Abstract
The phagocyte NADPH oxidase is a multicomponent enzyme complex mediating microbial killing. We find that NADPH oxidase p47phox-deficient (p47phox−/−) chronic granulomatous disease (CGD) mice develop lymph node hyperplasia even without obvious infection, where increased number of T and B lymphocytes is associated with increased percent of naïve cells and a lower T : B cell ratio than wild type. Paradoxically, despite lymphoid hyperplasia in vivo, when lymphocytes are placed in culture, p47phox−/− CD8+ lymphocytes progress more rapidly to apoptosis than wild type. This is associated in cultured p47phox−/− CD8+ lymphocytes with the induction of proapoptotic Bim and Puma expression, increased mitochondrial outer membrane permeabilization and depressed Bcl-2 expression. Addition of IL-7 to the culture partially corrects Bcl-2 levels in cultured p47phox−/− CD8+ lymphocytes and improves the survival. Adding glucose oxidase to the culture to generate hydrogen peroxide along with IL-7 further improves p47phox−/− CD8+ lymphocyte survival, but only to 30% of wild type. We conclude that p47phox−/− CD8+ lymphocytes have an intrinsic survival defect likely in part related to the oxidase deficiency, but in vivo in lymph nodes of CGD mice, there are microenvironmental factors yet to be delineated that suppress the progression of apoptosis and allow the accumulation of lymphocytes leading to lymphoid hyperplasia.
Similar content being viewed by others
Main
Within the complex microarchitecture of secondary lymphoid organs (SLOs), such as lymph nodes (LNs) and spleen, critical signals balance lymphocyte survival and homeostasis. Self-major histocompatibility molecule stimulation of the T-cell receptor (TcR) and extrinsic signals provided by cytokines, such as IL-7 and IL-15 control naïve T-lymphocyte survival.1, 2 In addition, these signals facilitate continuous low-level division of resting naïve T cells during homeostatic proliferation to maintain T-cell number and repertoire diversity.2 Homeostasis is disrupted during the mounting of an immune response allowing for clonal expansion of effector lymphocytes. Thereafter, the majority of effector cells die to prevent undesirable autoimmunity, and a subset survives as memory T cells.3, 4 Immune responses are mounted within SLOs to eradicate invading pathogens. However, impaired pathogen clearance in an immunocompromised host often results in sustained immune responses that produce local acute inflammatory responses and ultimately systemic chronic inflammation.
Resting naïve T cells recirculate between blood and lymphoid tissues, whereas memory T cells migrate to nonlymphoid tissue sites. Furthermore, without antigen encounter, resting naïve T cells eventually die within a defined half-life.5, 6 Survival of resting naïve T cells during recirculation between inflamed and noninflamed SLOs undoubtedly requires different signals than those required for survival during recirculation between noninflamed SLOs. In this manuscript, we examined the relationship between nicotinamide adenine dinucleotide phosphate (NADPH) oxidase deficiency and naïve T-cell survival within SLOs. The phagocyte multicomponent, NADPH oxidase, mediates the single electron reduction of oxygen to superoxide anion resulting in the well-characterized respiratory burst, which promotes innate cell killing of catalase-positive microorganisms.7, 8 Several nonphagocytic cells have been reported to express ligand-dependent NADPH oxidase-like reactive oxygen species (ROS).9 We reported that T cells express each of the NADPH oxidase structural proteins and TcR stimulation induces low level intracellular NADPH oxidase-dependent hydrogen peroxide.10 Chronic granulomatous disease of childhood (CGD) is the genetically inherited primary immunodeficiency, that is caused by defects of structural NADPH oxidase proteins.11 CGD patients are at increased risk of developing and succumbing to life-threatening infection and acute and chronic inflammatory diseases.12 Here, we report that NADPH oxidase p47phox-deficient (p47phox−/−) mice without the evidence of gross infection develop reactive SLOs characterized by LN hyperplasia with increased B- and T-lymphocyte accumulations.13 Nearly half of spleen and LN resting p47phox−/− CD8+ lymphocytes rapidly die ex vivo, and during the initial 24 h of in vitro culture, significantly more resting LN p47phox−/− CD8+ lymphocytes undergo caspase-independent cell death than splenic p47phox−/− CD8+ lymphocytes. BH3-only proapoptotic Bim and Puma protein expressions are significantly reduced in LN p47phox−/− CD8+ lymphocytes. However, Bim and Puma expressions are significantly enhanced in vitro, and dying p47phox−/− CD8+ lymphocytes from p47phox−/− LNs show increased mitochondrial outer membrane permeabilization (MOMP) and depressed Bcl-2 expression. These results indicate that microenvironmental factors generated during ongoing immune responses in p47phox−/− mice provide signals that regulate naïve T-lymphocyte homeostasis and survival, and may contribute to cellular immune dysfunction in CGD patients.
Results
LN hyperplasia in p47phox−/− mice
p47phox−/− mice have LN hyperplasia, increased total numbers of B and T lymphocytes and lower T : B cell ratios than age- and sex-matched wild-type (WT) mice (Figure 1). However, p47phox−/− and WT CD4 : CD8 ratios were comparable. Flow-cytometry analysis showed p47phox−/− and WT LNs contained phenotypically naïve B220+CD27− B cells, and comparable phenotypically naïve CD44lowCD62Lhigh and CD25lowCD69low CD4+ and CD8+ T lymphocytes (Supplementary Figure 1).
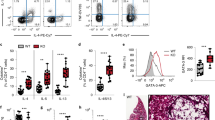
LN hyperplasia and in vivo lymphocyte proliferation in p47phox−/− mice. Single cell suspensions of resting LN cells from WT and p47phox−/− mice were generated. Surface B220, CD3 CD8 and CD4 expressions on peripheral LN cells of WT and p47phox−/− mice were assessed by flow cytometry. (a) The total number of cells as well as absolute number of B and T lymphocytes isolated from the peripheral LNs of WT and p47phox−/− mice were quantitated. (b) The ratios of T : B cells and CD4 : CD8 T cells in the peripheral LNs of WT and p47phox−/− mice were quantitated. The data shown are the mean±S.E.M. of five independent experiments with three mice/experiment. p47phox−/− responses are indicated by the open histograms and WT responses are indicated by the shaded histograms. *P=0.014, **P=0.007. p47phox−/− and WT mice (n=3) were fed with BrdU in their drinking water at a concentration of 1 mg/ml for 5 days. Lymph nodes were harvested on day 5. Whole lymph node cell populations were stained with anti-CD4, CD8, CD44, B220 and BrdU antibodies and assessed by flow cytometry. (c) The percentage of CD44+low and CD44high -BrdU+ CD4 (left) and CD8 (right) lymphocytes in WT or p47phox−/− lymph nodes is shown. (d) The percent of B220+-BrdU+ lymphocytes in WT or p47phox−/− lymph nodes is shown. *P<0.02
In vivo 5-bromo-2′deoxyuridine (BrdU) incorporation studies demonstrated that the peripheral LN CD4+ lymphocyte turnover was similar in p47phox−/− and WT mice, whereas p47phox−/− CD8+ CD44high T cells proliferated 1.5 times more than WT cells (Figure 1c). Peripheral LN p47phox−/− B cells also hyperproliferated compared to WT B cells (Figure 1d). Collectively, these data show that within the reactive p47phox−/− LN microenvironment, there is increased B-cell and memory CD8+-cell divisions along with an increased accumulation of naïve B and T lymphocytes.
