Abstract
Aim:
Cysteinyl leukotriene receptor 1 (CysLT1 receptor) is located in epithelial cells, and translocates from the plasma membrane to the nucleus in a ligand-dependent manner. Here, we investigated whether CysLT1 receptors translocated to the nucleus in endothelial cells after ischemic insult in vitro and whether it was involved in ischemic injury to endothelial cells.
Methods:
EA.hy926 cell line, derived from human umbilical vein endothelial cells, was subjected to oxygen-glucose deprivation (OGD). The expression and distribution of CysLT1 receptors were detected by immunofluorescent staining, immunogold labeling and immunoblotting analyses. Cell viability was evaluated using MTT reduction assay. Necrosis and apoptosis were determined by double fluorescent staining with propidium iodide and Hoechst 33342.
Results:
CysLT1 receptors were primarily distributed in the cytoplasm and nucleus in EA.hy926 cells, and few was found in the cell membrane. OGD induced the translocation of CysLT1 receptors from the cytoplasm to the nucleus in a time-depen dent manner, with a peak reached at 6 h. OGD-induced nuclear translocation of CysLT1 receptors was inhibited by pretreatment with the CysLT1 receptor antagonist pranlukast (10 μmol/L), or by preincubation with NLS-pep, a peptide corresponding to the nuclear localization sequence of CysLT1 receptor (10 μg/mL). However, zileuton, an inhibitor of 5-lipoxygenase that was a key enzyme in cysteinyl leukotriene generation, did not inhibit the nuclear translocation of CysLT1 receptors. Moreover, preincubation with NLS-pep (0.4 μg/mL) significantly ameliorated OGD-induced cell viability reduction and necrosis.
Conclusion:
CysLT1 receptors in endothelial cells translocate to the nucleus in a ligand-independent manner after ischemic insult in vitro, and it is involved in the ischemic injury.
Similar content being viewed by others
Introduction
Cysteinyl leukotrienes (CysLTs), namely LTC4, LTD4, and LTE4, are important inflammatory mediators produced from arachidonic acid via the 5-lipoxygenase (5-LOX) pathway. CysLTs exert their actions through the activation of the CysLT1 and CysLT2 receptors, which are G-protein-coupled receptors (GPCRs)1. The CysLT1 receptor has been extensively studied, and its selective antagonists have been used for the treatment of bronchial asthma2. Generally, CysLT1 receptor ligands initiate a series of intracellular signaling events by interacting with the receptor on the plasma membrane2. However, the CysLT1 receptor is also localized in the nuclear envelope in colon cancer cells and the epithelial cell line Int 407. The ligand LTD4 also induces translocation of the CysLT1 receptor from the plasma membrane to the nucleus3,4. In the process of nuclear translocation, a nuclear localization sequence (NLS) is necessary for the nuclear import of proteins. An NLS is contained within the structure of the CysLT1 receptor. Mutation of the NLS inhibits nuclear translocation of the CysLT1 receptor and LTD4-induced cell proliferation3. The nuclear distribution and translocation of the CysLT1 receptor may regulate physiological processes in cells. Previous studies have suggested that the nuclear distribution of the CysLT1 receptor may be involved in tumor cell proliferation3,4. However, whether pathological stimuli can induce the nuclear translocation of the CysLT1 receptor remains unknown.
The CysLT1 receptor mediates various pathophysiological responses in different disease processes. One typical response is a CysLT1 receptor-mediated change in vascular permeability. We have reported that the CysLT1 receptor mediates ischemic brain injury in vivo5,6. This effect is potentially governed by a CysLT1 receptor-mediated increase in blood-brain barrier permeability and, consequently, brain edema, after ischemia7,8. Endothelial cells are crucial to vascular permeability; thus, their injury or death after ischemia may contribute to secondary post-ischemic injury and tissue edema9,10. We have reported that the CysLT1 receptor antagonist pranlukast protects endothelial cells against ischemia-like injury11. However, the distribution of the CysLT1 receptor in endothelial cells after ischemia is not known. In intestinal epithelial cells, the CysLT1 receptor translocates to the nucleus after stimulation by the ligand LTD4, which mediates cell proliferation3. Based on these findings, whether ischemia induces nuclear translocation of the CysLT1 receptor and how this translocation affects ischemic injury warrants further study.
