Abstract
Study design:
Double-blind, randomized, placebo-controlled, parallel-group clinical trial.
Objective:
Assess safety and efficacy of sustained-release fampridine in subjects with chronic spinal cord injury.
Setting:
A total of 11 academic rehabilitation research centers in the United States.
Methods:
A total of 91 subjects with motor-incomplete spinal cord injury (SCI), randomized to three arms: fampridine, sustained release, 25 mg b.i.d. (Group I), 40 mg b.i.d. (Group II), and placebo (Group III) for 8 weeks. Outcome measures: Patient diary questionnaire, Ashworth score, American Spinal Cord Injury Association International Standards, International Index of Erectile Function, bladder and bowel management questionnaires, and Clinician and Subject Global Impressions (Clinician Global Impression of change, Subject Global Impression (SGI)). Safety was evaluated from adverse events, physical examinations, vital signs, electrocardiograms, and laboratory tests.
Results:
In total, 78% of the subjects completed the study. More (13/30) discontinued from Group II than Group I (4/30) and Group III (3/31). The most frequent adverse events across groups were hypertonia, generalized spasm, insomnia, dizziness, asthenia, pain, constipation, and headache. One subject in Group II experienced a seizure. SGI changed significantly in favor of Group I (P=0.02). Subgroup analysis of subjects with baseline Ashworth scores >1 showed significant improvement in spasticity in Group I versus III (P=0.02).
Conclusions:
Group I showed significant improvement in SGI, and potential benefit on spasticity. The drug was well tolerated. Group II showed more adverse events and discontinuations.
Sponsorship:
The study was sponsored by Acorda Therapeutics, Inc.
Similar content being viewed by others
Introduction
Fampridine (also known by its chemical name of 4-aminopyridine, or 4-AP) is a specific blocker of voltage-dependent, neuronal potassium (K+) channels in demyelinated axons. The proposed mechanism of action suggests that fampridine restores action potential conduction in damaged, poorly myelinated nerve fibers. It does this by blocking K+ channels that are exposed in the internodal membrane of demyelinated axons, thereby prolonging the duration of the action potential and restoring conduction.1 It may also directly enhance synaptic transmission.1, 2 Previous clinical studies have indicated that intravenous or oral administration of fampridine reduces spasticity and improves sensory and motor function in subjects with spinal cord injury (SCI).3, 4, 5, 6, 7 Additionally, studies indicate that fampridine may be associated with improvements in sexual function, increased bowel and bladder control, and reduced neurogenic pain.5, 6, 7
In published clinical trials, adverse events with fampridine have been generally transient and mild to moderate in severity. Adverse events associated with oral administration of fampridine at doses <80 mg/day have included dizziness, light-headedness, paresthesia/dysesthesias, nausea, insomnia, headache, and agitation.3, 4, 5, 6, 7, 8, 9, 10, 11 Serious adverse events have included seizures that were associated with uncontrolled overdose, high systemic doses, or relatively high plasma levels of fampridine (>100 ng/ml).12, 13, 14, 15
Orally administered immediate-release (IR) formulations of fampridine have been shown to produce rapid peak plasma concentrations shortly after dosing (time to maximum concentration [tmax] is approximately 1 h)16 and have a plasma half-life (t1/2) of approximately 3.5 h.17 This suggests that four or more daily doses of the IR formulation would be needed to maintain therapeutic effect. The sustained-release formulation used in this study, Fampridine-SR is slowly absorbed (mean tmax 2.6–3.7 h) and eliminated (mean t1/2 5.6–7.6 h) following oral administration, with steady state achieved following 4 days of twice-daily dosing.18 This study was designed to assess the safety and potential efficacy of two different doses of this formulation (25 mg b.i.d. and 40 mg b.i.d.) compared with placebo in subjects with chronic, motor-incomplete SCI. We hypothesized that subjects receiving fampridine would experience improvements in at least one of four functional status domains on a patient diary questionnaire.
Methods
Participants
Subjects enrolled in the study were 18–70 years of age with neurologic impairment secondary to SCI. Their injury had occurred at least 18 months before screening, and their neurologic status had been stable for at least 6 months. Subjects were either tetraplegic or paraplegic with an American Spinal Cord Injury Association (ASIA) Impairment Scale classification of grade C or D; in the clinician's judgment, had significant clinical impairment in at least two of four functional domains (spasticity, bowel, bladder, and sexual function); had a lesion level between C4 to T10, inclusive; and were able and willing to voluntarily give informed consent and comply with the protocol. Subjects could be included whether or not they were being treated concurrently with anti-spasticity medications, as long as such treatment was stable and consistent.