Exaggerated death of p47phox−/− CD8+ lymphocytes
Numerous investigations have reported that ROS mediates apoptosis in a variety of cells including T cells. Although investigations of activated T-cell death concluded that excess ROS disrupts mitochondrial membrane integrity by perturbing the balance of Bcl-2 antiapoptotic and proapoptotic proteins, and antioxidants protect activated T cells from ROS-mediated apoptosis,1, 6, 14, 15, 16 the role of ROS in naïve T-cell survival is less clear. To determine whether NADPH oxidase ROS mediates resting T-cell survival, we examined cytokine responses of LN-derived T lymphocytes. Viable and nonviable lymphocytes from 24 h cultures were differentially stained with DNA-binding dyes and the absolute number of viable versus nonviable nucleated cells were quantitated on the basis of cell size and staining properties using the Guava ViaCount assay (see Materials and Methods). Cell count and viability were determined and the data were normalized to the baseline values. After 24 h of culture in IL-2, fewer resting p47phox−/− CD4+ and CD8+ lymphocytes remained viable than WT lymphocytes. Furthermore, there was significantly more cell death of resting p47phox−/− CD8+ lymphocytes (Figure 2).
In vitro cytokine-activated lymphocyte survival. Fractionated CD4+ and CD8+ p47phox−/−and WT lymphocytes were cultured in IMDM alone or supplemented with IL-2 or IL-7, as indicated, for 24 h. The total number of viable and nonviable nucleated cells was measured using the Guava ViaCount assay. p47phox−/− responses are indicated by the open histograms and WT responses are indicated by the shaded histograms. (a) The percentage of viable CD4+ (right) and CD8+ (left) p47phox−/− and WT lymphocytes after 24 h in culture. (b) The total number of viable and nonviable nucleated CD8+ cells was measured using the Guava ViaCount assay, and responses were normalized to the baseline values. The percentage of viable p47phox−/− and WT cells was quantitated at 4 h (left) and 24 h (right). (c) The fold increase in dead CD8+-lymphocyte cell number in the p47phox−/− cultures supplemented with IL-2 (open histogram) and IL-7 (hatched histogram) at 24 h was quantitated. (d) Glucose oxidase-produced H2O2 enhances p47phox−/− CD8+-lymphocyte survival. Fractionated CD8+ p47phox−/−and WT lymphocytes were cultured with IL-2 or IL-7 supplemented culture medium with 1 pg/ml of glucose oxidase (GO) for 24 h. The histograms show the percentage of viable cells at 24 h. p47phox−/− IL-2±GO (open histogram), p47phox−/− IL-7±GO (gray shaded histogram), WT IL-2±GO (black shaded histogram) and WT IL-7±GO (hatched histogram). The data shown are the mean±S.E.M. of four independent experiments with three mice/experiment. *P=0.01, **P<0.0001, ***P=0.003
Both IL-4 and IL-7 have been shown to provide survival signals for resting T cells in vitro,17, 18, 19, 20, 21 and studies have shown IL-7 protects resting T cells from apoptotic death by regulating antiapoptotic and proapoptotic Bcl-2 factors.6, 22 Next, we cultured resting p47phox−/− and WT lymphocytes in IL-7 to determine whether IL-7 could rescue dying CD8+ p47phox−/− lymphocytes. At baseline, the percentage of viable p47phox−/− and WT CD8+ cells were comparable. Both WT and p47phox−/− CD8+ lymphocytes cultured in IL-7 for 24 h showed significantly enhanced survival over cells cultured in IMDM alone or with IL-2 (Figure 2b), and p47phox−/− CD8+ lymphocytes cultured in IL-7 contained significantly fewer dead cells than lymphocytes cultured in IL-2 (Figure 2c). However, p47phox−/− CD8+ lymphocytes die at an accelerated rate in vitro even when cultured in IL-7, which prevents WT CD8+ cell death.
We previously reported TcR-stimulated T-cell blasts release a prolonged pulse of NADPH oxidase-dependent hydrogen peroxide (H2O2).10 Consequently, to assess whether the survival defect in p47phox−/− CD8+ lymphocytes could be rescued by exogenous H2O2, CD8+ cells from p47phox−/− and WT mice were incubated with the H2O2 generating enzyme glucose oxidase (GO) for 24 h. GO is a flavoenzyme that catalyses the conversion of β-D-glucose to H2O2, and produces a continuous pulse of H2O2.23, 24 The combination of GO (1 pg/ml) and IL-7 enhanced p47phox−/−-lymphocyte survival 10% over that seen with IL-7 alone (Figure 2d, Supplementary Figure 2). Although 10 ng/ml GO was toxic to p47phox−/− and WT CD8+ cells (data not shown), 1 pg/ml GO was not toxic and did not alter WT-lymphocyte survival. Using lower concentrations of GO (see Materials and Methods) did not improve p47phox−/−-lymphocyte survival. These results indicate that exogenous replacement of intracellular H2O2 by enzymatic manipulation further enhances IL-7-mediated rescue of p47phox−/− CD8+ lymphocytes.
Prosurvival cytokines IL-2, IL-4, IL-7 and IL-15 are members of the IL-2 family of cytokines that share the common γ-c-receptor subunit,25 and Park et al.26 showed that these cytokines suppress IL-7 receptor (IL-7R) transcription and expression in resting T cells. To determine p47phox−/− CD8-lymphocyte responsiveness to extrinsic cytokine stimulation, we examined cytokine-regulated IL-7R expression. Freshly isolated resting WT and p47phox−/− cells express comparable levels of surface IL-7R. Similarly, viable WT and p47phox−/− cells downregulated IL-7R after overnight culture in IL-7, but retain surface IL-7R after overnight culture in IL-2 (Supplementary Figure 3). Collectively, these data indicate that although cytokine-activated p47phox−/− CD8+ lymphocytes undergo an exaggerated postactivation cell death in vitro, IL-2- and IL-7-triggered common γ-c-receptor pathways in p47phox−/− cells are responsive. In addition, the enhanced rescue of p47phox−/− CD8+ lymphocytes by the combination of IL-7 and GO suggests that NADPH oxidase p47phox and/or NADPH oxidase-mediated ROS may have a preferential role in regulating CD8+-lymphocyte survival.
