Abstract
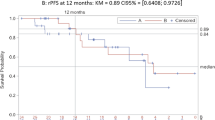
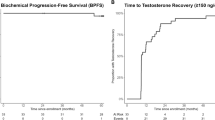
To compare combination therapy with bicalutamide 80 mg and a luteinizing hormone-releasing hormone agonist (LHRH-A) versus LHRH-A alone in Japanese men with untreated advanced prostate cancer. A total of 205 patients with stage C/D prostate cancer were randomized to either LHRH-A+once-daily oral bicalutamide 80 mg or placebo. Primary study variables have been reported previously. Secondary variables included: time to achieve prostate-specific antigen⩽4 ng/ml, time-to-treatment failure (TTTF), time-to-disease progression (TTP), overall survival (OS), adverse events and adverse drug reactions. Following combination therapy with bicalutamide 80 mg, there were significant (P<0.001) advantages over LHRH-A alone in terms of TTTF and TTP, but the difference in the interim OS was not statistically significant. First-line combination therapy with bicalutamide 80 mg in Japanese patients with advanced prostate cancer offers significant benefits over LHRH-A alone, with respect to TTTF and TTP. Follow-up for OS continues.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Cancer Registration Committee of the Japanese Urological Association. Clinicopathological statistics on registered prostate cancer patients in Japan: 2000 report from the Japanese Urological Association. Int J Urol 2005; 12: 46–61.
Akaza H, Usami M, Hinotsu S, Ogawa O, Kagawa S, Kitamura T et al. Characteristics of patients with prostate cancer who have initially been treated by hormone therapy in Japan: J-CaP surveillance. Jpn J Clin Oncol 2004; 34: 329–336.
Klotz L, Schellhammer P, Carroll K . A re-assessment of the role of combined androgen blockade for advanced prostate cancer. BJU Int 2004; 93: 1177–1182.
Prostate Cancer Trialists' Collaborative Group. Maximum androgen blockade in advanced prostate cancer: an overview of the randomised trials. Lancet 2000; 355: 1491–1498.
Schellhammer PF, Sharifi R, Block NL, Soloway MS, Venner PM, Patterson AL et al. Clinical benefits of bicalutamide compared with flutamide in combined androgen blockade for patients with advanced prostatic carcinoma: final report of a double-blind, randomized, multicenter trial. Casodex Combination Study Group. Urology 1997; 50: 330–336.
Akaza H, Homma Y, Okada K, Yokoyama M, Usami M, Hirao Y et al. A prospective and randomized study of primary hormonal therapy for patients with localized or locally advanced prostate cancer unsuitable for radical prostatectomy: results of the 5-year follow-up. BJU Int 2003; 91: 33–36.
Kotake T, Usami M, Akaza H, Koiso K, Homma Y, Kawabe K et al. Goserelin acetate with or without antiandrogen or estrogen in the treatment of patients with advanced prostate cancer: a multicenter, randomized, controlled trial in Japan. Zoladex Study Group. Jpn J Clin Oncol 1999; 29: 562–570.
Kanetake H, Akaza H, Usami M . A phase III randomized trial of low dose flutamide compared with luteinizing hormone releasing agonist (LHRHa) vs LHRHa monotherapy for advanced prostate cancer. Japan Flutamide Study Cooperative Group. BJU Int 2004; 94: 58–59 (abstract).
Akaza H, Yamaguchi A, Matsuda T, Igawa M, Kumon H, Soeda A et al. Superior anti-tumor efficacy of bicalutamide 80 mg in combination with a luteinizing hormone-releasing hormone (LHRH) agonist versus LHRH agonist monotherapy as first-line treatment for advanced prostate cancer: interim results of a randomized study in Japanese patients. Jpn J Clin Oncol 2004; 34: 20–28.
Kotake T, Akaza H, Usami M, Isaka S, Homma Y, Oishi K et al. Preliminary trial for clinical phase III study of Casodex (Bicalutamide ICI 176,334). J New Remedies Clinics 1999; 48: 1512–1533.
Kotake T, Usami M, Isaka S, Shimazaki J, Oishi K, Yoshida O et al. Phase I study of bicalutamide (Casodex), a nonsteroidal antiandrogen in patients with prostatic cancer. Hinyokika Kiyo 1996; 42: 143–153.
Kotake T, Usami M, Isaka S, Shimazaki J, Nakano E, Okuyama A et al. Clinical early phase II study of bicalutamide (Casodex) in patients with prostatic cancer. Hinyokika Kiyo 1996; 42: 157–168.
Japanese Urological Association and The Japanese Pathological Society. General Rule for Clinical and Pathological Studies on Prostate Cancer. Kanehara: Tokyo, Japan, 1992, pp 100–106.
Small EJ, Carroll PR . Prostate-specific antigen decline after casodex withdrawal: evidence for an antiandrogen withdrawal syndrome. Urology 1994; 43: 408–410.