Subjects were excluded from study entry if they were pregnant, lactating, or sexually active females subjects not using approved birth control; had a seizure or treatment for seizure disorders in the previous 12 months; had known allergies to pyridine or any inactive ingredient in Fampridine-SR; had evidence of significant, diffuse, or generalized lower motor neuron damage; had clinically significant abnormal laboratory values or an abnormal electrocardiogram (ECG); had received new concomitant medication less than 3 weeks before the study or had a dose of current concomitant medication that was expected to change during study, botulinum toxin injection for spasticity within 4 months of the screening visit, other investigational drugs within 30 days before screening, or previous treatment with fampridine; had a history of alcohol or drug abuse in the previous year; or any medical condition that would interfere with interpretation of study results or study conduct. The study enrollment period began on June 27, 2000 and concluded on March 6, 2001.
Design
This was a multicenter Phase 2, randomized, double-blind, parallel-group study with three treatment arms for comparison that included placebo, Fampridine-SR, 25 mg b.i.d., or 40 mg b.i.d. The treatment period began with a 2-week single-blind placebo lead-in to establish baseline levels of function and self-assessment, followed by a 2-week dose titration phase, 4 weeks at the fixed target dose (placebo, 25 mg b.i.d., or 40 mg b.i.d.), a 2-week downward titration, and a 1-week washout period (Table 1). Study drug was administered every 12 h at approximately the same time each day. Weekly visits to the clinic occurred on the last day of each treatment week. During the dose titration period, subjects were monitored for dose-limiting toxicity (defined as a drug-related adverse event severe enough to interfere with subject activity), and the investigator judged whether the subject should receive the next-higher dose. Subjects who withdrew from the study due to adverse events were asked to complete end-of-study assessments at the time of withdrawal.
Fampridine-SR (manufactured by Elan Corporation, plc., Athlone, Ireland) was provided in oval-shaped, sustained-release matrix tablets, containing fampridine equivalent to 5, 10, 15, 20, 25, 30, 35, or 40 mg. Placebo tablets were identical in appearance to the fampridine tablets and contained the same inactive ingredients. The study was conducted at 11 academic research centers in the United States.
Safety assessments
A complete medical history was taken for each subject during the screening visit. A full physical examination was performed at the screening visit, with a brief physical examination performed at each subsequent study visit. Vital signs (blood pressure, heart rate, respiratory rate, and body temperature) were measured at screening and at each study visit. Laboratory evaluations included clinical laboratory tests for blood chemistry, hematology, and urinalysis, and were obtained at the screening visit, after the 4-week fixed-dose period, and at follow-up (only if considered necessary by the investigator). ECGs were obtained at the screening visit, after 2 weeks of dose titration, after 4 weeks of fixed dose, and at follow-up (only if considered necessary by the investigator). Adverse events were reported throughout the study and came from three sources: those spontaneously reported by the subject, those elicited from the subject in response to a neutral question from study staff, and those observed by study staff. Adverse events were graded by severity (mild, moderate, or severe) and relationship to study drug (none, unlikely, possible, or probable).
Serious adverse events were reported to the study sponsor within 24 h. A serious adverse event was defined as any experience that was fatal or life-threatening (ie, the patient was at immediate risk of death from the event as it occurred); was permanently disabling; required inpatient hospitalization or prolonged hospitalization; resulted in a congenital anomaly, malignancy, or overdose; or was unusual and potentially serious.
Efficacy assessments
Primary outcome
The prospectively defined primary outcome for the study was positive response to treatment on a patient diary questionnaire (PDQ), developed for this study. The PDQ was used to evaluate a subject's daily experience of functional disabilities (spasticity, bladder, bowel, and male/female sexual function) and physical well-being (see Appendix A). The primary question for each of the four functional domains asked subjects to rate their experience over the previous 24 h within that domain. Possible response options corresponded to a scale of one (‘worst imaginable’) to seven (‘best imaginable’). The fifth domain captured overall self-reported health status, also on a scale of one (‘terrible’) to seven (‘delighted’). In addition, the PDQ provided specific questions about the frequency and duration of symptoms for each functional domain (see Appendix A). Positive response was defined as at least a one-unit improvement from the average score during baseline to the average score during the full-dose treatment period in at least one of the four self-reported functional status domains of the PDQ, and an improvement on the PDQ in overall self-reported physical well-being. The PDQ was completed daily and faxed to the data management center by each subject.
Other subject assessments
The International Index of Erectile Function (IIEF, 15-item questionnaire to assess male sexual function) was completed by male subjects at the visit before the placebo lead-in period and at the end of the 4-week fixed-dose period.19
A bladder management questionnaire (eight items regarding bladder routine) and bowel management questionnaire (nine items regarding bowel routine) were self-administered before the placebo lead-in period and at the end of the 4-week fixed-dose period (see Appendix B). Each subject completed an assessment of the effects of the study medication, over the preceding week, on his or her quality of life using the Subject Global Impression (SGI; seven-point scale ranked from terrible to delighted)3 at the end of the second week of the placebo lead-in period and each week until the end of the 4-week fixed-dose period. Each subject responded to a subject summary questionnaire at the follow-up visit. This consisted of three questions: whether the subject believed they received active drug, the reason for that belief, and whether they would continue to use the medication, once available.