Resting naïve p47phox−/− CD8 lymphocytes undergo a rapid and profound apoptotic death
To clarify the basis for the exaggerated p47phox−/− CD8+ cell death, we used flow cytometry to assess directly whether there was a difference in p47phox−/− CD8+-lymphocyte apoptosis. The forward and side scatter (FSC/SSC) properties of p47phox−/− cells cultured with IL-2 or IL-7 for 4 h (Figure 3) and 24 h (data not shown) showed significantly fewer p47phox−/− than WT CD8+ cells were viable, and that the majority of the cells outside of the viable gate were in late apoptosis (Annexin+, 7AAD+). Among the cells in the viable gate (solid line arrows), nearly twice as many p47phox−/− as WT cells cultured in IL-2 were in early (Annexin+, 7AAD−) and late (Annexin+, 7AAD+) apoptosis. For cells cultured in IL-7, twice as many p47phox−/− as WT cells were in late apoptosis. Consistent with the viability data in Figure 2, p47phox−/− viable : late apoptotic cell ratios at 4 versus 24 h revealed more p47phox−/− cells continue to die in IL-2 than in IL-7 (1.4±0.07 versus 0.44±0.16 P=0.02 for IL-2, and 1.5±0.13 versus 1±0.21 for IL-7).
Apoptosis of cytokine-activated CD8+ lymphocytes. Fractionated CD8+ cells were cultured in IMDM supplemented with IL-2 or IL-7. At 3 h, cells were removed from the cultures, stained for surface CD8 and Annexin (X-axis) and 7AAD (Y-axis), and assessed by flow cytometry. The dot plots are gated on the CD8+-cell population. The dot plots show the WT (left) and p47phox−/− (right) Annexin (X-axis) versus 7AAD (Y-axis) staining for cells cultured in IL-2 (a) or Il-7 (b). One representative experiment of four is shown. The data show the responses of 3 – 4 mice/experiment. (c) Fractionated CD8+ p47phox−/−and WT lymphocytes were cultured in IMDM supplemented with IL-2 or IL-7, with Z-VAD, as indicated, for 24 h. The total number of viable and nonviable nucleated CD8+ cells was measured using the Guava ViaCount assay, and responses were normalized to the baseline values. The percentage of viable p47phox−/− and WT cells at 24 h (right) is shown. The data shown are the mean±S.E.M. of four independent experiments with three mice/experiment
We also activated p47phox−/− and WT CD8+ lymphocytes in the presence of the soluble pan-caspase inhibitor Z-VAD-FMK, and found there was no difference in the survival of p47phox−/− CD8+ lymphocytes after 24 h (Figure 3c). Collectively, this data indicates that p47phox−/− CD8+ lymphocytes undergo a rapid and profound apoptosis, and the exaggerated in vitro p47phox−/− CD8+-lymphocyte cell death is triggered the upstream of caspase-mediated phenomenon.
Impaired survival of p47phox−/− CD8+ cells is due to an intrinsic apoptotic pathway defect
When purified resting naïve mouse T cells are placed into in vitro culture in the absence of required survival signals, intrinsic apoptotic pathways are initiated and T cells die rapidly due to the loss of control of mitochondrial homeostasis.27, 28 We cultured resting CD8+ lymphocytes from WT and p47phox−/− mice as described and examined antiapoptotic Bcl-2 and proapoptotic Bax protein expression along with mitochondrial transmembrane potential (ΔΨm) and apoptosis to determine whether the exaggerated p47phox−/− CD8+-lymphocyte apoptosis was due to aberrant intrinsic apoptotic pathway function. For these investigations, we performed a multiparametric vitality and apoptosis study using the cyanine dye 1,1′,3,3,3′,3′-hexamethylindodicarbo-cyanine iodide (DiIc1(5)) to assess ΔΨm in combination with Annexin-V and 7-AAD to asses apoptosis. In addition, we used surface staining for CD44 to distinguish survival parameters of naïve (CD44low) versus activated (CD44high) CD8+ cells. Consistent with the apoptosis data in Figure 2, FSC/SSC properties of p47phox−/− cells after 3 – 4 h of culture showed appreciably fewer p47phox−/− CD8 cells were viable (Figure 4). Additionally, as shown in histogram overlays of WT (bold-lined histograms) and p47phox−/− (shaded histograms) CD8+ lymphocytes, we also observed a dramatic and rapid shift of the p47phox−/− CD8+-lymphocyte CD44 profile. Although the baseline CD44 WT and p47phox−/− CD8+-lymphocyte profiles were essentially identical, after just 3 h in culture approximately 1/3 of p47phox−/− CD8+ cells are CD44high suggesting that during in vitro culture there is a preferential loss of naive CD44low p47phox−/− CD8+ lymphocytes. Further, after 24 h, we found that among the remaining viable p47phox−/− CD8+ lymphocytes, the majority of cells were CD44moderate-to-high in each of the culture conditions.
