Abstract
Objective:
To study the effect of the Lactobacillus plantarum (LP) enteral feeding on the gut permeability and sepsis in the patients with acute pancreatitis.
Subjects:
Seventy-six subjects who stayed over 1 week in the hospital completed the study. Subjects were not treated with any lactobacillus supplement before the intervention.
Methods:
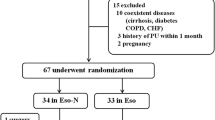
Seventy-six patients with acute pancreatitis were randomly divided into two groups, parenteral nutrition (PN) group (n=38) and ecoimmunonutrition (EIN) group supplied by LP enteral feeding (n=36). The acute physiology and chronic health evaluation score, Balthazar CT score, CRP, fecal bacterial species and DNA fingerprint profiles as well as the potentially pathologenic organisms in nasogastric aspirate were determined on the day of admission and on the 8 day. The intestinal permeability was assessed by measurement of the ratio of lactulose/rhamnose on the day of admission and on days 5 and 8. The rate of organ failure, septic complications and death cases were evaluated at the 8 day.
Results:
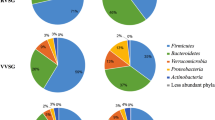
Following 7 days treatment, 38.9% patients in the EIN group were colonized with multiple organisms compared to 73.7% in the PN group (P<0.01), and 30.6% patients in the EIN grew potentially pathogenic organisms compared to 50% patients in PN group (P<0.05). The fecal bacterial DNA fingerprint profiles were less, the amount of lactobacteria and bifydobacteria decreased, and the amount of enterococci increased in PN group as compared with EIN group, P<0.05. By day 8, the lactulose/rhamnose ratio in EIN group were lower than that in PN group at days 5 and 8, P<0.05. The patients with LP got a better clinical outcomes as compared with the patients with PN.
Conclusion:
EIN enteral feeding can attenuate disease severity, improve the intestinal permeability and clinical outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Andersson R, Wang X, Sun Z, Deng X, Soltesz V, Ihse I (1998). Effect of a platelet-activating factor antagonist on pancreatitis-associated gut barrier dysfunction in rats. Pancreas 17, 107–119.
Baue AE (2006). MOF, MODS, and SIRS: what is in a name or an acronym? Shock 26, 438–449.
Bengmark S (2001). Pre-, pro and synbiotics? Curr Opin Clin Nutr Metab Care 4, 571–579.
Bengmark S (2002). Gut microbial ecology in critical illness: is there a role for prebiotics, probiotics and synbiotics? Curr Opin Crit Care 8, 145–151.
Blot F, Nitenberg G, Chachaty E, Raynard B, Germann N, Antoun S et al. (1999). Diagnosis of catheter-related bacteraemia: a prospective comparison of the time to positivity of hub-blood versus peripheral-blood cultures. Lancet 354, 1071–1077.
Bradley EL (1993). A fifteen-year experience with open drainage for infected pancreatic necrosis. Surg Gynecol Obstet 177, 215–222.
Branum G, Galloway J, Hirchowitz W, Fendley M, Hunter J (1998). Pancreatic necrosis: results of necrosectomy, packing, and ultimate closure over drains. Ann Surg 227, 870–877.
Collins MD, Glenn RG (1999). Probiotics, prebiotics and synbiotics: approaches for modulating the microbial ecology of the gut. Am J Clin Nutr 69 (Suppl), 1052–1057.
Foitzik T, Mithofer K, Ferraro MJ, Fernandez-del Castillo C, Lewandrowski KB, Rattner DW et al. (1994). Time course of bacterial infection of the pancreas and its relation to disease severity in a rodent model of acute necrotizing pancreatitis. Ann Surg 220, 193–198.
Foitzik T, Fernandez-del Castillo C, Ferraro MJ, Mithofer K, Rattner DW, Warshaw AL (1995). Pathogenesis and prevention of early pancreatic infection in experimental acute necrotizing pancreatitis. Ann Surg 222, 179–185.
Fuller R, Gibson GR (1997). Modification of the intestinal microflora using probiotics and prebiotics. Scand J Gastroenterol 222 (Suppl), S28–S31.
Gill HS, Rutherfurd KJ, Cross ML, Gopal PK (2001). Enhancement of immunity in the elderly by dietary supplementation with the probiotic bifidobacterium lactis HN019. Am J Clin Nutr 74, 833–839.
Gill HS, Rutherfurd KJ, Cross ML, Gopal PK (2001). Enhancement of immunity in the elderly by dietary supplementation with the probiotic bifidobacterium lactis HN019. Am J Clin Nutr 74, 833–889.
Gluck U, Olaf Gebbers J (2003). Ingested probiotics reduce nasal colonization with pathogenic bacteria (staphylococcus aureus, streptococcus pneumoniae, and β-hemolytic streptococci). Am J Clin Nutr 77, 517–520.
Harris CE, Griffiths RD, Freestone N, Billington D, Atherton ST, Macmillan RR (1992). Intestinal permeability in the critically ill. Intensive Care Med 18, 38–41.