Clinician assessments
Neurological examination performed with the International Standards for Neurological Classification20 at screening and at the end of the 4-week fixed-dose period. Spasticity assessments were evaluated at each study visit using the Ashworth Scale.21 The Ashworth score was averaged over four lower extremity muscle groups; left and right knee flexors and extensors. A trained individual experienced in the Ashworth assessment, such as a physical therapist or nurse coordinator, performed the Ashworth examination (usually and wherever possible the same evaluator at all study visits for a given subject). The Ashworth Scale data were collected on a 1–5 scale rather than the published 0–4 scale, but are presented here transformed to the original 0–4 scale for clarity and comparability with other studies. Spasticity was also assessed with the Spasm Frequency Score recorded and averaged for both arms and legs, and the Tendon Reflex Score for the lower extremities only, averaging the score for right and left sides. Using the neurologic status of each subject at the first (screening) visit as baseline, the study physician was to assess each subject using the Clinician Global Impression of Change (CGI; seven-point scale ranked from significantly worse to significantly improved) during the second week of the placebo lead-in period and each week through the end of the study.
Statistical analysis
Mean scores adjusted for baseline were calculated for each of the PDQ summary scales (spasticity; bladder, bowel, sexual function; and physical well-being), impairment-specific symptoms, CGI (unadjusted means), SGI, IIEF, and spasticity assessments. Analysis of variance (ANOVA) was used to compare treatment groups. χ2 or Fisher's exact tests were used to compare categorical variables. All significance tests used Bonferroni Type I error rates of 0.025 to allow for multiple (three group) comparisons.
The sample size in each group was selected to ensure sufficiently precise estimates of event rates in the placebo and treatment groups to design a potential future Phase 3 study. Assuming a placebo event rate of 0.20, the sample size of 30 would provide an estimated rate with a standard error of approximately 0.07 (i.e. √(0.8 × 0.2/30)). Assuming the success rates in the treated group to be between 0.5 and 0.8, the estimated standard errors were expected to lie somewhere between 0.07, for rates close to 0.8, and 0.09, for rates close to 0.5.
Results
Subject demographics and disposition
Of the 91 subjects randomized for treatment, 71 (78%) completed the study (Figure 1). The demographics and baseline characteristics of randomized subjects were comparable across the three treatment arms (Table 2). The proportion of subjects who failed to complete the study in the 40 mg b.i.d. treatment group (43%; 13/30) was higher when compared to the 25 mg b.i.d. group (13%; 4/30) or the placebo group (10%; 3/31). Most subjects were discontinued because of adverse events but two subjects were lost to follow-up and two withdrew consent for reasons unrelated to adverse events (Figure 1). With regard to the time of withdrawal from the study, 12 subjects (seven in the 40 mg b.i.d. group, three in the 25 mg b.i.d. group, and two in the placebo group) withdrew during the 2-week dose-titration period, six subjects (five in the 40 mg b.i.d. group and one in the placebo group) withdrew during the 4-week fixed-dose period, and two subjects (one in the 40 mg b.i.d. group and one in the 25 mg b.i.d. group) withdrew during the 2-week down-titration period.
Safety and tolerability
Adverse events experienced by at least 2% of enrolled subjects are noted in Table 3. The incidence of adverse events was highest in the 40 mg b.i.d. group. A statistically greater number of subjects in the 40 mg b.i.d. group than in the placebo group reported having abdominal pain, dizziness, insomnia, paresthesia, nervousness, and anxiety. Pain was the only adverse event that occurred in significantly more subjects in the 25 mg b.i.d. group than in the placebo group. Most adverse events were mild to moderate in severity and were transient. As noted in the previous section, a total of 16 subjects discontinued due to adverse events: two from the placebo group, three from the 25 mg b.i.d. group, and 11 from the 40 mg b.i.d. group. The adverse events most frequently associated with discontinuation were dizziness (8%), insomnia (4%), and nausea (3%).
Six subjects, two from each treatment group, reported a combined total of 10 serious adverse events (SAEs) (some subjects experienced more than one event). Only one SAE, a seizure in a subject with a history of traumatic brain injury, was considered probably related to the study drug. The subject was in the 40 mg b.i.d. group and had been taking study medication for approximately 7 weeks. The study drug was discontinued, the subject was treated briefly with phenytoin and carbamazepine and no further seizures occurred. Another subject, also in the higher dose group, developed gastrointestinal bleeding that was assessed as having a possible relationship to the study drug. He was treated with famotidine, and study drug was not interrupted. All other (eight) SAEs were considered either unlikely to be related or not related to the study drug. Two subjects in the placebo group experienced an SAE: one subject had sepsis, hemorrhagic gastritis, and a urinary tract infection (UTI), and one subject had dysautonomia, hypertonia, and a UTI. In the 25 mg b.i.d. group, one subject had deep vein thrombosis and one subject had a UTI. No clinically significant changes were reported for other parameters (physical examinations, vital signs, ECGs, or clinical laboratory tests).
