Abstract
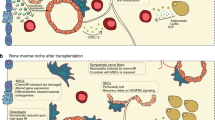
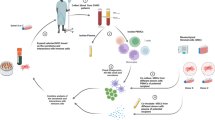
Poor graft function (PGF), including early and late PGF, is a serious complication following allotransplant. We recently reported that bone marrow microenvironment abnormalities may occur in cases of late PGF. Whether these abnormalities occur in early PGF remains unknown. To answer this question, we performed a nested case–control study comparing cellular elements of the bone marrow microenvironment in 10 subjects with early PGF, 30 subjects with late PGF and 40 subjects without PGF. Bone marrow endosteal cells, perivascular cells and endothelial cells were analyzed by flow cytometry and by hematoxylin–eosin and immunohistochemical staining in situ. Subjects with early and late PGF had similar abnormalities in these cell types compared with transplant recipients without PGF. However, none of the aforementioned elements of the bone marrow microenvironment were significantly different between early and late PGF patients. Our data suggest that similar abnormalities in the bone marrow microenvironment may occur in early and late PGF post allotransplant. Cellular approaches, such as the administration of mesenchymal stem cells, promise to be beneficial therapeutic strategies in patients with early or late PGF.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Larocca A, Piaggio G, Podestà M, Pitto A, Bruno B, Di Grazia C et al. Boost of CD34+-selected peripheral blood cells without further conditioning in patients with poor graft function following allogeneic stem cell transplantation. Haematologica 2006; 91: 935–940.
Kong Y, Chang YJ, Wang YZ, Chen YH, Han W, Wang Y et al. Association of an impaired bone marrow microenvironment with secondary poor graft function after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2013; 19: 1465–1473.
Liu X, Wu M, Peng Y, Chen X, Sun J, Huang F et al. Improvement in poor graft function after allogeneic hematopoietic stem cell transplantation upon administration of mesenchymal stem cells from third-party donors: a pilot prospective study. Cell Transplant 2014; 23: 1087–1098.
Sun YQ, He GL, Chang YJ, Xu LP, Zhang XH, Han W et al. The incidence, risk factors, and outcomes of primary poor graft function after unmanipulated haploidentical stem cell transplantation. Ann Hematol 2015; 94: 1699–1705.
Chang YJ, Zhao XY, Xu LP, Zhang XH, Wang Y, Han W et al. Donor-specific anti-human leukocyte antigen antibodies were associated with primary graft failure after unmanipulated haploidentical blood and marrow transplantation: a prospective study with randomly assigned training and validation sets. J Hematol Oncol 2015; 8: 84.
Reisner Y, Hagin D, Martelli MF . Haploidentical hematopoietic transplantation: current status and future perspectives. Blood 2011; 118: 6006–6017.
Olsson R, Remberger M, Schaffer M, Berggren DM, Svahn bone marrow, Mattsson J et al. Graft failure in the modern era of allogeneic hematopoietic SCT. Bone Marrow Transplant 2013; 48: 537–543.
Askaa B, Fischer-Nielsen A, Vindelov L, Haastrup EK, Sengelov H . Treatment of poor graft function after allogeneic hematopoietic cell transplantation with a booster of CD34-selected cells infused without conditioning. Bone Marrow Transplant 2014; 49: 720–721.
Klyuchnikov E, El-Cheikh J, Sputtek A, Lioznov M, Calmels B, Furst S et al. CD34(+)-selected stem cell boost without further conditioning for poor graft function after allogeneic stem cell transplantation in patients with hematological malignancies. Biol Blood Marrow Transplant 2014; 20: 382–386.
Stasia A, Ghiso A, Galaverna F, RaiolaAM, Gualandi F, Luchetti S et al. CD34 selected cells for the treatment of poor graft function after allogeneic stem cell transplantation. Biol Blood Marrow Transplant 2014; 20: 1440–1443.
Scadden DT . The stem-cell niche as an entity of action. Nature 2006; 441: 1075–1079.
Calvi LM, Adams GB, Weibrecht KW, Weber JM, Olson DP, Knight MC et al. Osteoblastic cells regulate the haematopoietic stem cell niche. Nature 2003; 425: 841–846.
Hooper AT, Butler JM, Nolan DJ, Kranz A, Iida K, Kobayashi M et al. Engraftment and reconstitution of hematopoiesis is dependent on VEGFR2-mediated regeneration of sinusoidal endothelial cells. Cell Stem Cell 2009; 4: 263–274.
Ding L, Saunders TL, Enikolopov G, Morrison SJ . Endothelial and perivascular cells maintain haematopoietic stem cells. Nature 2012; 481: 457–462.
Kong Y, Hu Y, Zhang XH, Wang YZ, Mo XD, Zhang YY et al. Association between an impaired bone marrow vascular microenvironment and prolonged isolated thrombocytopenia after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2014; 20: 1190–1197.
Wacholder S, Silverman DT, McLaughlin JK, Mandel JS . Selection of controls in case-control studies. III. Design options. Am J Epidemiol 1992; 135: 1042–1050.
