Abstract
Study design: Prospective analysis of relationships.
Objectives: (1) To quantify the relationship between individual lower extremity muscle strength and functional walking measures and (2) to determine whether a multiple regression model incorporating lower extremity muscle strength could predict the performance of functional walking measures in persons with incomplete spinal cord injury (ISCI) living in the community.
Setting: Tertiary rehabilitation center, Vancouver, Canada.
Methods: In all, 22 subjects with ISCI participated. The relationship between functional walking measures (gait speed, 6-min-walk distance, and ambulatory capacity) and muscle strength (manual tests of hip flexors/extensors/abductors, knee flexors/extensors, ankle dorsiflexors/plantarflexors, and great toe extensors) were measured by Pearson's correlation and regression procedures.
Results: For both the more and less affected sides, hip flexors, hip extensors, and hip abductors produced the highest correlations with the three functional measures. The less affected hip flexor strength explained more than 50% of the variance in gait speed and 6-min-walk distance while the less affected hip extensor strength explained up to 64% of the variance in ambulatory capacity. For all three functional measures, the strength of the less affected limb was more important than that of the more affected limb.
Conclusions: Lower extremity muscle strength, in particular that of hip flexors, hip extensors, and hip abductors, is an important determinant of functional walking performance.
Similar content being viewed by others
Introduction
A significant number of persons with incomplete spinal cord injury (ISCI) retain or regain the ability to walk; however, due to limitations in gait speed and endurance, walking may not be the practical method of mobility in the community.1,2 The gait speed of persons with ISCI has been reported to be considerably lower1,2 than the 1.2 m/s speed required to cross a street within the time allowed by a traffic signal.3 Reductions in gait speed and endurance, together with other factors such as the ability to transfer and manage curbs, stairs and crowded areas, could contribute to the limitation in ambulatory capacity, that is the degree of walking independence in the home and community.
Muscle strengthening is one of the principal interventions following ISCI aimed at improving functional abilities such as walking.4,5 Early recovery of muscle strength post-ISCI has been identified as a useful predictor of ambulatory capacity. For example, Waters et al6,7 reported that lower extremity motor recovery 1 month post-injury was a good predictor of whether an individual became a community ambulator at 1-year follow-up. Moreover, Crozier et al8 found that persons who recovered a greater than grade 3 strength in their less affected quadriceps by 2 months following ISCI had an excellent prognosis for ambulation. Correlational analysis has also been used to examine the relationship between muscle strength and walking abilities in persons with ISCI. Composite scores of lower extremity muscle strength, such as the Ambulatory Motor Index (sum of five lower extremity muscle grades) and the American Spinal Injury Association (ASIA) lower extremity motor scores, have been found to correlate with gait speed and ambulatory capacity both in persons with acute and chronic ISCI.9,10,11 These findings indicate that muscle strength is an important contributor of walking function.
However, the individual muscle groups that most closely relate to walking performance have not been investigated at the exception of one early study12 that identified the least affected hip flexors and quadriceps to be the most important muscle groups for community ambulation in persons with ISCI. Identifying the muscle groups most closely associated with walking can provide guidance for treatment aimed at improving walking in persons with ISCI. The purpose of this study was (1) to quantify the relationship between individual lower extremity muscle strength and functional walking measures (gait speed, endurance as measured by the 6-min-walk distance, and ambulatory capacity) and (2) to determine whether a multiple regression model incorporating lower extremity muscle strength could predict the performance of functional walking measures in persons with chronic ISCI living in the community.
