Abstract
The development of papillary thyroid carcinoma is influenced by many factors including genetic alterations, growth factors, and physical agents such as radiation. Arachidonic acid and its derivatives including prostaglandins (PG) and thromboxane along with the enzymes involved in their synthesis have been shown to influence the growth of various tumors. We analyzed the immunoreactivity for cyclooxygenase-2 (COX-2) and mRNA expression levels of the enzymes COX-2, thromboxane A2 (TXA2) synthase, and PGI2 synthase by RT-PCR in papillary carcinomas and matching normal tissues to determine the role of these enzymes in the development of papillary thyroid carcinomas. A papillary thyroid carcinoma cell line TPC-1 was also studied in vitro to determine the role of the specific COX-2 inhibitor NS-398 on COX-2 and vascular endothelial growth factor-A, since COX-2 also has a role in regulating tumor angiogenesis. RT-PCR analysis showed significant increases in TXA2 synthase mRNA levels in papillary thyroid carcinomas compared to normal thyroid tissues. Although COX-2 mRNA levels were generally increased in papillary carcinomas, the differences were not statistically significant. There were no significant differences in PGI2 synthase mRNA levels. COX-2 protein expression was greater in papillary carcinoma compared to normal thyroid tissues; however, the levels were quite variable. In vitro studies with a COX-2 inhibitor, NS-398, showed inhibition of tumor growth along with increased levels of COX-2 and vascular endothelial growth factor-A mRNA expression. These results indicate that specific enzyme levels in the PG synthesis pathway such as TXA2 synthase are increased in papillary thyroid carcinomas. COX-2 also has a role in papillary thyroid growth, since a specific inhibitor of COX-2 regulates papillary thyroid carcinoma cell proliferation. These results implicate several enzymes in the synthesis of prostanoids as regulators of thyroid papillary carcinoma proliferation and suggest that increased levels of expression of these enzymes may play a role in the pathogenesis of these tumors.
Similar content being viewed by others
Main
Arachidonic acid and its derivatives, the prostaglandins and thromboxane (Figure 1), are important in many physiological processes.1 They are also mediators of tumor progression. There are two major cyclooxygenases (COX). COX-1 is the constitutive form of the enzyme, which catalyzes formation of prostaglandin from arachidonic acid, while COX-2 is expressed as an inducible isoform. COX-2 expression is increased by various substances including mitogens,2 tumor promoters,3, 4 cytokines,1, 2, 5, 6 serum,5 and free fatty acids.7 Other studies have shown that COX-2 is also regulated by nonsteroidal anti-inflammatory drugs (NSAIDs) or by selective COX-2 inhibitors.7, 8, 9, 10
COX-2 is expressed in many types of cancers including colon,11, 12 pancreas,8, 13, 14 stomach,15, 16, 17 lung,12, 18 breast,12, 19 prostate,20 cervix,6 head and neck,21 esophagus,22 bladder,23 glioma,24 and melanomas.25 Recent studies have shown that COX-2 is expressed in thyroid lesions.26, 27, 28, 29 Thyroid tumors generally express higher levels of COX-2 than normal tissues and thyroid tissues from patients with thyroiditis.26, 27, 28, 29
Thromboxane A2 (TXA2) synthase and prostaglandin (PG) I2 synthase are enzymes located downstream from COX-1 and COX-2, and catalyze synthesis of PG H, TXA2 and PGI2 (Figure 1). TXA2 stimulates platelet aggregation, while PGI2 inhibits aggregation of platelets. Some studies have suggested that TXA2 synthase and PGI2 synthase contribute to tumor metastasis.30, 31, 32 TXA2 synthase was shown to stimulate tumor angiogenesis, while PGI2 synthase inhibited angiogenesis.33, 34, 35 Our recent studies on COX-2 and TXA2 synthase expression in thyroid tumors and other thyroid lesions using immunohistochemistry found higher levels of these proteins in papillary thyroid carcinomas compared to adenomatous nodules and benign thyroid tumors.36 The present study examines COX-2, TXA2 synthase, and PGI2 synthase mRNA expression in normal thyroid tissue and papillary thyroid carcinomas using semiquantitative RT-PCR to analyze the role of these enzymes in thyroid tumor growth. We also examined the selective inhibition of COX-2 by NS-398 in the papillary thyroid carcinoma cell line TPC-1 to study the effects of this inhibitor on cell growth as well as COX-2 and VEGF-A mRNA expression.