Wang Y, Wu DP, Liu QF, Qin YZ, Wang JB, Xu LP et al. In adults with t(8;21)AML, posttransplant RUNX1/RUNX1T1-based MRD monitoring, rather than c-KIT mutations,allows further risk stratification. Blood 2014; 124: 1880–1886.
Huang XJ, Zhu HH, Chang YJ, Xu LP, Liu DH, Zhang XH et al. The superiority of haploidentical related stem cell transplantation over chemotherapy alone as postremission treatment for patients with intermediate- or high-risk acute myeloid leukemia in first complete remission. Blood 2012; 119: 5584–5590.
Yan CH, Liu DH, Liu KY, Xu LP, Liu YR, Chen H et al. Risk stratification-directed donor lymphocyte infusion could reduce relapse of standard-risk acute leukemia patients after allogeneic hematopoietic stem cell transplantation. Blood 2012; 119: 3256–3262.
Xu LP, Huang XJ, Guo NL, Ren HY, Zhang YC, Lu DP . [Detection of cytomegalovirus infection by polymerase chain reaction in hematopoietic stem cell transplantation recipients]. Zhonghua Xue Ye Xue Za Zhi 2003; 24: 407–409.
Dominietto A, Raiola AM, van Lint MT, Lamparelli T, Gualandi F, Berisso G et al. Factors influencing haematological recovery after allogeneic haemopoietic stem cell transplants: graft-versus-host disease, donor type, cytomegalovirus infections and cell dose. Br J Haematol 2001; 112: 219–227.
Shono Y, Ueha S, Wang Y, Abe J, Kurachi M, Matsuno Y et al. Bone marrow graft versus-host disease: early destruction of hematopoietic niche after MHC mismatched hematopoietic stem cell transplantation. Blood 2010; 115: 5401–5411.
Yao Y, Song X, Cheng H, Tang G, Hu X, Zhou H et al. Dysfunction of bone marrow vascular niche in acute graft-versus-host disease after MHC-haploidentical bone marrow transplantation. PLoS ONE 2014; 9: e104607.
Simmons P, Kaushansky K, Torok-Storb B . Mechanisms of cytomegalovirus-mediated myelosuppression: perturbation of stromal cell function versus direct infection of myeloid cells. Proc Natl Acad Sci USA 1990; 87: 1386–1390.
Méndez-Ferrer S, Michurina TV, Ferraro F, Mazloom AR, Macarthur BD, Lira SA et al. Mesenchymal and haematopoietic stem cells form a unique bone marrow niche. Nature 2010; 466: 829–834.
Ball LM, Bernardo ME, Roelofs H, Lankester A, Cometa A, Egeler RM et al. Cotransplantation of ex vivo expanded mesenchymal stem cells accelerates lymphocyte recovery and may reduce the risk of graft failure in haploidentical hematopoietic stem-cell transplantation. Blood 2007; 110: 2764–2767.
Acknowledgements
Professor Robert Peter Gale (Imperial College London) kindly reviewed the manuscript. This work was supported by the National Natural Science Foundation of China (grant nos 81370638, 81570127, 81530046 and 81230013), the Beijing Municipal Science and Technology Program (grant nos Z151100004015164, Z151100001615020, Z141100000214011), the National High Technology Research Development Program of China (grant no. SS2013AA020104). We thank Professor Qing Ge for helpful discussions and suggestions. The language editing service American Journal Experts (www.americanjournalexperts.com) provided English editorial assistance to the authors during the preparation of this manuscript. We thank all the core facilities at Peking University Institute of Hematology for the sample collection.
Author contributions
X-JH designed the study and supervised the analyses and manuscript preparation. YK performed the research, analyzed and interpreted the data, performed statistical analysis and wrote the manuscript. All the other authors participated in the collection of patients’ data. All the authors agreed to submit the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kong, Y., Wang, YT., Hu, Y. et al. The bone marrow microenvironment is similarly impaired in allogeneic hematopoietic stem cell transplantation patients with early and late poor graft function. Bone Marrow Transplant 51, 249–255 (2016). https://doi.org/10.1038/bmt.2015.229
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2015.229
This article is cited by
-
Comparison of immunosuppressant regimens in salvage cord blood transplantation for graft failure after allogeneic hematopoietic stem cell transplantation
Bone Marrow Transplantation (2021)
-
PEDF promotes the repair of bone marrow endothelial cell injury and accelerates hematopoietic reconstruction after bone marrow transplantation
Journal of Biomedical Science (2020)
-
Comparison of the outcomes after haploidentical and cord blood salvage transplantations for graft failure following allogeneic hematopoietic stem cell transplantation
Bone Marrow Transplantation (2020)
-
Update of the “Beijing Protocol” haplo-identical hematopoietic stem cell transplantation
Bone Marrow Transplantation (2019)
-
Aberrant T cell responses in the bone marrow microenvironment of patients with poor graft function after allogeneic hematopoietic stem cell transplantation
Journal of Translational Medicine (2017)