Abstract
Background:
MicroRNAs alter multiple cell processes and thus influence tumour carcinogenesis and progression. MiR-100 and miR-99a have been reported to be aberrantly expressed in acute leukaemia. In this study, we focused on their functions in acute lymphoblastic leukaemia (ALL) and the molecular networks in which they are involved.
Methods:
MiR-100 and miR-99a expression levels were measured in acute leukaemia patients by qRT–PCR. Kaplan−Meier analysis and log-rank tests were used to calculate the survival rate. Three human ALL cell lines were studied. Apoptosis and proliferation were analysed using siRNA transfection, western blot and flow cytometry.
Results:
In vivo, miR-100 and miR-99a were down-regulated in 111 ALL patients, especially in high-risk groups; their expression levels were correlated with the patient’s 5-year survival. In vitro, the restoration of miR-100 and miR-99a in ALL cells suppressed cell proliferation and increased dexamethasone-induced cell apoptosis. Ectopic expression of miR-100 and miR-99a targeted FK506-binding protein 51 (FKBP51) and, in turn, influenced glucocorticoid receptor (GR) activity. Meanwhile, miR-100 and miR-99a overexpression inhibited the expression of IGF1R and mTOR and their downstream oncogene MCL1.
Conclusion:
MiR-100 and miR-99a have critical roles in altering cellular processes by targeting both the FKBP51 and IGF1R/mTOR signalling pathways in vitro and might represent a potential novel strategy for ALL treatment.
Similar content being viewed by others
Main
Childhood acute lymphoblastic leukaemia (ALL) is a commonly occurring malignancy characterised by the uncontrolled proliferation of immature lymphoid cells (Pui et al, 2004). Although treatment has improved remarkably over the past decade, ∼10% of ALL patients fail to reach long-term remission (Kraszewska et al, 2012). To better understand this disease, the intricate regulatory networks among molecular interactions and signalling pathways should be elucidated. In patients with ALL, several cell signalling pathways that control cancer occurrence and development have been shown to be altered (Weng et al, 2004; Hirsch and Chiarle, 2012); however, the specific mechanisms responsible for the development and treatment of this disease remain unknown. Hence, the discovery of more important molecules might further elucidate the networks and facilitate new therapeutic strategies. In the past decade, aberrant microRNA (miRNA) expression has been shown to have an essential role in the pathogenesis of leukaemia, and miRNAs have been considered as potential therapeutic targets for the disease (Fernando et al, 2012).
MicroRNAs are 20–22 nucleotides long and exert their regulatory effects by directly binding to the 3′ untranslated regions (UTRs) of their target genes, thus repressing the target gene at the level of translation (Esquela-Kerscher and Slack, 2006). Recent studies have demonstrated that miRNAs have important roles in cancer pathogenesis and development, and subsequently, in treatment and prognosis (Hwang and Mendell, 2006). In ALL, miR-125b has an important role in early hematopoietic development (Shaham et al, 2012); miR-124a contributes to the abnormal proliferation of ALL cells (Agirre et al, 2009), and knockdown of miR-17-92 clusters has been shown to increase glucocorticoid-mediated apoptosis in ALL cell lines (Molitoris et al, 2011).
MiR-100 and miR-99a belong to the same family and have similar roles in a variety of cancers (Doghman et al, 2010; Mueller et al, 2012; Chen et al, 2012b). Our previous study showed that both miR-100 and miR-99a are up-regulated in childhood acute myeloid leukaemia (AML) and that overexpression of miR-100 arrested the differentiation of human granulocyte and monocyte cells and promoted cell survival (Zhang et al, 2009; Zheng et al, 2012). In contrast, miR-100 and miR-99a have very low expression levels in ALL patients (Zhang et al, 2009), suggesting that these two miRNAs have different roles in myeloid cell and lymphocyte pathogenesis. However, the molecular basis of how miR-100 and miR-99a are involved in lymphoblastic leukaemogenesis and progression has not yet been elucidated.
Based on a bioinformatics analysis, FK506-binding protein 51 (FKBP51) was predicted to be a target of miR-100 and miR-99a (Bhushan and Kandpal, 2011). The evidence collected to date shows that FKBP51 is an immunophilin that is physiologically expressed in lymphocytes and is involved in sustaining cell growth, malignancy, and resistance to therapy (Li et al, 2011; Schmidt et al, 2012). Furthermore, IGF1R and mTOR are mutual targets of miR-100 and miR-99a in several cancer cells (Doghman et al, 2010; Lerman et al, 2011; Sun et al, 2011), and they have been implicated in the initiation and progression of several malignant neoplasms (Petroulakis et al, 2006), including ALL (Cardoso et al, 2009; Medyouf et al, 2011). Thus, we hypothesised that FKBP51, IGF1R, and mTOR are involved in the functioning of miR-100 and miR-99a in ALL and serve as their targets.
In this study, we found that miR-100 and miR-99a were down-regulated in childhood ALL patients and that their expression levels were related to the prognosis of the ALL patients. In vitro investigation further demonstrated that miR-100 and miR-99a participated in the regulation of cell proliferation and dexamethasone (Dex)-induced apoptosis in ALL cell lines. Our data revealed that FKBP51 is a novel target of miR-100 and miR-99a and, in turn, influences its downstream gene glucocorticoid receptor (GR). We also proved that miR-100 and miR-99a overexpression inhibited IGF1R and mTOR and down-regulated MCL1. The results of the present study suggest that miR-100 and miR-99a act as tumour suppressors and that their restoration might be a possible therapeutic strategy for patients with ALL.
Materials and methods
Patients
This study included 71 AML patients, 111 ALL patients, and 10 healthy donors from the First Affiliated Hospital of Sun Yat-sen University. Patient demographics are presented in supporting information Supplementary Table S1. Bone marrow was obtained from patients and healthy donors. Informed consent to perform the biological studies was obtained from all of the patients, and the study was approved by the Ethics Committee of the First Affiliated Hospital of Sun Yat-sen University.
Cell culture and cell treatment
The ALL cell lines, CCRF-CEM, CEM/C1, and Jurkat, and the HEK-293T cell line were purchased from American Type Culture Collection (ATCC, Manassas, VA, USA). All cell lines were grown with 10% fetal bovine serum (HyClone, Logan, UT, USA). Rapamycin (Beyotime, Haimen, China) was dissolved in dimethyl sulfoxide (Sigma, St Louis, MO, USA) and used at a concentration of 10-nM. Dexamethasone (Sigma) was dissolved in ethanol and used at concentrations of 1-μ M and 100-nM. The final concentrations of dimethyl sulfoxide and ethanol in the culture media were 0.05% and 0.1%, respectively.