Intrinsic apoptotic pathway defect in cytokine-activated p47phox−/− CD8+ lymphocytes. Fractionated CD8+ p47phox−/− and WT lymphocytes were cultured in IMDM supplemented with IL-2 (a) or IL-7 (b) for 24 h. At 3 h (right) and 24 h (left), cells were removed from the cultures, stained for surface CD8 and CD44, fixed, permeabilized and stained with anti-Bcl-2 or anti-Bax as indicated. The contour plots show the forward scatter verses side scatter cell phenotype and the analysis gates. The adjacent histograms show the flow cytometry phenotype of the CD8+CD44+ p47phox−/− (filled tinted histograms) and WT (bold-lined histograms) cells. The gates on the CD44 histograms correspond to the CD44low, CD44intermediate and CD44high populations used to generate the histograms showing the anti-Bcl-2 or anti-Bax staining for p47phox−/− (shaded histograms) and WT (bold-lined histograms) cells and the isotype control staining for p47phox−/−(dot-lined histogram) and WT (dash-lined histogram) cells. One representative experiment of three is shown. The data shows the responses of three mice/experiment. (c) Proapoptotic conformational change in Bax. Fractionated CD8+ p47phox−/− and WT lymphocytes were cultured in IMDM supplemented with IL-2 for 3 h, and then fixed, permeabilized and stained with conformation-specific anti-Bax (6A7) antibody as indicated. One representative experiment of two is shown. (d) Fractionated CD8+ p47phox−/− and WT lymphocytes were cultured in IMDM supplemented with IL-2 or IL-7 as indicated. At 3 h, cells were removed from the cultures, stained for surface CD8 and CD44, Annexin, PI and mitoprobe. The dot plots are gated on the CD8+-cell population. The dot plots show the CD44low (left) versus CD44high (right) populations of WT and p47phox−/− mitoprobe (Y-axis) versus PI (X-axis) and mitoprobe (Y-axis) versus Annexin (X-axis) staining for cells cultured in IL-2 or Il-7 as indicated. One representative experiment of three is shown. (e) CytochromeC release in p47phox−/− CD8+ lymphocytes at baseline (dash-lined histograms) and 3 h (WT: bold-lined histogram, p47phox−/−: shaded histogram) of culture with IL-2 as indicated. Fractionated CD8+ p47phox−/− and WT lymphocytes were cultured in IMDM supplemented with IL-2 for 3 h, and then permeabilized with digitonin, fixed, immunostained with an anticytochromeC antibody. One representative experiment of three is shown. Numbers indicate percentage of cells (mean±S.E.M.) with low fluorescence (cytochromeC release) for the three replicates. The data show the responses of 3–4 mice/experiment
Baseline Bcl-2 expression for WT and p47phox−/− CD8+ cells were essentially identical (Supplementary Figure 4), however, Bcl-2 expression was rapidly and dramatically reduced in CD44low and CD44high p47phox−/− CD8+ lymphocytes compared to WT lymphocytes cultured in IL-2 for 3 h (Figure 4a). After 24 h, Bcl-2 expression in CD44moderate and CD44high p47phox−/− cells was comparable to WT CD8+ lymphocytes. For cells cultured in IL-7 (Figure 4b), we found that Bcl-2 was rapidly and dramatically reduced in CD44low p47phox−/− CD8+ lymphocytes compared to WT CD8+ lymphocytes after 3 h. However, Bcl-2 was comparable in WT and p47phox−/− CD44high CD8+ lymphocytes at 3 h. After 24 h, we found a small fraction of CD44low p47phox−/− cells cultured with IL-7 retained Bcl-2, and as with IL-2 cultured cells, Bcl-2 expression in CD44moderate and CD44high p47phox−/− cells was comparable to WT. Bax expression in p47phox−/− CD8+ lymphocytes was comparable to WT lymphocytes cultured in IL-2 and in IL-7 for each characterized CD44 population. Additionally, Bax undergoes proapoptotic conformational changes in both WT and p47phox−/− apoptotic CD8+ lymphocytes (Figure 4c). These results indicate that the rapid loss of Bcl-2, preferentially among naïve CD44low cells, contributes to the profound death of p47phox−/− CD8+ lymphocytes in vitro. Furthermore, the ability of IL-7 to partially rescue p47phox−/− CD8+ lymphocytes from an exaggerated cell death in vitro is due in part to its regulation of Bcl-2 protein levels, especially among viable CD44high cells during the initial 3 h of culture.
Finally, when we examined the cells for ΔΨm, we observed that as rapidly as 3 h fewer CD44low and CD44high p47phox−/− CD8+ lymphocytes than WT retained the cyanine iodide dye (MtP+Ann−), indicating significantly more MOMP (Figure 4d, Table 1).27 We also found that compared to IL-7 cultured cells, significantly more CD44low p47phox−/− lymphocytes cultured with IL-2 showed reduced ΔΨm (Table 1). In additional experiments we confirmed that in addition to the loss of ΔΨm, dying p47phox−/− CD8+ lymphocytes also release mitochondrial cytochrome C (Figure 4e). For these analyses, we used a quantitative flow cytometric assay to differentiate cells with intact mitochondria (high fluorescence) from cells that had released mitochondrial cytochrome C (low fluorescence).29, 30 As indicated in the histograms in Figure 4e, the majority of WT lymphocytes had intact mitochondria at baseline and after culture in IL-2. However, although the majority of p47phox−/− lymphocytes also had intact mitochondria at baseline after 3 h in culture, cytochrome C was released in the apoptotic p47phox−/− cells (21%±3 p47phox−/− versus 5±0.1 WT, P=0.005). Collectively, these observations implicate a role for NADPH oxidase p47phox as an upstream effector of the mitochondrial apoptosis pathway via regulation of the antiapoptotic protein Bcl-2.
Survival of p47phox−/− CD8+ cells is dependent upon the lymphoid microenvironment
T-lymphocyte homeostasis is tightly controlled by multiple regulatory checkpoints that restrain T-lymphocyte differentiation within the thymus and expansion in the periphery. Post-thymic export resting naïve T cells are found concentrated in SLOs. However, resting naïve T cells are not stationary but constantly traffic between SLOs in search of antigen, thus providing an effective surveillance system within lymphoid organs. We compared survival of thymic, spleen and LN-derived resting naïve p47phox−/− CD8+ lymphocytes to discern whether the observed survival defect could be linked to the NADPH oxidase p47phox−/− physiologic microenvironment (Figure 5). We found that single positive p47phox−/− CD8+ thymocytes survived as well as WT thymocytes, whereas significantly more splenic resting p47phox−/− CD8+ lymphocytes rapidly succumb during the initial 3–4 h of in vitro culture in IL-2 or IL-7 similar to LN (Figure 2) p47phox−/− CD8+ lymphocytes. However, unlike LN p47phox−/− CD8+ lymphocytes, the majority of the remaining splenic p47phox−/− CD8+ lymphocytes remained viable after 24 h of culture in IL-2 or IL-7. Additionally, there was no difference in the in vitro survival of splenic p47phox−/− CD8+ lymphocytes cultured with IL-2 or IL-7 after 24 h. Consequently, post-thymic survival of resting naïve p47phox−/− CD8+ lymphocytes is highly variable and significantly impacted by NADPH oxidase p47phox−/− SLO microenvironmental factors.
In vitro cytokine-activated thymocyte and splenic lymphocyte survival. Fractionated CD8+ p47phox−/−and WT single positive thymocytes or splenic lymphocytes were cultured in IMDM supplemented with IL-2 or IL-7 as indicated for 24 h. The total number of viable and nonviable nucleated CD8+ cells was measured using the Guava ViaCount assay, and responses were normalized to the baseline values. p47phox−/− responses are indicated by the open histograms and WT responses are indicated by the shaded histograms. (a) The percentage of viable CD8+ p47phox−/− and WT thymocytes at 4 (left) and 24 h (right) in culture. (b) The percentage of viable CD8+ splenic p47phox−/− and WT lymphocytes after 4 (left) and 24 h (right) in culture. The data shown are the mean±S.E.M. of three independent experiments with 3 – 4 mice/experiment. *P<0.001, **P<0.02
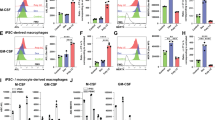
Although WT and p47phox−/− LN CD8+ lymphocytes have comparable baseline Bcl-2 and Bax expression, Bcl-2 rapidly declines in p47phox−/− CD8+ lymphocytes in vitro, while Bax remains stable. We also found that antiapoptotic Mcl-1 expression was comparable in resting naïve WT and p47phox−/− LN CD8+ lymphocytes at baseline and after in vitro culture (data not shown). The observed dysregulation of the intrinsic pathway in vitro lead us to question whether BH3-only proteins that regulate Bcl-231 are aberrant in p47phox−/− CD8+ lymphocytes. We found that baseline Puma and Bim EL expressions were significantly reduced in LN p47phox−/− CD8+ lymphocytes compared to WT lymphocytes. However, after 2 h of in vitro culture, LN p47phox−/− CD8+ lymphocytes expressed significantly more Bim EL and Bim L as well as Puma (Figure 6). For spleen, WT and p47phox−/− CD8+ lymphocytes showed comparable Bim and Puma expressions at baseline (data not shown). However, similar to LN, Bim EL and Puma were significantly induced in vitro in splenic p47phox−/− CD8+ lymphocytes compared to WT (Figure 6). These results suggest that resting naïve p47phox−/− CD8+ within p47phox−/− SLOs are signaled to suppress proapoptotic protein expression.