Materials and methods
Tissue Samples
In all, 15 cases of papillary thyroid carcinomas and adjacent normal tissues were obtained at the time of surgery and stored at −70°C. Hematoxylin and eosin staining was performed for each case to determine the diagnosis and distribution of tumor and normal thyroid cells. There were 12 cases of classic variant and three cases of follicular variant of papillary carcinomas.
Immunostaining for COX-2 with a monoclonal antibody from Cayman Chemicals, Ann Arbor, MI at a 1/200 dilution was carried out using frozen tissues fixed in formalin.36
RNA Extraction and RT-PCR
Total RNA was extracted from frozen normal and tumor tissue samples and from cultured cells using the TRIzol reagent as previously reported.37 A measure of 1 μg total RNA was converted to cDNA using the Prostar First Strand RT-PCR Kit (Stratagene, La Jolla, CA, USA) according to the manufacturer's instruction. A measure of 5 μl cDNA was amplified by hot-start PCR in a GeneAmp PCR system 9700 (Applied Biosystems, Foster City, CA, USA). Five specific primer sets with individual annealing temperatures were used (Table 1). Each PCR reaction was performed using 1 × PCR buffer, 2 mM MgCl2, 1.25 U Taq polymerase (Promega, Madision, WI, USA), 0.2 μM each dNTP (Roche Diagnostics, Alameda, CA, USA) in a final volume of 50 μl. PCR product identity was verified by automated sequencing using the 3730XL DNA Analyzer (Applied Biosystems, Foster City, CA, USA). In all, 20 μl of each PCR reaction as analyzed on a 1.5% agarose gel, stained briefly in ethidium bromide, and viewed under UV light.
Densitometric Analysis
Densitometric analysis was carried out with a Quantity One System (Bio-Rad Laboratories, Hercules, CA, USA). Relative densities of the samples were calculated and compared with the housekeeping gene HPRT expression level. Samples were normalized and expressed relative to HPRT.
Cell Culture
A human papillary thyroid carcinoma cell line, TPC1, was obtained from Dr Yuri Nikiforov (University of Cincinnati Medical Center). The cell line has a rearranged form of RET/PTC1.43 Cells were cultured in DMEM, supplemented with 10% FBS, 1 μg/ml insulin, 100 U/ml penicillin, 100 μg/ml streptomycin, and 0.25 μg/ml fungizone (InVitrogen Life Technologies, Carlsbad, CA, USA) using cell culture conditions as previously reported.44
Cell Treatments and Reagents
A stock solution of 40 mM NS398 (Cayman Chemical Company, Ann Arbor, MI, USA) was dissolved in dimethyl sulfoxide (DMSO) (Sigma) and diluted in standard growth medium to a final concentration of 20–80 μM for the cell growth experiments. COX-2 expression experiments were performed with NS-398, which was diluted in serum-free medium and treated with 80 μM NS-398. The final concentration of DMSO was 0.2% in each experiment. The experiments were performed at least three times.
Growth Inhibition Experiments
Cells were seeded at a density of 0.2 × 106 per six-well plates. They were allowed to grow for 24 h, and then the medium was replaced with NS-398 and/or DMSO-containing control medium. Cells were counted with a hemocytometer after 72 h of NS-398 treatment.
COX-2 Induction Experiments
Cells were seeded at a density of 0.5 × 106 cells in a 75 cm2 flask. After 72 h, the cells were treated with 80 μM NS-398 or DMSO in serum-free medium. At 24 h before treatment, the medium was replaced with serum-free media. Total RNA was extracted after 8, 24, and 32 h. The samples were subsequently analyzed by RT-PCR.