RNA isolation and real-time quantitative RT−PCR
Total RNA was extracted using TRIzol reagent (Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s guidelines. Real-time PCR was performed to quantify mRNA expression using ExTaq SYBR Green Supermix (Bio-Rad, Hercules, CA, USA) according to the manufacturer’s instructions (details are provided in the supporting information, Supplementary Table S2).
Proliferation and apoptosis assays
Cell proliferation was assessed using the Cell Counting Kit-8 (CCK-8). After transfection, 1*104 cells per well were plated in 96-well sterile plastic culture plates, and the CCK-8 assay (Dojindo Molecular Technologies, Shanghai, China) was performed after 0, 24, 48, 72, and 96 h. To assess the rate of apoptosis, transfected cells were harvested and washed twice with cold PBS, and the Annexin V-PI Kit (Nanjing Keygen, Nanjing, China) was used according to the manufacturer’s guidelines. The detection was performed with a FACS Calibur using CellQuest software (BDIS, San Jose, CA, USA).
Transient transfection
For the luciferase reporter assay, HEK-293T cells were transfected with Lipofectamine 2000 (Invitrogen) following the manufacturer’s protocol. CCRF-CEM, CEM/C1, and Jurkat cells were transfected with the small molecular RNAs using the Neon Transfection System (Invitrogen) according to the manufacturer’s guidelines (details are provided in the Supporting Information Online, Supplementary Materials and Methods).
Dual luciferase activity assay
Luciferase constructs were established by inserting oligonucleotides containing the wild-type or mutant putative target site of the FKBP51 3′-UTR into the multi-cloning site of the psiCHECK2 vector (Promega, Fitchburg, WI, USA) (see Supporting Information Online, Supplementary Materials and Methods for more details).
Western blot assay
Western blot analyses were performed as described previously (Zheng et al, 2012). Nuclear–cytoplasmic fractionation was conducted using the NE-PER Nuclear and Cytoplasmic Extraction Reagents kit (Pierce, Rockford, IL, USA) according to the manufacturer’s protocol. Transfected cells were assayed with anti-FKBP51 (Epitomics, Zhejiang, China); anti-H3 (Abcam, Cambridge, UK); anti-MCL1 and anti-GR (Santa Cruz, Paso Robles, CA, USA); and anti-IGF1R, anti-mTOR, anti-phospho-mTOR (Ser-2448), anti-phospho-GR (Ser-211), and anti-GAPDH (Cell Signalling Technology, Boston, MA, USA). After a 1-h incubation with anti-rabbit (Sigma-Aldrich) HRP-conjugated secondary antibody, the protein level was detected using a luminal reagent (Millipore). X-ray films were acquired and quantified with the densitometric software Quantity One (Bio-Rad). The value under each sample indicates the fold change of protein amounts that normalised with the corresponding GAPDH or H3 in each sample.
Bioinformatic and statistical analyses
Online miRNA databases (TargetScan and PicTarget) were used to predict the miR-100 and miR-99a target genes. SPSS13.0 software (Chicago, IL, USA) was used for statistical analysis. Data are expressed as the mean±s.d. The differences between two groups were analysed using the Mann−Whitney U test for two groups or the Kruskal−Wallis test when more than two groups were compared. All tests were two-sided. The Kruskal−Wallis test was implemented for the comparison of three groups, and multiple comparisons were performed using one-way ANOVA and a least significant difference t test after the relative concentration was ranked. Differences were considered significant at *P<0.05, **P<0.01, and ***P<0.001.
Results
MiR-100 and miR-99a are associated with specific risk groups and survival in childhood ALL
To investigate the link between miR-100 and miR-99a and childhood ALL, we first measured the expression levels of miR-100 and miR-99a in both childhood ALL and AML patients at diagnosis using qRT−PCR. As shown in Figure 1A, both miRNAs showed significantly different expression patterns between ALL and AML compared with healthy donors. MiR-100 and miR-99 showed very low expression levels in most ALL patients compared with AML patients and healthy donors. We next analysed their correlation with the patient characteristics. Although the expression levels of miR-100 and miR-99a had no correlation with sex, age, or therapy (data not shown), we found that the expression levels of these two miRNAs were significantly correlated with patients who carried known high-risk prognostic factors, including white blood cell (WBC) count, ALL sub-classification (here, indicated as T-cell and B-cell ALL), the MLL-rearranged gene and the BCR-ABL fusion gene. As shown in Figure 1B, a higher WBC count (>5 × 104 mm−3) before chemotherapy was observed in patients with lower expression levels of miR-100 and miR-99a. Notably, all T-ALL cases showed low expression levels of miR-100 and miR-99a compared with B-ALL patients (Figure 1C). We also found that patients carrying the MLL-rearranged or BCR-ABL fusion gene, two crucial biological mutations associated with poor outcome, expressed lower levels of miR-100 and miR-99 compared with patients without these two fusion genes (Figure 1D). These results suggest that miR-100 and miR-99a are associated with specific risk groups within childhood ALL.
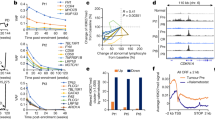
MiR-100 and miR-99a are associated with specific risk groups and the survival of patients with childhood ALL. (A) The expression levels of miR-100 (left) and miR-99a (right) were quantified by real-time PCR in 111 ALL patients, 71 AML patients and 10 healthy donors. MiR-100 and miR-99a were significantly down-regulated in ALL patients compared with AML patients (P<0.0001 and P<0.0001, respectively) and healthy donors (P=0.001 and P=0.0086, respectively). (B) miR-100 (left) and miR-99a (right) expression levels, determined by qRT−PCR, in ALL patients with more than 5 × 104 mm−3 white blood cells (WBCs) or less than 5 × 104 mm−3 WBCs at diagnosis (P<0.0001 and P<0.0001, respectively). (C) Comparison of the expression of miR-100 (left) and miR-99a (right) between B-ALL (n=93) and T-ALL (n=18) patients by qRT–PCR (P=0.0004 and P=0.0004, respectively). (D) The expression levels of miR-100 (left) and miR-99a (right) were significantly down-regulated in ALL patients with the MLL-rearranged gene (n=22) and the BCR-ABL fusion gene (n=11), in comparison with the patients without fusion genes (n=78) (P<0.001 and P<0.05, respectively, for miR-99a, and P<0.05 and P<0.05, respectively, for miR-99a). Wild type (WT): patients without these two fusion genes. (E) The OS of patients with high miR-100 and miR-99a expression levels was significantly higher than that of patients with low miR-100 and miR-99a expression levels (P=0.0466 and P=0.0126, respectively). (F) The leukaemia-free survival (LFS) of patients with high miR-100 and miR-99a expression levels was significantly higher than that of patients with low miR-100 and miR-99a expression levels (P=0.0054 and P=0.0233, respectively). The Kruskal−Wallis test was implemented for the comparison of three groups, and multiple comparisons were performed using one-way ANOVA and a least significant difference t test after the relative concentration was ranked. A Kaplan−Meier analysis and the log-rank test were used to analyse OS and LFS. *P<0.05, **P<0.01, and ***P<0.001 vs control or WT.