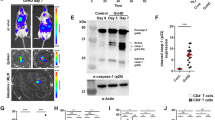
Secondary lymphoid organ factors alter BH3-only Bim and Puma expressions in p47phox−/− CD8+ lymphocytes. Fractionated CD8+ p47phox−/−and WT lymphocytes were cultured in IMDM supplemented with IL-2 for 1.5 h. Baseline and 1.5 h western blot analysis for Bim or Puma expressions were performed as described in the Materials and Methods. Bars show the quantitative analysis (mean±S.E.M.) of lymph node and spleen lymphocyte protein expression. The percent change in LN p47phox−/−CD8+ lymphocyte Bim (a) or Puma (b) expression compared to WT CD8+-lymphocyte protein expression. The percentage induction in Bim (c) or Puma (d) expressions in lymph node p47phox−/− CD8+ lymphocytes at 1.5 h of culture compared to baseline protein expression. The percentage induction in Bim (e) or Puma (f) expressions in splenic p47phox−/− CD8+ lymphocytes at 1.5 h of culture compared to baseline protein expression. The data shown are the mean±S.E.M. of three independent experiments with 3–4 mice/experiment. Representative western blot analysis of Bim or Puma expression in lymph node and spleen are shown adjacent to the bar graphs
To assess the fate of p47phox−/− T cells within normal SLO microenvironments, we adoptively transferred equal numbers of resting WT and p47phox−/− splenocytes into a WT recipient. Similar to what we observed in vitro, the ratio of p47phox−/− : WT lymphocytes recovered from the LNs and spleens of recipient mice 24-h post-adoptive transfer indicates a profound loss of p47phox−/− cells (Figure 7). We also observed a greater loss of p47phox−/− CD8+ cells than CD4+ cells, and found that there was a greater loss of naïve p47phox−/− CD44lowCD8+ lymphocytes than CD44high lymphocytes in vivo.
Unrestrained death of p47phox−/− lymphocytes in WT secondary lymphoid organs. Single cell suspensions of resting LN cells from WT and p47phox−/− mice were generated and pooled. A total of 10 × 106 LN cells were transferred into Ly5.1 congenic recipient mice (n=3). After 24 h, the recipients were killed, and lymph nodes and spleen were harvested and stained for surface markers. Cells were gated on CD45.2+ CD45.1−, and then analyzed for CD4, CD8 and CD44 staining among WT (Thy1.1+, Thy1.2−) or p47phox−/− (Thy1.2+, Thy1.1−) donor T cells in the (a) LNs and (b) spleens. The results show the cell ratios for p47phox−/− : WT donor cells (gray histogram) and the CD4 : CD8 and CD8+ CD44high : CD44low for p47phox−/− or WT cells as indicated. *P<0.01, **P<0.04
In summary, these observations implicate a role for NADPH oxidase p47phox as an upstream effector of the mitochondrial apoptosis pathway via regulation of Bcl-2 protein family members. Furthermore, the increase death of adoptively transferred p47phox−/− CD8+ lymphocytes within WT mouse SLOs suggest that the signals generated within the complex NADPH oxidase p47phox−/− SLO microenvironment restrain CD8+ lymphocyte apoptosis.
Discussion
Previous observations revealed that T cells express each of the NADPH oxidase structural proteins; pg91phox p22phox p47phox and p67phox and TcR stimulation induces low level intracellular NADPH oxidase-dependent H2O2.10 These observations suggested a role of NADPH oxidase-mediated ROS in T-cell function. We report that post-thymic resting naïve p47phox−/− CD8+ cells exhibit an intrinsic survival defect. We link the defect to higher levels of intrinsic apoptotic pathway activity in p47phox−/− CD8+ lymphocytes in vitro and showed that naïve CD44low p47phox−/− lymphocytes have lower Bcl-2 levels that are only partially rescued by prosurvival cytokine IL-7. We also found that in vitro p47phox−/− CD8+-lymphocyte survival could be distinguished by BH3-only Bim and Puma protein expression. Although Bim and Puma were significantly reduced in isolated LN p47phox−/− CD8+ lymphocytes, protein expression in splenic p47phox−/− CD8+ lymphocytes was comparable to WT lymphocytes. Interestingly, both proteins were induced in vitro in LN and splenic p47phox−/− CD8+ lymphocytes indicating that enhanced Bim and Puma expression regulates the rapid in vitro death of p47phox−/− cells.
Supplementing cultures with exogenous IL-7 in vitro normally regulates cellular Bcl-2 proteins to maintain equilibrium of antiapoptotic and proapoptotic proteins. However, even with the addition of IL-7 leading to a demonstrative reduction in resting p47phox−/− lymphocyte death after 24 h in culture, the overall survival of p47phox−/− lymphocytes was only 61%, P<0.0001, of WT cells. Thus, indicating that additional and as yet defined signaling events may be aberrant in p47phox−/− lymphocytes. On the basis of our observation that NADPH oxidase-dependent H2O2 is differentially regulated in activated T-cell blasts,10 we asked whether the aberrant death of p47phox−/− CD8+ cells was due to H2O2 deficiency. To avoid the potential of causing oxidative stress in our in vitro culture model,32 we used GO rather than an H2O2 bolus to restore intracellular H2O2 in p47phox−/− cells. However, one of the inherent limitations of this in vitro experimental design is that we cannot control the timing of H2O2 generation. Subsequently, it is unclear whether the partial rescue of p47phox−/− CD8+ cells is due to a disparity in the timing of H2O2 delivery. The finding that the optimal survival of p47phox−/− CD8+ cells only occurred when both GO and IL-7 were used indicates neither is sufficient to support resting p47phox−/− CD8+-cell survival. However, finding that low-level H2O2 enhances IL-7-mediated p47phox−/− CD8+-cell survival suggests an optimum physiologic H2O2 concentration released at the appropriate time during cytokine stimulation maybe a previously unrecognized pivotal, although partial, signal for lymphocyte survival. We plan to examine these questions in future investigations.