Statistical Analysis
Comparison between tumor and normal tissue were calculated using the Student's t-tests and by the Wilcoxon signed rank-sum test. NS-398 cell growth inhibition was analyzed by dose-response regression analysis. A P-value less than 0.05 was considered to be statistically significant.
Results
Immunohistochemistry
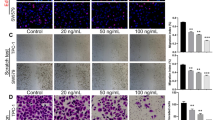
Immunoreactivity for COX-2 was stronger in the papillary carcinomas compared to the normal thyroid tissues (Table 2). However, immunostaining was variable among the tumors.
Expression of COX-2, TXA2 Synthase, and PGI-2 Synthase mRNA
Analysis of COX-2 mRNA by RT-PCR in 15 cases of papillary thyroid carcinoma (Table 2) (Figure 2) showed that COX-2 expression was upregulated more than 1.8-fold in four cases (Figures 3 and 4a). In four cases, the tumors were downregulated to less than 50% of normal tissues. The expression levels of TXA2 synthase showed upregulation more than 1.8-fold in eight cases (Figures 3 and 4b). There were significant differences of TXA2 synthase expression between carcinomas and normal tissues (P=0.008). The expression of PGI2 synthase was quite variable, and there were no significant differences between tumor and normal tissues (Figures 3 and 4c).
Densitometric analysis of mRNA for the three enzymes analyzed in the study. (a) COX-2 analysis in the 15 cases comparing normal and papillary carcinoma for each case. (b) Thromboxane synthase (TXA2 synthase) analysis of normal and papillary carcinoma. (c) PGI2 synthase analysis of normal and papillary carcinoma.
In Vitro Studies of the COX-2 Inhibitor NS-398
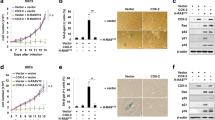
The effects of the specific COX-2 inhibitor NS-398 were examined in the TPC-1 cell line. A titration experiment with varying concentrations of NS-398 showed inhibition of cell growth which was statistically significant in a dose-dependent manner (R2=0.590, P=0.0035), and the maximum inhibition was at 80 μM of NS-398 (Figure 5).
When the TPC-1 cells were treated with NS-398 for varying periods under serum-free conditions, preliminary experiments showed no change over control after 1 and 2 h of treatment (data not shown). Treatment of cells with NS-398 for 8 and 24 h produced a significant increase in COX-2 and VEGF-A mRNAs (P=0.0025 and 0.00189) (Figure 6a–c). After 32 h of treatment, there were no significant differences in the treated cells for COX-2 or VEGF mRNA levels (Figures 6a–c).
(a) RT-PCR analysis of COX-2 and VEGF-A levels after 8, 24, and 32 h of treatment with 80 μM NS-398 on PTG-1 cells. (b) Densitometric analysis of COX-2 mRNA levels after 8, 24, and 32 h of treatment with NS-398. There was a significant increase in COX-2 mRNA levels after 8 and 24 h of treatment. (c) Densitometric analysis of VEGF-A mRNA levels after 8, 24, and 32 h of treatment with NS-398. There was a significant increase in VEGF-A mRNA after 8 and 24 h of treatment.