Methods
Subjects and setting
In all, 22 subjects with ISCI were recruited on a volunteer basis. Criteria for inclusion in the study were as follows: (1) have some residual lower extremity weakness secondary to an ISCI, (2) be at least 1-year post-injury, and (3) be able to walk independently or with supervision for at least 6 min (with rest intervals) with or without assistive device. Subjects who had orthopedic or neurological conditions in addition to the spinal cord injury (SCI) were excluded from the study. Ethics approval was obtained from the local university and hospital ethics committees. Each subject was informed of the study procedures before giving their consent to participate in the study. Subject characteristics are summarized in Table 1. Neurological levels and impairment scales were determined according to the American Spinal Injury Association (ASIA) standards.13
Procedures
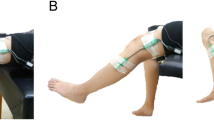
A physical therapist performed the manual muscle test on each subject for eight lower limb muscle groups (hip flexors/extensors/abductors, knee flexors/extensors, ankle dorsiflexors/plantarflexors, and great toe extensors) in standardized positions.14 Muscle strength was graded on a scale from zero to five using 10 intervals as per Herbison et al15 (Table 2). We evaluated the test–retest reliability (separate days) for manual muscle testing in a small group (N=8) of individuals with SCI and found the intraclass correlations to be 0.82–0.99 for the eight lower limb muscle groups. Others15,16,17 have also reported high reliability for upper and lower limb manual muscle testing in persons with SCI. The ASIA lower extremity muscle score (LEMS) was derived from manual muscle tests of five lower extremity muscle groups (hip flexors, knee extensors, ankle dorsiflexors, great toe extensors, and ankle plantarflexors) evaluated using the standard zero to five, six interval scale.13
For the assessment of gait speed, subjects were asked to walk with their usual mobility aid at their ‘most comfortable speed’ (ie self-selected speed) along an 8-m walkway three times. When necessary, rest breaks were taken between trials to ensure that subjects were not fatigued and the trial reflected their true self-selected speed. An optoelectronic sensor (Nothern Digital, Waterloo, Canada) was used to track infrared emitting diodes (IREDs) attached to the participants’ lateral malleoli. In this camera set-up, the error of locating the coordinates of an IRED in space was 0.9 mm in the anterior/posterior direction and 0.45 mm in the up/down direction. Data were collected at 60 Hz. Gait speed was calculated using cumulative consecutive stride lengths (forward distance covered by the lateral malleolus marker from initial contact to the next initial contact of the same leg) in the middle 4-m section (ie, representative window of constant gait speed) of the 8-m walkway and the corresponding elapsed time.
The 6-min-walk test was then performed as a measure of gait endurance. Subjects were instructed to walk for 6 min, covering as much ground as possible, on a flat surface around two marked lines that were 18.5 m apart without stopping unless they needed to.18 No verbal feedback or phrases of encouragement were provided except 1 min before the end of the test, at which point they were informed of the elapsed time. If necessary, subjects performed the 6-min-walk test on a second day. Two subjects did not attend the second session to complete the 6-min-walk test.
Ambulatory capacity, the degree or extent of walking independence in the home and community, was categorized into six levels as described by Perry et al19 (Table 3). The categorization was based on therapist's assessment of their walking level and subjects’ description of the walking activities regularly practiced at home and the community.
Data analysis
Descriptive statistics were performed for all variables measured. To account for possible effects due to anthropometries (eg leg length), gait speed and the 6-min-walk distance were divided by leg length and expressed in relative terms. Leg length was measured from the greater trochanter to the lateral malleolus in meters. Pearson's product moment correlation was used to quantify the relationship between muscle strength and the three functional walking measures: relative self-selected gait speed, relative 6-min-walk distance, and ambulatory capacity. Significance was accepted at an alpha level of 0.05. Scatterplots of the bivariate correlations were visually examined to ensure outliers did not compromise the results of the correlations. Correlational descriptors of Munro et al20 were used to rate the correlations as very high (0.90–1.00), high (0.70–0.89), moderate (0.50–0.69), and low (0.26–0.49). Three separate forward linear multivariate regression models were then used to predict (a) relative self-selected gait speed, (b) relative 6-min-walk distance, and (c) ambulatory capacity using the various muscle strengths from the lower limbs. Variables (ie muscle strengths) were entered in the model at a significance level of P<0.05 and removed from it at P>0.1. All statistical analyses were performed with SPSS 9.0 software.
Results
Strength and functional walking performance – descriptive
All but two subjects had bilateral weakness with one side more affected than the other (Table 4). The weakest muscle groups were the more affected ankle dorsiflexors and hip extensors. Only two and four subjects showed a greater than or equal to grade 3 muscle strength (ie active movement against gravity) in their more affected ankle dorsiflexors and hip extensors, respectively. Moreover, the strength range for the more affected ankle dorsiflexors was only between grade 0 and 3. The least affected muscle groups were the knee extensors and great toe extensors with 18 and 17 subjects, respectively, achieving a greater than grade 3 strength on their more affected side.