Furthermore, the association of miR-100 and miR-99a expression with the prognosis of ALL patients was investigated using Kaplan−Meier analysis and a log-rank test. As shown in Figure 1E, the 5-year overall survival (OS) of patients with high miR-100 and miR-99a expression levels was significantly higher than in patients with low miR-100 and miR-99a expression levels. Moreover, a trend towards increased leukaemia-free survival was observed in patients with ALL and up-regulated miR-100 and miR-99a expression levels over the 5-year follow-up period (Figure 1F). Taken together, these results suggest that higher expression levels of miR-100 and miR-99a were associated with better survival and prognosis.
MiR-100 and miR-99a inhibit cell proliferation and promote Dex-induced apoptosis in ALL cell lines and function as potential tumour suppressors
The observations described above suggest that both miR-100 and miR-99a are clinically relevant and might affect leukaemic cell progression. To explore the role of miR-100 and miR-99a, we investigated their influences on leukaemic cell proliferation and cell apoptosis. Three ALL cell lines, CCRF-CEM, CEM/C1, and Jurkat, were used to perform the in vitro functional analysis. A qRT−PCR assay was used to measure the transfection efficiency of the miRNAs (supporting information, Supplementary Figure S1). The results of a CCK-8 assay indicated that overexpression of miR-100 and miR-99a inhibited cell proliferation of all three ALL cell lines in a time-dependent manner (Figure 2A).
MiR-100 and miR-99a inhibit cell proliferation and promote Dex-induced apoptosis in ALL cell lines and function as potential tumour suppressors. (A) Transfection of miR-100 and miR-99a slowed ALL cell proliferation. The time points after transfection with control miRNA, miR-100, or miR-99a are indicated. MiR-100 and miR-99a significantly inhibited cell proliferation in CCRF-CEM (left), CEM/C1 (middle), and Jurkat (right) cells, as determined using the CCK-8 assay. (B–D) miR-100 and miR-99a significantly promoted Dex-induced cell apoptosis. CCRF-CEM (B), CEM/C1 (C), and Jurkat (D) cells were transfected with miR-100, miR-99a, or control miRNA and cultured for 24 h; the three cell lines were exposed to 1-μ M Dex for 8, 18, and 24 h, respectively. Cells were stained with PI/Annexin V and analysed by flow cytometry. A representative experiment is shown. **P<0.01 and ***P<0.001 vs control. Values are presented as the mean±s.d. of at least three independent experiments performed in triplicate.
We further studied the effect of miR-100 and miR-99a on Dex-induced ALL cell apoptosis. After transfection of miR-100 and miR-99a mimics for 24 h, cells were treated with 1-μ M Dex, a therapeutic drug that is widely used to treat ALL by triggering leukaemic cell apoptosis. Overexpression of miR-100 and miR-99a increased Dex-induced apoptosis compared with control miRNA in CCRF-CEM, CEM/C1, and Jurkat cells (Figure 2B–D). These data suggest that the ectopic expression of miR-100 and miR-99a inhibits cell proliferation and promotes the response to Dex-induced apoptosis in ALL cells.
FKBP51 is a novel target of miR-100 and miR-99a
To determine the molecular mechanism by which miR-100 and miR-99a are involved in ALL pathogenesis, we further investigated their downstream targets. Among the nearly 100 predicted targets, FKBP51 was chosen for further investigation because this gene has an active role in cancer aetiology and responds to antineoplastic therapy (Baughman et al, 1995; Febbo et al, 2005; Pei et al, 2009). As shown in Figure 3A, to test whether FKBP51 is directly regulated by miR-100 and miR-99a, a dual-luciferase assay was performed, and the 3′ UTR fragment, which was cloned into a reporter plasmid, was inserted into the luciferase open reading frame. The interaction between the miRNAs and the target mRNA sequences was further validated using a point mutation of the putative miRNA-binding site in the 3′ UTR of the FKBP51 gene. We found that the luciferase activity of the 3′ UTR of FKBP51 was reduced nearly 50% and 70% after transfection of both miR-100 and miR-99a; when the predicted target sites were mutated, the luciferase activity was unaffected (Figure 3B).
MiR-100 and miR-99a target FKBP51. (A) Schematic representation of the constructs used in the luciferase assay.The sequences shown below indicate the putative miR-100 and miR-99a target site on the wild-type 3′ UTR (construct FKBP51-wt), its mutated derivative (construct FKBP51-mut), and the pairing regions of miR-100 and miR-99a. (B) 293T cells were co-transfected with pSi-Check2 with either FKBP51-wt or FKBP51-mut and with miR-100, miR-99a, or empty vector (pCD6.2). Repression of luciferase activity due to the interaction between miR-100, miR-99a, and the luciferase constructs. Each Renilla luciferase reading was normalised to that obtained for the control firefly luciferase. (C, D) Jurkat cells were electroporated with 100-nmol mimics-NC (control miRNA), mimics-miR-100, or miR-99a and anti-scramble (control miRNA), anti-miR-100, or anti-miR-99a. The levels of miR-100 and miR-99a were assessed by qRT−PCR. Cell lysates were prepared for western blotting with the antibody against FKBP51, and the expression of GAPDH served as a loading control. Western blot figures are representative of at least three independent experiments. The value under each sample indicates the fold change of FKBP51 protein levels relative to that of the control. ***P<0.001. Values are presented as the mean±s.d. of at least three independent experiments performed in triplicate.
To further confirm that the FKBP51 protein is suppressed by miR-100 and miR-99a, we performed both miR-100/99a overexpression and knockdown experiments in Jurkat cells and examined FKBP51 expression. As shown in Figure 3C and D, the level of FKBP51 protein was significantly reduced in Jurkat cells that were transfected with the miR-100 and miR-99a mimics, whereas it was increased in cells that were transfected with the antisense of miR-100 and miR-99a. These data indicate that FKBP51 is a bona fide target of miR-100 and miR-99a in ALL cells.