Therefore, we investigated whether the CysLT1 receptor translocates to the nucleus after in vitro ischemia and its involvement in ischemic injury to endothelial cells. In this study, the EA.hy926 cell line, derived from human umbilical vein endothelial cells (HUVECs), was used. This cell line displays a wide range of properties ascribed to differentiated endothelial cells and has been used to investigate endothelial cell inflammatory responses12,13,14.
Materials and methods
Cell culture and oxygen-glucose deprivation (OGD)
EA.hy926 cells were a kind gift from Dr CJ Edgell (University of North Carolina, Chapel Hill, NC, USA). Cells were cultured in Dulbecco's modified Eagle's medium (DMEM, Gibco, Grand Island, NY, USA), supplemented with 10% heat-inactivated fetal calf serum, penicillin (100 U/mL) and streptomycin (100 mg/mL). Experiments were conducted 24 h after cells were seeded.
OGD was performed as described previously15. Briefly, the original medium was removed; the cells were washed twice with glucose-free Earle's balanced salt solution (EBSS) and placed in fresh glucose-free EBSS. Cultures were then placed in an incubator containing 5% CO2 and 95% N2 at 37 °C for 2 to 8 h. Control cultures were maintained in glucose-containing EBSS under normal conditions. Ten μmol/L pranlukast (a gift from Ono Pharmaceutical Co, Osaka, Japan), 10 μmol/L zileuton, a 5-LOX inhibitor (Comens Chemical Co, Beijing, China) or 10 μmol/L pyrrolidine dithiocarbamate (PDTC), a specific NF-κB inhibitor (Aldrich-Sigma, Saint Louis, MO, USA), was added to the culture 30 min before OGD exposure and maintained during OGD.
Osmotic loading of synthetic peptides into EA.hy926 cells
A peptide corresponding to a putative NLS of the CysLT1 receptor [amino acids 312–323, (NLS-pep)], and its mutant, in which the NLS was replaced by a non-NLS of CysLT2 [amino acids 323–330, (NLS-mut)], were synthesized by GL Biochem Ltd (Shanghai, China)3. Osmotic loading of peptides was performed as described previously16,17. In brief, EA.hy926 cells were rinsed in glucose-containing EBSS, incubated for 10 min with loading solution (0.5 mol/L sucrose, 10% polyethylene glycol 1000, 10% FBS, and 10 mg/mL NLS-pep or NLS-mut in DMEM, buffered with 25 mmol/L HEPES, pH 6.8), and then rapidly rinsed with a hypotonic solution (6.5 vol H2O:3.5 vol DMEM, buffered with 25 mmol/L HEPES, pH 6.8). Cells were then incubated in DMEM and used immediately for experiments.
Nuclear isolation and immunoblotting
EA.hy926 cells were rinsed twice with ice-cold PBS and collected with a cell scraper. The cell membrane, cytosolic and nuclear fractions were extracted using a protein extraction kit (DBI-1031, DBI, USA) according to the manufacturer's instructions. The protein concentration was determined by Coomassie blue protein assay. To determine CysLT1 receptor expression, samples (30 μg protein) were separated by 10% SDS-polyacrylamide gel electrophoresis and then electrically transferred to nitrocellulose membranes. The membranes were blocked with 5% bovine serum albumin and incubated overnight at 4 °C with a rabbit polyclonal antibody against the CysLT1 receptor (1:100, Cayman Chemical, USA). Then, the membranes were washed repeatedly and incubated with IRDye™700 conjugated affinity-purified anti-rabbit IgG (1:8000, Rockland Immunochemicals, Inc, USA). Finally, the protein bands were detected using an Odyssey fluorescent scanner (LI-COR Bioscience, USA). The purity of subcellular fractions was routinely verified by immunoblotting with antibodies specific for markers of different subcellular components: CD44 for the plasma membrane, GAPDH for the cytoplasm, and lamin B for the nucleus. Data are reported as fold increases compared with control cells.
Immunofluorescent staining
EA.hy926 cells cultured on coverslips were fixed with cold methanol (-20 °C) for 5 min and subsequently incubated with 10% normal goat serum for 120 min. Cells were then incubated with a rabbit polyclonal antibody against the CysLT1 receptor (1:100, Cayman Chemical, USA) or a rabbit polyclonal antibody against NF-κB (1:50, Santa Cruz Biotechnology, Santa Cruz, CA, USA) as the primary antibody at 4 °C overnight. After washing with PBS, the cells were incubated for 2 h with FITC-conjugated goat anti-rabbit IgG antiserum (1:200, Chemicon, USA) and examined under a fluorescence microscope (Olympus X51) or a laser scanning confocal microscope (Olympus FV1000). Control coverslips were incubated with normal goat serum instead of the primary antibody, and no positive staining was observed.
