Abstract
Adult T-cell leukemia/lymphoma (ATL) is an aggressive T-cell neoplasm. The health of ATL patients rapidly deteriorates resulting in death; however, the induction of death in a small animal model due to tumor has not yet been reported. SCID mice, 5 weeks old, younger than those previously used, which were inoculated with ATL cells, eliminated NK cell activity and showed rapid tumor formation resulting in death. Age is the crucial factor influencing tumor formation and death in the SCID mice model for cancer.
Similar content being viewed by others
Main
Human T-cell leukemia virus type I (HTLV-I), the first human retrovirus isolated, is the causative agent of adult T-cell leukemia/lymphoma (ATL).1, 2 ATL is a rapidly aggressive, lethal disease and no effective treatment yet exists. It has recently been reported that the nuclear transcription factor, NF-κB, plays a central role in oncogenesis induced by HTLV-I.3 Therefore, NF-κB inhibitors are potential candidates for the treatment of HTLV-I infections. However, an appropriate animal model is required to evaluate the inhibitory effects of any novel NF-κB activation inhibitor on the progression of ATL. ATL cells do not form tumors in nude mice, which are widely used in cancer research. The severe combined immunodeficiency (SCID) mice, lacking functional T and B cells, were engrafted successfully with leukemic cell lines from ATL patients or HTLV-I in vitro-transformed cells.4, 5, 6 However, a long period of time is required for tumor formation using this system, and, in addition, well-characterized HTLV-I-transformed cell lines did not engraft when injected via the peritoneal route.7, 8 Furthermore, ATL patients progress to death rapidly, however, the induction of tumor death in SCID mice injected with ATL cells or HTLV-I-transformed cell lines has not yet been reported. Here, we established a small animal model appropriate for the assay of therapeutic agents for the treatment of ATL, in which rapid tumor formation and death is successfully induced by using younger mice than in previous studies.
Materials and methods
Male C. B-17 scid/scid (SCID) mice, 4 weeks of age, were obtained from Charles River Japan, Inc. (Tokyo, Japan). The mice were maintained in laminar-flow benches with controlled temperature (22±2°C), and lighting (12 h light/dark cycles) under specific pathogen-free conditions. They were fed with mouse pellets that were sterilized by γ-irradiation and received hyperchlorinated water ad libitum. After 1 week of preliminary care, mice at 5, 7, 9 and 11 weeks of age were used, and treated intraperitoneally with 1 mg of anti-murine interleukin-2 receptor (IL2R) β chain antibody9 in phosphate-buffered saline (PBS) to reduce NK cell activity, starting at 3 days before the MT-2 cell injection. Then, the mice were injected intraperitoneally with 5 × 107 cells of the HTLV-I-transformed human T-cell line, MT-2.
The mice injected with MT-2 cells were anesthetized with ether and killed after 40 days, and their blood was obtained by heart puncture. Peripheral blood mononuclear cells (PBMC) were separated using the Ficoll–Paque (Pharmacia, Uppsala, Sweden) gradient. High molecular weight cellular DNA was extracted from PBMC, gross tumor, lung, liver, spleen, mesenteric lymph nodes (MLN) and kidney by standard procedures. To assess the growth of the inoculated cells in the mice, 0.5 μg of the DNA from various organs was subjected to polymerase chain reaction (PCR) using the primers for the HTLV-I Tax and human β-globin genes.10, 11 The organs of the mice died within 40 days after the MT-2 cell injection were also examined for the presence of both genes by PCR.
For histological examination, the tumors were fixed in 10% formalin. Paraffin sections were cut and stained with hematoxylin and eosin (HE). Immunofluorescence assays were also performed on the paraffin sections. These sections were incubated with anti-HTLV-I p19 monoclonal antibody (Chemicon International, Inc., CA, USA), or with anti-HLA-DR monoclonal antibody (INCSTAR Co., MN, USA), followed by staining with FITC-conjugated anti-mouse IgG (Cappel, NC, USA).