Discussion
COX are enzymes which convert arachidonic acid to PG-H. COX-2 has been reported to be upregulated in various cancers including thyroid tumors.6, 8, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29 COX-2 is also induced in inflammatory conditions such as thyroiditis. COX-2 expression was also higher in the carcinomas compared to the normal thyroid tissue. However, as we recently reported,36 there was variable expression in both normal thyroid tumors. Although COX-2 mRNA was elevated above levels in normal thyroids in several papillary carcinomas, our results did not show significant differences in COX-2 mRNA expression between normal thyroid and papillary carcinoma, because of the variation in mRNA levels. Other studies have also found variable levels of COX-2 proteins in papillary thyroid carcinomas.29, 36 Ito et al29 found nine COX-2-negative cases (18.4%) among the 49 papillary carcinoma cases studied by immunohistochemistry. They showed that COX-2 levels varied with certain conditions and were significantly reduced in older patients, in patients with large tumors, and with advanced disease stages.29 Three of the patients in our series were over 54 years of age (the cutoff age used by Ito et al.30 Five cases had tumors larger than 4 cm which could contribute to the reduced expression levels of COX-2 in our study. Five patients had tumors showing extrathyroidal invasion. Seven cases had lymph node metastases. However, the influence of age on COX-2 expression remains controversial since another recent study found that COX-2 expression was increased with age in papillary thyroid carcinoma.45
Our studies found significant upregulation of TXA2 synthase in papillary thyroid carcinomas which implicate TXA2 synthase in the pathogenesis of papillary thyroid carcinoma. Pradono et al,34 recently showed that TXA2 synthase and PGI2 synthase-transfected cancer cells had opposite stimulatory and inhibitory effects on their growth in vivo, and these effects were related to vascular density. PGI2 synthase was not significantly different in normal thyroid or tumors in our study. TXA2 has been associated with tumor proliferation and metastasis and is considered to be proangiogenic while PGI2 is considered to be an anticancer prostanoid.34 The number of cases of the nonclassical (follicular) variant of papillary carcinoma was too small (n=3) to observe a relationship between tumor subtype and COX-2 or TXA2 expression.
To examine directly the role of COX-2 on growth regulation of thyroid tumors, we performed in vitro studies with the TPC-1 thyroid papillary carcinoma cell line. Studies with NS-398, a COX-2 specific inhibitor of COX-2 enzymatic activity, inhibited growth of these tumor cells. Interestingly, with the inhibition of COX-2 enzymatic activity, there was an increase in COX-2 mRNA levels. These results indicate that COX-2 has a role in the growth of thyroid papillary cell lines. Previous studies have shown that NSAIDs and COX-2 inhibitors have growth inhibitory effects on various tumors including the colon, pancreas,8, 37 stomach,38 esophagus,22 liver,46 lung, and prostate,48 carcinoma cell lines. NS-398 has been shown to inhibit cell growth, and induce apoptosis via activating caspase-3 in vitro.47 This is the first report of the growth inhibitory effect of NS-398 on thyroid tumor cells with selective inhibition of COX-2. One earlier study examined NS-398 effects on COX-2 expression in a human thyroid epithelial cell line and found that NS-398 inhibited COX enzyme activity by proinflammatory cytokines.49
The TPC-1 cell line expressed COX-2, PGI2 synthase, and VEGF. TPC-1 had very low expression levels of TXA2 synthase. NS-398 upregulated COX-2 expression in TPC-1 cells. Our results are similar to those for other tumors such as colon,10 pancreas,8 and gliomas.9 A previous study showed that in transfected colon carcinoma cells, COX-2 upregulated VEGF expression. This expression could be downregulated by NS-398.50 Related drugs such as NSAIDs had similar effects in prostate,48 transitional cell carcinoma51 and pancreatic cells.52 In our study, VEGF expression level was noticeably affected by NS-398 treatment. This would agree with previous studies, since we also observed an increase in COX-2 mRNA levels after NS-398 treatment. The importance of VEGF in thyroid tumor growth has been well documented.53, 54, 55
In summary, analysis of papillary thyroid carcinomas and normal thyroid tissue mRNAs by RT-PCR showed significantly increased expression of TXA2 synthase in the tumors. Although there was an increase in COX-2 mRNA levels in some cases, the differences were not statistically significant. However, our in vitro studies showed that the COX-2-specific inhibitor NS-398 increased COX-2 messenger RNA expression, while inhibiting tumor growth implicating a role of COX-2 as well as TXA2 synthase in papillary thyroid carcinoma proliferation.
References
Smith WL, DeWitt DL, Garavito RM . Cyclooxygenases: structural, cellular, and molecular biology. Annu Rev Biochem 2000;69:145–182.
Hamasaki Y, Kitzler J, Hardman R, et al. Phorbol ester and epidermal growth factor enhance the expression of two inducible prostaglandin H synthase genes in rat tracheal epithelial cells. Arch Biochem Biophys 1993;304:226–234.