Efficacy
Primary end point – PDQ
Overall positive response rates on the PDQ were low and not significantly different between treatment groups, with five subjects (17%) in the fampridine 25 mg b.i.d. group versus three (10%) in the placebo and one (3%) in the fampridine 40 mg b.i.d. group. Different definitions of positive response, including lowering the criterion to an average half point change, did not reveal more significant differences between treatment groups.
Despite the lack of significance on overall positive response rate, some of the individual questions within the PDQ appeared to show more differentiation. A significantly larger number of subjects in the 25 mg b.i.d. and 40 mg b.i.d. groups had an increase in the number of days with bowel movements compared to subjects in the placebo group (P=0.02 and P=0.01, respectively), as derived from responses to the question: ‘Did you have a bowel movement in the last 24 h?’ Two questions in the bladder function domain of the PDQ (‘Over the last 24 h, did you experience accidental urination or ‘leaking’?’ and ‘If yes, indicate the number of times’) showed a strong trend (P=0.06 and 0.04, respectively) for reduced frequency of bladder accidents in subjects in the fampridine 25 mg b.i.d group compared to placebo. The percentage of subjects showing improvement on this measure in the 40 mg b.i.d. group was also higher than in the placebo group, but did not show a marked statistical trend. No statistically significant differences were identified between treatment groups for other individual questions on the PDQ.
Secondary end points
Subjects in the fampridine 25 mg b.i.d. group showed statistically significant improvement in SGI scores compared with placebo (P=0.02) (Table 4). The 40 mg b.i.d. group was not statistically different from the placebo group. Marked trends for improvement in IIEF scores were seen for both fampridine treatment groups compared to the placebo group, although the sample of male subjects was relatively small (Table 4). Mean scores (adjusted for baseline) for erection frequency and firmness, ability to maintain erections, and levels of sexual desire showed greater improvements in fampridine groups than in the placebo group. There was a statistically significant difference in the fampridine 25 mg b.i.d. group compared with placebo for erection frequency (P=0.02). While not statistically significant, total IIEF score changes favored both fampridine doses over placebo, with an average difference of approximately 7.5 points for both.
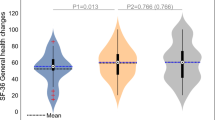
The clinician-assessed measures, including neurologic assessments (ASIA International Standards at screening and end of 4-week fixed-dose period), spasticity assessments (Ashworth Scale, Tendon Reflex Score, Spasm Frequency Score), and CGI did not show statistically significant treatment differences. However, the Ashworth Score showed a strong trend to improvement in the 25 mg b.i.d. group compared to placebo (P=0.04). As the difference between these groups was limited by the fact that a large proportion of subjects had little or no spasticity at baseline, a post hoc subgroup analysis was performed for subjects with a baseline Ashworth score greater than the median score of 1.0. In 14 subjects with a baseline Ashworth score greater than median who received fampridine 25 mg b.i.d., the reduction in mean total Ashworth score was statistically significant (P=0.02) following 4 weeks of treatment compared with baseline (Figure 2). In seven subjects with a baseline Ashworth score ⩾2.0, the reduction in mean total Ashworth score did not quite reach statistical significance (P=0.03), but the magnitude of the reduction was even greater than that of the first subgroup when compared with placebo.
Histograms to show the changes in Ashworth score from baseline (placebo run-in) to treatment period (average of weeks 5–8) for the placebo and 25 mg b.i.d. groups. In addition to the prospective analysis of the intent-to-treat population, two subgroups were examined post hoc, one containing all subjects with baseline Ashworth scores greater than the median (1.0) and the other containing all subjects with baseline Ashworth scores greater than or equal to 2.0 on the 0–4 point scale. Statistical significance was assigned at P<0.025 to allow for the three group comparison. The reduction in score with treatment was significantly larger for the fampridine-treated subjects compared to the placebo-treated subjects for the subgroup with baseline scores greater than the median
Discussion
The primary goals of the study were to compare the safety and preliminary efficacy of two doses of fampridine using the PDQ instrument, collecting sufficient data on positive response rate to allow calculation of a suitable group size for a well-powered efficacy study. The PDQ instrument was developed to address the testing of an intervention with the potential for affecting numerous aspects of neurological dysfunction in SCI, and with the likelihood of affecting different aspects to different extents in each subject. The questionnaire was designed to standardize the approach to four key domains of SCI symptoms and at the same time to address the lack of validated assessment tools for bladder and bowel function in this population. The structure of the instrument was a logical pyramid, leading from an overall subject assessment of physical well-being, to the overall assessments of the four domains (bowel, bladder, sexual function, and spasticity), each of which could be illuminated by specific and largely quantitative questions about daily experience.
