Abstract
Aim:
To explore the mechanisms underlying the protection by SO2 preconditioning against rat myocardial ischemia/reperfusion (I/R) injury.
Methods:
Male Wistar rats underwent 30-min left coronary artery ligation followed by 120-min reperfusion. An SO2 donor (1 μmol/kg) was intravenously injected 10 min before the ischemia, while LY294002 (0.3 mg/kg) was intravenously injected 30 min before the ischemia. Plasma activities of LDH and CK were measured with an automatic enzyme analyzer. Myocardial infarct size was detected using Evans-TTC method. The activities of caspase-3 and -9 in myocardium were assayed using a commercial kit, and the levels of p-Akt, Akt, PI3K and p-PI3K were examined with Western blotting.
Results:
Pretreatment with SO2 significantly reduced the myocardial infarct size and plasma LDH and CK activities, as well as myocardial caspase-3 and -9 activities in the rats. Furthermore, the pretreatment significantly increased the expression levels of myocardial p-Akt and p-PI3K p85. Administration of the PI3K inhibitor LY294002 blocked all the effects induced by SO2 pretreatment.
Conclusion:
The results suggest that the PI3K/Akt pathway mediates the protective effects of SO2 preconditioning against myocardial I/R injury in rats.
Similar content being viewed by others
Introduction
Ischemia preconditioning was first described by Murry in 19861. The author demonstrated that brief episodes of ischemia reperfusion (I/R) could induce resistance to cell injury following lethal ischemia and reduce infarct size. A similar protective effect of preconditioning was observed in other organs and tissues, which led to the induction of an endogenous protective substance to resist lethal ischemia. However, applying ischemia preconditioning in clinical therapy is not practical. Therefore, pharmacological preconditioning, such as with adenosine, nicorandil and isoflurane, has been found to show a protective effect similar to that of ischemia preconditioning on myocardial I/R2.
SO2 was considered to be a pollutant gas and toxic in mammals. SO2 dissociates to its derivatives bisulfite and sulfite (1:3 M/M) in neutral fluid and plasma in vivo3. Recently, SO2 was found to be generated endogenously4. Sulfite has previously been identified as the physiological form of SO25,6,7. SO2 has physiologic effects on the cardiovascular system, including regulation of negative cardiac function and inhibition of L-type calcium channel activity8. In addition, the pathophysiologic effects of SO2 have recently been found to aggravate myocardial I/R injury9. Zhang et al9 observed that SO2 treatment after I/R could provoke radical generation and aggravate I/R injury. A recent study revealed that low doses (1–10 μmol/kg) of SO2 preconditioning could inhibit myocardial injury10. However, the mechanism responsible for protection by SO2 preconditioning against myocardial I/R injury is not fully understood.
The phosphoinositide 3-kinase (PI3K)/Akt pathway has been identified as a key component of the protective mechanism of ischemia preconditioning11. PI3Ks play an important role in the control of cell growth, proliferation, survival and migration12. The activation of Akt, which is downstream of PI3K, may ameliorate I/R injury13. The PI3K/Akt pathway is also involved in the preconditioning of hydrogen sulfide (H2S), another sulfur-containing gas in the methionine metabolic pathway with effects on myocardial I/R similar to those of SO214. The aim of the present study was to investigate whether the PI3K/Akt pathway is involved in the cardioprotective effect of SO2 preconditioning.
Materials and methods
The investigation was approved by the Institutional Authority for Laboratory Animal Care of Peking University and complied with the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication No 85–23, revised in 1996).
Creation of myocardial I/R rat model in vivo
Male Wistar rats (250–300 g) were from Vital River (Beijing, China). The rats were anaesthetized using urethane (1 g/kg) via intraperitoneal injection. The surgical procedures were performed as previously described10. After pericardiotomy, a 5–0 silk suture was placed under the left coronary artery (LCA), which was occluded by tightening the snare using a lightweight hemostatic clamp. After 30 min of myocardial ischemia, the suture was loosened for 120 min for reperfusion15,16. The sham-operated animals underwent the same surgical procedures except that the suture around the LCA was not fastened. Standard lead II electrocardiography was used for monitoring during I/R. Ischemia was confirmed by a transient decrease in blood pressure and cyanosis on the myocardial surface. Reperfusion was indicated by an epicardial hyperemic response and the rapid disappearance of cyanosis.
