Abstract
Aim:
ATP-sensitive potassium (KATP) channels formed by a combination of SUR/Kir6.x subunits play a crucial role in protection against hypoxic or ischemic injuries resulting from cell metabolic disorders. In this study we investigated the effects of Na-azide, a metabolic inhibitor, on KATP channels expressed in Xenopus oocytes, and explored the structure basis for their sensitivity to cell metabolic disorders.
Methods:
Six subtypes of KATP channels (wild SUR1/Kir6.2, SUR2B/Kir6.2, SUR1/Kir6.1, SUR2B/Kir6.1, SUR2A/Kir6.2 and SUR2A/Kir6.1), as well as eleven subtypes of KATP channels with mutant subunits were expressed in Xenopus oocytes. KATP currents were recorded using a two-electrode voltage clamp recording technique. The drugs were applied through bath.
Results:
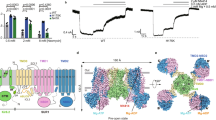
Except SUR2A/Kir6.1, five subtypes of KATP channels were activated by Na-azide (3 mmol/L) with an order of the responses: SUR1/Kir6.2>SUR2B/Kir6.2>SUR1/Kir6.1>SUR2B/Kir6.1>SUR2A/Kir6.2, and the opening rate (t1/2) was SUR1/Kir6.x>SUR2B/Kir6.x>SUR2A/Kir6.2. Furthermore, Kir6.2, rather than Kir6.1, had intrinsic sensitivity to Na-azide, and the residues involved in ATP-binding (R50 and K185) or pH-sensing (H175) were associated with the sensitivity of the Kir6.2 subunit to Na-azide. Moreover, the residues (K707 and K1348) within the Walker A (WA) motifs of two nucleotide-binding domains (NBDs) were essential for SUR2B/Kir6.x (especially SUR2B/Kir6.1) channel activation by Na-azide, suggesting a key role for Mg-adenine nucleotide binding and/or hydrolysis in the SUR2B subunit.
Conclusion:
Among the six subtypes of KATP channels, SUR1/Kir6.2 is the most sensitive, whereas SUR2A/Kir6.1 is insensitive, to cell metabolic disorders. The Kir6.2 subunit, rather than the Kir6.1 subunit, has intrinsic sensitivity to cell metabolic disorders. The residues (K707 and K1348) within the WA motifs of SUR2B are important for the sensitivity of SUR2B/Kir6.x channels to cell metabolic disorders.
Similar content being viewed by others
Introduction
ATP-sensitive potassium (KATP) channels are widely distributed in many tissues and play a variety of physiological and pathological roles by coupling the metabolic state to cellular electrical activity1,2,3. In the heart, brain and blood vessels, KATP channels remain closed under normal physiological conditions, however, they can be activated when cell metabolism is disturbed by hypoxia or ischemia, resulting in an efflux of potassium ions and membrane hyperpolarization. The decreased membrane excitability leads to shortened cardiac action potential, inhibition of neurotransmitter release and relaxation of vascular smooth muscles, which play a key role in limiting cellular damage or regulating blood pressure4,5,6. In addition, metabolic disorders are observed in hypertension, and KATP channels in vascular endothelial cells can be activated by low metabolic status from elevated shear stress7,8,9. Therefore, KATP channels are potentially important for treatments of cardiovascular diseases with metabolic disorders, such as myocardial ischemia and hypertension.
As a hetero-octameric complex, KATP channels are formed by the combination of the SUR and Kir6.x subunits1,2,10,11,12. SUR1/Kir6.2, SUR2A/Kir6.2 and SUR2B/Kir6.2 channels have been reported to reconstitute pancreatic β-cell/neuron, cardiac/skeletal muscle, and non-vascular smooth muscle KATP channels, respectively. The SUR/Kir6.2 combinations are considered classical KATP channels with ∼50–80 pS single channel conductance that can be inhibited by micromolar concentration of ATP. In contrast, the Kir6.1-containing channels with smaller conductance (∼30 pS) can be stimulated by nucleoside diphosphates (NDPs) in the presence of Mg2+13,14. The tissue-specific distribution of the Kir6.1 subunit is still being debated. A variety of studies have indicated that SUR2B/Kir6.1 is a subtype of the KATP channel in vascular smooth muscles and endothelial cells14,15,16. The molecular composition of the microglia KATP channel may be Kir6.1 and SUR217 and the astrocytes express the KATP channel composed of SUR1/Kir6.118. Moreover, emerging evidence demonstrates that the specific combination of SUR1/Kir6.1 forms channels with strong resemblances to mitochondria KATP (mitoKATP) channels19,20.