Results
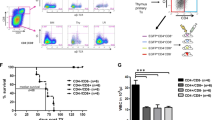
Of 10 mice, eight (80%), inoculated with MT-2 cells at 5 weeks of age, died within 30 days after inoculation (Figure 1a). Of 10 mice, two (20%), inoculated with the cells at 7 weeks of age, died, whereas no mice injected with the cells at 9 and 11 weeks of age died. No control mice of any age, inoculated with culture medium, died. The formation of gross tumors in peritoneal cavities or in other organs was observed in all mice inoculated with the cells at 5 weeks of age, in five of 10 (50%) mice inoculated with the cells at 7 weeks of age, in two of 10 (20%) mice inoculated with the cells at 9 weeks of age, and in none of the mice inoculated with the cells at 11 weeks of age (Figure 1b). To confirm that these tumors were derived from the inoculated cells, PCR was performed to detect the HTLV-I Tax and human β-globin genes. All of the tumors forming in the mice were positive for both genes. Histological examination of HE-stained sections revealed that the tumor mass consisted of fibrosis tissues and a diffuse distribution of lymphoid cells of various sizes was observed. These findings were similar to those reported previously.4, 11 All tumors reacted with anti-HTLV-I p19 and anti-HLA-DR monoclonal antibodies in the immunofluorescence assays. No gross tumors in control mice of any age were observed.
Survival curves (a) and the incidence of gross tumor formation (b) in SCID mice injected with MT-2 cells at different ages. All of the age groups, consisting of 10 mice each, were treated with 1 mg of anti-murine IL-2R β chain antibody to reduce NK activity, and inoculated intraperitoneally with MT-2 cells (5 × 107 cells/mouse) 3 days later.
In ATL patients, tumor cells infiltrate into various organs. Thus, we attempted to detect the HTLV-I Tax and human β-globin genes from various organs in the mice inoculated with MT-2 cells (Table 1). The organs in which both genes were detected were considered positive. All organs tested were positive in the mice inoculated with the cells at 5 weeks of age. The incidence of positive results in the various organs was 100% of livers, 50% of spleens, 50% of mesenteric lymph nodes (MLN), 50% of peripheral blood mononuclear cells (PBMC), 40% of kidneys and 30% of lungs. The incidence of positive organs decreased as the age of the mice, at the time of injection with the MT-2 cells, increased. In mice inoculated with the cells at 11 weeks of age, only the livers were positive (30% incidence), while all of the other organs were negative. These results indicate that the HTLV-I-transformed T-cell line, MT-2, could infiltrate into various organs in 5-week-old SCID mice and that the mouse may be a good animal model for the analysis of infiltration of ATL cells into various organs.
Discussion
In this report, we found that age is the crucial factor influencing the induction of rapid tumor formation and death in the SCID mice injected with MT-2 cells. Using this model, the effect of new therapeutic agents for ATL can be compared with each other, both in vitro and in vivo, using the same cell lines. The development of NK-cell activity is age-dependent12, 13 and this factor may partially explain the rapid tumor formation and death in SCID mice inoculated with MT-2 cells reported here. NK-cell activity has been shown to play a key role in the rejection of human lymphoid neoplasms in SCID mice.7 Therefore, different methods to improve the xenograft efficiency of ATL cells in SCID mice, including γ-irradiation, and the administration of anti-NK cell antibodies several times, were performed by other workers, in order to reduce NK cell activity.4, 7 Recently, new immunodeficiency mice, such as SCID/beige, lacking NK activity, and NOD/SCID mice have become available for use in the ATL model,14, 15, 16, 17 but tumor death due to intraperitoneally injection of HTLV-I transformed cell lines does not occur in these mice, they are difficult to maintain, and they require genetic monitoring.
To date, the age of mice in this type of experiment has received very little attention. The SCID mice used in this report were 5 weeks old, younger than those used previously, and a single treatment with IL-2R β chain antibody TM-β1, 3 days prior to MT-2 cell injection, to eliminate NK-cell activity, appears to be sufficient at this age to permit rapid tumor formation and death in this model. In conclusion, we propose the following animal model for the evaluation of new therapeutic agents for adult T-cell leukemia:
-
4-week-old SCID mice are used just after weaning (preliminary care of 1 week).
-
1 mg of anti-murine IL-2R β chain antibody TM-β1 for the elimination of NK activity is used to pretreat the mice once.
-
After 3 days, 5 × 107 MT-2 cells are inoculated intraperitoneally into 5-week-old SCID mice.