Nieh PT . Withdrawal phenomenon with the antiandrogen casodex. J Urol 1995; 153: 1070–1073.
Schellhammer PF, Venner P, Haas GP, Small EJ, Nieh PT, Seabaugh DR et al. Prostate specific antigen decreases after withdrawal of antiandrogen therapy with bicalutamide or flutamide in patients receiving combined androgen blockade. J Urol 1997; 157: 1731–1735.
Aus G, Abbou CC, Bolla M, Heidenreich A, Schmid HP, van Poppel H et al. European Association of Urology Guidelines on Prostate Cancer 2005, (online). http://www.uroweb.nl/files/uploaded_files/2005ProstateCancer.pdf.
Kojima S, Suzuki H, Akakura K, Shimbo M, Ichikawa T, Ito H . Alternative antiandrogens to treat prostate cancer relapse after initial hormone therapy. J Urol 2004; 171: 679–683.
Kaisary AV . Compliance with hormonal treatment for prostate cancer. Br J Hosp Med 1996; 55: 359–366.
Fourcade R-O, McLeod D . Tolerability of antiandrogens in the treatment of prostate cancer. Uro Oncol 2004; 4: 5–13.
Acknowledgements
Financial sponsorship for this trial was provided by AstraZeneca.
We thank Dr Chris Rapier, PhD, from Complete Medical Group, who provided editing assistance on behalf of AstraZeneca. We also thank Dr Toshihiko Kotake for valuable medical advice and the study institutions for data collection.
Study institutions, listed in descending order of the number of patients that they enlisted*, were:
Harasanshin Hospital (22); Kansai Medical University Hospital (nine); Shimane University Hospital (eight); Nishi-Kobe Medical Center (seven); Okayama University Hospital (seven); Fujieda Municipal General Hospital (six); Kurashiki Central Hospital (six); Nihon University Itabashi Hospital (six); Shikoku Cancer Center (six); Showa University Hospital (six); Tokushima University Hospital (six); Gifu University Hospital (five); Kanazawa University Hospital (five); Kobe University Hospital (five); Kyushu University Hospital (five); Nagasaki Medical Center (five); Nara University of Medical Science Hospital (five); Tokyo Medical University Hospital (five); Hirosaki University School of Medicine and Hospital (four); Hiroshima University Hospital (four); Kawasaki Medical School Hospital (four); Keio University Hospital (four); Kyoto University Hospital (four); Nagasaki University Hospital (four); Osaka University Hospital (four); Sasebo Municipal General Hospital (four); Tokyo Women's Medical University Hospital (four); Kitasato University Hospital (three); Osaka City University Hospital (three); The University of Tokyo Hospital (three); Teikyo University Ichihara Hospital (three); University Hospital, Kyoto Prefectural University of Medicine (three); Yamagata University Hospital (three); Asahi Central Hospital (two); Jikei University School of Medicine Hospital (two); Kochi Medical School Hospital (two); Nagoya City University Hospital (two); Nagoya Daini Red Cross Hospital (two); Niigata Cancer Center Hospital (two); Niigata University Medical and Dental Hospital (two); Sapporo Medical University Hospital (two); Tohoku University Hospital (two); Tsukuba University Hospital (two); Yokohama City University Hospital (two); Chiba University Hospital (one); Hokkaido University Hospital (one); Osaka Medical Center for Cancer and Cardiovascular Diseases (one); Toranomon Hospital (one); Tottori University Hospital (one).
*Values in parentheses represent the number of enrolled patients.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Usami, M., Akaza, H., Arai, Y. et al. Bicalutamide 80 mg combined with a luteinizing hormone-releasing hormone agonist (LHRH-A) versus LHRH-A monotherapy in advanced prostate cancer: findings from a phase III randomized, double-blind, multicenter trial in Japanese patients. Prostate Cancer Prostatic Dis 10, 194–201 (2007). https://doi.org/10.1038/sj.pcan.4500934
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.pcan.4500934
Keywords
This article is cited by
-
A phase III multicenter, randomized, controlled study of combined androgen blockade with versus without zoledronic acid in prostate cancer patients with metastatic bone disease: results of the ZAPCA trial
International Journal of Clinical Oncology (2017)
-
Clinical outcomes and nadir prostate-specific antigen (PSA) according to initial PSA levels in primary androgen deprivation therapy for metastatic prostate cancer
World Journal of Urology (2016)
-
Drug costs in the management of metastatic castration-resistant prostate cancer in Canada
BMC Health Services Research (2014)
-
Differences in maximum tolerated doses and approval doses of molecularly targeted oncology drug between Japan and Western countries
Investigational New Drugs (2014)
-
Impact of pretreatment factors, biopsy Gleason grade volume indices and post-treatment nadir PSA on overall survival in patients with metastatic prostate cancer treated with step-up hormonal therapy
Prostate Cancer and Prostatic Diseases (2012)