The metabolic inhibitor Na-azide, which lowers intracellular ATP concentrations significantly, has been widely used for inducing energy depletion21. As previously reported, when expressed in Xenopus oocytes, SUR1/Kir6.2 and SUR2B/Kir6.2 channels were robustly activated by Na-azide, whereas SUR2A/Kir6.2 was not21,22,23. Few similar studies, however, have been conducted on the Kir6.1-containing channels. Therefore, the inherent metabolic sensitivity of the SUR/Kir6.x channels have not been fully investigated and systematically compared. In addition, there are still other puzzles, such as, “what are the differences in the metabolic regulation mechanism of Kir6.1-containing KATP channels and their Kir6.2-containing counterparts?” or, “besides adenine nucleotides, are there additional cytosolic factors contributing to the metabolic regulation of KATP channel activity?”. Given these issues, we examined the effects of Na-azide on whole-cell currents recorded from oocytes expressing all six subtypes of SUR/Kir6.x combination channels and further explored the possible molecular structure basis intrinsic to Kir6.x or specifically correlated with SUR2B.
Materials and methods
Molecular biology
Rat Kir6.1 (D42145), mouse Kir6.2 (D50581), hamster SUR1 (L40623), rat SUR2A (D83598) and rat SUR2B (AF087838) cDNAs were subcloned into the pGEMHE vector24. The C-terminal truncations of Kir6.x (Kir6.1ΔC45, Kir6.2ΔC36) were made via conventional polymerase chain reactions. Point mutations were generated by site-directed mutagenesis using the Fast Mutagenesis System (TransGen Biotech, Beijing, China) according to the manufacturer's instructions. All constructs were confirmed by DNA sequencing. Capped cRNAs were transcribed in vitro with T7 RNA polymerase using the Ribomax large scale RNA production kit (Promega, Madison, WI, USA).
Oocyte preparation and injection
Oocytes were obtained from adult female Xenopus laevis (Nasco, USA) and the follicle membrane of the oocyte was removed by treatment with 1.5 mg/mL collagenase (type IA, Sigma-Aldrich, St Louis, MO, USA) for 60–90 min at room temperature with agitation in a Ca2+-free OR2 solution (82.5 mmol/L NaCl, 2 mmol/L KCl, 1 mmol/L MgCl2, and 5 mmol/L HEPES, pH 7.4). Then, after several washes with the OR2 solution, the Stage V or VI oocytes were collected and incubated at 18 °C in ND96 solution (containing, in mmol/L, 96 NaCl, 2 KCl, 1 MgCl2, 1.8 CaCl2, 5 HEPES, pH 7.4) supplemented with 100 U/mL penicillin, 100 μg/mL streptomycin and 2.5 mmol/L sodium pyruvate. These oocytes were co-injected the following day with ∼1 ng of Kir6.x cRNA and ∼5 ng of cRNA encoding wildtype or mutant SUR. In some experiments, oocytes were injected with ∼2 ng of cRNA encoding Kir6.1, Kir6.2, Kir6.1ΔC45 or Kir6.2ΔC36 (or the corresponding mutant). The final injection volume was 46 nL/oocyte. The control oocytes were injected with an equal volume of nuclease-free water. Whole-cell currents were studied in the oocytes 2–5 days after injection.
The functional expressions of these SUR/Kir6.x channels in Xenopus oocytes were confirmed by their properties as previously reported for cloned KATP channels11,21,25. For example, the SUR/Kir6.x channels were selectively activated by pinacidil or diazoxide, two classical KATP channel openers; they were all inhibited by glibenclamide, a specific KATP channel blocker. Nevertheless, the control oocytes (water-injected) had no response to these drugs.
Electrophysiology
Channel currents were recorded in whole-cell configurations by the standard two-electrode voltage clamp (TEVC) technique using an AxoClamp2B amplifier (Axon Instruments, Union City, CA, USA). Current signals were low-pass filtered at 1 kHz and digitized at 10 kHz using an Axon Digidata 1440A interface (Molecular Devices, Sunnyvale, CA, USA). The electrodes were pulled from borosilicate glass capillaries using a puller Narishige PP-830 (Narishige Scientific Instrument, Tokyo, Japan) and had resistances of 0.5–1.5 MΩ when filled with 3 mol/L KCl. Oocytes were bathed in a high-potassium solution (ND96K) containing (mmol/L): 96 KCl, 2 NaCl, 1 MgCl2, 1.8 CaCl2, 5 HEPES (pH 7.4 with KOH) and whole-cell KATP currents were evoked by a series of 300 ms depolarizing voltage steps from −120 to +50 mV with 10 mV increments per step. The holding potential was −10 mV, which was close to the resting membrane potential in the ND96K solution. Voltage commands were applied repeatedly at 1 min intervals until the resulting currents reached a steady state. Currents at −80 mV were used to plot the time courses and for comparing current magnitudes. Chemicals and drugs were applied into the bath solution in a cumulative fashion. All experiments were carried out at room temperature (20–24°C).