Xie W, Herschman HR . v-src induces prostaglandin synthase 2 gene expression by activation of the c-Jun N-terminal kinase and the c-Jun transcription factor. J Biol Chem 1995;270:27622–27628.
Sheng H, Shao J, Dixon DA, et al. Transforming growth factor-beta1 enhances Ha-ras-induced expression of cyclooxygenase-2 in intestinal epithelial cells via stabilization of mRNA. J Biol Chem 2000;275:6628–6635.
Xie W, Herschman HR . Transcriptional regulation of prostaglandin synthase 2 gene expression by platelet-derived growth factor and serum. J Biol Chem 1996;271:31742–31748.
Kulkarni S, Rader JS, Zhang F, et al. Cyclooxygenase-2 is overexpressed in human cervical cancer. Clin Cancer Res 2001;7:429–434.
Meade EA, McIntyre TM, Zimmerman GA, et al. Peroxisome proliferators enhance cyclooxygenase-2 expression in epithelial cells. J Biol Chem 1999;274:8328–8334.
Molina MA, Sitja-Arnau M, Lemoine MG, et al. Increased cyclooxygenase-2 expression in human pancreatic carcinomas and cell lines: growth inhibition by nonsteroidal anti-inflammatory drugs. Cancer Res 1999;59:4356–4362.
Moalic S, Liagre B, Le Bail JC, et al. Dose-dependent modulation of apoptosis and cyclooxygenase-2 expression in human 1547 osteosarcoma cells by NS-398, a selective cyclooxygenase-2 inhibitor. Int J Oncol 2001;18:533–540.
Elder DJ, Halton DE, Crew TE, et al. Apoptosis induction and cyclooxygenase-2 regulation in human colorectal adenoma and carcinoma cell lines by the cyclooxygenase-2-selective non-steroidal anti-inflammatory drug NS-398. Int J Cancer 2000;86:553–560.
Sano H, Kawahito Y, Wilder RL, et al. Expression of cyclooxygenase-1 and -2 in human colorectal cancer. Cancer Res 1995;55:3785–3789.
Soslow RA, Dannenberg AJ, Rush D, et al. COX-2 is expressed in human pulmonary, colonic, and mammary tumors. Cancer 2000;89:2637–2645.
Tucker ON, Dannenberg AJ, Yang EK, et al. Cyclooxygenase-2 expression is up-regulated in human pancreatic cancer. Cancer Res 1999;59:987–990.
Okami J, Yamamoto H, Fujiwara Y, et al. Overexpression of cyclooxygenase-2 in carcinoma of the pancreas. Clin Cancer Res 1999;5:2018–2024.
Murata H, Kawano S, Tsuji S, et al. Cyclooxygenase-2 overexpression enhances lymphatic invasion and metastasis in human gastric carcinoma. Am J Gastroenterol 1999;94:451–455.
Lim HY, Joo HJ, Choi JH, et al. Increased expression of cyclooxygenase-2 protein in human gastric carcinoma. Clin Cancer Res 2000;6:519–525.
Uefuji K, Ichikura T, Mochizuki H . Cyclooxygenase-2 expression is related to prostaglandin biosynthesis and angiogenesis in human gastric cancer. Clin Cancer Res 2000;6:135–138.
Achiwa H, Yatabe Y, Hida T, et al. Prognostic significance of elevated cyclooxygenase 2 expression in primary, resected lung adenocarcinomas. Clin Cancer Res 1999;5:1001–1005.
Half E, Tang XM, Gwyn K, et al. Cyclooxygenase-2 expression in human breast cancers and adjacent ductal carcinoma in situ. Cancer Res 2002;62:1676–1681.
Yoshimura R, Sano H, Masuda C, et al. Expression of cyclooxygenase-2 in prostate carcinoma. Cancer 2000;89:589–596.
Chan G, Boyle JO, Yang EK, et al. Cyclooxygenase-2 expression is up-regulated in squamous cell carcinoma of the head and neck. Cancer Res 1999;59:991–994.