MiR-100 and miR-99a affect cell proliferation and the response to Dex by targeting FKBP51 and, in turn, influencing the activity of steroid receptor GR
Although FKBP51 has important roles in neoplastic diseases (Rees-Unwin et al, 2007), the function of FKBP51 in leukaemia has not yet been elucidated. To explore the function of FKBP51, we used RNAi to investigate the role of this gene in cell proliferation and apoptosis. As shown in the upper-right corner of Figure 4A, FKBP51 expression was remarkably reduced after the silencing of FKBP51 in CEM/C1 cells. FKBP51 knockdown inhibited cell proliferation after 4 days of incubation using a CCK-8 assay (Figure 4A) and led to a significant increase in Dex-induced apoptosis in CEM/C1 cells by flow cytometry analysis (Figure 4B). Similar results were obtained in CCRF-CEM and Jurkat cell lines (Supplementary Figure S2). These results show that FKBP51 knockdown has a positive effect, similar to that of miR-100 and miR-99a (Figure 2), suggesting that miR-100 and miR-99a exert their functions of inhibiting cell proliferation and promoting Dex-induced cell apoptosis by reducing FKBP51 expression.
MiR-100 and miR-99a affected cell proliferation and the response to Dex by targeting FKBP51 and, in turn, influenced the activity of steroid receptor GR. (A) Transfecting CEM/C1 cells with si-FKBP51 significantly inhibited cell proliferation. Cell viability was determined using the CCK-8 assay. The time points after transfection with control siRNA or si-FKBP51 are indicated. The western blot analysis of the effect of si-FKBP51 is shown in the upper-right corner. The value under each sample indicates the fold change of FKBP51 protein levels relative to that of the control. (B) FKBP51 knockdown enhanced Dex-induced apoptosis. CEM/C1 cells were transfected with control siRNA or si-FKBP51 24 h after transfection, which was followed by 1-μ M Dex treatment for 18 h. Control siRNA served as a negative control. Then, the cells were collected for apoptosis analysis by PI/Annexin V staining and flow cytometry. A representative experiment is shown. (C) FKBP51 knockdown promoted the expression of GR and phosphorylated forms of GR in the nucleus. After 48 h of transfection with control siRNA or si-FKBP51, cells were exposed to 100-nM Dex for 24 h, and then cytoplasm and nucleus extracts were prepared. Equal amounts of protein from each fraction were analysed by immunoblotting with anti-FKBP51, anti-GR (total GR protein), and anti-phospho-Ser211 (p-GR), using GAPDH as an internal control for the cytoplasm fraction and H3 for the nucleus fraction. The value under each sample indicates the fold changes of FKBP51, GR, and p-GR protein levels relative to that of the control. (D) miR-100 and miR-99a overexpression induced the expression of GR and p-GR by down-regulating FKBP51 in the nucleus. After 48 h of transfection with control miRNA, miR-100, or miR-99a, cells were exposed to 100-nM Dex for 24 h, and then cytoplasm and nucleus extracts were prepared to detect the protein levels of FKBP51, GR, p-GR, and GAPDH in the cytoplasm fraction and of H3 in the nucleus fraction. Western blot figures are representative of at least three independent experiments. ***P<0.001 vs control. Values are presented as the mean±s.d. of at least three independent experiments.
Glucocorticoid receptor is an essential transcription factor that is involved in cellular proliferation, inflammatory responses, and cell differentiation (Rogatsky and Ivashkiv, 2006; Chen et al, 2012a), and FKBP51 is a potent inhibitor of GR activity on hormone induction and influences GR nuclear translocation (Ratajczak et al, 2003; Denny et al, 2005). Because the presence of FKBP51 reflected a decreased amount of GR accumulation in the nucleus (Wochnik et al, 2005; Binder, 2009) and phosphorylation at Ser-211 is the monophosphorylated version of the hormone-activated form of GR that accumulates in the nucleus (Wang et al, 2002; Chen et al, 2008), we tested whether knockdown of FKBP51 expression influenced the subcellular localisation of GR and Ser211-phosphorylated forms of GR in Jurkat cells. To address this issue, cytosolic and nuclear extracts were prepared from FKBP51-silenced and control cells following exposure to 100-nM Dex for 24 h. As shown in Figure 4C, after the silence of FKBP51, the phosphor-GR (Ser-211) expression was increased in the nucleus by western blotting using H3 protein as an internal control, accompanied by a slight increase of total GR expression level. However, the relative levels of total GR and phosphor-GR (Ser-211) expression were unaffected in the cytosolic fraction. Furthermore, we asked whether miR-100 and miR-99a affected this downstream target of FKBP51. In the nuclear fractions of miR-100/99a overexpressed cells, we observed increases in GR and phosphor-GR (Ser-211) expression, with down-regulation of FKBP51 levels, while the expression of total GR and phosphor-GR (Ser-211) was unchanged in the cytosolic fraction (Figure 4D). A similar result in which overexpression of miR-100/99a and silencing of FKBP51 increased the expression of GR and phosphor-GR (Ser-211) in the nucleus of Jurkat cells was obtained under the treatment of 1-μ M Dex (Supplementary Figure S3). These data showed that miR-100/99a contributed to the influence of GR nuclear translocation and enhancement of the phosphorylated forms of GR at Ser211 in the nucleus, which resemble the FKBP51-silencing effect. This effect is, at least in part, mediated by the inhibition of FKBP51.
MiR-100/99a target the IGF1R/mTOR pathways in ALL
Previous studies have reported that IGF1R and mTOR are direct targets of miR-100 and miR-99a in several human cancers (Doghman et al, 2010; Torres et al, 2012; Chen et al, 2012b). We thus asked whether IGF1R and mTOR are targets of miR-100 and miR-99a in ALL and whether these proteins act downstream from both miRNAs to alter cellular processes in ALL, similar to what occurs in FKBP51. As shown in Figure 5A, the protein levels of IGF1R and mTOR were reduced in Jurkat cells that were transfected with miR-100/99a mimics, while they were increased in cells that were transfected with the miR-100/99a inhibitors (antisense). These data confirmed that IGF1R and mTOR are targets of miR-100/99a. To further unravel whether IGF1R and mTOR are also involved in the miR-100- and miR-99a-mediated alterations in cell proliferation and Dex-induced apoptosis in ALL, we performed loss-of-function analyses with RNAi and found that the growth rates of the CEM/C1 cells were dramatically decreased and that the Dex-induced apoptosis rates were significantly enhanced after the silencing of IGF1R and mTOR (Figure 5B and C).