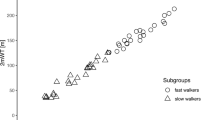
Gait speed was low with only four subjects walking faster than 1 m/s (Table 5). Similarly, the 6-min-walk distance was low with as many as five subjects covering less than 100 m during the allotted 6 min. However, 16 out of 22 subjects were categorized as community ambulators and just one subject was limited to walking only as a form of exercise. Of note, gait speed was determined while subjects walked without orthoses although four subjects customarily used an ankle foot orthosis for community mobility.
Strength and functional walking performance – correlation
Pearson's product moment correlation resulted in significant correlations between all muscle groups and each of the three functional measures with a few exceptions (Table 6). The great toe extensors, the more affected knee extensors, and the less affected ankle dorsiflexors were not significantly related to gait speed or 6-min-walk distance. For ambulatory capacity, the knee extensors and the more affected hip flexors were not significantly related. The ASIA LEMS produced the highest correlation coefficient with all three functional measures. Analysis of individual muscle groups revealed that the less affected hip flexors produced high correlations (r⩾0.70) with both gait speed and 6-min-walk distance. The muscle groups that highly correlated with ambulatory capacity were the hip extensors, hip abductors, and knee flexors of the less affected side. For both the more and less affected sides, hip flexors and hip abductors produced the highest correlations with gait speed and 6-min-walk distance while hip extensors and hip abductors were the most important muscle groups for ambulatory capacity.
The less affected hip flexor strength was selected by the regression model as the best predictor for both self-selected gait speed and 6-min-walk distance accounting for 54 and 57% of the variance in the two tasks, respectively (Table 7). The less affected hip extensor strength was the best predictor for ambulatory capacity and accounted for 64% of the variance. Up to 91% of the variance in ambulatory capacity could be explained when the strength's of the great toe extensors and ankle dorsiflexors from both sides were added to the model.
The three functional measures were significantly correlated with each other (Table 8). However, while gait speed and 6-min-walk distance were very highly correlated (r⩾0.90), ambulatory capacity was only moderately correlated with these two measures.
Discussion
This study examined the relationship between lower extremity muscle strength and walking performance in persons with chronic ISCI. A limitation of this study is the small sample size, which limits the generalizability of the findings. In addition, level of injury and use of mobility aids were not controlled. However, most of our subjects could not perform the tasks without aids. Furthermore, when the data were sorted by injury level (ie paraplegia versus tetraplegia), gait speed/capacity ranges were widely distributed across the two groups. In spite of the variability and small sample, analysis of the data has produced significant results and provided some new findings regarding the relationship between muscle strength and functional walking performance in persons with ISCI.
Our mean age of 41 of our population is well within the typical Canadian who currently has an SCI as the largest segment of Canadians with an SCI are currently between 35 and 49 years of age and this segment represents almost half of that population.21 Our sample did have a greater proportion of females (one-third) compared to the Canadian population, which has approximately one-fifth females.21 Although muscle strength was graded relative to movement against gravity, there are potential gender differences regarding the mechanisms of SCI injury and recovery of muscle function.
Unfortunately, we do not have any statistics available on the mass or bodymass index of Canadians currently with SCI (interesting study for the future though). There are statistics on mobility aids, but they are not specifically for the lesion level that we have in our study or for only incomplete injuries which also makes a large difference. However, we do have statistics on the age and gender of the average Canadian with an SCI.
Concurrent with previous findings,9,10,11 the results of this study indicate that lower extremity muscle strength scores are significantly associated with functional walking performance. Previous investigations,9,10,11 however, have only looked at composite strength scores such as the ASIA scores to evaluate the relationship between muscle strength and function. The present study extends those findings to include individual muscle groups and provides additional information regarding the contribution of each muscle to the performance of walking.
For gait speed and 6-min-walk distance, the strongest correlations were produced by the hip flexors and hip abductors on both sides. In fact, hip flexor strength of the less affected side alone explained more than 50% of the variance in gait speed and 6-min-walk distance. The hip flexors play an important role during the initial swing phase of gait to pull the swinging limb forward,22 and the hip abductors are important for stability during stance.23 It is possible that subjects with strong hip flexors and abductors were able to better control medio-lateral balance during stance and pull their swinging limb forward to increase stride length and consequently increase gait speed.
