Abstract
Repetitive transcranial magnetic stimulation (rTMS) is increasingly used as a therapeutic tool in various neurological and psychiatric disorders, and we recently found that it has a neuroprotective effect both in vitro and in vivo. However, the neurochemical mechanisms underlying the therapeutic effects are still unknown. We investigated the effects of long-term rTMS on the expression of brain-derived neurotrophic factor (BDNF), cholecystokinin (CCK), and neuropeptide tyrosine (NPY) mRNA in rat brain. In situ hybridization revealed a significant increase in BDNF mRNA in the hippocampal areas CA3 and CA3c, the granule cell layer, as well as in the parietal and the piriform cortex after rTMS. BDNF-like immunoreactivity was markedly increased in the same areas. A significant increase in CCK mRNA was observed in all brain regions examined. NPY mRNA expression, in contrast, was not altered. The present results suggest that BDNF may contribute to the neuroprotective effects of rTMS. Furthermore, the rTMS-induced changes in BDNF and CCK expression are similar to those reported after antidepressant drug treatment and electroconvulsive seizures, suggesting that a common molecular mechanism may underlie different antidepressant treatment strategies.
Similar content being viewed by others
Main
Transcranial magnetic stimulation (TMS), a technique in which a time-varying strong electric current is applied through a coil held in direct contact with the subject's head, was originally developed for diagnostic use in neurology (for review see Rossini and Rossi 1998). A possible effect of TMS on mood was first reported in 1987 (Bickford et al. 1987) and, although discussed controversially, to date several lines of evidence resulting from both preclinical (Fleischmann et al. 1995; Zyss et al. 1997) and clinical (e.g., Pascual-Leone et al. 1996) studies support the notion that repetitive TMS (rTMS) may have antidepressant properties: rTMS induces transient enhancement of mood in healthy subjects, and daily application alleviates symptoms in patients suffering from treatment-resistant major depression (for review see George et al. 1999).
Although rTMS is currently being evaluated as a possible alternative or add-on therapy in the treatment of refractory depression, knowledge concerning its effects at the molecular and cellular level is still very limited. Recently, Ji et al. (1998) reported a specific activation of brain regions in terms of immediate early gene expression in rats in response to rTMS. In addition, we provided a first evidence for a neuroprotective effect of long-term rTMS in vivo and in vitro (Post et al. 1999). The in vitro studies showed that magnetic stimulation analogous to TMS increased the overall viability of mouse monoclonal hippocampal HT22 cells and had a neuroprotective effect against oxidative stressors such as amyloid beta (Aβ) and glutamate. Moreover, the treatment increased the release of the potentially neuroprotective secreted amyloid precursor protein (sAPP) into the supernatant of HT22 cells and into cerebrospinal fluid from rats. Accordingly, HT22 cells preincubated with cerebrospinal fluid from long-term rTMS-treated rats were found to be protected against Aβ (Post et al. 1999). However, the neurochemical mechanisms underlying these neuroprotective properties as well as the putative therapeutic effects of rTMS in neurological and psychiatric disorders still remain to be elucidated.
Brain-derived neurotrophic factor (BDNF) is a member of the neurotrophin family and is abundantly expressed in the adult brain. The neurotrophic and also neuroprotective effects of BDNF have been characterized extensively both in vitro and in vivo. In addition, upregulation of BDNF has been implicated in neuronal responses to various kinds of injuries, such as epileptic seizures, cerebral ischemia, and hypoglycemia (for review see Connor and Dragunow 1998). Recent work raised the possibility that one of the many long-term effects of antidepressant treatment may be regulation of neurotrophins: antidepressant drug treatment and electroconvulsive seizures (ECS) were shown to markedly induce BDNF expression in selected areas of rat brain (Altar 1999; Nibuya et al. 1995; Zetterström et al. 1998).