Measuring intracellular ATP concentrations and the ADP/ATP ratio
Values were estimated by performing bioluminescence assays based on a luciferin–luciferase reaction. The intracellular ATP concentration ([ATP]i) was measured by the ATP assay kit (Beyotime Biotechnology, Beijing, China), and the ADP/ATP ratio was determined by the ADP/ATP-lite assay kit (Vigorous Biotechnology, Beijing, China). Batches of five intact oocytes (water-injected) were incubated in the absence (0 min, as control) or presence of 3 mmol/L Na-azide for 5, 10, 15, 20, 30, 60 min. Then, samples were prepared for analysis following the manufacturer's instructions and plated in 96-white-well plates (Costar 3917, Corning Inc, USA) for luminescence readings on a FlexStation3 (Molecular Devices, Sunnyvale, CA, USA) plate reader. Serially diluted ATP (Sigma-Aldrich, St Louis, MO, USA) was used as a standard in both the ATP and ADP/ATP ratio assays. ATP values for samples were obtained from the ATP standard curve and [ATP]i values were calculated by assuming the volume of an average oocyte (diameter of 1 mm) was 500 nL. The ATP signal, expressed as the number of relative light units (RLU), was taken as value A; 10 min later an immediate reading was taken to determine the baseline ADP level (taken as value B); then the ADP in the wells was converted to ATP by the addition of ADP converting enzymes and after a 10 min incubation, a third reading was taken (value C). The ratio of ADP/ATP for each well was calculated from these three readings as follows: (C-B)/A.
Chemicals and drugs
All chemicals and drugs were obtained from Sigma-Aldrich, except PNU-37883A, which was purchased from Tocris Bioscience (Bristol, UK). The 3 mol/L sodium azide, 100 mmol/L BaCl2 (in distilled water); 100 mmol/L PNU-37883A (in ethanol); 10 mmol/L glibenclamide (in DMSO) were prepared as stock solutions and stored at −20 °C. They were diluted in the ND96K solution for the final desired concentration before each experiment.
Data analysis and statistics
Data acquisition and analyses were conducted using pClamp10.2 (Molecular Devices) and Origin 8.1 (OriginLab Corporation) software. All data were expressed as the mean±standard deviation (SD) and n indicates the number of cells used for each experimental condition. The significance of difference was assessed using a two-tailed Student's t-test between the different groups. A level of P<0.05 was considered to be statistically significant.
Results
Sensitivity of SUR/Kir6.x channels to cellular metabolic disorders
The effects of the metabolic inhibitor Na-azide (3 mmol/L) on intracellular ATP concentrations ([ATP]i) and ADP/ATP ratios were investigated in Xenopus oocytes. After application on intact oocytes (water-injected), 3 mmol/L Na-azide reduced the [ATP]i and increased the ADP/ATP ratio in a time-dependent manner, which reached steady-state levels approximately 15 min later (Figure 1A and B). The [ATP]i decreased from 3.7±0.2 mmol/L (0 min, as control) to 1.4±0.15 mmol/L (P<0.01), whereas the ADP/ATP ratio increased from 0.036±0.001 to 0.069±0.003 (P<0.01).
Effects of metabolic disorders induced by Na-azide on SUR/Kir6.x channels expressed in Xenopus oocytes. (A) The time courses of metabolic disorders induced by Na-azide at 3 mmol/L on the intracellular concentrations of ATP or (B) the ratio between ADP and ATP in Xenopus oocytes. Each value is the mean of 3–5 samples, each consisting of 5 oocytes (ie, n=15–25). bP<0.05, cP<0.01 vs control (0 min). (C) The opening effects of Na-azide (3 mmol/L) on SUR/Kir6.x channels. The dashed line indicates the control level, n=16–33 in each column. bP<0.05, cP<0.01 vs control. (D) Effects of Na-azide (3 mmol/L) on the opening rates of SUR/Kir6.x channels (all n=15). bP<0.05, cP<0.01 vs SUR2B/Kir6.1. fP<0.01 vs SUR2B/Kir6.2. iP<0.01 vs SUR2A/Kir6.2. No significance (ns) means P>0.05.
In the high-potassium (ND96K) bath solution, SUR/Kir6.x channels expressed in intact oocytes were normally closed due to the high [ATP]i, exhibiting small basal currents. We explored the effects of 3 mmol/L Na-azide on water-injected oocytes and on oocytes expressing six molecularly defined KATP channels by recording the inward current changes at −80 mV (Figure S1). Na-azide, as well as the KATP channel blockers glibenclamide and Ba2+, had no effect on the currents of water-injected oocytes. In contrast, five subtypes of the SUR/Kir6.x channels were activated by Na-azide, excluding the SUR2A/Kir6.1 channel. In most cases, steady-state currents were observed within 10–15 min after Na-azide application. The activated currents were inhibited by 10 μmol/L glibenclamide and further blocked by 1 mmol/L Ba2+.