Immune responses are mounted within SLOs to eradicate invading pathogens. However, impaired pathogen clearance in immunocompromised host often results in sustained immune responses. Furthermore, the persistent immune challenge experienced by immunocompromised host undermines the need to maintain a consistent level of naïve T cells capable of regulating homeostasis. Our findings putatively implicate a role for dynamic physiologic cues generated within reactive SLO microenvironments that balance and modulate the transition to effector cells without exhausting naïve CD8+ lymphocytes. We propose NADPH oxidase p47phox and/or NADPH oxidase-mediated ROS is/are a regulator of these adaptive immune phenomenon. The mechanisms appear to involve the regulated suppression of prosurvival members of the Bcl-2 protein family that protect post-thymic naïve CD8+ lymphocytes from Bim and Puma driven apoptosis as well as through mechanisms associated with the removal of in vivo suppressive factor(s) that allow enhanced apoptotic BH3-only protein expression in vitro. This indicates that the characterization of molecular pathways that are controlled by NADPH oxidase p47phox and/or NADPH oxidase-mediated ROS may discern previously unrecognized targets for the development of immunomodulatory therapies.
Materials and Methods
Mice
p47phox-deficient mice have been described.13 Congenic p47phox−/− mice are on a C57BL/6NTac background. WT control mice (C57BL/6NTac) were obtained from Taconic Farms (Hudson, NY). Animal care was provided in accordance with Institutional Animal Care and Use Committee procedures approved by NIAID/NIH. NADPH oxidase-deficient mice were housed in aseptic conditions. Tissues showing gross evidence of infection were discarded and not used for the investigations reported.
Cell isolation
Lymph node single cell suspensions were prepared from peripheral mouse LNs or thymus. CD4+ and CD8+ T cells were negatively selected using the Dynal bead mouse CD4- or CD8-negative isolation kit (Invitrogen Corp., Carlsbad, CA) according to the manufacturer's protocol. The purity of each cell population was >98% as determined by flow cytometry.
Cell culture and stimulation
Lymph node purified CD4 or CD8 T lymphocytes were cultured at a concentration of 1 × 106 cell/ml in IMDM complete : IMDM (Gibco/Invitrogen Corp.) containing 10% FBS (Hyclone Laboratories, Logan, UT), 2.0 mM L-glutamine (Hyclone), 50 μM β-mercaptoethanol (β-ME, Sigma Aldrich, St. Louis, MO) and 100 U/ml penicillin and 10 U/ml streptomycin (Gibco/Invitrogen Corp.) supplemented with 10 U/ml rhIL-2 (Rohmann-LaRoche Inc., Nutley, NJ) or 100 ng/ml IL-7 (PeproTech, Rocky Hill, NJ). For initial experiments, cells were cultured using 10 – 100 U/ml rhIL-2. There was no difference in the relative cell viability differences between WT and p47phox−/− cells using 100 U/ml of IL-2. Subsequently for later experiments, the cells were cultured using 10 U/ml IL-2.
Caspase inhibition
Lymph node purified CD8+ T cells were cultured in IMDM complete and supplemented with 10 U/ml rhIL-2 or 100 ng/ml IL-7, and treated with 50 μM Z-VAD (OMe)-FMK (EMD Chemicals, San Diego, CA).
Cell counts and viability
Resting CD4+ or CD8+ LN cells were incubated with IL-2 or IL-7 as indicated, and cell count and viability were determined. Viable and nonviable lymphocytes from cultures were differentially stained with DNA-binding dyes and the absolute number of viable versus nonviable nucleated cells were quantitated on the basis of cell size and staining properties using the Guava ViaCount (Guava Technologies, Hayward, CA) assay. Cells were diluted with the Guava Viacount (Guava Technologies) reagent in a total volume of 400 μl at the indicated time intervals. Cell counts and viable and dead cell numbers were determined using Guava ViaCount Software on the Guava PCA (Guava Technologies).
Antibodies, immunofluorescent staining and flow cytometry
Fluorescein isothiocyanate (FITC)-conjugated monoclonal antibodies (mAB) against CD11b (Mac-1), Gr-1, B220, CD44, CD25 and (BD Pharmingen,); R-phycoerythrin (PE)-conjugated mAB against B220, CD27, CD62L, CD69 and CD127 (IL-7R; BD Pharmingen); allophycocyanin (APC)-conjugated CD11b, CD3, CD4 and CD8 were used. Cells were stained with the designated FITC (1 : 250), APC (1 : 250) or PE (1 : 500)-conjugated mAb or isotype control for 25 min at room temperature in 1 – 2% FBS – HBSS containing purified rat antimouse CD16/CD32 Fc Block (BD Pharmingen) to minimize nonspecific binding. For the analysis, all cells were resuspended in 1 – 2% FBS – HBSS containing propidium iodide (50 ng/ml; Invitrogen) to distinguish viable cells. Cell acquisition was performed on the Becton Dickinson FACSort or FACSCalibur (BD Biosciences, San Jose, CA) using CellQuest Pro software (BD Biosciences). Analysis was performed using FlowJo software (FlowJo, LCC, Ashland, OR).
Adoptive transfer
Single cell suspensions were made from LNs from p47phox−/− mice (CD45.2 Thy 1.2) and Thy1.1+ WT C57/BL6 mice. Ten million of each were injected i.v. into CD45.1 WT C57/BL6 recipients. LNs and spleen were harvested from recipients at 24 h and stained for surface markers CD45.1 PE, Thy.1 PerCp, CD44 FITC (BD Pharmingen), CD4 Pacific Blue, CD8 Alexa Flour 700, CD45.2 Alexa Flour 750 and Thy1.2 Pe-Cy5 (eBioscience, San Diego, CA). Cells were gated on CD45.2+ CD45.1−, and then analyzed for CD4, CD8 and CD44 staining among WT (Thy1.1+ and Thy1.2−) or KO (Thy1.2+ and Thy1.1−) donors. Cell acquisition was performed on the Becton Dickinson LSR II (BD Biosciences) using CellQuest Pro software (BD Biosciences). Analysis was performed using FlowJo software (FlowJo, LCC, Ashland, OR).
BrdU stimulation
p47phox−/− and WT mice were fed with BrdU (BD Pharmingen) in their drinking water at a concentration of 1 mg/ml for 5 days. LNs were harvested on day 5. Whole LN cell populations were stained with anti-CD4, CD8, CD44, B220 and BrdU antibodies (BD Pharmingen). Cell acquisition was performed on the Becton Dickinson LSRII (BD Biosciences) using CellQuest Pro software (BD Biosciences). Analysis was performed using FlowJo software (FlowJo, LCC, Ashland, OR).