Safety
With regard to the safety and tolerability of Fampridine-SR, this study highlights the need for gradual dose titration. Subjects randomized to fampridine 25 mg b.i.d. and 40 mg b.i.d. were titrated to their target dose over a 2-week period, with steps of 5 mg b.i.d. every three and a half days. This titration schedule was more rapid than in a previous study, which explored even higher doses at steps of 5 mg b.i.d. every 7 days.22 That study involved a lower incidence of discontinuation during dose escalation. The rapid dose escalation in the present study may have contributed to the higher dropout rate owing to adverse events in the 40 mg b.i.d. group (n=11) as compared with the 25 mg b.i.d. group (n=3) or the placebo group (n=2). More rapid titration to higher doses of fampridine appears to be associated with adverse events involving the central nervous system and digestive system, most notably dizziness, insomnia, and nausea.
One subject with a history of traumatic brain injury suffered a seizure during study week 8 at the end of the 40 mg b.i.d. dose period. Subjects experiencing a seizure or receiving therapy for a seizure disorder in the 12 months preceding the study were excluded from the study because of the known potential for enhancing susceptibility to seizure with this drug. Cases of seizure activity that have been reported in subjects with multiple sclerosis were associated with uncontrolled overdose,15 high systemic doses, or high plasma levels of Fampridine (>150 ng/ml).13, 14, 15 At the time of the current study, there had been no report of seizures in any clinical study of fampridine in chronic SCI. It should be noted that the subject who experienced the seizure in this study had a history of traumatic brain injury and was taking a concomitant antispasticity medication (baclofen) that has been reported to lower the seizure threshold.23 The experience in this study continues to suggest that study subjects with a history of seizures, prior traumatic brain injury, or other risk of seizure should be evaluated carefully before starting treatment with fampridine.
Efficacy
Efficacy findings of this study should be interpreted cautiously because of the small sample size (approximately 30 subjects per group) and the extent of significance testing on multiple outcome variables that was performed. Nonetheless, the overall results of this small study, in combination with broadly consistent published experience, continue to support the concept that fampridine may have value in the treatment of patients with SCI.
Both subject and clinician global assessment variables (SGI and CGI) favored fampridine 25 mg b.i.d. over placebo, with results on the SGI reaching statistical significance (P=0.02). These global ratings are more encouraging when viewed together with improvements in specific functional aspects of the PDQ, including bladder function (decrease in days with accidental urination and decrease in number of bladder ‘accidents’ per day), bowel function (more days with bowel movements, suggesting improved regularity), and in combination with strong trends for improvement on the IIEF and the Ashworth scores. Even modest improvements in bowel, bladder, and sexual function and spasticity can be meaningful to people with chronic SCI.
Two limitations of this study are likely to have contributed to the relatively low rate of positive response on the PDQ and the limited evidence of efficacy on other measures. First, the only symptom severity requirement for study entry was that the subject show deficits on at least two of the functional domains in the PDQ. Second, concomitant medications for spasticity were allowed during the study, because of the subject discomfort potentially associated with discontinuing these treatments. Consequently, 53 subjects (58%) were receiving concomitant treatment for spasticity. This almost certainly contributed to the low average baseline Ashworth scores and thereby decreased the ability to evaluate the effect of fampridine on spasticity in the population sample.
The change from baseline in mean Ashworth score was not statistically significant when fampridine-treated subjects were compared to those receiving placebo (P=0.04 in a three group comparison). However, in a post hoc subgroup analysis, regardless of the presence or absence of concomitant medications for spasticity, changes in Ashworth mean scores in subjects receiving fampridine 25 mg b.i.d. versus placebo were statistically significant (P<0.025) for those subjects with more marked levels of spasticity at baseline (Figure 2).
A benefit on spasticity is consistent with earlier studies. Marked improvement in spasticity following intravenous infusion of 4-aminopyridine was reported in two subjects in a small double-blind, placebo-controlled crossover study5 involving six subjects with incomplete SCI. A larger, double-blind, crossover study of fampridine subsequently showed a dose-related improvement in average Modified Ashworth Score.3 The improvement in spasticity was significant for the higher dose period (17.5 mg b.i.d.).
Conclusions
In this study, treatment with fampridine, sustained release, 25 mg b.i.d. was associated with significantly improved SGI (P=0.02) in subjects with chronic motor-incomplete SCI. Also, in a post hoc subgroup analysis of subjects with baseline Ashworth scores greater than the median, treatment with fampridine 25 mg b.i.d. was associated with significantly reduced spasticity (P=0.02). Safety and tolerability results in this study indicate that, with appropriate patient selection and gradual dose titration, sustained release fampridine can be well tolerated. Based on the results of this and previous studies, fampridine should be investigated further as a potential treatment for spasticity in patients with chronic SCI.
References
Blight AR . Effect of 4-aminopyridine on axonal conduction-block in chronic spinal cord injury. Brain Res Bull 1989; 22: 47–52.
Waxman SG . Aminopyridines and the treatment of spinal cord injury. J Neurotrauma 1993; 10: 19–24.