Zimmermann KC, Sarbia M, Weber AA, et al. Cyclooxygenase-2 expression in human esophageal carcinoma. Cancer Res 1999;59:198–204.
Mohammed SI, Knapp DW, Bostwick DG, et al. Expression of cyclooxygenase-2 (COX-2) in human invasive transitional cell carcinoma (TCC) of the urinary bladder. Cancer Res 1999;59:5647–5650.
Joki T, Heese O, Nikas DC, et al. Expression of cyclooxygenase 2 (COX-2) in human glioma and in vitro inhibition by a specific COX-2 inhibitor, NS-398. Cancer Res 2000;60:4926–4931.
Denkert C, Kobel M, Berger S, et al. Expression of cyclooxygenase 2 in human malignant melanoma. Cancer Res 2001;61:303–308.
Specht MC, Tucker ON, Hocever M, et al. Cyclooxygenase-2 expression in thyroid nodules. J Clin Endocrinol Metab 2002;87:358–363.
Nose F, Ichikawa T, Fujiwara M, et al. Up-regulation of cyclooxygenase-2 expression in lymphocytic thyroiditis and thyroid tumors: significant correlation with inducible nitric oxide synthase. Am J Clin Pathol 2002;117:546–551.
Cornetta AJ, Russell JP, Cunnane M, et al. Cyclooxygenase-2 expression in human thyroid carcinoma and Hashimoto's thyroiditis. Laryngoscope 2002;112:238–242.
Ito Y, Yoshida H, Nakano K, et al. Cyclooxygenase-2 expression in thyroid neoplasms. Histopathology 2003;42:492–497.
Honn KV, Cicone B, Skoff A . Prostacyclin: a potent antimetastatic agent. Science 1981;212:1270–1272.
Honn KV, Meyer J . Thromboxanes and prostacyclin: positive and negative modulators of tumor growth. Biochem Biophys Res Commun 1981;102:1122–1129.
Nie D, Lamberti M, Zacharek A, et al. Thromboxane A(2) regulation of endothelial cell migration, angiogenesis, and tumor metastasis. Biochem Biophys Res Commun 2000;267:245–251.
Daniel TO, Liu H, Morrow JD, et al. Thromboxane A2 is a mediator of cyclooxygenase-2-dependent endothelial migration and angiogenesis. Cancer Res 1999;59:4574–4577.
Pradono P, Tazawa R, Maemondo M, et al. Gene transfer of thromboxane A(2) synthase and prostaglandin I(2) synthase antithetically altered tumor angiogenesis and tumor growth. Cancer Res 2002;62:63–66.
Ermert L, Dierkes C, Ermert M . Immunohistochemical expression of cyclooxygenase isoenzymes and downstream enzymes in human lung tumors. Clin Cancer Res 2003;9:1604–1610.
Casey MB, Zhang S, Jin L, et al. Expression of cyclooxygenase-2 and thromboxane synthase in non-neoplastic and neoplastic thyroid lesions. Endocrinol Pathol 2004;15:107–116.
Jin L, Kulig E, Qian X, et al. A human pituitary adenoma cell line proliferates and maintains some differentiated functions following expression of SV40 large T antigen. Endocrinol Pathol 1998;9:169–184.
Jin L, Qian X, Kulig E, et al. Transforming growth factor-beta, transforming growth factor-beta receptor II, and p27Kip1 expression in nontumorous and neoplastic human pituitaries. Am J Pathol 1997;151:509–519.
Hla T, Neilson K . Human cyclooxygenase-2 cDNA. Proc Natl Acad Sci USA 1992;89:7384–7388.
Ohashi K, Ruan KH, Kulmacz RJ, et al. Primary structure of human thromboxane synthase determined from the cDNA sequence. J Biol Chem 1992;267:789–793.
Miyata A, Hara S, Yokoyama C, et al. Molecular cloning and expression of human prostacyclin synthase. Biochem Biophys Res Commun 1994;200:1728–1734.
