Abstract
Data sources
Medline, Embase, Cochrane Central Register of Controlled Trials (CENTRAL), CINHAL, Web of Science, Scopus, LILACS, Conference proceedings of the International Society of Paediatric Oncology, American Society of Clinical Oncology, American Society of Hematology, American Society of Pediatric Hematology and Oncology, and Multinational Association of Supportive Care in Cancer and the reference lists of identified studies.
Study selection
Two reviewers independently selected studies for inclusion with randomised controlled trials (RCTs) and quasi-RCTs being considered.
Data extraction and synthesis
Data were extracted using a specifically developed form and study quality was assessed using the Cochrane risk of bias tool. Dichotomous outcomes data were synthesised using the risk ratio (RR) and 95% confidence interval (CI). Continuous outcomes measured using different scales were synthesised using the standardised mean difference (SMD) while those using the same scale were synthesised using the weighted mean difference (WMD).
Results
Eighteen RCTs involving 1144 patients were included. Four trials were considered to be at low risk of bias across all domains. Prophylactic LLLT reduced the overall risk of severe mucositis (risk ratio (RR) 0.37, 95% confidence interval (CI) 0.20 to 0.67; P = 0.001). Compared to placebo/no therapy LLLT also reduced the following outcomes; severe mucositis at the time of anticipated maximal mucositis RR = 0.34, (95% CI; 0.20 to 0.59); overall mean grade of mucositis SMD -1.49, (95% CI; -2.02 to -0.95); duration of severe mucositis WMD -5.32, 95% (CI; -9.45 to -1.19) and incidence of severe pain (RR 0.26, 95% CI; 0.18 to 0.37).
Conclusions
Prophylactic LLLT reduced severe mucositis and pain in patients with cancer and HSCT recipients. Future research should identify the optimal characteristics of LLLT and determine feasibility in the clinical setting.
Similar content being viewed by others
Commentary
The main objective of this comprehensive systematic review was to establish if using low-level laser therapy (LLLT) prophylactically would reduce mucositis severity in adults and children undergoing cancer treatment or haematopoietic stem cell transplantation (HSCT).
The authors performed a very extensive search across six online databases; they also reviewed relevant conferences and went over references manually with no language restriction.
They included RCTs using LLLT as prophylaxis for oral mucositis until 2014.
The primary outcome was overall incidence of mucositis but also they evaluated its severity, duration and incidence of pain.
Two of the reviewers independently evaluated the studies using clear inclusion and exclusion criteria set a priori and the results were clearly reported. Agreement between reviewers was very high and it was practised during study inclusion.
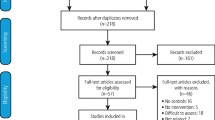
Eighteen studies were included in the review and their quality was assessed based on the risk of bias using the Cochrane tool. Four studies were considered low risk of bias overall. Ten studies were included in the meta-analysis of the primary outcome.
The results presented as risk reduction (RR) for the presence or no of severe mucositis showed an overall beneficial effect when LLLT was used of 0.37 RR, 95% CI 0.20 to 0.67; p=0.001. Heterogeneity between studies was high. Statistically significant benefits were also evident for each of the secondary outcomes but incidence of pain.
The authors evaluated publication bias using a funnel plot. After adjusting for 'missing' studies, the effect, although reduced to RR 0.51, 95% CI 0.29 to 0.90, continues to show benefits.
Despite this promising result, no clear recommendation can be made because of the variability among studies concerning the laser characteristics, schedule, evaluation interval and assessment scale. Only one study included a paediatric population.
No patient centred outcomes were evaluated. Improvement of quality of life or personal preferences may be more important than any objective measurement on this patient population.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Lillian Sung, Division of Haematology/Oncology, The Hospital for Sick Children, Toronto, Ontario, Canada; Program in Child Health Evaluative Sciences, The Hospital for Sick Children, Peter Gilgan Centre for Research and Learning, Toronto, Ontario, Canada E-mail: lillian.sung@sickkids.ca
Oberoi S, Zamperlini-Netto G, Beyene J, Treister NS, Sung L. Effect of prophylactic low level laser therapy on oral mucositis: a systematic review and meta-analysis. PLoS One 2014; 9: e107418.
Rights and permissions
About this article
Cite this article
Spivakovsky, S. Low level laser therapy may reduce risk of oral mucositis. Evid Based Dent 16, 49 (2015). https://doi.org/10.1038/sj.ebd.6401095
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6401095