Bcl-2 and Bax staining
Cells were washed twice in 1% FBS/PBS and surface stained for CD8 (1 : 500) and CD44 (1 : 125 – 500) as indicated. Cells were fixed according to the (Cytofix/Cytoperm Plus Kit, BD Pharmingen) manufacturer's protocol. Cells were stained for intracellular Bcl-2 (BD Pharmingen) or Bax (Santa Cruz, Santa Cruz, CA) according to the manufacturer's protocol. Conformational change in the Bax protein was assessed by intracellular immunostaining using a specific antibody that recognizes only the proapoptotic conformation : anti-Bax (6A7; BD Pharmingen) using the method described by Gómez-Benito et al.29 Briefly, cells were cultured with IL-2 supplemented medium for 3 h. Then, 1 × 106 cells were fixed with 0.5% paraformaldehyde in PBS for15 min at 4°C and incubated for 25 min at room temperature with 0.5 μg of anti-Bax or a mouse IgG isotype control (BD Pharmingen) in 100 μl of PBS containing 0.1% saponin and 5% goat serum. Cells were washed with 0.03% saponin in PBS and incubated with a FITC-labeled antimouse IgG antibody (BD Pharmingen) at room temperature. Cell acquisition was performed on the Becton Dickinson FACSCalibur (BD Biosciences) using CellQuest Pro software (BD Biosciences). Analysis was performed using FlowJo software (FlowJo, LCC, Ashland, OR).
Cytochrome C release
Quantitative analysis of cytochrome C release from mitochondria was assessed by a modification of the method described by Waterhouse and Trapani.29, 30 Briefly, cells were cultured with IL-2 supplemented medium for 3 h. Then, 1 × 106 cells were permeabilized with 100 μl of digitonin (50 μg/ml in PBS containing 100 mM KCl) for 5 min on ice, fixed in 4% paraformaldehyde in PBS for 20 min at room temperature, and resuspended in 3% bovine serum albumin, 0.05% saponin in PBS (blocking buffer). Cells were incubated overnight at 4°C with a 1 : 500 dilution of anti-cytochrome C antibody (InnoCyte™ Flow Cytometric Cytochrome C Release Kit, Calbiochem, EMD Chemicals, Inc., Gibbstown, NJ) in blocking buffer, washed, and then incubated with a 1 : 300 dilution of FITC-labeled anti-mouse IgG antibody (InnoCyte™ Flow Cytometric Cytochrome C Release Kit, Calbiochem). Control cells were stained with a 1 : 300 dilution of the FITC-labeled anti-mouse IgG antibody in the absence of a primary antibody. Cell acquisition was performed on the Becton Dickinson FACSCalibur (BD Biosciences) using CellQuest Pro software (BD Biosciences). Analysis was performed using FlowJo software (FlowJo).
Cell death analysis
Lymph node purified CD8+ T cells were cultured as indicated. Cells were harvested at the designated time, washed with 1%FBS/PBS and stained for surface CD8 and CD44 (BD Pharmingen). Mitochondrial membrane integrity and cell death were determined using the Mitoprobe kit (Invitrogen) or the Annexin V: PE Apoptosis Detection Kit I (BD Pharmalgen) according to the manufactures protocols.
Glucose oxidase stimulation
Lymph node purified CD8+ T cells were cultured in IMDM complete without β-ME and supplemented with 10 U/ml rhIL-2 or 100 ng/ml IL-7. Cells were treated with the following range of GO (Sigma-Aldrich): log 10 concentration, 10 ng/ml – 1 pg/ml and log2 concentrations, 0.3 – 1.2 pg/ml. Cells counts were determined at 24 h using Guava ViaCount Software on the Guava PCA (Guava Technologies).
Cell fractionation and Western blot analysis
After CD8 isolation, cells were counted and resuspended at 1 × 106 cells/ml in IMDM complete with 10 U/ml rhIL-2 (Rohmann-LaRoche Inc.) for 1.5 h, and then washed with cold PBS. Cells were lysed in ice-cold mammalian protein extraction reagent (Pierce Biotechnology, Rockford IL), 1X mammalian protease inhibitor (Sigma-Aldrich) and 5 mM EDTA followed by sonication for 10 min. Insoluble material was removed by centrifugation at 12 000 × g at 4°C for 10 min. Equivalent amounts of protein were denatured in Laemmli buffer for direct resolution by 10–20% SDS-polyacrylamide gel electrophoresis (SDS-PAGE), and transferred to a nitrocellulose membrane (Millipore Corporation, Billerica, MA). Immunoblotting was performed using anti-Puma Ab, anti-Bim Ab, anti-BMF Ab, (Cell Signaling Technology, Danvers, MA), anti-Mcl-1 Ab, (Abcam Inc., Cambridge, MA) anti-actin Ab (Sigma-Aldrich), HRP-conjugated antirabbit Ab and HRP-conjugated antimouse Ab (GE Healthcare, Piscataway, NJ). Immunoreactive proteins were visualized using an ECL detection kit (GE Healthcare) upon exposure to BioMax™ light film (Kodak). For the relative quantification of the proteins, scanned images were analyzed using Image J.33
Statistical analysis
Means and S.E.M. of cell count and viability were determined. Differences between the group means were analyzed by the Student's t-test. (Prism 4, GraphPad Software Inc. San Diego, CA).
Abbreviations
- ΔΨμ:
-
mitochondrial transmembrane potential
- BrdU:
-
5-bromo-2′deoxyuridine
- CGD:
-
chronic Granulomatous Disease
- FSC/SSC:
-
forward and side scatter
- GO:
-
glucose oxidase
- H2O2:
-
hydrogen peroxide
- LNs:
-
lymph nodes
- MOMP:
-
mitochondrial outer membrane permeabilization
- NADPH:
-
nicotinamide adenine dinucleotide phosphate
- p47phox−/−:
-
oxidase, p47phox deficient
- ROS:
-
reactive oxygen species
- SLOs:
-
secondary lymphoid organs
References
Rathmell JC, Thompson CB . Pathways of apoptosis in lymphocyte development, homeostasis, and disease. Cell 2002; 109 (Suppl): S97–S107.
Guimond M, Fry TJ, Mackall CL . Cytokine signals in T-cell homeostasis. J Immunother 2005; 28: 289–294.
Van Parijs L, Abbas AK . Homeostasis and self-tolerance in the immune system: turning lymphocytes off. Science (New York, NY) 1998; 280: 243–248.
Walker LS, Abbas AK . The enemy within: keeping self-reactive T cells at bay in the periphery. Nat Rev 2002; 2: 11–19.