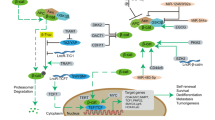
MiR-100/99a target the IGF1R/mTOR pathways in ALL. (A) IGF1R and mTOR are direct targets of miR-100 and miR-99a. Jurkat cells were electroporated with 100-nmol mimics-NC, miR-100-mimics, or miR-99a-mimics and 100 nmol Control miRNA, anti-miR-100, or anti-miR-99a. Cell lysates were prepared for western blotting with an antibody against IGF1R and mTOR, and the expression of GAPDH served as a loading control. The value under each sample indicates the fold changes of IGF1R and mTOR protein levels relative to that of the control. (B) CEM/C1 cell proliferation was significantly inhibited, and Dex-induced apoptosis (C) was significantly enhanced after the transfection of si-IGF1R and si-mTOR, as determined using the CCK-8 assay and flow cytometry. For flow cytometry, the apoptotic cells were stained by PI/Annexin V 18 h after exposure to 1 μ M Dex. Control siRNA served as a negative control. A representative experiment is shown. The western blot analysis of the transfection efficiency of si-IGF1R and si-mTOR in CEM/C1 cells is shown in the upper-right corner of (B). (D) Western blot analysis of the expression level of mTOR and MCL1 in Jurkat cells following treatment with vehicle, 1-μ M Dex, 10-nM Rap, or 1-μ M Dex plus 10-nM Rap for 24 h. The value under each sample indicates the fold changes of mTOR and MCL1 protein levels relative to that of the control. The expression levels of miR-100 and miR-99a were detected after the treatment described above. These two miRNAs were significantly up-regulated after the combined treatment of Dex and Rap. (E) Both overexpression of miR-100/99a and knockdown of mTOR reduced the expression of MCL1. At 48 h after the transfection, Jurkat cells were treated with 1 μ M Dex for 24 h, as determined by Western blot analysis. The value under each sample indicates the fold changes of mTOR and MCL1 protein levels relative to that of the control. (F) IGF1R knockdown promoted the phosphorylation of mTOR and, in turn, repressed the expression of MCL1. At 48 h after transfection, Jurkat cells were exposed to 1-μ M Dex for 24 h, and the expression of IGF1R, p-mTOR (Ser-2448), and MCL1 was detected by western blot analysis. The value under each sample indicates the fold changes of IGF1R, p-mTOR, mTOR, and MCL1 protein levels relative to that of the control. (G) CEM/C1 cell proliferation was significantly inhibited, and (H) Dex-induced apoptosis was significantly enhanced after the transfection of si-MCL1. Control si-RNA served as a negative control. A representative experiment is shown. (I) Schematic shows the function of miR-100 and miR-99a in cell proliferation and cell apoptosis in ALL. (i) Upon post-transcriptional suppression, FKBP51 was inhibited by miR-100 and miR-99a, thus restraining cell proliferation and activating the GR at the phosphorylation site of Ser-211, which in turn led to apoptosis. (ii) Through inhibition of mTOR, miR-100 and miR-99a suppressed the expression of MCL1, which resulted in the blockade of cell proliferation and led to cell apoptosis. By targeting IGF1R, miR-100 and miR-99a triggered cell apoptosis and inhibited cell proliferation. In the meantime, down-regulated expression of IGF1R inhibited the activity of mTOR (phosphorylation at the site of Ser-2448), which also led to the suppression of the mTOR/MCL1 signalling pathway. Western blot figures are representative of at least three independent experiments. ***P<0.001 vs Control. Values are presented as the mean±s.d. of at least three independent experiments.
MCL1 is highly suppressed during the increased Dex-induced apoptosis observed in ALL cells that have been treated with rapamycin, which is a newly FDA-approved immunosuppressant drug that inhibits mTOR (Wei et al, 2006). The results of this study indicate that mTOR is directly involved in the miR-100- and miR-99a-mediated apoptotic response to Dex. Thus, we hypothesised that MCL1 might also be involved in miR-100- and miR-99a-triggered apoptosis. To prove this hypothesis, we first examined the expression of mTOR and MCL1 protein levels following induction with rapamycin and Dex and found significant decreases in both protein levels after exposure to both drugs. In addition, we found that the expression levels of miR-100 and miR-99a were significantly up-regulated after treatment with both rapamycin and Dex (Figure 5D). Therefore, miR-100 and miR-99a might regulate the expression of MCL1 by suppressing mTOR. We determined that the protein expression of MCL1 was down-regulated in Jurkat cells with miR-100 and miR-99a overexpression and with mTOR knockdown, following the exposure of 1-μ M Dex for 24 h (Figure 5E). Furthermore, the expression of MCL1 was also down-regulated after the knockdown of IGF1R through the inhibition of activated mTOR (with phosphorylation at the site of ser-2448) followed by the exposure to Dex (Figure 5F) because mTOR is a downstream gene of IGF1R (Eroles et al, 2012). To elucidate the function of MCL1 in the miR-100- and miR-99a-mediated signalling pathway, we investigated the roles of MCL1 in cell apoptosis and cell growth. As shown in Figure 5G and H, after silencing MCL1, its influences on cell proliferation and cell apoptosis were similar to the findings obtained in the miR-100 and miR-99a studies and further confirmed our hypothesis that miR-100 and miR-99a are important regulators of MCL1 in ALL.
Discussion
Human miR-100 and miR-99a, which are encoded on different chromosomes but share the same seed region, exhibit a similar expression pattern (Hertel et al, 2012). Both miRNAs are down-regulated in several human cancers and act as tumour suppressors via their influence on cell processes (Sun et al, 2011; Torres et al, 2012; Chen et al, 2012b). However, they are up-regulated in paediatric AML patients and are correlated with poor prognosis (Bai et al, 2012; Zheng et al, 2012). In this study, we showed that both miR-100 and miR-99a were significantly down-regulated in ALL patients and that ectopic expression of miR-100 and miR-99a inhibited cell proliferation and enhanced Dex-induced cell apoptosis. These findings suggest that these two miRNAs may have different roles in the adaptation of cells to the transformed state of myeloid and lymphoblastic cells.
This study provides evidence that miR-100 and miR-99a function in ALL. First, we revealed a differential expression pattern of miR-100 and miR-99a in different ALL subtypes. Lower expression levels of both miR-100 and miR-99a were found in T-ALL patients and in patients carrying the MLL-rearrangement and BCR-ABL fusion genes, and these lower expression levels correlated with poor prognosis. These results indicate that the expressions of miR-100 and miR-99a are cell-type specific and suggest that both miRNAs are associated with leukemogenesis and the prognostic outlook of ALL.