Leung DW, Cachianes G, Kuang WJ, et al. Vascular endothelial growth factor is a secreted angiogenic mitogen. Science 1989;246:1306–1309.
Ishizaka Y, Ushijima T, Sugimura T, et al. cDNA cloning and characterization of ret activated in a human papillary thyroid carcinoma cell line. Biochem Biophys Res Commun 1990;168:402–408.
Riss D, Jin L, Qian X, et al. Differential expression of galectin-3 in pituitary tumors. Cancer Res 2003;63:2251–2255.
Siironen P, Ristimaki A, Nordling S, et al. Expression of COX-2 is increased with age in papillary thyroid cancer. Histopathology 2004;44:490–497.
Cheng J, Imanishi H, Amuro Y, et al. NS-398, a selective cyclooxygenase 2 inhibitor, inhibited cell growth and induced cell cycle arrest in human hepatocellular carcinoma cell lines. Int J Cancer 2002;99:755–761.
Chang HC, Weng CF . Cyclooxygenase-2 level and culture conditions influence NS398-induced apoptosis and caspase activation in lung cancer cells. Oncol Rep 2001;8:1321–1325.
Liu XH, Kirschenbaum A, Yao S, et al. Inhibition of cyclooxygenase-2 suppresses angiogenesis and the growth of prostate cancer in vivo. J Urol 2000;164:820–825.
Yu HP, Shi LY, Lu WH, et al. Expression of cyclooxygenase-2 (COX-2) in human esophageal cancer and in vitro inhibition by a specific COX-2 inhibitor, NS-398. J Gastroenterol Hepatol 2004;19:638–642.
Berg J, Stocher M, Bogner S, et al. Inducible cyclooxygenase-2 gene expression in the human thyroid epithelial cell line Nthy-ori3-1. Inflamm Res 2000;49:139–143.
Tsujii M, Kawano S, Tsuji S, et al. Cyclooxygenase regulates angiogenesis induced by colon cancer cells. Cell 1998;93:705–716.
Li G, Yang T, Yan J . Cyclooxygenase-2 increased the angiogenic and metastatic potential of tumor cells. Biochem Biophys Res Commun 2002;299:886–890.
Eibl G, Bruemmer D, Okada Y, et al. PGE(2) is generated by specific COX-2 activity and increases VEGF production in COX-2-expressing human pancreatic cancer cells. Biochem Biophys Res Commun 2003;306:887–897.
Huang SM, Lee JC, Wu TJ, et al. Clinical relevance of vascular endothelial growth factor for thyroid neoplasms. World J Surg 2001;25:302–306.
Tuttle RM, Fleisher M, Francis GL, et al. Serum vascular endothelial growth factor levels are elevated in metastatic differentiated thyroid cancer but not increased by short-term TSH stimulation. J Clin Endocrinol Metab 2002;87:1737–1742.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kajita, S., Ruebel, K., Casey, M. et al. Role of COX-2, thromboxane A2 synthase, and prostaglandin I2 synthase in papillary thyroid carcinoma growth. Mod Pathol 18, 221–227 (2005). https://doi.org/10.1038/modpathol.3800285
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.3800285
Keywords
This article is cited by
-
Senescent thyrocytes and thyroid tumor cells induce M2-like macrophage polarization of human monocytes via a PGE2-dependent mechanism
Journal of Experimental & Clinical Cancer Research (2019)
-
Gamabufotalin, a bufadienolide compound from toad venom, suppresses COX-2 expression through targeting IKKβ/NF-κB signaling pathway in lung cancer cells
Molecular Cancer (2014)
-
Up-regulation of Kv7.1 channels in thromboxane A2-induced colonic cancer cell proliferation
Pflügers Archiv - European Journal of Physiology (2014)
-
Examination of thromboxane synthase as a prognostic factor and therapeutic target in non-small cell lung cancer
Molecular Cancer (2011)
-
COX-2 expression in papillary thyroid carcinoma (PTC) in cytological material obtained by fine needle aspiration biopsy (FNAB)
Thyroid Research (2011)