Experimental protocol for assessing I/R in rats
To determine the effect of SO2 preconditioning on myocardial I/R injury and expression levels of p-Akt, Akt, PI3K, and p-PI3K in the rat myocardium, healthy, clean-grade male Wistar rats were randomly divided into a sham group, in which rats underwent the LCA surgical procedures except that the suture around the LCA was not fastened (n=6); an I/R group, in which LCA ligation was performed as described above (n=7); an I/R+SO2 group (n=7); and a 0.3 mg/kg LY294002 plus 1 μmol/kg SO2 preconditioning group (I/R+LY294002+SO2 group, n=7). For rats in the I/R+SO2 group and I/R+LY294002+SO2 group, 10 min before ischemia, an SO2 donor (NaHSO3 and Na2SO3, 1:3 MM ratio) was intravenously injected at 1 μmol/kg for 5 min. In the sham group, the rats were intravenously injected with the same volume of normal saline. A total of 0.3 mg/kg LY294002 was given via right external jugular intravenous administration 30 min before ischemia in rats in the I/R+LY294002+SO2 group.
To determine the effect of SO2 treatment on expression levels of p-Akt, Akt, PI3K, and p-PI3K in the rat myocardium, rats that did not undergo surgical operation were divided into a control group, in which rats were intravenously injected with the same volume of normal saline for 5 min (n=6); a 1 μmol/kg SO2 treatment group, in which an SO2 donor at 1 μmol/kg was intravenously injected for 5 min (SO2 group, n=7); and a 0.3 mg/kg LY294002 plus 1 μmol/kg SO2 group (LY294002+SO2 group, n=7), in which an SO2 donor at 1 μmol/kg was intravenously injected 20 min after 0.3 mg/kg LY294002 had been given via right external jugular intravenous administration. At the end of the experiment, plasma myocardial enzymes [creatine kinase (CK) and lactate dehydrogenase (LDH)], myocardial infarct size and myocardial caspase-3 and -9 activities were detected. The expression levels of p-Akt, Akt, PI3K, and p-PI3K in the rat myocardium were detected by Western blotting.
Measurement of LDH and CK activities in rats with I/R
After treatment, plasma samples were obtained from carotid aorta using a heparinized syringe and immediately centrifuged. The activities of LDH and CK were assayed using an automatic enzyme analyzer (Hitachi 7080, Hitachi, Japan).
Determination of myocardial infarct size in rats with I/R
At the end of the experiment, the LCA was reoccluded, and the area at risk (AAR) in the heart was delineated by injecting Evans blue dye (1 mL of a 3% solution) via the external jugular vein. The heart was rapidly excised, washed with 0.9% saline and cut into 5 transverse slices of equal thickness (2.0 mm) from the apex to the base. The slices were incubated for 10 min in phosphate-buffered 1% 2,3,5-triphenyltetrazolium chloride (TTC) at 37 °C and then fixed with 10% formalin solution. The AAR was the area that was not stained with Evans blue dye. The AARs not stained by TTC were defined as the area of infarction (AI). The AAR, AI and ventricle size (VS) were assessed by a blinded observer using computer-assisted planimetry (NIH Image 1.57 software). The procedures for determining the AAR and AI were as previously described17.
Measurement of myocardial caspase-3 and -9 activities in rats with I/R
We used the AAR of the ischemic heart as a sample to determine the activity of caspase-3 and -9. The activities of caspase-3 and -9 were assayed using the caspase activity quantitative detection kit (Genmed Scientifics Inc, Shanghai, China) according to the manufacturer's instructions.
Western blot analysis in vivo
We used the AAR of the ischemic heart as a sample for Western blot analysis of Akt and PI3K expression. After homogenization with lysis buffer (50 mmol/L Tris-HCl, pH 7.5, 150 mmol/L NaCl, 1% Nonidet P-40, and 0.5% sodium deoxycholate), the supernatants were boiled and separated using sodium dodecyl polyacrylamide gel electrophoresis (SDS-PAGE) and transferred onto a nitrocellulose membrane. The antibodies against Akt and PI3K were purchased from Cell Signaling Technology (Boston, MA, USA). The antibody against GAPDH (0411) was purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Anti-rabbit and anti-mouse HRP-labeled antibodies and the ECL detection reagents were purchased from Santa Cruz Biotechnology. The X-ray film used for Western blotting was obtained from Kodak (Rochester, NY, USA). The developed signal was visualized using an enhanced chemiluminescence (ECL) detection kit and quantified using AlphaImager (San Leandro, CA, USA)18.