Cell viability and cell death
Cell viability was evaluated by the MTT reduction assay. At the end of OGD, the media were removed, and the cells were incubated in 0.5 mg/mL 3-(4,5-dimethyl-2-thiazolyl)-2,5-diphenyl-2H-tetrazolium bromide (MTT) solution for 2 h in a humidified 5% CO2 incubator at 37 °C. The incubation was stopped by removing the media and adding dimethylsulfoxide (DMSO) to solubilize the formed formazan salt. The absorbance of formazan was read at 490 nm on a microplate reader (ELX800, Bio-Tex Instruments Inc, USA). Data are reported as the percentage of the absorbance in control cells.
As described previously, death of endothelial cells by necrosis and apoptosis was determined by double fluorescent staining with propidium iodide (PI) and Hoechst 3334211. In brief, monolayers of cells on slides were stained with PI (10 μg/mL) and Hoechst 33342 (10 μg/mL) for 10 min at 37 °C. After washing with EBSS, the cells were fixed in 3.7% (v/v) paraformaldehyde and then examined under a fluorescence microscope. The necrotic cells stained red by PI and the apoptotic cells showed nuclear condensation and fragmentation after Hoechst 33342 staining. The total necrotic and apoptotic cells were counted, and the percentages of necrotic and apoptotic cells were calculated.
Statistical analysis
Data are presented as mean±SEM. For statistical comparisons, differences between groups were analyzed by a one-way analysis of variance (ANOVA), followed by Dennett's post-hoc test. A value of P<0.05 was considered to be statistically significant.
Results
The CysLT1 receptor is localized in the nuclear compartment
The subcellular distribution of the CysLT1 receptor in EA.hy926 cells was analyzed by confocal microscopy after immunofluorescent staining and by electron microscopy after immunogold labeling. Immunofluorescent staining showed that the CysLT1 receptor was primarily distributed in the cytoplasm and the nucleus (Figure 1A). This result was verified by immunogold labeling followed by electron microscopy (Figure 1B). To further confirm the nuclear localization of the CysLT1 receptor, the nuclei were isolated, and the purity of the nuclear fraction was confirmed by immunoblotting with markers for the nucleus (Lamin B), cell membrane (CD44) and cytoplasm (GAPDH). Lamin B was detected only in the purified nuclear fraction. The CysLT1 receptor was primarily detected in the nuclear and cytosolic fractions, and little was detected in the cell membrane (Figure 1C). The specificity of anti-CysLT1 receptor antibody (Cayman Chemical) used in these experiments has been verified in previous reports18,19.
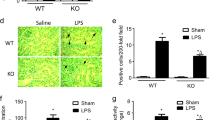
Nuclear localization of the CysLT1 receptor in EA.hy926 cells. Confocal microscopy assay showing CysLT1 receptor distribution after immunostaining and DAPI counterstaining (A). Immunogold detection of nuclear CysLT1 receptors (B). EA.hy926 cells were immunostained with antibody against the CysLT1 receptor followed by gold-particle conjugated secondary antibody. Arrows indicate gold particles, and arrow heads indicate the nuclear envelope. Immunoblotting analysis of CysLT1 receptor expression (C). The membrane (M), cytosolic (C), and nuclear (N) fractions were extracted, and equal amounts of proteins were used for SDS polyacrylamide gel analysis. The purity of subcellular fractions was verified by immunoblotting for CD44 for the plasma membrane, GAPDH for the cytoplasm, and lamin B for the nucleus. Scale bar=5 μm in Figure 1A and 0.5 μm in Figure 1B.
OGD-induced nuclear translocation of the CysLT1 receptor
Next, we determined whether induction of in vitro ischemia by OGD induces nuclear translocation of the CysLT1 receptor. We found that the CysLT1 receptor in the nucleus increased gradually after OGD, and CysLT1 receptor-positive staining was almost entirely distributed in the nucleus 6 or 8 h after OGD (Figure 2A). The results were verified by immunoblotting assay, which showed that the amount of CysLT1 receptor in the nucleus significantly increased 4–8 h after OGD, with the maximum at 6 h (Figure 2D), whereas the amount of CysLT1 receptor in the cytoplasm decreased (Figure 2C). In addition, we found no change in the total CysLT1 receptor expression level after OGD (Figure 2B).