Similar muscle groups were related to both gait speed and 6-min-walk distance and, in addition, gait speed was very highly correlated with the 6-min-walk distance (r=0.98). These findings suggest that the simple measure of gait speed may be a sufficient measure and that the 6-min-walk distance does not provide any additional information regarding gait. Similar findings have been reported in persons with stroke where the correlation coefficient between gait speed and 6-min-walk distance was found to be as high as 0.92.24 However, Eng et al24 suggested that although the 6-min-walk distance may not provide different information from gait speed, monitoring the change in heart rate and blood pressure during the 6-min-walk test provided important information regarding an individual's myocardial exertion over the task. The change in hemodynamics may be a worthy measure to monitor during the 6-min-walk test in the future for individuals with SCI.
Interestingly, the muscles important for level walking (gait speed and endurance) were not always the same muscles important for ambulatory capacity, which may be more involved than the simple task of walking. The hip extensors were more important than the hip flexors in determining subjects’ level of ambulatory capacity suggesting that the stabilizing role of the hip extensors and abductors during loading is essential for a higher level of community mobility. The different key muscles could arise from the need for a community ambulator to perform a variety of mobility tasks. Tasks such as transfers, standing, and stairs, which are important activities for functioning in the community, have different strength demands from gait. The correlation between ambulatory capacity and gait speed or walking endurance was not high, which also suggested that other factors may influence the extent to which an individual uses walking to participate in the home and community. For a comprehensive evaluation of walking performance, the use of such classification system as the ambulatory capacity measure, in addition to the more commonly used measure of gait speed, may be useful.
For ambulatory capacity, the strongest correlations were produced by hip extensors and hip abductors, with the less affected hip extensor strength alone explaining 64% of the variance. Contrary to expectations, the knee extensor strength was not related to ambulatory capacity. Other studies8,12 have previously reported the knee extensor strength to be associated with ambulatory capacity. Both Crozier et al8 and Hussey and Stauffer12 found that a minimum of grade 3 knee extensor strength on the less affected side was required for community ambulation (ie able to walk in- and outdoors). Our subjects, however, had relatively high knee extensor strength with as many as 18 out of 22 achieving at least grade 3 strength even on their more affected side, which possibly accounts for the differences in findings across studies. That is, once anti-gravity knee extensor strength is achieved, an increase in knee extensor strength does not appear to further contribute to an increase in walking performance.
Contrary to expectation, the strength of the less affected limb, as opposed to that of the more affected limb, seems more important in determining the level of functional performance as revealed by the results of the correlation and regression analyses. More than 50% of the variance in all three functional measures could be explained by the strength of a single muscle group on the less affected side. These results suggest that persons with at least one strong limb are able to perhaps compensate for the weakness on the more affected side and thus demonstrate higher functional performance. Future clinical trials on the effects of strengthening the less affected limb on function would be beneficial in providing the clinician a focus of intervention during the rehabilitation of individuals with ISCI.
Given these results, we conclude that in persons with ISCI (1) proximal lower extremity muscle strength, in particular that of hip flexors, hip extensors, and hip abductors, is an important determinant of walking performance in persons living in the community, (2) hip flexor and hip extensor strength of the less affected side can significantly predict walking performance, (3) in general, the strength of the less affected lower limb is a more important determinant of function than that of the more affected side, and (4) for a comprehensive measure of walking performance, the use of such measures as the ambulatory capacity classification used in this study, in addition to the more commonly used gait speed measure, is advised. Readers are reminded, however, to be cautious when generalizing our results to other groups of persons with ISCI as our sample consisted of a group of mostly young (mean age 41 years) male subjects with chronic ISCI (on average 10 years post-injury) with generally good social support living in the community.
References
Krawetz P, Nance P . Gait analysis of spinal cord injured subjects: effects of injury level and spasticity. Arch Phys Med Rehabil 1996; 77: 635–638.
Waters RL, Yakura JS, Adkins RH . Gait performance after spinal cord injury. Clin Orthop 1993; 288: 87–96.
Lerner-Frankiel M, Vargus S, Brown M, Krusell L, Schoneberger W . Functional community ambulation: what are your criteria? Clin Manage Phys Ther 1986; 6: 12–15.
Frost FS . Role of rehabilitation after spinal cord injury. Urol Clin N Am 1993; 20: 549–559.
Perry J . Rehabilitation of the neurologically disabled patient: principles, practice, and scientific basis. J Neurosurg 1983; 58: 799–816.
Waters RL, Adkins RH, Yakura JS, Sie I . Motor and sensory recovery following incomplete tetraplegia. Arch Phys Med Rehabil 1994; 75: 306–311.
Waters RL, Adkins RH, Yakura JS, Sie I . Motor and sensory recovery following incomplete paraplegia. Arch Phys Med Rehabil 1994; 75: 67–72.