The opening effects of Na-azide on the SUR/Kir6.x channels were compared qualitatively. The summarized data were measured at 15 min after Na-azide application and the current amplitudes were expressed relative to those before Na-azide addition (control or basal current, taken as 1) (Figure 1C). Among all the SUR/ Kir6.x channels, Na-azide was most potent to activate SUR1/Kir6.2 channel, which showed a current amplitude markedly increased to 28.12±6.56 (P<0.01); it had no opening effects on the SUR2A/Kir6.1 channel (0.95±0.14, P>0.05); and it had mild opening effects on the SUR2A/Kir6.2 channel (1.56±0.77, P<0.05). Na-azide produced increases of whole-cell currents in oocytes expressing SUR2B/Kir6.2 (19.05±4.51, P<0.01), SUR1/Kir6.1 (8.71±1.90, P<0.01) and SUR2B/Kir6.1 (2.49±0.64, P<0.01). The opening effects of Na-azide (3 mmol/L) were listed as SUR1/Kir6.2>SUR2B/Kir6.2>SUR1/Kir6.1>SUR2B/Kir6.1>SUR2A/Kir6.2>SUR2A/Kir6.1.
The opening rates of the Kir6.x/SUR channels were compared in the following tests (Figure 1D). After exposure to Na-azide, the time required to reach half-maximal response (t1/2) for the SUR1/Kir6.1 or SUR1/Kir6.2 channel were 2.21±0.44 or 2.08±0.47 min, respectively (P>0.05). The t1/2 values for the SUR2B/Kir6.1 or SUR2B/Kir6.2 channel were 5.77±0.73 or 6.33±0.73 min, respectively (P>0.05). The opening process for the SUR1/Kir6.x channel was significantly faster compared with the SUR2B/Kir6.x channel, which was faster than the SUR2A/Kir6.2 channel (t1/2=8.73±0.78 min). Therefore, the rates of the SUR/Kir6.x channels response to cellular metabolic disorders could be divided into three grades: SUR1/Kir6.x channels were fastest (shortest t1/2), SUR2B/Kir6.x channels were intermediate, and the SUR2A/Kir6.2 channel was slowest.
Intrinsic sensitivity of Kir6.x to cellular metabolic disorders
The cRNAs encoding Kir6.1 or Kir6.2 were injected separately into the Xenopus oocytes, and no detectable currents were recorded in response to Na-azide or the pore-inhibitors PNU-37883A and Ba2+. Next, we generated two ΔC mutants of Kir6.x, Kir6.1ΔC45 and Kir6.2ΔC36, which were independently and functionally expressed on the membrane surface in the absence of SUR24,26. Na-azide also had no opening effects on Kir6.1ΔC45; however, the basal currents were inhibited by the pore-inhibitors PNU-37883A and Ba2+. In contrast, the Kir6.2ΔC36 currents were stimulated by Na-azide (2.56±0.48, P<0.01) and then blocked by PNU-37883A or Ba2+. Therefore, it is reasonable to conclude that the Kir6.1 subunit had no intrinsic sensitivity, but the Kir6.2 subunit had intrinsic sensitivity to cellular metabolic disorders (Figure 2).
Effects of metabolic disorders on Kir6.x channels and the ΔC mutants expressed in Xenopus oocytes. (A) Representative time courses of currents recorded at −80 mV from Xenopus oocytes injected with cRNAs encoding Kir6.1, Kir6.1ΔC45, Kir6.2, and Kir6.2ΔC36. Whole-cell currents were evoked by a series of 300 ms voltage steps (from −120 to +50 mV with 10 mV increments, holding at −10 mV); the raw current traces at the time points (a–d) are shown on right. a: control; b: Na-Azide; c: PNU-37883A; d: BaCl2. (B) The effects of the drugs on currents mediated by Kir6.x channels and the ΔC mutants. Number of oocytes: Kir6.1, n=8; Kir6.1ΔC45, n=15; Kir6.2, n=7; Kir6.2ΔC36, n=17. cP<0.01 vs control. fP<0.01 vs Na-azide (3 mmol/L).
To elucidate the possible molecular basis underlying the sensitivity of Kir6.2 to cellular metabolism, we further studied the effects of Na-azide on three mutants of Kir6.2ΔC36, including R50G, K185E and H175A. These residues are located in the ATP-binding (R50 and K185) or pH-sensing (H175) domains of the Kir6.2 subunit. Under control conditions (in ND96K solution), the basal currents of the Kir6.2ΔC36 or Kir6.2ΔC36-H175A channel recorded at −80 mV were −388.49±61.03 or −401.92±70.06 nA, respectively (P>0.05), which were significantly smaller than those of Kir6.2ΔC36-R50G or Kir6.2ΔC36-K185E (–1543.71±102.10 or −1738.31±172.38 nA, respectively) (Figure 3A, B).