Statistical analysis
All data were expressed as the mean±SD. Significant differences were evaluated by a one-way ANOVA followed by a post hoc test (least significant difference, LSD test). Statistical significance was set at P<0.05. All analyses were performed using SPSS 16.0 (Chicago, IL, USA).
Results
SO2 preconditioning reduced the myocardial infarct size of rats with I/R
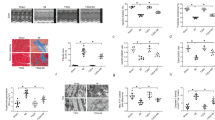
We determined the infarct size using the Evans-TTC method to evaluate the direct effect of SO2 preconditioning on myocardial I/R injury17. The area at risk was expressed as a ratio of AAR to VS (AAR/VS), and the area of the infarct size was expressed as a ratio of AI to AAR (AI/AAR). There were no differences in AAR/VS between the I/R, I/R+SO2, and I/R+LY294002+SO2 groups. In rats treated with I/R, the percentage of AI/AAR was approximately 43.37%. Compared with the I/R group, the I/R+SO2 group showed significant reductions in myocardial infarct size by 32.91%. By contrast, pretreatment with LY294002 successfully abolished the effect of 1 μmol/kg SO2 pretreatment, and the myocardial infarct size was increased by 58.70% (P<0.01) (Figure 1A).
Effect of SO2 preconditioning on myocardial injury. Effect of SO2 preconditioning on myocardial infarct size (A), n=21. Effect of SO2 preconditioning on plasma lactate dehydrogenase (LDH) and creatine kinase (CK) activities (B), n=27. Mean±SD. bP<0.05, cP<0.01 vs the sham group. eP<0.05, fP<0.01 vs the I/R group. hP<0.05, iP<0.01 vs the I/R+SO2 group.
SO2 preconditioning reduced plasma LDH and CK activities in rats with I/R
To evaluate the extent of myocardial injury in rats with I/R, we detected plasma LDH and CK activities. At the end of the experiment, compared with activities in the sham group, the plasma CK and LDH activities in the I/R group were significantly increased — by 105.38% and 549.24%, respectively (P<0.01). Pretreatment with SO2 significantly reduced plasma LDH and CK activities by 32.91% and 27.13%, respectively (P<0.01), compared with the I/R group (P<0.05). However, the plasma LDH and CK activities in the I/R+LY294002+SO2 group were higher than those in the I/R+SO2 group (P<0.05) (Figure 1B).
SO2 preconditioning reduced myocardial caspase-3 and -9 activities
Compared with levels in the sham group, the myocardial caspase-3 and -9 activities in the I/R group were significantly increased—by 103% and 82.69%, respectively (P<0.01). Pretreatment with an SO2 donor significantly reduced the increased myocardial caspase-3 and -9 activities by 44.05% and 38.3%, respectively (P<0.01), as compared with the I/R group. However, the myocardial caspase-3 activities in the I/R+LY294002+SO2 group were higher than those in the I/R+SO2 group (P<0.05) (Figure 2).
Effect of SO2 preconditioning on myocardial caspase-3 and −9 activities. Mean±SD. n=27. cP<0.01 vs the sham group. fP<0.01 vs the I/R group. hP<0.05, iP<0.01 vs the I/R+SO2 group.
SO2 preconditioning induced myocardial PI3K expression prior to ischemia in rats
To investigate whether PI3K/Akt is involved in cardioprotection via SO2 preconditioning, we detected PI3K phosphorylation levels using Western blot analysis. Rat hearts were extracted 10 min after SO2 injection and prior to myocardial ischemia. LY294002, which was originally identified as an inhibitor of PI3K, was used in the experiment. Compared with the control group, pretreatment with 1 μmol/kg of SO2 increased myocardial p-PI3K p85 expression by 45.21% (P<0.01) but did not affect the expression levels of p-PI3K p55. However, pretreatment with LY294002 significantly decreased the expression levels of p-PI3K p85 by 18.89% (P<0.05) but did not affect the expression levels of p-PI3K p55 (Figure 3).
Effect of SO2 on PI3K expression prior to ischemia. Mean±SD. n=20. cP<0.01 vs the control group. eP<0.05 vs the SO2 group.