Second, when addressing the molecular basis for the phenotype of miR-100 and miR-99a, FKBP51 was identified as a novel target of both miRNAs. FKBP51 has effective roles in cell proliferation, neoplastic diseases, and cell apoptosis in several tumour cell lines (Jiang et al, 2008; Li et al, 2011; Schmidt et al, 2012). However, the involvement of FKBP51 in lymphoblastic leukaemia cells has not yet been elucidated. The observation that FKBP51 knockdown caused the same effect as miR-100 and miR-99a overexpression indicates that FKBP51 contributes to the miR-100 and miR-99a phenotypes.
FKBP51 has the overall effect of impairing GR nuclear translocation and reducing GR activity, and by down-regulating the GR signalling pathway, it exerts proliferative and anti-apoptotic properties (Denny et al, 2000; Romano et al, 2011). GR, which can continuously shuttle between the nuclear and cytoplasmic compartments, is an important ligand-dependent transcription factor that belongs to the nuclear receptor family and is also a monomeric protein that cooperates with other transcription factors to induce transcription (Bray and Cotton, 2003; Vandevyver et al, 2012). Davies and colleagues revealed that the Dex-binding event causes a dissociation of FKBP51 and GR-complex that, in turn, control the intracellular trafficking of GR (Davies et al, 2002). In a loss-of-function study, our results demonstrated that the relatively silenced expression of FKBP51 is responsible for the accumulation of GR expression in the nucleus after Dex induction, and our results further revealed that miR-100/99a overexpression influenced the translocation of GR to the nucleus. After translocating to the nucleus, phosphorylation at Ser-211 is essential for subsequent GR-dependent signalling (Chen et al, 2008). We found that silenced FKBP51 increased the phosphor-GR (Ser-211) expression in the nucleus of Jurkat cells. Furthermore, miR-100 and miR-99a overexpression decreased the FKBP51 protein levels and led to GR activation in the nucleus after exposure to Dex. These findings suggest that, in the miR-100- and miR-99a-mediated response to Dex in ALL cells, the GR signalling pathway is activated by the suppression of FKBP51. Recent studies have shown that multimeric chaperones, including hsp90, p23, FKBP52, dynamitin, and dynein, are required for the translocation of GR (Echeverria et al, 2009), yet further research will be needed to determine whether other importins or nucleoporins are required and to elucidate the complete details of how miR-100 and miR-99a affect GR activity through FKBP51.
Another contribution of the study is the validation of two other important target genes, IGF1R and mTOR, which are involved in the miR-100- and miR-99-regulated pathways. Activation of the IGF1R and mTOR pathways, here referred to as the IGFIR/mTOR pathway, triggers a complex signalling cascade that stimulates cell proliferation, differentiation, and survival (Johnston et al, 2010; Laplante and Sabatini, 2012; Tognon and Sorensen, 2012). The results of several clinical investigations have indicated that IGF1R and mTOR are promising therapeutic targets for breast cancer, renal cell carcinoma, and hepatocellular carcinoma (Busaidy et al, 2012; Laplante and Sabatini, 2012; Tognon and Sorensen, 2012). In the present study, we further demonstrated that both genes are also the targets of miR-100 and miR-99a and contribute to the ALL cell process. Knockdown of IGF1R and mTOR mimicked the effects of miR-100 and miR-99a on the phenotypes of ALL cells. The IGF1R and mTOR signalling pathways are activated in ALL and are associated with ALL pathogenesis and progression (Cardoso et al, 2009; Medyouf et al, 2011). Thus, the identification of IGF1R and mTOR as the targets of miR-100 and miR-99a further emphasises the roles of these two miRNAs in ALL and provides evidence for developing potential miRNA-based therapy for ALL.
In addition, Wei et al, (2006) reported that reducing the expression of MCL1 in ALL is key for the rapamycin-mediated enhancement of Dex-induced apoptosis. In a murine lymphoma model, Mills et al, reported that MCL1 down-regulation is dependent on the inhibition of the mTOR complex 1 (mTORC1), which has the classic features of mTOR (Mills et al, 2008). Because rapamycin is a specific inhibitor of mTOR and, to some extent, miR-100 and miR-99a function similarly to rapamycin by suppressing mTOR, we speculated that MCL1 might also be involved in the miR-100- and miR-99a-mediated enhancement of Dex-induced apoptosis. Two observations confirmed our hypothesis. First, the MCL1 protein level was significantly decreased after the cells were transfected with these two miRNAs and treated with Dex. Second, MCL1 knockdown mimicked the effect of overexpressing miR-100 and miR-99a on the cellular processes. These findings highlight the critical roles of miR-100 and miR-99a in controlling cell growth and Dex-induced cell apoptosis in ALL cells through MCL1 by targeting IGF1R and mTOR.
Finally, as summarised in Figure 5I, both miR-100 and miR-99a are candidate tumour suppressor miRNAs in ALL that influence cell proliferation and the response to Dex-induced apoptosis. Specifically, our experimental data indicate that miR-100 and miR-99a are involved in two essential signalling pathways: (i) influencing GR signalling by targeting FKBP51 and (ii) suppressing the IGF1R/mTOR pathway and down-regulating the expression of the anti-apoptotic gene MCL1 to inhibit cell growth and initiate cell apoptosis. The modulation of multiple cancer-associated pathways underscores the significance of miR-100 and miR-99a for future clinical treatments. Therefore, our study suggests a novel gene therapy strategy, namely, the enhancement of Dex-induced apoptosis, for patients with ALL.
Change history
15 October 2013
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Agirre X, Vilas-Zornoza A, Jimenez-Velasco A, Martin-Subero JI, Cordeu L, Garate L, San Jose-Eneriz E, Abizanda G, Rodriguez-Otero P, Fortes P, Rifon J, Bandres E, Calasanz MJ, Martin V, Heiniger A, Torres A, Siebert R, Roman-Gomez J, Prosper F (2009) Epigenetic silencing of the tumor suppressor microRNA Hsa-miR-124a regulates CDK6 expression and confers a poor prognosis in acute lymphoblastic leukemia. Cancer Res 69 (10): 4443–4453.
Bai J, Guo A, Hong Z, Kuai W (2012) Upregulation of microRNA-100 predicts poor prognosis in patients with pediatric acute myeloid leukemia. OncoTargets Ther 5: 213–219.
Baughman G, Wiederrecht GJ, Campbell NF, Martin MM, Bourgeois S (1995) FKBP51, a novel T-cell-specific immunophilin capable of calcineurin inhibition. Mol Cell Biol 15 (8): 4395–4402.