OGD time-dependently induces nuclear translocation of the CysLT1 receptor in EA.hy926 cells. Intracellular distribution of the CysLT1 receptor (A), immunoblotting analysis of CysLT1 receptor expression (B), immunoblotting analysis of the CysLT1 receptor in the cytoplasmic fraction (C), and immunoblotting analysis of the CysLT1 receptor in the nuclear fraction (D) after OGD are shown. OGD did not change the CysLT1 receptor expression level, but induced nuclear translocation of the CysLT1 receptor in a time-dependent manner. Data are expressed as mean±SEM, n=4 experiments and bP<0.05 vs control. Data were analyzed by one-way ANOVA. Ctrl, control; OGD, oxygen-glucose deprivation. Scale bar=50 μm.
NLS-pep and a CysLT1 receptor antagonist inhibit the nuclear translocation of the CysLT1 receptor
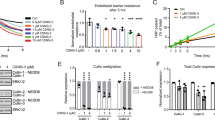
Because a peptide corresponding to the NLS inhibits nuclear translocation of the corresponding protein17, we used the peptide corresponding to the NLS of the CysLT1 receptor (NLS-pep) to determine its effect on translocation. The results show that preincubation with NLS-pep significantly inhibited OGD-induced nuclear translocation of the CysLT1 receptor, whereas the control NLS-mut had no effect (Figure 3A and 3B). The inhibitory effect of NLS-pep was specific to the CysLT1 receptor because NLS-pep had no effect on OGD-induced nuclear translocation of NF-κB (Figure 4). We also assessed the effects of the CysLT1 receptor antagonist pranlukast and the 5-lipoxygenase inhibitor zileuton on translocation. The results showed that pranlukast, but not zileuton, inhibited the translocation of the CysLT1 receptor 6 h after OGD (Figure 3A and 3C).
NLS-pep and pranlukast inhibit OGD-induced nuclear translocation of the CysLT1 receptor in EA.hy926 cells. Six hours of OGD significantly induced nuclear translocation of the CysLT1 receptor. The translocation was reduced by NLS-pep (a peptide corresponding to the NLS of the CysLT1 receptor) and pranlukast (a CysLT1 receptor antagonist), but not by NLS-mut or zileuton (a 5-lipoxygenase inhibitor). Data are expressed as mean±SEM, n=4, bP<0.05 vs control, eP<0.05. Data were analyzed by one-way ANOVA. Ctrl, control; OGD, oxygen-glucose deprivation; Pran, pranlukast; Zileu, zileuton. Scale bar=50 μm.
NLS-pep does not inhibit OGD-induced nuclear translocation of NF-κB in EA.hy926 cells. Eight hours of OGD significantly induced nuclear translocation of NF-κB. The translocation was reduced by PDTC (a specific NF-κB inhibitor), but not by NLS-pep or NLS-mut. Ctrl, control; OGD, oxygen-glucose deprivation; PDTC, pyrrolidine dithiocarbamate. Scale bar=50 μm.
Nuclear translocation of the CysLT1 receptor is involved in OGD-induced cell damage
Finally, we investigated whether nuclear translocation of the CysLT1 receptor is involved in OGD-induced cell damage. OGD reduced cell viability in a time-dependent manner (data not shown). Cell viability was reduced by 34% at 6 h after OGD as determined by the MTT reduction assay. The addition of NLS-pep or NLS-mut alone did not induce any cell damage (Figure 5A). The presence of NLS-pep significantly increased cell viability after OGD, whereas NLS-mut did not have this effect (Figure 5A).
NLS-pep protects EA.hy926 cells from OGD-induced damage. Cell viability was determined by MTT reduction assay (A), and cell death by PI (red) and Hoechst 33342 (blue) staining (B and C). Necrosis was the primary cause of OGD-induced cell death. OGD-induced cell viability reduction and cell necrosis were ameliorated by NLS-pep, but not by NLS-mut. Data are expressed as mean±SEM, n=8, bP<0.05 vs control, and eP<0.05 vs OGD at 8 h. Data were analyzed by one-way ANOVA. Scale bar=50 μm.