Potter PJ et al. Randomized double-blind crossover trial of Fampridine-SR (sustained release 4-aminopyridine) in patients with incomplete spinal cord injury. J Neurotrauma 1998; 15: 837–849.
Hayes KC et al. Preclinical trial of 4-aminopyridine in patients with chronic spinal cord injury. Paraplegia 1993; 31: 216–224.
Hansebout RR, Blight AR, Fawcett S, Reddy K . 4-Aminopyridine in chronic spinal cord injury: a controlled, double-blind, crossover study in eight patients. J Neurotrauma 1993; 10: 1–18.
Hayes KC et al. 4-Aminopyridine-sensitive neurologic deficits in patients with spinal cord injury. J Neurotrauma 1994; 11: 433–446.
Potter PJ et al. Sustained improvements in neurological function in spinal cord injured patients treated with oral 4-aminopyridine: three cases. Spinal Cord 1998; 36: 147–155.
Davis FA, Stefoski D, Rush J . Orally administered 4-aminopyridine improves clinical signs in multiple sclerosis. Ann Neurol 1990; 27: 186–192.
Jones RE et al. Effects of 4-aminopyridine in patients with multiple sclerosis. J Neurol Sci 1983; 60: 353–362.
Sanders DB, Kim YI, Howard Jr JF, Goetsch CA . Eaton–Lambert syndrome: a clinical and electrophysiological study of a patient treated with 4-aminopyridine. J Neurol Neurosurg Psychiatry 1980; 43: 978–985.
Stefoski D et al. 4-Aminopyridine in multiple sclerosis: prolonged administration. Neurology 1991; 41: 1344–1348.
Bever Jr CT et al. The effects of 4-aminopyridine in multiple sclerosis patients: results of a randomized, placebo-controlled, double-blind, concentration-controlled, crossover trial. Neurology 1994; 44: 1054–1059.
Ball AP et al. Human botulism caused by Clostridium botulinum type E: the Birmingham outbreak. Q J Med 1979; 48: 473–491.
Murray NM, Newsom-Davis J . Treatment with oral 4-aminopyridine in disorders of neuromuscular transmission. Neurology 1981; 31: 265–271.
Spyker DA, Lynch C, Shabanowitz J, Sinn JA . Poisoning with 4-aminopyridine: report of three cases. Clin Toxicol 1980; 16: 487–497.
Evenhuis J et al. Pharmacokinetics of 4-aminopyridine in human volunteers. A preliminary study using a new GLC method for its estimation. Br J Anaesth 1981; 53: 567–570.
Hayes KC et al. Pharmacokinetics of an immediate release oral formulation of fampridine (4-aminopyridine) in normal subjects and patients with spinal cord injury. J Clin Pharmacol 2003; 43: 379–385.
Hayes KC et al. Pharmacokinetic studies of single and multiple oral doses of Fampridine-SR (sustained-release 4-aminopyridine) in patients with chronic spinal cord injury. Clin Neuropharmacol 2003; 26: 185–192.
Rosen RC et al. The International Index of Erectile Function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 1997; 49: 822–830.
American Spinal Injury Association (ASIA). Standards for Neurological Classification of Spinal Injury Patients (revised 1996).
Ashworth B . Preliminary trial of carisoprodol in multiple sclerosis. Practitioner 1964; 192: 540–542.
Hayes KC et al. Pharmacokinetics and safety of multiple oral doses of sustained-release 4-aminopyridine (Fampridine-SR) in subjects with chronic, incomplete spinal cord injury. Arch Phys Med Rehabil 2004; 85: 29–34.
Schuele SU et al. Incidence of seizures in patients with multiple sclerosis treated with intrathecal baclofen. Neurology 2005; 64: 1086–1087.
Acknowledgements
We thank Professor Donald L Patrick, PhD, Michelle Althuis, PhD, and Janet Wittes, PhD for their contributions to the development of the PDQ instrument. Acorda Therapeutics, Inc. sponsored this study. The following principal investigators and clinical sites contributed data to the study: Virginia Graziani, MD, Thomas Jefferson University Hospital, Philadelphia, PA; Daniel Lammertse, MD, Craig Hospital, Englewood, CO; Aḿie B Jackson, MD, Spain Rehabilitation Center, Birmingham, AL; Ralph Marino, MD, Mt Sinai Medical Center, New York, NY; Steven Kirshblum, MD, Kessler Institute for Rehabilitation, West Orange, NJ; William L Bockeneck, MD, Charlotte Institute of Rehabilitation, Charlotte, NC; Diana D Cardenas, MD, University of Washington Medical Center, Seattle, WA; Marca L Sipski, MD, University of Miami School of Medicine, Miami, FL; John W McDonald, MD, PhD, Washington University School of Medicine, St Louis, MO; Dennis J Maiman, MD Medical College of Wisconsin, Milwaukee, WI; Suzanne Groah MD Santa Clara Valley Medical Center, San Jose, CA.