Finally, other cancer cell lines that did not engraft in older SCID mice in previous reports, are likely to grow using our proposed model of 5-week-old SCID mice, treated to eliminate NK-cell activity at this young age.
References
Hinuma Y, Nagata K, Hanaoka M, et al. Adult T-cell leukemia: antigen in an ATL cell line and detection of antibodies to the antigen in human sera. Proc Natl Acad Sci USA 1981;78:6476–6480.
Poiesz BJ, Ruscetti FW, Gazdar AF, et al. Detection and isolation of type C retrovirus particles from fresh and cultured lymphocytes of a patient with cutaneous T-cell lymphoma. Proc Natl Acad Sci USA 1980;77:7415–7419.
Mori N, Fujii M, Ikeda S, et al. Constitutive activation of NF-κB in primary adult T-cell leukemia cells. Blood 1999;93:2360–2368.
Ishihara S, Tachibana N, Okayama A, et al. Successful graft of HTLV-I-transformed human T-cells (MT-2) in severe combined immunodeficiency mice treated with anti-asialo GM-1 antibody. Jpn J Cancer Res 1992;83:320–323.
Feuer G, Zack JA, Harrington Jr WJ, et al. Establishment of human T-cell leukemia virus type I T-cell lymphomas in severe combined immunodeficient mice. Blood 1993;82:722–731.
Kondo A, Imada K, Hattori T, et al. A model of in vivo cell proliferation of adult T-cell leukemia. Blood 1993;82:2501–2509.
Feuer G, Stewart SA, Baird SM, et al. Potential role of natural killer cells in controlling tumorigenesis by human T-cell leukemia viruses. J Virol 1995;69:1328–1333.
Imada K, Takaori-Kondo A, Akagi T, et al. Tumorigenicity of human T-cell leukemia virus type I-infected cell lines in severe combined immunodeficient mice and characterization of the cells proliferating in vivo. Blood 1995;86:2350–2357.
Tanaka T, Kitamura F, Nagasaka Y, et al. Selective long-term elimination of natural killer cells in vivo by an anti-interleukin 2 receptor beta chain monoclonal antibody in mice. J Exp Med 1993;178:1103–1107.
Saiki RK, Gelfand DH, Stoffel S, et al. Primer-directed enzymatic amplification of DNA with a thermostable DNA polymerase. Science 1988;239:487–491.
Ohsugi T, Ishibashi K, Shingu M, et al. Engraftment of HTLV-I-transformed human T-cell line into SCID mice with NK cell function. J Vet Med Sci 1994;56:601–603.
Kiessling R, Hochman PS, Haller O, et al. Evidence for a similar or common mechanism for natural killer cell activity and resistance to hemopoietic grafts. Eur J Immunol 1977;7:655–663.
Pflumio F, Lapidot T, Murdoch B, et al. Engraftment of human lymphoid cells into newborn SCID mice leads to graft-versus-host disease. Int Immunol 1993;5:1509–1522.
Richard V, Lairmore MD, Green PL, et al. Humoral hypercalcemia of malignancy: severe combined immunodeficient/beige mouse model of adult T-cell lymphoma independent of human T-cell lymphotropic virus type-1 tax expression. Am J Pathol 2001;158:2219–2228.
Liu Y, Dole K, Stanley JR, et al. Engraftment and tumorigenesis of HTLV-1 transformed T cell lines in SCID/bg and NOD/SCID mice. Leuk Res 2002;26:561–567.
Tan C, Waldmann TA . Proteasome inhibitor PS-341, a potential therapeutic agent for adult T-cell leukemia. Cancer Res 2002;62:1083–1086.
Dewan MZ, Terashima K, Taruishi M, et al. Rapid tumor formation of human T-cell leukemia virus type 1-infected cell lines in novel NOD-SCID/γcnull mice: suppression by an inhibitor against NF-κB. J Virol 2003;77:5286–5294.
Acknowledgements
This work was supported in part by a Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ohsugi, T., Yamaguchi, K., Kumasaka, T. et al. Rapid tumor death model for evaluation of new therapeutic agents for adult T-cell leukemia. Lab Invest 84, 263–266 (2004). https://doi.org/10.1038/labinvest.3700034
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3700034