Many necrotic cells and a few apoptotic cells were detected 6 h after OGD (Figure 5B). Necrosis was the main pathway of OGD-induced cell death, which is consistent with the findings of our previous study11. OGD-induced necrosis was significantly reduced by 0.4 μg/mL NLS-pep (from 35% to 23%), but not by NLS-mut (Figure 5B and 5C). In addition, we found that pranlukast, but not zileuton, protected EA.hy926 cells against OGD-induced damage (data not shown), similar to our previous study11.
Discussion
In the present study, we found that the CysLT1 receptor in EA.hy926 cells was primarily distributed in the cytoplasm and the nucleus, with little detected in the plasma membrane. This finding differs from that in epithelial cells and mast cells, in which the CysLT1 receptor is primarily distributed in the plasma membrane and the nucleus3,19. This difference may be cell-type specific, because the same anti-CysLT1 receptor antibody was used here and in other studies3,19.
The most important finding is that the CysLT1 receptor translocates from the cytoplasm to the nucleus after in vitro OGD and is involved in ischemic injury to endothelial cells. Increasing evidence has demonstrated that a number of G protein-coupled receptors are located in the nuclear membrane or intranuclear sites. These receptors include members of all major classes of GPCRs, such as lysophosphatidic acid receptor-1 (LPA1R)20, metabotropic glutamate receptors (mGluR5)21, apelin receptors22, platelet-activating factor (PAF) receptors23, angiotensin 2 type I receptors17,24, prostaglandin EP3 receptors25, endothelin receptors26 and β-adrenergic receptors27,28. The significance of the nuclear translocation of GPCRs is not known. Limited reports have shown that nuclear LPA1R or PAF receptors modulate pro-inflammatory gene expression in cells that stably express these receptors20,23. Furthermore, mGluR5 on nuclear membranes mediates intranuclear Ca2+ changes in neurons21, and nuclear β-adrenergic receptors modulate gene expression in adult rat hearts28. Here, we found that ischemic stimulation induced nuclear translocation of the CysLT1 receptor in a time-dependent manner. The CysLT1 receptor was almost entirely distributed in the nucleus after 6 or 8 h of OGD. This nuclear distribution could be attenuated by inhibiting its nuclear import sequence using NLS-pep. Moreover, NLS-pep decreased ischemia-induced cell damage. These findings indicate that nuclear translocation of the CysLT1 receptor is involved in ischemic injury of endothelial cells. This phenomenon is different from the ligand-induced proliferation mediated by nuclear translocation of the CysLT1 receptor in intestinal epithelial cells3.
The mechanisms underlying OGD-induced nuclear translocation of the CysLT1 receptor remain unknown. However, it has been reported that GPCRs are translocated from the plasma membrane to the nucleus in either a ligand-dependent3,29 or ligand-independent manner22. We found that the CysLT1 receptor antagonist pranlukast inhibited OGD-induced nuclear translocation of the receptor, but the 5-lipoxygenase inhibitor zileuton had no effect. If endogenous agonists of CysLTs induced this translocation, zileuton would be effective because it inhibits enhanced production of CysLTs after exposure to OGD30. Moreover, we have reported that pranlukast ligand-independently attenuates ischemic injury in EA.hy926 cells by inhibiting reactive oxygen species production and nuclear factor-kappaB activation11. Therefore, we suggest that the CysLT1 receptor may translocate to the nucleus after OGD, in part by a ligand-independent mechanism. Based on previous and present findings3,4, we hypothesize that the CysLT1 receptor exhibits ligand-dependent or ligand-independent nuclear translocation.
In conclusion, our results show that after in vitro ischemia, the CysLT1 receptor translocates to the nucleus in a ligand-independent manner and that this translocation is involved in ischemic injury to endothelial cells.
Author contribution
San-hua FANG, Ka-na LIN, and Xue-qin HUANG performed the experiments; Yun-bi LU and Wei-ping ZHANG supervised all aspects of the research and revised the manuscript; and San-hua FANG and Er-qing WEI prepared the manuscript.
References
Singh RK, Gupta S, Dastidar S, Ray A . Cysteinyl leukotrienes and their receptors: molecular and functional characteristics. Pharmacology 2010; 85: 336–49.