Author information
Authors and Affiliations
Additional information
Statement of Ethics: We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the completion of this research
Disclosures: Ron Cohen and Andrew Blight are employees and hold equity positions in Acorda Therapeutics, the study sponsor. All the other authors on this paper are consultants to, and have served as clinical investigators for Acorda Therapeutics in this or other studies
Appendices
Appendix A: PDQ
This instrument was developed on the basis of interviews with subjects from earlier completed studies of fampridine in SCI. Subjects were asked to describe their impressions of any changes they experienced during treatment. The resultant questionnaire was designed to try to evaluate changes across a wide range of symptomatology and to support broader qualitative impressions with detailed quantitative observations. The content and format of the questions was refined by extensive discussion and iterative revision between clinicians, statisticians, and an experienced psychometrician. The questionnaire was initially explored in a smaller, open-label dose-ranging study22 but has not been published previously.
The definitions, questions, and potential responses used in the PDQ instrument are provided here. The actual questionnaire was formatted to allow subjects to complete it with a combination of checked boxes and entering numbers into prepared spaces.
PDQ – spasticity
Definition: ‘Spasticity’ is defined here as problems with your muscles that include uncontrolled movements or muscle contractions (spasms) and/or stiffness. These may cause pain, discomfort, and/or difficulty in making voluntary movements. Some people find their spasticity is helpful at times.
-
a)
We would like to know about the strength of your muscle spasms and how often they occurred. Please mark the one response that best describes your spasms over the last 24 h. None/mild/full spasms a little of the time/some of the time/a good bit of the time /most of the time/all of the time.
-
b)
Considering the amount of stiffness throughout the day, please mark the one response that best describes your stiffness, on average, over the last 24 h. None/a little/some/a good bit/a great deal of stiffness.
-
c)
We would like to know how much you feel spasticity affected ease of movement. Please mark the one response that best describes how spasticity affected your ease of movement over the last 24 h. Helpful, on the whole/no effect, on the whole/restricted it a little/somewhat/a good bit/severely.
-
d)
Were you awakened last night by spasticity? If yes, how many times.
-
e)
Overall evaluation: Taking into account your responses to these questions, please mark the one response that best expresses your overall impression of your spasticity in the last 24 h: worst imaginable/very poor/poor/fair/good/very good/best imaginable.
PDQ – bladder
Definition: Bladder function is defined here as your ability to control urination (emptying your bladder). This can be measured in a number of ways, such as the frequency of catheterization or voluntary urination, the amount of time you can hold your urine, the frequency of waking at night with the need to urinate, and the presence of problems such as leaking, difficulty urinating, and urinary tract infections (UTIs).
-
a)
Over the last 24 h, what was your bladder routine based on:? (please mark one response for each numbered item) indwelling Foley catheter/suprapubic catheter/condom catheter/intermittent catheterization/voluntary urination. How many times did you catheterize in the last 24 h? How many times did you urinate voluntarily in the last 24 h?
-
b)
Over the last 24 h, did you experience any of the following?
-
1)
Sensation of the need to urinate? If yes, how long could you hold your urine after first feeling the need to go?
-
2)
Accidental urination or ‘leaking’? If yes, how many times?
-
3)
Difficulty starting or continuing the stream? If yes, how long it took you to urinate, on average.
-
4)
Waking at night with the need to urinate? If yes, the number of times you got up to urinate.
-
5)
Symptoms of a UTI?
-
1)
-
c)
Overall evaluation: Taking into account your responses to these questions, please mark the one response that best expresses your impression of your bladder function in the last 24 h: worst imaginable/very poor/poor/fair/good/very good/best imaginable.
PDQ – bowel
Definition: Bowel function is defined here as your ability to control your bowel movements. This can be measured in a number of ways, such as the length and frequency of your bowel routine, the medication or stimulation you require, and whether you experience various problems with bowel movements.
-
a)
Approximately how long did you spend on your bowel routine in the last 24 h?
-
b)
Did you have a bowel movement in the last 24 h? If yes, how many times?
-
c)
Did you use any of the following as part of your bowel routine in the last 24 h? digital stimulation or assistance/a suppository/an enema (such as Fleets)/pulsed irrigation enema (PIE) system, or high colonic enema/oral medication (over-the-counter or prescription)
-
d)
In the last 24 h, have you experienced any of the following? feeling constipated/diarrhea/painful bowel movement/accidental bowel movement/the feeling of ‘almost having’ an accidental bowel movement If yes, how many times did you had the feeling of almost having an accidental bowel movement.
-
e)
Overall evaluation: Taking into account your responses to these questions, please mark the one box that best expresses your impression of your bowel function in the last 24 h: worst imaginable/very poor/poor/fair/good/very good/best imaginable.
PDQ – male sexual function
Definition: Sexual function is defined as the amount of physical sensation you experience, the duration and strength of your erections, and your ability to achieve orgasms, all related to sexual activity of any kind, whether this activity occurred with or without a partner.