Effects of metabolic disorders on the Kir6.2ΔC36 channel with the mutations R50G, K185E and H175A expressed in Xenopus oocytes. (A) Currents recorded from oocytes expressing Kir6.2ΔC36 and its mutants. Whole-cell currents were evoked by a series of 300 ms voltage steps (from −120 to +50 mV with 10 mV increment, holding at −10 mV). (B) The basal currents of Kir6.2ΔC36 and its mutants recorded at −80 mV. n= 9–14 in each column. cP<0.01 vs Kir6.2ΔC36. fP<0.01 vs H175A. (C) The opening effects of Na-azide on Kir6.2ΔC36 and its mutants, the dashed line indicates the control level, n=9–14 in each column. cP<0.01 vs control. fP<0.01 vs Kir6.2ΔC36.
Na-azide activated the Kir6.2ΔC36 channel, and the current amplitude at −80 mV increased to 2.42±0.39 (P<0.01); it had similar opening effects on the Kir6.2ΔC36-R50G channel (2.29±0.24, P<0.01) and Kir6.2ΔC36-K185E channel (2.22±0.32, P<0.01); and it had slight opening effects on the Kir6.2ΔC36-H175A channel (1.25±0.07, P<0.01) (Figure 3A, C). Notably, the opening effects of Na-azide on the Kir6.2ΔC36-H175A channel were significantly weaker than those on the other three channels (P<0.01).
Sensitivity of SUR2B mutants to cellular metabolic disorders
We mutated one or both WA lysines within the NBDs of SUR2B to alanines, represented as K707A, K1348A and K707A/K1348A. When SUR2B and its mutants were co-expressed with Kir6.1 in Xenopus oocytes, Na-azide produced a notable activation on whole-cell currents of the wild-type (WT) SUR2B (2.38±0.71, P<0.01); whereas it had no opening effects on SUR2B-K707A (0.91±0.07, P>0.05), SUR2B-K1348A (0.92±0.07, P>0.05) and SUR2B-K707A/K1348A (0.89±0.09, P>0.05) (Figure 4A). The data indicated that mutating the WA lysine either in NBD1 or NBD2 abolished the response of the SUR2B/Kir6.1 channel to cellular metabolic disorders.
Effects of metabolic disorders on SUR2B and its mutants co-expressed with Kir6.x in Xenopus oocytes. The currents records and the effects of Na-azide on channel currents recorded from oocytes expressing SUR2B and its mutants with Kir6.1 (A) or Kir6.2 (B). The dashed line indicates the control level. The number of oocytes expressing SUR2B/Kir6.1 channels was: 25 (WT), 19 (K707A), 15 (K1348A) and 15 (K707A/K1348A). In SUR2B/Kir6.2 channels, the number was 18, 25, 12 and 9, respectively. bP<0.05, cP<0.01 vs control. No significance (ns) means P>0.05.
Similar results were found in oocytes co-expressing wild-type or mutant SUR2B with Kir6.2 (Figure 4B). Na-azide was potent to activate the SUR2B-WT channel, and the current amplitude increased markedly to 18.41±4.24 (P<0.01); it had mild opening effects on SUR2B-K707A (1.25±0.28, P<0.05) and no opening effects on SUR2B- K1348A (0.94±0.07, P>0.05) and SUR2B-K707A/K1348A (0.96±0.06, P>0.05). These data suggested that the WA lysines of NBDs, especially in NBD2 (K1348), are predominantly important in the sensitivity of the SUR2B/Kir6.2 channel to cellular metabolic disorders.
Discussion
KATP channels are well known to act as molecular sensors of cellular metabolism2, and their activation is commonly associated with disordered cellular metabolism induced by hypoxia, ischemia, or shear stress on vascular endothelial cells; therefore, they are important molecular targets for certain drugs, such as KCOs, which have been applied clinically to treat ischemic cardio-cerebral diseases or used as antihypertensive agents. In this study, we successfully expressed six subtypes of KATP channels, and all possible combinations of SUR and Kir6.x subunits, in Xenopus oocytes and found that the potency of Na-azide at 3 mmol/L activates SUR/Kir6.x channels in the following order: SUR1/Kir6.2>SUR2B/Kir6.2>SUR1/Kir6.1>SUR2B/Kir6.1>SUR2A/Kir6.2>SUR2A/Kir6.1. In addition, the rates of the five SUR/Kir6.x channels responding to cellular metabolic disorders were ranked as SUR1/Kir6.2 or SUR1/Kir6.1>SUR2B/Kir6.2 or SUR2B/Kir6.1>SUR2A/Kir6.2. It is reasonable to suggest that SUR1/Kir6.2 was most sensitive, with the largest extent and shortest t1/2 of activation, whereas SUR2A/Kir6.1 was insensitive to cellular metabolic disorders. Interestingly, the SUR2A/Kir6.2 channel was only slightly activated by metabolic disorders (∼50% increase of currents). The vascular-type KATP channel (SUR2B/Kir6.1) was also only slightly activated by metabolic disorders (∼1.5-fold increase of currents), indicating that under hypertension, KATP channels in blood vessels can be partly activated by the disordered cellular metabolism resulting from elevated shear stress. Treatment with antihypertensive KATP channel openers (KCOs) is necessary to reduce blood pressure more effectively.
