling and the accurate mass and time tag approach. Mol Cell Proteomics 2005; 4: 700–709.
Han Z, Hendrickson EA, Bremner TA, Wyche JH . A sequential two-step mechanism for the production of the mature p17:p12 form of caspase-3 in vitro. J Biol Chem 1997; 272: 13432–13436.
Meergans T, Hildebrandt AK, Horak D, Haenisch C, Wendel A . The short prodomain influences caspase-3 activation in HeLa cells. Biochem J 2000; 349 (Pt 1): 135–140.
Buytaert E, Dewaele M, Agostinis P . Molecular effectors of multiple cell death pathways initiated by photodynamic therapy. Biochim Biophys Acta 2007; 1776: 86–107.
Castano AP, Mroz P, Hamblin MR . Photodynamic therapy and anti-tumour immunity. Nat Rev Cancer 2006; 6: 535–545.
Garg AD, Nowis D, Golab J, Agostinis P . Photodynamic therapy: illuminating the road from cell death towards anti-tumour immunity. Apoptosis 2010; 15: 1050–1071.
Xiang J, Chao DT, Korsmeyer SJ . BAX-induced cell death may not require interleukin 1 beta-converting enzyme-like proteases. Proc Natl Acad Sci USA 1996; 93: 14559–14563.
Hirsch T, Marchetti P, Susin SA, Dallaporta B, Zamzami N, Marzo I et al. The apoptosis-necrosis paradox. Apoptogenic proteases activated after mitochondrial permeability transition determine the mode of cell death. Oncogene 1997; 15: 1573–1581.
Vercammen D, Beyaert R, Denecker G, Goossens V, Van Loo G, Declercq W et al. Inhibition of caspases increases the sensitivity of L929 cells to necrosis mediated by tumor necrosis factor. J Exp Med 1998; 187: 1477–1485.
Riedl SJ, Renatus M, Schwarzenbacher R, Zhou Q, Sun C, Fesik SW et al. Structural basis for the inhibition of caspase-3 by XIAP. Cell 2001; 104: 791–800.
Yamniuk AP, Ishida H, Lippert D, Vogel HJ . Thermodynamic effects of noncoded and coded methionine substitutions in calmodulin. Biophys J 2009; 96: 1495–1507.
Schoneich C . Methionine oxidation by reactive oxygen species: reaction mechanisms and relevance to Alzheimer's disease. Biochim Biophys Acta 2005; 1703: 111–119.
Yan P, Xiong Y, Chen B, Negash S, Squier TC, Mayer MU . Fluorophore-assisted light inactivation of calmodulin involves singlet-oxygen mediated cross-linking and methionine oxidation. Biochemistry 2006; 45: 4736–4748.
Pop C, Chen YR, Smith B, Bose K, Bobay B, Tripathy A et al. Removal of the pro-domain does not affect the conformation of the procaspase-3 dimer. Biochemistry 2001; 40: 14224–14235.
Kim SY, Tak JK, Park JW . Inactivation of NADP(+)-dependent isocitrate dehydrogenase by singlet oxygen derived from photoactivated rose bengal. Biochimie 2004; 86: 501–507.
Suto D, Sato K, Ohba Y, Yoshimura T, Fujii J . Suppression of the pro-apoptotic function of cytochrome c by singlet oxygen via a haem redox state-independent mechanism. Biochem J 2005; 392 (Pt 2): 399–406.
Ferens B, Kawiak A, Banecki B, Bielawski KP, Zawacka-Pankau J . Aberration of the enzymatic activity of Fhit tumor suppressor protein enhances cancer cell death upon photodynamic therapy similarly to that driven by wild-type Fhit. Cancer Lett 2009; 280: 101–109.
Acknowledgements
We thank the members of the Proteomics Core Laboratory for helping with the mass spectrometry. We are grateful to Mr. Chien-Wei Lee for assisting with the 16O/18O labeling, Mr. Yuan-Ming Yeh for helping with online searches and the use of the post-translational modification database and Mr. Chi-De Chen for helping us generate our LTQ-orbitrap data. This work was supported by grants NSC94-2745-B-182-003-URD and NSC99-2320-B-182-017-MY3 (National Science Council of Taiwan, ROC), EMRPD190041 (the Ministry of Education, Taiwan, ROC) and CMRPD33026 (Chang Gung Memorial Hospital, Tao-Yuan, Taiwan, ROC).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by T Brunner
Supplementary Information accompanies the paper on Cell Death and Disease website
Supplementary information
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Hsieh, YJ., Chien, KY., Lin, SY. et al. Photofrin binds to procaspase-3 and mediates photodynamic treatment-triggered methionine oxidation and inactivation of procaspase-3. Cell Death Dis 3, e347 (2012). https://doi.org/10.1038/cddis.2012.85
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2012.85
Keywords
This article is cited by
-
Oxidation of protein-bound methionine in Photofrin-photodynamic therapy-treated human tumor cells explored by methionine-containing peptide enrichment and quantitative proteomics approach
Scientific Reports (2017)
-
Interaction and oxidative damage of DVDMS to BSA: a study on the mechanism of photodynamic therapy-induced cell death
Scientific Reports (2017)