Marrack P, Bender J, Hildeman D, Jordan M, Mitchell T, Murakami M et al. Homeostasis of alpha beta TCR+ T cells. Nat Immunol 2000; 1: 107–111.
Marrack P, Kappler J . Control of T cell viability. Annu Rev Immunol 2004; 22: 765–787.
Babior BM . The respiratory burst oxidase. Adv Enzymol Relat Areas Mol Biol 1992; 65: 49–95.
Nauseef WM . Assembly of the phagocyte NADPH oxidase. Histochem Cell Biol 2004; 122: 277–291.
Sauer H, Wartenberg M, Hescheler J . Reactive oxygen species as intracellular messengers during cell growth and differentiation. Cell Physiol Biochem 2001; 11: 173–186.
Jackson SH, Devadas S, Kwon J, Pinto LA, Williams MS . T cells express a phagocyte-type NADPH oxidase that is activated after T cell receptor stimulation. Nat Immunol 2004; 5: 818–827.
Assari T . Chronic Granulomatous Disease; fundamental stages in our understanding of CGD. Med Immunol (London, England) 2006; 5: 4.
Rosenzweig SD . Inflammatory Manifestations in Chronic Granulomatous Disease (CGD). J Clin Immunol 2008; 28 (Suppl 1): S67–S72.
Jackson SH, Gallin JI, Holland SM . The p47phox mouse knock-out model of chronic granulomatous disease. J Exp Med 1995; 182: 751–758.
Hildeman DA . Regulation of T-cell apoptosis by reactive oxygen species. Free Radic Biol Med 2004; 36: 1496–1504.
Hildeman DA, Mitchell T, Teague TK, Henson P, Day BJ, Kappler J et al. Reactive oxygen species regulate activation-induced T cell apoptosis. Immunity 1999; 10: 735–744.
Hockenbery DM, Oltvai ZN, Yin XM, Milliman CL, Korsmeyer SJ . Bcl-2 functions in an antioxidant pathway to prevent apoptosis. Cell 1993; 75: 241–251.
Vella A, Teague TK, Ihle J, Kappler J, Marrack P . Interleukin 4 (IL-4) or IL-7 prevents the death of resting T cells: stat6 is probably not required for the effect of IL-4. J Exp Med 1997; 186: 325–330.
Tan JT, Dudl E, LeRoy E, Murray R, Sprent J, Weinberg KI et al. IL-7 is critical for homeostatic proliferation and survival of naive T cells. Proc Natl Acad Sci USA 2001; 98: 8732–8737.
Ku CC, Murakami M, Sakamoto A, Kappler J, Marrack P . Control of homeostasis of CD8+ memory T cells by opposing cytokines. Science (New York, NY) 2000; 288: 675–678.
Fry TJ, Mackall CL . The many faces of IL-7: from lymphopoiesis to peripheral T cell maintenance. J Immunol 2005; 174: 6571–6576.
Kishimoto H, Sprent J . Strong TCR ligation without costimulation causes rapid onset of Fas-dependent apoptosis of naive murine CD4+ T cells. J Immunol 1999; 163: 1817–1826.
Jiang Q, Li WQ, Aiello FB, Mazzucchelli R, Asefa B, Khaled AR et al. Cell biology of IL-7, a key lymphotrophin. Cytokine Growth Factor Rev 2005; 16: 513–533.
Bentley R . Glucose oxidase. In: Boyer PD, Lardy H, Myrbäck K (eds). The Enzymes, 2nd edn. Vol. 7, Academic Press: New York, 1963, pp 567–586.
Pazur JH . Glucose oxidase. In: Cowolick SP, Kaplan NO (eds). Methods in Enzymology, Vol. 9, Academic Press: New York, 1966, pp 82–87.
Kovanen PE, Leonard WJ . Cytokines and immunodeficiency diseases: critical roles of the gamma(c)-dependent cytokines interleukins 2, 4, 7, 9, 15, and 21, and their signaling pathways. Immunol Rev 2004; 202: 67–83.
Park JH, Yu Q, Erman B, Appelbaum JS, Montoya-Durango D, Grimes HL et al. Suppression of IL7Ralpha transcription by IL-7 and other prosurvival cytokines: a novel mechanism for maximizing IL-7-dependent T cell survival. Immunity 2004; 21: 289–302.
Spierings D, McStay G, Saleh M, Bender C, Chipuk J, Maurer U et al. Connected to death: the (unexpurgated) mitochondrial pathway of apoptosis. Science (New York, NY) 2005; 310: 66–67.
Green DR, Kroemer G . The pathophysiology of mitochondrial cell death. Science (New York, NY) 2004; 305: 626–629.
Gomez-Benito M, Marzo I, Anel A, Naval J . Farnesyltransferase inhibitor BMS-214662 induces apoptosis in myeloma cells through PUMA up-regulation, Bax and Bak activation, and Mcl-1 elimination. Mol Pharmacol 2005; 67: 1991–1998.
Waterhouse NJ, Trapani JA . A new quantitative assay for cytochrome c release in apoptotic cells. Cell Death Differ 2003; 10: 853–855.
Youle RJ, Strasser A . The BCL-2 protein family: opposing activities that mediate cell death. Nat Rev Mol Cell Biol 2008; 9: 47–59.
Antunes F, Cadenas E, Brunk UT . Apoptosis induced by exposure to a low steady-state concentration of H2O2 is a consequence of lysosomal rupture. Biochem J 2001; 356 (Pt 2): 549–555.
Rasband WS . ImageJ, US National Institutes of Health: Bethesda, Maryland, USA, http://rsb.info.nih.gov/ij/, 1997–2007.
Acknowledgements
We thank Kevin Gardner and Richard Youle for helpful discussions and critique of an earlier draft of this manuscript. We also thank Harry Malech and Michael Davis for careful review of this manuscript. This research was supported by the Division of Intramural Research of the National Institutes of Health/National Institute of Allergy and Infectious Diseases.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by SJ Martin
Supplementary Information accompanies the paper on Cell Death and Differentiation website (http://www.nature.com/cdd)
Rights and permissions
About this article
Cite this article
Donaldson, M., Antignani, A., Milner, J. et al. p47phox-deficient immune microenvironment signals dysregulate naive T-cell apoptosis. Cell Death Differ 16, 125–138 (2009). https://doi.org/10.1038/cdd.2008.129
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cdd.2008.129
Keywords
This article is cited by
-
Clinical and Molecular Features of Chronic Granulomatous Disease in Mainland China and a XL-CGD Female Infant Patient After Prenatal Diagnosis
Journal of Clinical Immunology (2019)
-
PP2A-dependent control of transcriptionally active FOXO3a in CD8+ central memory lymphocyte survival requires p47phox
Cell Death & Disease (2012)