The sensitivity of SUR/Kir6.x channels to the metabolic inhibitor Na-azide was influenced by both the pore-forming subunit Kir6.x and the regulatory subunit SUR; we studied intrinsic sensitivity of Kir6.x to cellular metabolic disorders and further explored the possible underlying molecular basis. When the endoplasmic reticulum retention signal (RKR motif) was removed, the C-terminal truncations of Kir6.x (Kir6.1ΔC45 and Kir6.2ΔC36) could express functionally without SUR24,26. We found that the independently expressed Kir6.2 subunit (Kir6.2ΔC36) could be immediately activated after applying Na-azide at 3 mmol/L. Conversely, the Kir6.1 subunit (Kir6.1ΔC45) was unresponsive to Na-azide. Therefore, Kir6.2, but not Kir6.1, had intrinsic sensitivity to cellular metabolic disorders. It is known that ATP inhibits KATP channels by binding directly to Kir6.22,27 and our data showed that the intracellular ATP concentrations of oocytes decreased markedly from 3.7 mmol/L to 1.4 mmol/L after a 15 min application of 3 mmol/L Na-azide; therefore, Kir6.2ΔC36 responded to azide-induced metabolic disorders because there were less ATP binding to the inhibitory site of the Kir6.2 subunit. The molecular basis of the ATP inhibitory site of the Kir6.2 subunit has been studied in detail, leading to the identification of several key residues that form an ATP-binding pocket2,3,27. For example, R50 in the N terminus and K185 in the C terminus interact with the β-phosphate and γ-phosphate of ATP, respectively. Therefore, when the ATP-binding site was impaired, Kir6.2ΔC36-R50G and Kir6.2ΔC36-K185E exhibited much more significant basal currents because the blocking effect of the resting ATP levels was weaker.
In addition, cellular pH changes are common in hypoxia, ischemia and acidosis4,6,28,29. Intracellular H+ has been demonstrated to be a potent activator of KATP channels and the residue H175 in Kir6.2 is involved in pH-sensing29. Therefore, another interesting phenomenon observed in our study was that the sensitivity of Kir6.2ΔC36-H175A to cellular metabolic disorders was severely impaired, which may be due to the allosteric effects of H+ and ATP in regulating KATP channel activity29.
The Kir6.1 subunit was not inherently sensitive to 3 mmol/L Na-azide, therefore, the major possible mechanism for Kir6.1-containing channel activation during metabolic disorders may be located in SUR. The Kir6.2-containing channels responded significantly differently to Na-azide mainly because of their differences in SUR subunits. The SUR subunit, especially the WA motifs in NBDs, the stimulatory site that interacts with Mg-adenine nucleotides2,30,31,32,33, may play a more important role in metabolic sensing of SUR/Kir6.x channels. To test these hypotheses, two subtypes of the KATP channels, SUR2B/Kir6.1 and SUR2B/Kir6.2, were further studied in detail because they all have definite and intermediate sensitivity to azide-induced metabolic disorders and have not been studied in the oocyte expression system.
The results of SUR2B and its mutants co-expressed with Kir6.1 indicated that both the single-point mutations (K707A and K1348A) and double-point mutation (K707A/ K1348A) were unresponsive to azide-induced metabolic disorders, suggesting that the WA lysines in NBD1and NBD2 are both required for coupling metabolic disorders to channel activation in SUR2B/Kir6.1 channels. Similarly, in SUR2B/Kir6.2 channels, the mutation in NBD2 (K1348) also completely abrogated the response of the channel to metabolic disorders; and, although Na-azide could slightly stimulate the NBD1 (K707) mutant, the channel exhibited an extremely impaired sensitivity to cellular metabolic disorders. These findings are different in some respects from those of previously reported experiments34. The discrepancies may be due to the differences in expression systems (Xenopus oocytes vs HEK-293) and the different agents used to induce metabolic disorders: Na-azide vs sodium cyanide (NaCN) plus 2-deoxyglucose (2-DG). Given this evidence from other studies35, our data supports the idea that the metabolic sensitivity of SUR2B/Kir6.x channels is endowed mostly by the SUR2B subunit and the WA lysines (K707 and K1348) of the NBDs are primarily responsible for the sensitivity of SUR2B-containing channels to cellular metabolic disorders. It is uncertain whether the reconstituted double-point mutants were truly expressed on membrane surface. The answer seems to be yes because the basal currents of these mutants were inhibited by the pore-inhibitor PNU-37883A or Ba2+ in contrast to the water-injected oocytes.