Bhushan L, Kandpal RP (2011) EphB6 receptor modulates micro RNA profile of breast carcinoma cells. PloS One 6 (7): e22484.
Binder EB (2009) The role of FKBP5, a co-chaperone of the glucocorticoid receptor in the pathogenesis and therapy of affective and anxiety disorders. Psychoneuroendocrinology 34 (Suppl 1): S186–S195.
Bray PJ, Cotton RG (2003) Variations of the human glucocorticoid receptor gene (NR3C1): pathological and in vitro mutations and polymorphisms. Human Mutat 21 (6): 557–568.
Busaidy NL, Farooki A, Dowlati A, Perentesis JP, Dancey JE, Doyle LA, Brell JM, Siu LL (2012) Management of metabolic effects associated with anticancer agents targeting the PI3K-Akt-mTOR pathway. J Clin Oncol 30 (23): 2919–2928.
Cardoso BA, Martins LR, Santos CI, Nadler LM, Boussiotis VA, Cardoso AA, Barata JT (2009) Interleukin-4 stimulates proliferation and growth of T-cell acute lymphoblastic leukemia cells by activating mTOR signaling. Leukemia 23 (1): 206–208.
Chen DW, Saha V, Liu JZ, Schwartz JM, Krstic-Demonacos M (2012a) Erg and AP-1 as determinants of glucocorticoid response in acute lymphoblastic leukemia. Oncogene 32 (25): 3039–3048.
Chen W, Dang T, Blind RD, Wang Z, Cavasotto CN, Hittelman AB, Rogatsky I, Logan SK, Garabedian MJ (2008) Glucocorticoid receptor phosphorylation differentially affects target gene expression. Mol Endocrinol 22 (8): 1754–1766.
Chen Z, Jin Y, Yu D, Wang A, Mahjabeen I, Wang C, Liu X, Zhou X (2012b) Down-regulation of the microRNA-99 family members in head and neck squamous cell carcinoma. Oral Oncol 48 (8): 686–691.
Davies TH, Ning YM, Sanchez ER (2002) A new first step in activation of steroid receptors: hormone-induced switching of FKBP51 and FKBP52 immunophilins. J Biol Chem 277 (7): 4597–4600.
Denny WB, Prapapanich V, Smith DF, Scammell JG (2005) Structure-function analysis of squirrel monkey FK506-binding protein 51, a potent inhibitor of glucocorticoid receptor activity. Endocrinology 146 (7): 3194–3201.
Denny WB, Valentine DL, Reynolds PD, Smith DF, Scammell JG (2000) Squirrel monkey immunophilin FKBP51 is a potent inhibitor of glucocorticoid receptor binding. Endocrinology 141 (11): 4107–4113.
Doghman M, El Wakil A, Cardinaud B, Thomas E, Wang J, Zhao W, Peralta-Del Valle MH, Figueiredo BC, Zambetti GP, Lalli E (2010) Regulation of insulin-like growth factor-mammalian target of rapamycin signaling by microRNA in childhood adrenocortical tumors. Cancer Res 70 (11): 4666–4675.
Echeverria PC, Mazaira G, Erlejman A, Gomez-Sanchez C, Piwien Pilipuk G, Galigniana MD (2009) Nuclear import of the glucocorticoid receptor-hsp90 complex through the nuclear pore complex is mediated by its interaction with Nup62 and importin beta. Mol Cell Biol 29 (17): 4788–4797.
Eroles P, Bosch A, Perez-Fidalgo JA, Lluch A (2012) Molecular biology in breast cancer: intrinsic subtypes and signaling pathways. Cancer Treat Rev 38 (6): 698–707.
Esquela-Kerscher A, Slack FJ (2006) Oncomirs—microRNAs with a role in cancer. Nature Rev Cancer 6 (4): 259–269.
Febbo PG, Lowenberg M, Thorner AR, Brown M, Loda M, Golub TR (2005) Androgen mediated regulation and functional implications of fkbp51 expression in prostate cancer. J Urol 173 (5): 1772–1777.
Fernando TR, Rodriguez-Malave NI, Rao DS (2012) MicroRNAs in B cell development and malignancy. J Hematol Oncol 5: 7.
Hertel J, Bartschat S, Wintsche A, Otto C, Stadler PF (2012) Evolution of the let-7 microRNA family. RNA Biol 9 (3): 231–241.
Hirsch E, Chiarle R (2012) Calming down T cell acute leukemia. Cancer Cell 21 (4): 449–450.
Hwang HW, Mendell JT (2006) MicroRNAs in cell proliferation, cell death, and tumorigenesis. Br J Cancer 94 (6): 776–780.
Jiang W, Cazacu S, Xiang C, Zenklusen JC, Fine HA, Berens M, Armstrong B, Brodie C, Mikkelsen T (2008) FK506 binding protein mediates glioma cell growth and sensitivity to rapamycin treatment by regulating NF-kappaB signaling pathway. Neoplasia 10 (3): 235–243.
Johnston PB, Yuan R, Cavalli F, Witzig TE (2010) Targeted therapy in lymphoma. J Hematol Oncol 3: 45.
Kraszewska MD, Dawidowska M, Szczepanski T, Witt M (2012) T-cell acute lymphoblastic leukaemia: recent molecular biology findings. Br J Haematol 156 (3): 303–315.
Laplante M, Sabatini DM (2012) mTOR signaling in growth control and disease. Cell 149 (2): 274–293.
Lerman G, Avivi C, Mardoukh C, Barzilai A, Tessone A, Gradus B, Pavlotsky F, Barshack I, Polak-Charcon S, Orenstein A, Hornstein E, Sidi Y, Avni D (2011) MiRNA expression in psoriatic skin: reciprocal regulation of hsa-miR-99a and IGF-1R. PloS One 6 (6): e20916.
Li L, Lou Z, Wang L (2011) The role of FKBP5 in cancer aetiology and chemoresistance. Br J Cancer 104 (1): 19–23.
Medyouf H, Gusscott S, Wang H, Tseng JC, Wai C, Nemirovsky O, Trumpp A, Pflumio F, Carboni J, Gottardis M, Pollak M, Kung AL, Aster JC, Holzenberger M, Weng AP (2011) High-level IGF1R expression is required for leukemia-initiating cell activity in T-ALL and is supported by Notch signaling. J Exp Med 208 (9): 1809–1822.
Mills JR, Hippo Y, Robert F, Chen SM, Malina A, Lin CJ, Trojahn U, Wendel HG, Charest A, Bronson RT, Kogan SC, Nadon R, Housman DE, Lowe SW, Pelletier J (2008) mTORC1 promotes survival through translational control of Mcl-1. Proc Natl Acad Sci USA 105 (31): 10853–10858.
