Abstract
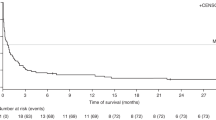
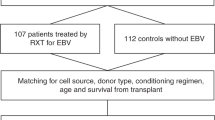
The mortality associated with post-transplant lymphoproliferative disorder (PTLD) induced by EBV infection can be reduced by monitoring EBV by polymerase-chain-reaction and rituximab given pre-emptively. We performed a retrospective analysis of the risk factors for the occurrence of EBV infection/disease and EBV-related mortality among 273 consecutive recipients of a T-cell-depleted allo-SCT during two periods: (a) before the implementation of a comprehensive protocol (2006–2008) and (b) afterwards (2009–2011). EBV infection was detected in 61 (22%) cases, and 28 cases were considered to have had EBV disease. Treatment with antithymocyte globulin was the most important risk factor (odds ratio (OR) 2.4; 95% confidence interval (CI) 1.3–4.2, P=0.001). After implementation of the protocol, in patients experiencing EBV infection, pre-emptive therapy was started more often and sooner (median 3 vs 6 days, P=0.002). Moreover, there were fewer cases of monomorphic PTLD (4/33 (12%) vs 11/28 (39%), P=0.01), and the EBV-related mortality was lower for patients experiencing EBV infection (2/33 (6%) vs 8/28 (29%), OR 0.2; 95% CI 0.05–0.9, P=0.03). The EBV protocol proved feasible and resulted in faster initiation of pre-emptive therapy, the diagnosis in an earlier stage of EBV disease, and decreased EBV-related mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Styczynski J, Einsele H, Gil L, Ljungman P . Outcome of treatment of Epstein-Barr virus-related post-transplant lymphoproliferative disorder in hematopoietic stem cell recipients: a comprehensive review of reported cases. Transpl Infect Dis 2009; 11: 383–392.
Loren AW, Porter DL, Stadtmauer EA, Tsai DE . Post-transplant lymphoproliferative disorder: a review. Bone Marrow Transplant 2003; 31: 145–155.
Heslop HE . How I treat EBV lymphoproliferation. Blood 2009; 114: 4002–4008.
Landgren O, Gilbert ES, Rizzo JD, Socie G, Banks PM, Sobocinski KA et al. Risk factors for lymphoproliferative disorders after allogeneic hematopoietic cell transplantation. Blood 2009; 113: 4992–5001.
Hoegh-Petersen M, Goodyear D, Geddes MN, Liu S, Ugarte-Torres A, Liu Y et al. High incidence of post transplant lymphoproliferative disorder after antithymocyte globulin-based conditioning and ineffective prediction by day 28 EBV-specific T lymphocyte counts. Bone Marrow Transplant 2011; 46: 1104–1112.
Cohen J, Gandhi M, Naik P, Cubitt D, Rao K, Thaker U et al. Increased incidence of EBV-related disease following paediatric stem cell transplantation with reduced-intensity conditioning. Br J Haematol 2005; 129: 229–239.
Sundin M, Le Blanc K, Ringden O, Barkholt L, Omazic B, Lergin C et al. The role of HLA mismatch, splenectomy and recipient Epstein-Barr virus seronegativity as risk factors in post-transplant lymphoproliferative disorder following allogeneic hematopoietic stem cell transplantation. Haematologica 2006; 91: 1059–1067.
Reddy N, Rezvani K, Barrett AJ, Savani BN . Strategies to Prevent EBV Reactivation and Posttransplant Lymphoproliferative Disorders (PTLD) after Allogeneic Stem Cell Transplantation in High-Risk Patients. Biol Blood Marrow Transplant 2011; 17: 591–597.
Coppoletta S, Tedone E, Galano B, Soracco M, Raiola AM, Lamparelli T et al. Rituximab treatment for Epstein-Barr virus DNAemia after alternative-donor hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2011; 17: 901–907.
Kuehnle I, Huls MH, Liu Z, Semmelmann M, Krance RA, Brenner MK et al. CD20 monoclonal antibody (rituximab) for therapy of Epstein-Barr virus lymphoma after hemopoietic stem-cell transplantation. Blood 2000; 95: 1502–1505.
Ocheni S, Kroeger N, Zabelina T, Sobottka I, Ayuk F, Wolschke C et al. EBV reactivation and post transplant lymphoproliferative disorders following allogeneic SCT. Bone Marrow Transplant 2008; 42: 181–186.
Doubrovina E, Oflaz-Sozmen B, Prockop SE, Kernan NA, Abramson S, Teruya-Feldstein J et al. Adoptive immunotherapy with unselected or EBV-specific T cells for biopsy-proven EBV+ lymphomas after allogeneic hematopoietic cell transplantation. Blood 2012; 119: 2644–2656.
Weinstock DM, Ambrossi GG, Brennan C, Kiehn TE, Jakubowski A . Preemptive diagnosis and treatment of Epstein-Barr virus-associated post transplant lymphoproliferative disorder after hematopoietic stem cell transplant: an approach in development. Bone Marrow Transplant 2006; 37: 539–546.
Styczynski J, Reusser P, Einsele H, de la Camara R, Cordonnier C, Ward KN et al. Management of HSV, VZV and EBV infections in patients with hematological malignancies and after SCT: guidelines from the Second European Conference on Infections in Leukemia. Bone Marrow Transplant 2009; 43: 757–770.