In conclusion, our study demonstrated that among the six subtypes of SUR/Kir6.x channels, SUR1/Kir6.2 was the most sensitive, whereas SUR2A/Kir6.1 was insensitive to cellular metabolic disorders induced by 3 mmol/L Na-azide; and the sensitivities followed this rank: SUR1/Kir6.2>SUR2B/Kir6.2>SUR1/Kir6.1>SUR2B/Kir6.1>SUR2A/Kir6.2 >SUR2A/Kir6.1. The Kir6.2 subunit, rather than the Kir6.1 subunit, had intrinsic sensitivity to cellular metabolic disorders, and the molecular basis associated with residues involved in ATP-binding (R50 and K185) or pH-sensing (H175). The sensitivity of SUR/Kir6.x channels to cellular metabolic disorders are more predominantly determined by the SUR subunit. The WA lysines of both NBDs play a key role in determining the metabolic sensitivities of the SUR2B/Kir6.x (especially SUR2B/Kir6.1) channels. Therefore, the results of this study provide useful information for understanding the pathophysiological role of different KATP channel subtypes under metabolic disorder conditions, and we provided the basis for further study of the pharmacology of KCOs against cardio-cerebral vascular diseases, hypertension or pulmonary hypertension with metabolic disorders.
Author contribution
Hai WANG designed the research and wrote the paper; Chun-gang LI performed the research, analyzed the data and wrote the paper; Wen-yu CUI participated in the research.
References
Seino S, Miki T . Physiological and pathophysiological roles of ATP-sensitive K+ channels. Prog Biophys Mol Biol 2003; 81: 133–76.
Nichols CG . KATP channels as molecular sensors of cellular metabolism. Nature 2006; 440: 470–6.
Olson TM, Terzic A . Human KATP channelopathies: diseases of metabolic homeostasis. Pflugers Arch 2010; 460: 295–306.
Ballanyi K . Protective role of neuronal KATP channels in brain hypoxia. J Exp Biol 2004; 207: 3201–12.
Flagg TP, Enkvetchakul D, Koster JC, Nichols CG . Muscle KATP channels: recent insights to energy sensing and myoprotection. Physiol Rev 2010; 90: 799–829.
Hsu CY, Fang SY, Chen YZ, Roan JN, Chang SW, Huang CC, et al. Cardiovascular protection of activating KATP channel during ischemia-reperfusion acidosis. Shock 2012; 37: 653–8.
Barakat AI, Lieu DK, Gojova A . Ion channels in shear stress sensing in vascular endothelium. In: Bazopoulou D, Voglis G, Tavernarakis N, Benson CJ, Mccleskey EW, editors. Molecular sensors for cardiovascular homeostasis. Vienna: Springer-Verlag GmbH; 2007. Part III: 155–70.
Chatterjee S, Levitan I, Wei Z, Fisher AB . KATP channels are an important component of the shear-sensing mechanism in the pulmonary microvasculature. Microcirculation 2006; 13: 633–44.
Title LM, Lonn E, Charbonneau F, Fung M, Mather KJ . Relationship between brachial artery flow-mediated dilatation, hyperemic shear stress, and the metabolic syndrome. Vasc Med 2008; 13: 263–70.
Babenko AP, Aguilar-Bryan L, Bryan J . A view of SUR/KIR6.x KATP channels. Annu Rev Physiol 1998; 60: 667–87.
Hibino H, Inanobe A, Furutani K, Murakami S, Findlay I, Kurachi Y . Inwardly rectifying potassium channels: their structure, function, and physiological roles. Physiol Rev 2010; 90: 291–366.
Proks P, Ashcroft FM . Modeling KATP channel gating and its regulation. Prog Biophys Mol Biol 2009; 99: 7–19.
Kono Y, Horie M, Takano M, Otani H, Xie LH, Akao M, et al. The properties of the Kir6.1-6.2 tandem channel co-expressed with SUR2A. Pflugers Arch 2000; 440: 692–8.
Yamada M, Isomoto S, Matsumoto S, Kondo C, Shindo T, Horio Y, et al. Sulphonylurea receptor 2B and Kir6.1 form a sulphonylurea-sensitive but ATP-insensitive K+ channel. J Physiol 1997; 499: 715–20.
Li L, Wu J, Jiang C . Differential expression of Kir6.1 and SUR2B mRNAs in the vasculature of various tissues in rats. J Membr Biol 2003; 196: 61–9.
Shi W, Cui N, Wu Z, Yang Y, Zhang S, Gai H, et al. Lipopolysaccharides up-regulate Kir6.1/SUR2B channel expression and enhance vascular KATP channel activity via NF-kappaB-dependent signaling. J Biol Chem 2010; 285: 3021–9.
Zhou F, Yao HH, Wu JY, Ding JH, Sun T, Hu G . Opening of microglial KATP channels inhibits rotenone-induced neuroinflammation. J Cell Mol Med 2008; 12: 1559–70.
Thomzig A, Wenzel M, Karschin C, Eaton MJ, Skatchkov SN, Karschin A, et al. Kir6.1 is the principal pore-forming subunit of astrocyte but not neuronal plasma membrane KATP channels. Mol Cell Neurosci 2001; 18: 671–90.