SO2 preconditioning further increased myocardial Akt and PI3K expression levels in rats with I/R
Furthermore, we assessed the expression of Akt and PI3K in rats with myocardial I/R. LY294002, a PI3K inhibitor, was also used in this experiment. Compared with the sham group, rats with I/R alone showed an increase in Akt and PI3K p85 phosphorylation levels by 97.64% and 65.36%, respectively (P<0.05 or P<0.01), whereas the expression levels of p-PI3K p55 did not change. In addition, pretreatment with 1 μmol/kg of SO2 further increased Akt and PI3K p85 phosphorylation levels by 89.29% and 58.07%, respectively (P<0.05 or P<0.01), but the expression levels of p-PI3K p55 did not change. Pretreatment with LY294002 reversed the above effect, and myocardial Akt and PI3K p85 phosphorylation levels were decreased by 33.60% and 52.11% (both P<0.01), respectively, but the expression levels of p-PI3K p55 did not change (Figure 4).
Effect of preconditioning with SO2 on the expression of Akt (A) and PI3K (B) after ischemia reperfusion. Mean±SD. n=27. bP<0.05 vs the sham group. fP<0.01 vs the SO2 group. iP<0.01 vs the I/R+SO2 group.
Discussion
The present study revealed that the PI3K/Akt pathway is involved in the cardioprotective effect of SO2 preconditioning against myocardial I/R injury in rats.
It has been reported that SO2 can induce negative inotropic effects and relax isolated aortic rings and vascular smooth muscles19,20. Previously, we found that SO2 treatment after reperfusion aggravated myocardial I/R injury. Therefore, we further explored the cardioprotective effect of SO2 preconditioning on I/R injury. We recently found that low doses (1–10 μmol/kg) of SO2 preconditioning had a protective effect on rat myocardial I/R injury10. The heart infarct size and increased plasma myocardial enzymes are characteristics of I/R injury in the heart21. In the present study, treatment with I/R significantly increased plasma CK and LDH activities in rats with myocardial I/R. In addition, the infarct size was also observed using Evans blue-TTC staining. Pretreatment with SO2 significantly decreased the infarct size and plasma CK and LDH activities, which agrees with previous reports10. Additionally, in the present study, we observed that SO2 pretreatment significantly decreased caspase-3 and -9 activities in the myocardium of rats with I/R. In a previous investigation, we also showed that preconditioning with SO2 improved cardiac functionality in rats with myocardial I/R injury10. However, the mechanism underlying SO2 preconditioning in I/R injury is not fully understood.
PI3K/Akt was thought to be involved in I/R and plays an important role in ischemia preconditioning11,22,23. PI3Ks play a key role in the control of cell growth, proliferation, survival and migration12. It was reported that the adenoviral gene transfer of activated phosphatidylinositol 3′-kinase and Akt inhibited the apoptosis of hypoxic cardiomyocytes in vitro24. Additionally, Akt activation ameliorated cardiac function and prevented injury after transient cardiac ischemia in vivo25. However, whether the PI3K/Akt pathway was involved in the cardioprotective effect of SO2 preconditioning was not clear.
We previously found that, after injecting 1 μmol/kg SO2 donor (NaHSO3 and Na2SO3, 1:3 MM ratio), the circulatory SO2 level increased from 7.07±0.42 μmol/L to 16.3±3.44 μmol/L10. In the present study, we observed that treatment with an SO2 donor significantly increased PI3K p85 phosphorylation expression levels but did not affect the expression levels of p-PI3K p55. An inhibitor of PI3K, LY294002, reversed the above effect of SO2 and reduced the PI3K p85 phosphorylation levels.
Next, the expression levels of Akt and PI3K were detected after I/R. We found that SO2 preconditioning markedly increased the levels of Akt and PI3K p85 phosphorylation and protected the rats from I/R myocardial injury. However, pretreatment with LY294002 successfully reversed the above cardioprotective effect of SO2 along with inhibition of the PI3K/Akt pathway. These data indicated that the PI3K/Akt pathway mediated the cardioprotective effect of SO2 preconditioning. However, the mechanism underlying the SO2-mediated activation of the PI3K-Akt signaling pathway is not clear. Previous studies indicated that SO2 could increase oxidative stress in myocardial tissues26, and the over-production of oxidants upregulated the PI3K-Akt signaling pathway27,28. Therefore, SO2 may have activated the PI3K-Akt signaling pathway by stimulating the oxidative response. However, further work is needed to determine the exact mechanisms through which SO2 upregulates the PI3K/Akt pathway in rats.
In conclusion, SO2 preconditioning had a cardioprotective effect on rats with myocardial I/R injury. The PI3K/Akt pathway was likely involved in the process of SO2 preconditioning. Further studies are needed to determine the exact mechanisms through which SO2 preconditioning protects against I/R myocardial injury in rats.