Capra V, Thompson MD, Sala A, Cole DE, Folco G, Rovati GE . Cysteinyl-leukotrienes and their receptors in asthma and other inflammatory diseases: critical update and emerging trends. Med Res Rev 2007; 27: 469–527.
Nielsen CK, Campbell JI, Ohd JF, Morgelin M, Riesbeck K, Landberg G, et al. A novel localization of the G-protein-coupled CysLT1 receptor in the nucleus of colorectal adenocarcinoma cells. Cancer Res 2005; 65: 732–42.
Parhamifar L, Sime W, Yudina Y, Vilhardt F, Morgelin M, Sjolander A . Ligand-induced tyrosine phosphorylation of cysteinyl leukotriene receptor 1 triggers internalization and signaling in intestinal epithelial cells. PLoS One 2010; 5: e14439.
Fang SH, Wei EQ, Zhou Y, Wang ML, Zhang WP, Yu GL, et al. Increased expression of cysteinyl leukotriene receptor-1 in the brain mediates neuronal damage and astrogliosis after focal cerebral ischemia in rats. Neuroscience 2006; 140: 969–79.
Yu GL, Wei EQ, Wang ML, Zhang WP, Zhang SH, Weng JQ, et al. Pranlukast, a cysteinyl leukotriene receptor-1 antagonist, protects against chronic ischemic brain injury and inhibits the glial scar formation in mice. Brain Res 2005; 1053: 116–25.
Wang ML, Huang XJ, Fang SH, Yuan YM, Zhang WP, Lu YB, et al. Leukotriene D4 induces brain edema and enhances CysLT2 receptor-mediated aquaporin 4 expression. Biochem Biophys Res Commun 2006; 350: 399–404.
Zhang LH, Wei EQ . Neuroprotective effect of ONO-1078, a leukotriene receptor antagonist, on transient global cerebral ischemia in rats. Acta Pharmacol Sin 2003; 24: 1241–7.
Xu J, He L, Ahmed SH, Chen SW, Goldberg MP, Beckman JS, et al. Oxygen-glucose deprivation induces inducible nitric oxide synthase and nitrotyrosine expression in cerebral endothelial cells. Stroke 2000; 31: 1744–51.
Kim JH, Yu YS, Kim KW, Min BH . The role of clusterin in in vitro ischemia of human retinal endothelial cells. Curr Eye Res 2007; 32: 693–8.
Fang SH, Yuan YM, Peng F, Li CT, Zhang LH, Lu YB, et al. Pranlukast attenuates ischemia-like injury in endothelial cells via inhibiting reactive oxygen species production and nuclear factor-kappaB activation. J Cardiovasc Pharmacol 2009; 53: 77–85.
Edgell CJ, McDonald CC, Graham JB . Permanent cell line expressing human factor VIII-related antigen established by hybridization. Proc Natl Acad Sci U S A 1983; 80: 3734–7.
Ahn K, Pan S, Beningo K, Hupe D . A permanent human cell line (EA.hy926) preserves the characteristics of endothelin converting enzyme from primary human umbilical vein endothelial cells. Life Sci 1995; 56: 2331–41.
Bouis D, Hospers GA, Meijer C, Molema G, Mulder NH . Endothelium in vitro: a review of human vascular endothelial cell lines for blood vessel-related research. Angiogenesis 2001; 4: 91–102.
Ge QF, Wei EQ, Zhang WP, Hu X, Huang XJ, Zhang L, et al. Activation of 5-lipoxygenase after oxygen-glucose deprivation is partly mediated via NMDA receptor in rat cortical neurons. J Neurochem 2006; 97: 992–1004.
Ahmad F, Li PM, Meyerovitch J, Goldstein BJ . Osmotic loading of neutralizing antibodies demonstrates a role for protein-tyrosine phosphatase 1B in negative regulation of the insulin action pathway. J Biol Chem 1995; 270: 20503–8.
Lu D, Yang H, Shaw G, Raizada MK . Angiotensin II-induced nuclear targeting of the angiotensin type 1 (AT1) receptor in brain neurons. Endocrinology 1998; 139: 365–75.
Sjostrom M, Jakobsson PJ, Heimburger M, Palmblad J, Haeggstrom JZ . Human umbilical vein endothelial cells generate leukotriene C4 via microsomal glutathione S-transferase type 2 and express the CysLT1 receptor. Eur J Biochem 2001; 268: 2578–86.