Isolauri E (2001). Probiotics in human disease. Am J Clin Nutr 73 (Suppl), S1142–S1146.
Kazantsev GB, Hecht DW, Rao R, Fedorak IJ, Gattuso P, Thompson K et al. (1994). Plasmid labeling confirms bacterial translocation in pancreatitis. Am J Surg 167, 201–206.
Kolida S, Tuohy K, Gibson GR (2002). Prebiotic effect of inulin and oligofructose. Br J Nutr 87 (Suppl), S193–S197.
Marshall JC, Christou NV, Horn R, Meakins JL (1988). The microbiology of multiple organ failure. The proximal gastrointestinal tract as an occult reservoir of pathogens. Arch Surg 123, 309–315.
Marshall JC (1993). The gastrointestinal tract: the ‘undrained abscess’ of multiple organ failure. Ann Surg 218, 111–119.
Marshall JC, Cook DJ, Christou NV (1995). Multiple organ dysfunction score: a reliable descriptor of a complex clinical outcome. Crit Care Med 23, 1638–1652.
McNaught CE, Woodcock NP, Anderson ADG, MacFie J (2005). A prospective randomised trial of probiotics in critically ill patients. Clin Nutr 24, 211–219.
Meier R, Ockenga J, Pertkiewicz M, Pap A, Milinic N, Macfie J et al. (2006). ESPEN guidelines on enteral nutrition: pancreas. Clin Nutr 25, 375–384.
Miller BJ, Henderson A, Strong RW, Fielding GA, DiMarco AM, O'Loughlin BS (1994). Necrotizing pancreatitis: operating for life. World J Surg 8, 906–911.
Olah A, Belagyi T, Issekutz A, Gamal ME, Bengmark S (2002). Randomized clinical trial of specific lactobacillus and fibre supplement to early enteral nutrition in patients with acute pancreatitis. Br J Surg 89, 1103–1107.
Osman NE, Westrom B, Karlsson B (1998). Serosal but not mucosal endotoxin exposure increases intestinal permeability in vitro in the rat. Scand J Gastroenterol 33, 1170–1174.
Pastor CM, Matthay MA, Frossard JL (2003). Pancreatitis-associated acute lung injury. Chest 124, 2341–2351.
Perdigon G, Vintini E, Alvarez S, Medina M, Medici M (1999). Study of the possible mechanisms involved in the mucosal immune system activation by lactic acid bacteria. J Dairy Sci 82, 1108–1114.
Qin HL, Shen TY, Gao ZG, Fan XB, Hang XM, Jiang YQ et al. (2005). Effect of lactobacillus on the gut microflora and barrier function of the rats with abdominal infection. World J Gastroenterol 11, 2591–2596.
Rayes N, Hansen S, Seehofer D, Muller AR, Serke S, Bengmark S et al. (2002a). Early enteral supply of fiber and Lactobacilli versus conventional nutrition: a controlled trial in patients with major abdominal surgery. Nutrition 18, 609–615.
Rayes N, Seehofer D, Hansen S, Boucsein K, Muller AR, Serke S et al. (2002b). Early enteral supply of lactobacillus and fiber versus selective bowel decontamination: a controlled trial in liver transplant recipients. Transplantation 74, 123–127.
Reid G, Charbonneau D, Erb J, Kochanowski B, Beurerman D, Poehner R et al. (2003). Oral use of lactobacillus rhamnosus GR-1 and L. fermentum RC-14 significantly alters vaginal flora: randomized, placebo-controlled trial in 64 healthy women. FEMS Immunol Med Microbiol 35, 131–134.
Acknowledgements
This work was supported by the Natural Science Foundation of Shanghai Goverment, No.200401.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantor: HL Qin.
Contributors: HLQ designed the study, wrote the original manuscript and edited all subsequent versions. JJZ and DND carried out the study, were responsible for data coding, sample analyses and stastical analyses. WXC was responsible for the screening and intervention of subjects. XBF and XMH were responsible for the fecal bacterial DNA fingerprint analyses. YQJ was responsible for the bacterial culture.
Rights and permissions
About this article
Cite this article
Qin, HL., Zheng, JJ., Tong, DN. et al. Effect of Lactobacillus plantarum enteral feeding on the gut permeability and septic complications in the patients with acute pancreatitis. Eur J Clin Nutr 62, 923–930 (2008). https://doi.org/10.1038/sj.ejcn.1602792
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602792
Keywords
This article is cited by
-
Effect of enteral ecoimmunonutrition support for patients undergoing hepatectomy: A meta-analysis of randomized controlled trials
European Journal of Clinical Nutrition (2022)
-
Gastrointestinal microecology: a crucial and potential target in acute pancreatitis
Apoptosis (2018)
-
Pre‐surgical Administration of Microbial Cell Preparation in Colorectal Cancer Patients: A Randomized Controlled Trial
World Journal of Surgery (2016)
-
Bugs or Drugs: Are Probiotics Safe for Use in the Critically Ill?
Current Gastroenterology Reports (2014)
-
The use of probiotics in the surgical patient
European Surgery (2012)