Author contribution
Jun-bao DU, Hong-fang JIN, and Xin-bao WANG designed the research; Man-man ZHAO, Jin-yan YANG, and Xin-bao WANG performed the research and contributed new analytical reagents and tools; Man-man ZHAO, Hong-fang JIN, Jin-yan YANG, and Xin-bao WANG collected and analyzed data; Xin-bao WANG and Chao-shu TANG interpreted the data; Man-man ZHAO, Jin-yan YANG, and Xin-bao WANG wrote the paper; Chao-shu TANG and Hong-fang JIN revised the paper.
References
Murry CE, Jennings RB, Reimer KA . Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 1986; 74: 1124–36.
Toller WG, Kersten JR, Gross ER, Pagel PS, Warltier DC . Isoflurane preconditions myocardium against infarction via activation of inhibitory guanine nucleotide binding proteins. Anesthesiology 2000; 92: 1400–7.
Shapiro R . Genetic effects of bisulfite (sulfur dioxide). Mutat Res 1977; 39: 149–75.
Stipanuk MH, Dominy JE Jr, Lee JI, Coloso RM . Mammalian cysteine metabolism: new insights into regulation of cysteine metabolism. J Nutr 2006; 136: 1652S–1659S.
Meng Z, Zhang B . Polymerase chain reaction-based deletion screening of bisulfite (sulfur dioxide)-enhanced gpt-mutants in CHO-AS52 cells. Mutat Res 1999; 425: 81–5.
Mottley C, Trice TB, Mason RP . Direct detection of the sulfur trioxide radical anion during the horseradish peroxidase-hydrogen peroxide oxidation of sulfite (aqueous sulfur dioxide). Mol Pharmacol 1982; 22: 732–7.
Reed GA, Ryan MJ, Adams KS . Sulfite enhancement of diolepoxide mutagenicity: the role of altered glutathione metabolism. Carcinogenesis 1990; 11: 1635–9.
Zhang RY, Du JB, Sun Y, Chen S, Tsai HJ, Yuan L, et al. Sulfur dioxide derivatives depress L-type calcium channel in rat cardiomyocytes. Clin Exp Pharmacol Physiol 2011; 38: 416–22.
Zhang S, Du J, Jin H, Li W, Liang Y, Geng B, et al. Endogenous sulfur dioxide aggravates myocardial injury in isolated rat heart with ischemia and reperfusion. Transplantation 2009; 87: 517–24.
Wang XB, Huang XM, Ochs T, Li XY, Jin HF, Tang CS, et al. Effect of sulfur dioxide preconditioning on rat myocardial ischemia/reperfusion injury by inducing endoplasmic reticulum stress. Basic Res Cardiol 2011; 106: 865–78.
Shanmuganathan S, Hausenloy DJ, Duchen MR, Yellon DM . Mitochondrial permeability transition pore as a target for cardioprotection in the human heart. Am J Physiol Heart Circ Physiol 2005; 289: H237–42.
Wymann MP, Zvelebil M, Laffargue M . Phosphoinositide 3–kinase signalling-which way to target? Trends Pharmacol Sci 2003; 24: 366–76.
Forster K, Paul I, Solenkova N, Staudt A, Cohen MV, Downey JM, et al. NECA at reperfusion limits infarction and inhibits formation of the mitochondrial permeability transition pore by activating p70S6 kinase. Basic Res Cardiol 2006; 101: 319–26.
Hu Y, Chen X, Pan TT, Neo KL, Lee SW, Khin ES, et al. Cardioprotection induced by hydrogen sulfide preconditioning involves activation of ERK and PI3K/Akt pathways. Pflugers Arch 2008; 455: 607–16.
Song JQ, Teng X, Cai Y, Tang CS, Qi YF . Activation of Akt/GSK-3beta signaling pathway is involved in intermedin (1–53) protection against myocardial apoptosis induced by ischemia/reperfusion. Apoptosis 2009; 14: 1299–307.
Zatta AJ, Kin H, Lee G, Wang N, Jiang R, Lust R, et al. Infarct-sparing effect of myocardial postconditioning is dependent on protein kinase C signalling. Cardiovasc Res 2006; 70: 315–24.
