Abstract
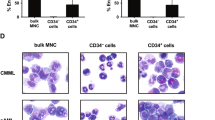
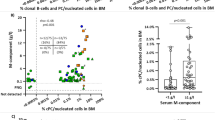
A quantitative analysis of expression levels of GM-CSF receptors was performed by flow cytometry in different disease categories, ie AML (n = 72), ALL (n = 18), and MDS (n = 12), as well as 12 healthy volunteers, using three different unconjugated GM-CSF/R monoclonal antibodies (McAbs) (HGM-CSFR (CD116), M5D12, 4B5F5), and appropriate standards. By using the reference HGM-CSFR McAb, in healthy subjects we found detectable levels of GM-CSF/R on blood monocytes (mean MESF (molecules of equivalent soluble fluorochrome)/cell: 36.1 × 103), neutrophils (mean MESF/cell: 7.4 × 103), bone marrow (BM) myelo-monocytic precursors (MESF range for the myeloid component, ie promyelocytes, myelocytes, metamyelocytes: 11.7–40.5 × 103, and for the monocytic lineage: 25.7–69.2 × 103), and in two distinct subsets of BM CD34+ progenitor cells (GM-CSF/R dim: 2.5 × 103 MESF/cell, GM-CSF/R bright (10% of the total number of CD34 cells: 22.0 × 103 MESF/cell). In these subjects, there was no correlation between the expression levels of GM-CSF/R and CFU (CFU-GM, CFU-GEMM, BFU-E) colony production. Among the AML samples, M5D12 McAb was positive in 33%, 4B5F5 McAb in 90%, and HGM-CSF/R McAb in 78% of the cases examined (range of MESF/cell for the HGM-CSFR McAb: 0.9 × 103–106.7 × 103). The highest MESF values were seen in the M5 FAB subvariety (mean: 39.4 × 103), where all the patients tested (n = 20) showed a strong positivity for the HGM-CSFR McAb. On the contrary, all ALL samples were GM-CSF/R negative except in two patients, who displayed a dim GM-CSF/R positivity (My+ALL: 1.3 × 103 MESF/cell; pro-B ALL: 1.0 × 103 MESF/cell). In most (>70%) M1 FAB subtypes, GM-CSF/R+ blasts co-expressed CD34low, HLA-DRhigh, CD33, CD38 antigens, and had little or no capacity to form CFU-GM colonies. GM-CSF/R+ blasts from the M5 FAB category were also positive for CD14, CD11c, CD33 and CD87. Furthermore, the number of GM-CSF/R expressed by leukemic cells from five out of 72 (7%) AML patients was above the highest values seen in normal samples (>69.2 × 103 MESF/cell), allowing the possibility of using this marker for the monitoring of the minimal residual disease (MRD) in a subset of AML. Cell culture studies aimed at evaluating GM-CSF receptor modulation following AML blast exposure to rhGM-CSF showed two distinct patterns of response; in the first group (6/10 cases) rhGM-CSF down-modulated GM-CSF receptors, whereas in the second group (4/10 cases), rhGM-CSF treatment was associated with either an increase or no change in the number of GM-CSF/R. In conclusion, cellular GM-CSF/R expression was variable and ranged from undetectable (ALL and a minority of AML) to very high intensities in M5 AML, and were also documented in some M0 AML, thus suggesting the concept that GM-CSF/R detection may be of help in lineage assignment of undifferentiated forms. Since the number of GM-CSF/R on AML blasts may be modulated after GM-CSF treatment, it can be postulated that the clinical use of GM-CSF in this disease may be optimized by a dynamic analysis of the number and the affinity status of GM-CSF-R in blasts and normal hemopoietic cells.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Lanza, F., Castagnari, B., Rigolin, G. et al. Flow cytometry measurement of GM-CSF receptors in acute leukemic blasts, and normal hemopoietic cells. Leukemia 11, 1700–1710 (1997). https://doi.org/10.1038/sj.leu.2400794
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2400794
Keywords
This article is cited by
-
Restoration of MYC-repressed targets mediates the negative effects of GM-CSF on RUNX1-ETO leukemogenicity
Leukemia (2017)
-
Dendritic cell phenotype can be improved by certain chemotherapies and is associated with alterations to p21waf1/cip1
Cancer Immunology, Immunotherapy (2013)