Kinch A, Oberg G, Arvidson J, Falk KI, Linde A, Pauksens K . Post-transplant lymphoproliferative disease and other Epstein-Barr virus diseases in allogeneic haematopoietic stem cell transplantation after introduction of monitoring of viral load by polymerase chain reaction. Scand J Infect Dis 2007; 39: 235–244.
van Esser JW, Niesters HG, Thijsen SF, Meijer E, Osterhaus AD, Wolthers KC et al. Molecular quantification of viral load in plasma allows for fast and accurate prediction of response to therapy of Epstein-Barr virus-associated lymphoproliferative disease after allogeneic stem cell transplantation. Br J Haematol 2001; 113: 814–821.
Omar H, Hagglund H, Gustafsson-Jernberg A, LeBlanc K, Mattsson J, Remberger M et al. Targeted monitoring of patients at high risk of post-transplant lymphoproliferative disease by quantitative Epstein-Barr virus polymerase chain reaction. Transpl Infect Dis 2009; 11: 393–399.
van Esser JW, Niesters HG, van der HB, Meijer E, Osterhaus AD, Gratama JW et al. Prevention of Epstein-Barr virus-lymphoproliferative disease by molecular monitoring and preemptive rituximab in high-risk patients after allogeneic stem cell transplantation. Blood 2002; 99: 4364–4369.
Worth A, Conyers R, Cohen J, Jagani M, Chiesa R, Rao K et al. Pre-emptive rituximab based on viraemia and T cell reconstitution: a highly effective strategy for the prevention of Epstein-Barr virus-associated lymphoproliferative disease following stem cell transplantation. Br J Haematol 2011; 155: 377–385.
Faraci M, Caviglia I, Morreale G, Lanino E, Cuzzubbo D, Giardino S et al. Viral-load and B-lymphocyte monitoring of EBV reactivation after allogeneic hemopoietic SCT in children. Bone Marrow Transplant 2010; 45: 1052–1055.
Schattenberg A, van der Meer A, Preijers F, Schaap N, Rinkes M, van der Maazen R et al. Addition of ATG to the conditioning regimen is a major determinant for outcome after transplantation with partially lymphocyte-depleted grafts from voluntary unrelated donors. Bone Marrow Transplant 2004; 33: 1115–1121.
van der Velden WJ, Herbers AH, Feuth T, Schaap NP, Donnelly JP, Blijlevens NM . Intestinal damage determines the inflammatory response and early complications in patients receiving conditioning for a stem cell transplantation. PLoS One 2010; 5: e15156.
van der Velden WJ, Blijlevens NM, Maas FM, Schaap NP, Jansen JH, van der Reijden BA et al. NOD2 polymorphisms predict severe acute graft-versus-host disease and treatment-related mortality in T-cell-depleted haematopoietic stem cell transplantation. Bone Marrow Transplant 2009; 44: 243–248.
Schaap N, Schattenberg A, Bar B, Preijers F, Geurts van Kessel A, van der Maazen R et al. Outcome of transplantation for standard-risk leukaemia with grafts depleted of lymphocytes after conditioning with an intensified regimen. Br J Haematol 1997; 98: 750–759.
Niesters HG, van Esser J, Fries E, Wolthers KC, Cornelissen J, Osterhaus AD . Development of a real-time quantitative assay for detection of Epstein-Barr virus. J Clin Microbiol 2000; 38: 712–715.
Carpenter B, Haque T, Dimopoulou M, Atkinson C, Roughton M, Grace S et al. Incidence and dynamics of Epstein-Barr virus reactivation after alemtuzumab-based conditioning for allogeneic hematopoietic stem-cell transplantation. Transplantation 2010; 90: 564–570.
Wolach O, Shpilberg O, Lahav M . Neutropenia after rituximab treatment: new insights on a late complication. Curr Opin Hematol 2012; 19: 32–38.
Koo S, Baden LR . Infectious complications associated with immunomodulating monoclonal antibodies used in the treatment of hematologic malignancy. J Natl Compr Canc Netw 2008; 6: 202–213.
Kang HJ, Park JS, Kim DW, Lee J, Jeong YJ, Choi SM et al. Adverse pulmonary reactions associated with the use of monoclonal antibodies in cancer patients. Respir Med 2012; 106: 443–450.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Bone Marrow Transplantation website
Rights and permissions
About this article
Cite this article
van der Velden, W., Mori, T., Stevens, W. et al. Reduced PTLD-related mortality in patients experiencing EBV infection following allo-SCT after the introduction of a protocol incorporating pre-emptive rituximab. Bone Marrow Transplant 48, 1465–1471 (2013). https://doi.org/10.1038/bmt.2013.84
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2013.84
Keywords
This article is cited by
-
Post-transplantation lymphoproliferative disorder after haematopoietic stem cell transplantation
Annals of Hematology (2021)
-
Epstein–Barr virus reactivation after allogeneic hematopoietic stem cell transplantation: multifactorial impact on transplant outcomes
Bone Marrow Transplantation (2020)
-
A retrospective analysis on anti-CD20 antibody–treated Epstein–Barr virus–related posttransplantation lymphoproliferative disorder following ATG-based haploidentical T-replete hematopoietic stem cell transplantation
Annals of Hematology (2020)
-
Second Malignancies after Hematopoietic Stem Cell Transplantation
Current Treatment Options in Oncology (2018)
-
Greatly reduced risk of EBV reactivation in rituximab-experienced recipients of alemtuzumab-conditioned allogeneic HSCT
Bone Marrow Transplantation (2016)