-
a)
How much physical sensation did you have related to sexual activity over the last 24 h? none/a little/some/a good bit/full sensation/not sexually active, with or without a partner
-
b)
Have you had erection(s) in the last 24 h? If yes, were you able to maintain your erection(s) satisfactorily? Rate (on average) the hardness of your erection(s) over the last 24 h: not hard at all/slightly hard/moderately hard/hard/full erection.
-
c)
Have you had orgasm(s) in the last 24 h? If yes, how many times? On average, how long was the time of stimulation needed to orgasm?
-
d)
Overall evaluation: Taking into account your responses to these questions, what is your impression of your sexual function in the last 24 h: worst imaginable/very poor/poor/fair/good/very good/best imaginable.
PDQ – female sexual function
Definition: Sexual function is defined here as the amount of physical sensation and the extent of natural lubrication you experience, and your ability to achieve orgasm related to sexual activity of any kind, whether this activity occurred with or without a partner.
-
a)
How much physical sensation did you have related to sexual activity over the last 24 h? None/a little/some/a good bit/full sensation/not sexually active, with or without a partner
-
b)
Did you have vaginal pain related to sexual activity over the last 24 h? None/mild/moderate/severe pain/I was not sexually active, with or without a partner
-
c)
How much natural lubrication did you experience related to sexual activity over the last 24 h? None/a little/some/a good bit/full lubrication/not sexually active, with or without a partner
-
d)
Have you had orgasm(s) in the last 24 h? If yes, how many times? On average, about how long was the time of stimulation needed to orgasm?
-
e)
Overall evaluation: Taking into account your responses to these questions, what is your impression of your sexual function in the last 24 h: worst imaginable/very poor/poor/fair/good/very good/best imaginable.
PDQ – overall response
Overall, taking into account your spasticity, and your bowel, bladder, and sexual function, what is your impression of your physical well-being in the last 24 h:
terrible/unhappy/mostly dissatisfied/mixed (about equally satisfied and dissatisfied)/mostly satisfied/pleased/delighted
-
a)
Did you take study medication in the last 24 h?
-
b)
Have you experienced or noticed in the past 24 h anything related to your physical well-being that has not been covered in this diary. If yes, describe what you experienced or noticed.
-
c)
Who wrote your responses on this form? self/spouse/partner/other
Appendix B: Bladder and bowel management questionnaire
Bladder management
-
1)
Was your bladder routine over the past month based on: indwelling Foley catheter/suprapubic catheter/condom catheter/intermittent catheterization/voluntary urination.
-
2)
If you void voluntarily, please answer the following questions, using the scale: not at all/less than one time in five/less than half the time/about half the time/more than half the time/almost always.
-
a)
Over the past month, how often have you had a sensation of not emptying your bladder completely after you finished urinating?
-
b)
Over the past month, how often have you had to urinate again less than 2 h after you finished urinating?
-
c)
Over the past month, how often have you stopped and started again several times when you urinated?
-
d)
Over the past month, how often have you found it difficult to postpone urination?
-
e)
Over the past month, how often have you had a weak urinary stream?
-
f)
Over the past month, how often have you had to push or strain to begin urination?
-
g)
Over the past month, how many times did you most typically get up to urinate from the time you went to bed at night until the time you got up in the morning?
-
a)
Bowel management
Please answer the following questions , using the scale:
not at all/less than one time in five/less than half the time/about half the time/more than half the time/almost always.
In your bowel routine over the last month, did you typically use any of the following:
-
a)
Digital stimulation or assistance?
-
b)
A suppository?
-
c)
An enema (such as Fleets)?
-
d)
Oral medication (over-the counter or prescription)?
Over the last month, have you experienced any of the following:
-
a)
Constipation
-
b)
Diarrhea
-
c)
Painful bowel movement(s)
-
d)
Accidental bowel movement(s) between your normal routines
-
e)
The feeling of ‘almost having’ bowel movement(s) between your routines.
Rights and permissions
About this article
Cite this article
Cardenas, D., Ditunno, J., Graziani, V. et al. Phase 2 trial of sustained-release fampridine in chronic spinal cord injury. Spinal Cord 45, 158–168 (2007). https://doi.org/10.1038/sj.sc.3101947
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101947
Keywords
This article is cited by
-
The challenge of recruitment for neurotherapeutic clinical trials in spinal cord injury
Spinal Cord (2019)
-
Treatments for erectile dysfunction in spinal cord patients: alternatives to phosphodiesterase type 5 inhibitors? A review study
Spinal Cord (2015)
-
Two phase 3, multicenter, randomized, placebo-controlled clinical trials of fampridine-SR for treatment of spasticity in chronic spinal cord injury
Spinal Cord (2014)
-
Clinical trials in spinal cord injury: lessons learned on the path to translation. The 2011 International Spinal Cord Society Sir Ludwig Guttmann Lecture
Spinal Cord (2013)
-
Spinal cord injury sequelae alter drug pharmacokinetics: an overview
Spinal Cord (2011)