Liu Y, Ren G, O'Rourke B, Marban E, Seharaseyon J . Pharmacological comparison of native mitochondrial KATP channels with molecularly defined surface KATP channels. Mol Pharmacol 2001; 59: 225–30.
Ng KE, Schwarzer S, Duchen MR, Tinker A . The intracellular localization and function of the ATP-sensitive K+ channel subunit Kir6.1. J Membr Biol 2010; 234: 137–47.
Gribble FM, Ashfield R, Ammala C, Ashcroft FM . Properties of cloned ATP-sensitive K+ currents expressed in Xenopus oocytes. J Physiol 1997; 498: 87–98.
Tammaro P, Proks P, Ashcroft FM . Functional effects of naturally occurring KCNJ11 mutations causing neonatal diabetes on cloned cardiac KATP channels. J Physiol 2006; 571: 3–14.
Dabrowski M, Larsen T, Ashcroft FM, Bondo Hansen J, Wahl P . Potent and selective activation of the pancreatic beta-cell type KATP channel by two novel diazoxide analogues. Diabetologia 2003; 46: 1375–82.
Zerangue N, Schwappach B, Jan YN, Jan LY . A new ER trafficking signal regulates the subunit stoichiometry of plasma membrane KATP channels. Neuron 1999; 22: 537–48.
Moreau C, Prost AL, Derand R, Vivaudou M . SUR, ABC proteins targeted by KATP channel openers. J Mol Cell Cardiol 2005; 38: 951–63.
Tucker SJ, Gribble FM, Zhao C, Trapp S, Ashcroft FM . Truncation of Kir6.2 produces ATP-sensitive K+ channels in the absence of the sulphonylurea receptor. Nature 1997; 387: 179–83.
Antcliff JF, Haider S, Proks P, Sansom MS, Ashcroft FM . Functional analysis of a structural model of the ATP-binding site of the KATP channel Kir6.2 subunit. EMBO J 2005; 24: 229–39.
Wang X, Wu J, Li L, Chen F, Wang R, Jiang C . Hypercapnic acidosis activates KATP channels in vascular smooth muscles. Circ Res 2003; 92: 1225–32.
Wu J, Cui N, Piao H, Wang Y, Xu H, Mao J, et al. Allosteric modulation of the mouse Kir6.2 channel by intracellular H+ and ATP. J Physiol 2002; 543: 495–504.
Matsuo M, Kimura Y, Ueda K . KATP channel interaction with adenine nucleotides. J Mol Cell Cardiol 2005; 38: 907–16.
Matsuo M, Tanabe K, Kioka N, Amachi T, Ueda K . Different binding properties and affinities for ATP and ADP among sulfonylurea receptor subtypes, SUR1, SUR2A, and SUR2B. J Biol Chem 2000; 275: 28757–63.
Yamada M, Kurachi Y . A functional role of the C-terminal 42 amino acids of SUR2A and SUR2B in the physiology and pharmacology of cardiovascular ATP-sensitive K+ channels. J Mol Cell Cardiol 2005; 39: 1–6.
Masia R, Enkvetchakul D, Nichols CG . Differential nucleotide regulation of KATP channels by SUR1 and SUR2A. J Mol Cell Cardiol 2005; 39: 491–501.
Farzaneh T, Tinker A . Differences in the mechanism of metabolic regulation of ATP-sensitive K+ channels containing Kir6.1 and Kir6.2 subunits. Cardiovasc Res 2008; 79: 621–31.
Gribble FM, Tucker SJ, Ashcroft FM . The essential role of the Walker A motifs of SUR1 in KATP channel activation by Mg-ADP and diazoxide. EMBO J 1997; 16: 1145–52.
Acknowledgements
We thank Prof LY JAN (Howard Hughes Medical Institute) for kindly providing cDNAs for the KATP channels used for expression in Xenopus oocytes.
This work was supported by grants from the State Key Research Project of China (No AWS11J003) and the National Basic Research “973” Program (No 2012CB518200 and JCKY2013000B001).
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Figure S1 is available in the Acta Pharmacologica Sinica's website.
Supplementary information
Supplementary Information, Figure S1
Representative time courses of currents recorded at -80 mV from water-injected Xenopus oocytes (B1), oocytes expressing SUR1/Kir6.1 (B2), SUR2A/Kir6.1 (B3), SUR2B/Kir6.1 (B4), SUR1/Kir6.2 (B5), SUR2A/Kir6.2 (B6) and SUR2B/Kir6.2 (B7). (DOC 24 kb)
Rights and permissions
About this article
Cite this article
Li, Cg., Cui, Wy. & Wang, H. Sensitivity of KATP channels to cellular metabolic disorders and the underlying structural basis. Acta Pharmacol Sin 37, 134–142 (2016). https://doi.org/10.1038/aps.2015.134
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2015.134
Keywords
This article is cited by
-
Ion channels research in the post-genomic era
Acta Pharmacologica Sinica (2016)