Molitoris JK, McColl KS, Distelhorst CW (2011) Glucocorticoid-mediated repression of the oncogenic microRNA cluster miR-17∼92 contributes to the induction of Bim and initiation of apoptosis. Mol Endocrinol 25 (3): 409–420.
Mueller AC, Sun D, Dutta A (2012) The miR-99 family regulates the DNA damage response through its target SNF2H. Oncogene 32 (9): 1164–1172.
Pei H, Li L, Fridley BL, Jenkins GD, Kalari KR, Lingle W, Petersen G, Lou Z, Wang L (2009) FKBP51 affects cancer cell response to chemotherapy by negatively regulating Akt. Cancer Cell 16 (3): 259–266.
Petroulakis E, Mamane Y, Le Bacquer O, Shahbazian D, Sonenberg N (2006) mTOR signaling: implications for cancer and anticancer therapy. Br J Cancer 94 (2): 195–199.
Pui CH, Relling MV, Downing JR (2004) Acute lymphoblastic leukemia. N Engl J Med 350 (15): 1535–1548.
Ratajczak T, Ward BK, Minchin RF (2003) Immunophilin chaperones in steroid receptor signalling. Curr Top Med Chem 3 (12): 1348–1357.
Rees-Unwin KS, Craven RA, Davenport E, Hanrahan S, Totty NF, Dring AM, Banks RE, J Morgan G, Davies FE (2007) Proteomic evaluation of pathways associated with dexamethasone-mediated apoptosis and resistance in multiple myeloma. Br J Haematol 139 (4): 559–567.
Rogatsky I, Ivashkiv LB (2006) Glucocorticoid modulation of cytokine signaling. Tissue Antigens 68 (1): 1–12.
Romano S, Sorrentino A, Di Pace AL, Nappo G, Mercogliano C, Romano MF (2011) The emerging role of large immunophilin FK506 binding protein 51 in cancer. Curr Med Chem 18 (35): 5424–5429.
Schmidt MV, Paez-Pereda M, Holsboer F, Hausch F (2012) The prospect of FKBP51 as a drug target. Chem Med Chem 7 (8): 1351–1359.
Shaham L, Binder V, Gefen N, Borkhardt A, Izraeli S (2012) MiR-125 in normal and malignant hematopoiesis. Leukemia 26 (9): 2011–2018.
Sun D, Lee YS, Malhotra A, Kim HK, Matecic M, Evans C, Jensen RV, Moskaluk CA, Dutta A (2011) miR-99 family of MicroRNAs suppresses the expression of prostate-specific antigen and prostate cancer cell proliferation. Cancer Res 71 (4): 1313–1324.
Tognon CE, Sorensen PH (2012) Targeting the insulin-like growth factor 1 receptor (IGF1R) signaling pathway for cancer therapy. Expert Opin Ther Targets 16 (1): 33–48.
Torres A, Torres K, Pesci A, Ceccaroni M, Paszkowski T, Cassandrini P, Zamboni G, Maciejewski R (2012) Deregulation of miR-100, miR-99a and miR-199b in tissues and plasma coexists with increased expression of mTOR kinase in endometrioid endometrial carcinoma. BMC Cancer 12: 369.
Vandevyver S, Dejager L, Libert C (2012) On the trail of the glucocorticoid receptor: into the nucleus and back. Traffic 13 (3): 364–374.
Wang Z, Frederick J, Garabedian MJ (2002) Deciphering the phosphorylation "code" of the glucocorticoid receptor in vivo. J Biol Chem 277 (29): 26573–26580.
Wei G, Twomey D, Lamb J, Schlis K, Agarwal J, Stam RW, Opferman JT, Sallan SE, den Boer ML, Pieters R, Golub TR, Armstrong SA (2006) Gene expression-based chemical genomics identifies rapamycin as a modulator of MCL1 and glucocorticoid resistance. Cancer Cell 10 (4): 331–342.
Weng AP, Ferrando AA, Lee W, Morris JPt, Silverman LB, Sanchez-Irizarry C, Blacklow SC, Look AT, Aster JC (2004) Activating mutations of NOTCH1 in human T cell acute lymphoblastic leukemia. Science 306 (5694): 269–271.
Wochnik GM, Ruegg J, Abel GA, Schmidt U, Holsboer F, Rein T (2005) FK506-binding proteins 51 and 52 differentially regulate dynein interaction and nuclear translocation of the glucocorticoid receptor in mammalian cells. J Biol Chem 280 (6): 4609–4616.
Zhang H, Luo XQ, Zhang P, Huang LB, Zheng YS, Wu J, Zhou H, Qu LH, Xu L, Chen YQ (2009) MicroRNA patterns associated with clinical prognostic parameters and CNS relapse prediction in pediatric acute leukemia. PloS One 4 (11): e7826.
Zheng YS, Zhang H, Zhang XJ, Feng DD, Luo XQ, Zeng CW, Lin KY, Zhou H, Qu LH, Zhang P, Chen YQ (2012) MiR-100 regulates cell differentiation and survival by targeting RBSP3, a phosphatase-like tumor suppressor in acute myeloid leukemia. Oncogene 31 (1): 80–92.
Acknowledgements
This work was supported by grants from the National Science and Technology Department of China and National Science Foundation of China.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Supplementary Information accompanies this paper on British Journal of Cancer website
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Li, XJ., Luo, XQ., Han, BW. et al. MicroRNA-100/99a, deregulated in acute lymphoblastic leukaemia, suppress proliferation and promote apoptosis by regulating the FKBP51 and IGF1R/mTOR signalling pathways. Br J Cancer 109, 2189–2198 (2013). https://doi.org/10.1038/bjc.2013.562
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2013.562
Keywords
This article is cited by
-
MicroRNA based combinatorial therapy against TKIs resistant CML by inactivating the PI3K/Akt/mTOR pathway: a review
Medical Oncology (2023)
-
miR-100 inhibits cell proliferation in mantle cell lymphoma by targeting mTOR
Experimental Hematology & Oncology (2020)
-
miR-125b-5p and miR-99a-5p downregulate human γδ T-cell activation and cytotoxicity
Cellular & Molecular Immunology (2019)
-
MicroRNA as a prognostic biomarker for survival in childhood acute lymphoblastic leukemia: a systematic review
Cancer and Metastasis Reviews (2019)
-
Circulating microRNA-99 family as liquid biopsy marker in pancreatic adenocarcinoma
Journal of Cancer Research and Clinical Oncology (2018)