Abstract
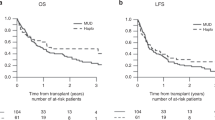
In a multicentre trial involving 20 transplant centres from 10 countries haematopoietic stem cells were obtained either from the bone marrow of 33 sibling donors or from the peripheral blood of 33 such donors after administration of filgrastim (10 μg/kg/day). The haematopoietic stem cells were infused into their HLA-identical recipients suffering from acute leukaemias in remission or chronic myeloid leukaemia in chronic phase. PBPC donors tolerated filgrastim administration and leukapheresis well with the most frequent side-effects being musculoskeletal pain, headache, and mild increases of LDH, AP, Gamma-GT or SGPT. Pain and haematoma at the harvest site and mild anaemia were the most frequent complaints of BM donors. Severe or life-threatening complications were not seen with any type of harvest procedure. Time to platelet recovery greater than 20 × 109/l was 15 days (95% confidence interval (CI) 13–16 days) in the PBPCT group and 19 days (CI 16–25) in the BMT group. Time to neutrophil recovery greater than 0.5 × 109/l was 14 days (CI 12–15 days) in the PBPCT group as compared to 15 days (CI 15–16 days) in the BMT group. The numbers of platelet transfusions administered to PBPCT and BMT patients were 12 (range: 1–28) and 10 (range: 3–39), respectively. Sixteen patients (48%) transplanted with bone marrow and 18 patients (54%) transplanted with PBPC developed acute GVHD of grades II–IV; acute GVHD of grades III or IV developed in six (18%) and seven (21%) patients, respectively. Kaplan–Meier plots for transplant-related mortality until day 100 and leukaemia-free survival at a median of 400 days after BMT or PBPCT showed no significant differences. Administration of filgrastim and leukapheresis in normal donors were feasible and well tolerated. The number of days with restricted activity and of nights spent in hospital was lower in donors of PBPC. Transplantation of PBPC to HLA-identical siblings with early leukaemia resulted in earlier platelet engraftment. The incidence of moderate to severe acute GVHD, transplant-related mortality, and leukaemia-free survival did not show striking differences. Further investigation of allogeneic PBPCT as a substitute for allogeneic BMT is warranted.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Schmitz, N., Bacigalupo, A., Hasenclever, D. et al. Allogeneic bone marrow transplantation vs filgrastim-mobilised peripheral blood progenitor cell transplantation in patients with early leukaemia: first results of a randomised multicentre trial of the European Group for Blood and Marrow Transplantation. Bone Marrow Transplant 21, 995–1003 (1998). https://doi.org/10.1038/sj.bmt.1701234
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701234
Keywords
This article is cited by
-
Short treatment of peripheral blood cells product with Fas ligand using closed automated cell processing system significantly reduces immune cell reactivity of the graft in vitro and in vivo
Bone Marrow Transplantation (2022)
-
Cytokine levels following allogeneic hematopoietic cell transplantation: a match-pair analysis of home care versus hospital care
International Journal of Hematology (2021)
-
High incidence of severe chronic GvHD after HSCT with sibling donors. A single center analysis
Bone Marrow Transplantation (2016)
-
The impact of CD34+ cell dose on engraftment after SCTs: personalized estimates based on mathematical modeling
Bone Marrow Transplantation (2014)
-
PBSC collection from family donors in Japan: a prospective survey
Bone Marrow Transplantation (2014)