Elrod JW, Greer JJ, Bryan NS, Langston W, Szot JF, Gebregzlabher H, et al. Cardiomyocyte-specific overexpression of NO synthase-3 protects against myocardial ischemia-reperfusion injury. Arterioscler Thromb Vasc Biol 2006; 26: 1517–23.
Wei H, Zhang R, Jin H, Liu D, Tang X, Tang C, et al. Hydrogen sulfide attenuates hyperhomocysteinemia-induced cardiomyocytic endoplasmic reticulum stress in rats. Antioxid Redox Signal 2010; 12: 1079–91.
Zhang QN, Meng ZQ . The negative inotropic effects of gaseous sulfur dioxide and its derivatives in the isolated perfused rat heart. Environ Toxicol 2012; 27: 175–84.
Zhang QN, Meng ZQ . The vasodilator mechanism of sulfur dioxide on isolated aortic rings of rats: Involvement of the K+ and Ca2+ channels. Eur J Pharmacol 2009; 602: 117–23.
Bopassa JC, Ferrera R, Gateau-Roesch O, Couture-Lepetit E, Ovize M . PI3-kinase regulates the mitochondrial transition pore in controlled reperfusion and postconditioning. Cardiovasc Res 2006; 69: 178–85.
Zhang CM, Gao L, Zheng YJ, Yang HT . Berbamine protects the heart from ischemia/reperfusion injury by maintaining cytosolic Ca2+ homeostasis and preventing calpain activation. Circ J 2012; 76: 1993–2002.
Izuishi K, Fujiwara M, Hossain MA, Usuki H, Maeta H . Significance of phosphoinositide 3-kinase pathway on ischemic preconditioning followed by ischemia reperfusion in mice liver. Transplant Proc 2003; 35: 132–3.
Matsui T, Li L, del Monte F, Fukui Y, Franke TF, Hajjar RJ, et al. Adenoviral gene transfer of activated phosphatidylinositol 3′-kinase and Akt inhibits apoptosis of hypoxic cardiomyocytes in vitro. Circulation 1999; 100: 2373–9.
Matsui T, Tao J, del Monte F, Lee KH, Li L, Picard M, et al. Akt activation preserves cardiac function and prevents injury after transient cardiac ischemia in vivo. Circulation 2001; 104: 330–5.
Liang Y, Liu D, Ochs T, Tang C, Chen S, Zhang S, et al. Endogenous sulfur dioxide protects against isoproterenol-induced myocardial injury and increases myocardial antioxidant capacity in rats. Lab Invest 2011; 91: 12–23.
Lu Q, Zhai Y, Cheng Q, Liu Y, Gao X, Zhang T, et al. The Akt-FoxO3a-manganese superoxide dismutase pathway is involved in the regulation of oxidative stress in diabetic nephropathy. Exp Physiol 2012. DOI: 10.1113/expphysiol.2012.068361.
Wang Z, Zhang H, Xu X, Shi H, Yua X, Wang X, et al. bFGF inhibits ER stress induced by ischemic oxidative injury via activation of the PI3K/Akt and ERK1/2 pathways. Toxical Lett 2012; 212: 137–46.
Acknowledgements
This work was supported by the Major Basic Research Program of China (2012CB517806 and 2011CB503904) and the National Natural Science Foundation of China (81121061, 81070111, 31130030, and 81070212).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, Mm., Yang, Jy., Wang, Xb. et al. The PI3K/Akt pathway mediates the protection of SO2 preconditioning against myocardial ischemia/reperfusion injury in rats. Acta Pharmacol Sin 34, 501–506 (2013). https://doi.org/10.1038/aps.2012.204
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2012.204
Keywords
This article is cited by
-
Near-infrared light-triggered nano-prodrug for cancer gas therapy
Journal of Nanobiotechnology (2021)
-
Mechanism of Human Umbilical Cord Mesenchymal Stem Cells Derived-Extracellular Vesicle in Cerebral Ischemia-Reperfusion Injury
Neurochemical Research (2021)
-
Short-term effects of ambient air pollutants and myocardial infarction in Changzhou, China
Environmental Science and Pollution Research (2018)
-
Methylophiopogonanone A suppresses ischemia/reperfusion-induced myocardial apoptosis in mice via activating PI3K/Akt/eNOS signaling pathway
Acta Pharmacologica Sinica (2016)
-
The PI3K/Akt, p38MAPK, and JAK2/STAT3 signaling pathways mediate the protection of SO2 against acute lung injury induced by limb ischemia/reperfusion in rats
The Journal of Physiological Sciences (2016)