Crozier KS, Cheng LL, Graziani V, Zorn G, Herbison G, Ditunno Jr JF . Spinal cord injury: prognosis for ambulation based on quadriceps recovery. Paraplegia 1992; 30: 762–767.
Curt A, Dietz V . Ambulatory capacity in spinal cord injury: significance of somatosensory evoked potentials and ASIA protocol in predicting outcome. Arch Phys Med Rehabil 1997; 78: 39–43.
Waters RL, Yakura JS, Adkins R, Barnes G . Determinants of gait performance following spinal cord injury. Arch Phys Med Rehabil 1989; 70: 811–818.
Waters RL, Adkins R, Yakura J, Vigil D . Prediction of ambulatory performance based on motor scores derived from standards of the American Spinal Injury Association. Arch Phys Med Rehabil 1994; 75: 756–760.
Hussey RW, Stauffer ES . Spinal cord injury: requirements for ambulation. Arch Phys Med Rehabil 1973; 54: 544–547.
Maynard Jr FM et al. International standards for neurological and functional classification of spinal cord injury. Spinal Cord 1997; 35: 266–274.
Kendall FP, McCreary EK, Provance PG . Muscles: Testing and Function, 4th edn. Lippincott Williams & Wilkins: Baltimore 1993.
Herbison GJ, Isaac Z, Cohen ME, Ditunno Jr JF . Strength post-spinal cord injury: myometer vs manual muscle test. Spinal Cord 1996; 34: 543–548.
Frese E, Brown M, Norton BJ . Clinical reliability of manual muscle testing: middle trapezius and gluteus medius muscles. Phys Ther 1987; 67: 1072–1076.
Wadsworth CT, Krishnan R, Sear M, Harrold J, Nielsen DH . Intrarater reliability of manual muscle testing and hand-held dynametric muscle testing. Phys Ther 1987; 67: 1342–1347.
Guyatt GH et al. The 6-minute walk: a new measure of exercise capacity in patients with chronic heart failure. Can Med Assoc J 1985; 132: 919–923.
Perry J, Garrett M, Gronley JK, Mulroy SJ . Classification of walking handicap in the stroke population. Stroke 1995; 26: 982–989.
Munro BH, Visintainer MA, Page EB . Statistical Methods for Health Care Research. JB Lippincott Co: Philadelphia 1986, p 70.
Canadian Paraplegic Association. Workforce Participation Survey of Canadians with Spinal Cord Injuries. Canadian Paraplegic Association: Ottawa 1997.
Eng JJ, Winter DA . Kinetic analysis of the lower limb during walking: what information can be gained from a three-dimensional model? J Biomech 1995; 28: 753–758.
McKinnon CD, Winter DA . Control of whole body balance in the frontal plane during human walking. J Biomech 1993; 26: 633–644.
Eng JJ, Chu KS, Dawson AS, Kim CM, Hepburn KE . Functional walk tests in individuals with stroke: relationship to perceived exertion and myocardial exertion. Stroke 2002; 33: 756–761.
Acknowledgements
We wish to acknowledge grant funding from the Paralyzed Veterans of America Spinal Cord Research Foundation and the BC Neurotrauma Fund, in addition to career scientist awards to JJE from the Canadian Institute of Health Research and Michael Smith Foundation for Health Research.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kim, C., Eng, J. & Whittaker, M. Level walking and ambulatory capacity in persons with incomplete spinal cord injury: relationship with muscle strength. Spinal Cord 42, 156–162 (2004). https://doi.org/10.1038/sj.sc.3101569
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101569
Keywords
This article is cited by
-
The effects of virtual soccer game on balance, gait function, and kick speed in chronic incomplete spinal cord injury: a randomized controlled trial
Spinal Cord (2022)
-
Anodal transcutaneous DC stimulation enhances learning of dynamic balance control during walking in humans with spinal cord injury
Experimental Brain Research (2022)
-
Changes in cardiorespiratory fitness and activity levels over the first year after discharge in ambulatory persons with recent incomplete spinal cord injury
Spinal Cord (2021)
-
Validation of a clinical prediction rule for ambulation outcome after non-traumatic spinal cord injury
Spinal Cord (2020)
-
Quality of life and psychological outcomes of body-weight supported locomotor training in spinal cord injured persons with long-standing incomplete lesions
Spinal Cord (2020)