Jiang Y, Borrelli LA, Kanaoka Y, Bacskai BJ, Boyce JA . CysLT2 receptors interact with CysLT1 receptors and down-modulate cysteinyl leukotriene dependent mitogenic responses of mast cells. Blood 2007; 110: 3263–70.
Gobeil F Jr, Bernier SG, Vazquez-Tello A, Brault S, Beauchamp MH, Quiniou C, et al. Modulation of pro-inflammatory gene expression by nuclear lysophosphatidic acid receptor type-1. J Biol Chem 2003; 278: 38875–83.
O'Malley KL, Jong YJ, Gonchar Y, Burkhalter A, Romano C . Activation of metabotropic glutamate receptor mGlu5 on nuclear membranes mediates intranuclear Ca2+ changes in heterologous cell types and neurons. J Biol Chem 2003; 278: 28210–9.
Lee DK, Lanca AJ, Cheng R, Nguyen T, Ji XD, Gobeil F Jr, et al. Agonist-independent nuclear localization of the Apelin, angiotensin AT1, and bradykinin B2 receptors. J Biol Chem 2004; 279: 7901–8.
Marrache AM, Gobeil F Jr, Bernier SG, Stankova J, Rola-Pleszczynski M, Choufani S, et al. Proinflammatory gene induction by platelet-activating factor mediated via its cognate nuclear receptor. J Immunol 2002; 169: 6474–81.
Chen R, Mukhin YV, Garnovskaya MN, Thielen TE, Iijima Y, Huang C, et al. A functional angiotensin II receptor-GFP fusion protein: evidence for agonist-dependent nuclear translocation. Am J Physiol Renal Physiol 2000; 279: F440–8.
Gobeil F Jr, Dumont I, Marrache AM, Vazquez-Tello A, Bernier SG, Abran D, et al. Regulation of eNOS expression in brain endothelial cells by perinuclear EP(3) receptors. Circ Res 2002; 90: 682–9.
Boivin B, Chevalier D, Villeneuve LR, Rousseau E, Allen BG . Functional endothelin receptors are present on nuclei in cardiac ventricular myocytes. J Biol Chem 2003; 278: 29153–63.
Boivin B, Lavoie C, Vaniotis G, Baragli A, Villeneuve LR, Ethier N, et al. Functional beta-adrenergic receptor signalling on nuclear membranes in adult rat and mouse ventricular cardiomyocytes. Cardiovasc Res 2006; 71: 69–78.
Vaniotis G, Del Duca D, Trieu P, Rohlicek CV, Hebert TE, Allen BG . Nuclear beta-adrenergic receptors modulate gene expression in adult rat heart. Cell Signal 2010; 23: 89–98.
Estrada R, Wang L, Jala VR, Lee JF, Lin CY, Gray RD, et al. Ligand-induced nuclear translocation of S1P(1) receptors mediates Cyr61 and CTGF transcription in endothelial cells. Histochem Cell Biol 2009; 131: 239–49.
Li CT, Zhang WP, Lu YB, Fang SH, Yuan YM, Qi LL, et al. Oxygen-glucose deprivation activates 5-lipoxygenase mediated by oxidative stress through the p38 mitogen-activated protein kinase pathway in PC12 cells. J Neurosci Res 2009; 87: 991–1001.
Acknowledgements
This study was supported by grants from the National Natural Science of China (81273491, 30801397, 30873053, and 81072618), Zhejiang Provincial Natural Science of China (Y207343 and Y2090069), and Fundamental Research Funds for the Central Universities (2009QNA7008). We thank Dr IC BRUCE for critically reading and revising this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fang, Sh., Lin, Kn., Huang, Xq. et al. Nuclear translocation of cysteinyl leukotriene receptor 1 is involved in oxygen-glucose deprivation-induced damage to endothelial cells. Acta Pharmacol Sin 33, 1511–1517 (2012). https://doi.org/10.1038/aps.2012.101
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2012.101
Keywords
This article is cited by
-
Copper-catalyzed C2-selective alkynylation of chromones via 1,4-conjugate addition
Molecular Diversity (2024)
-
Cysteinyl leukotrienes regulate endothelial cell inflammatory and proliferative signals through CysLT2 and CysLT1 receptors
Scientific Reports (2013)