Both repeated ECS and treatment with different antidepressant drugs have been reported to significantly alter cholecystokinin (CCK) (Brodin et al. 1989, 1994; Lindefors et al. 1991; Orzi et al. 1990) and neuropeptide tyrosine (NPY) expression in selected brain regions. CCK is the most abundant neuropeptide in the mammalian brain, and its anatomical distribution, with high levels of expression in the cerebral cortex, the amygdala, the hippocampus and the septum strongly suggests that it is one of the modulators of emotionality (for review see Moran and Schwartz 1994). CCK is co-localized with dopamine in a large proportion of the neurons in the mesolimbic system (for review see Crawley and Corwin 1994). These CCK-containing dopaminergic pathways have been implicated in the pathophysiology of human affective disorders and Parkinson's disease, and in both of these disease states rTMS has been suggested to exert beneficial effects (Pascual-Leone and Catala 1995; Pascual-Leone et al. 1994; Siebner et al. 1999).
In patients with major depression, decreased cerebrospinal fluid levels of NPY (Gjerris et al. 1992) and a decreased NPY-like immunoreactivity in specific brain areas (Widdowson et al. 1992) have been reported, giving rise to the hypothesis of a NPYergic deficit in depression (for review see Heilig and Widerlov 1995). Consistent with this hypothesis, an increase in NPY expression in frontal cortical brain areas and in the hippocampus after chronic ECS application (Wahlestedt et al. 1990; Mikkelsen et al. 1994) and antidepressant drug treatment (Heilig et al. 1988) has been demonstrated in several animal studies.
We conducted the present study to investigate the effects of long-term rTMS treatment performed under conditions comparable to those in clinical use to further elucidate the mechanisms underlying the recently discovered neuroprotective effects of this technique. In addition, we wanted to test the hypothesis that the molecular and cellular effects of chronic rTMS are similar to those observed following other forms of antidepressant therapy, namely drug treatment and ECS. Therefore, we examined the effects of rTMS on the expression of both BDNF mRNA and protein as well as of the neuroactive peptides CCK and NPY mRNA in distinct areas of the rat brain.
MATERIALS AND METHODS
Animals
The animal studies were conducted in accordance with the Guide for the Care and Use of Laboratory Animals of the Government of Bavaria, Germany. Experiments were performed on young, conscious, male Wistar rats from the age of four weeks (50 ± 8 g body weight at the beginning of the study; n = five per group). Rats were housed in groups of six in the breeding unit under standard laboratory conditions (12:12 h light/dark cycle with lights on at 0700 h, 22 ± 1°C, 60% humidity, pelleted food and water ad libitum).
Repetitive Transcranial Magnetic Stimulation
A commercially available stimulator (MagPro™; DANTEC, Skovlunde, Denmark) was used for TMS. The stimulus waveform was biphasic and had a pulse width of 280 μs. The temperature of the stimulation coil (°C) and the stimulus intensity (A/μs) were monitored from a digital display. A round prototype coil was selected (S60, DANTEC; inner diameter: 6 mm; outer diameter: 57 mm; 21 windings). The initial current direction was clockwise. Trains were separated by 2-min intervals to allow for cooling of the stimulation coil. The animals were treated with 150 stimuli/day resulting from three trains at a rate of 20 Hz for 2.5 s (4 Tesla, 120 A/μs; 130% of rats’ motor threshold). These handled, conscious rats were treated in 5-day series separated by 2-day intervals for 11 weeks and cooperated well with the procedure (n = 5).
Due to direct muscular activation, animals of the rTMS treatment group experienced a slight tremor of the head during stimulation. A similarly aversive stimulus for the control rats was achieved by stimulation of the low lumbar spine region (n = 5). In a pilot study unrestrained, non-handled, adult rats that were subjected to the same rTMS protocol as in the present study showed clear unspecific stress responses, as evidenced, for instance, by consecutive locomotor hyperactivity and aggressive behavior. Therefore, to avoid unspecific stress due to rTMS, rats were allowed to adapt to the rTMS artifact noise beginning at the age of 3 weeks and were subjected to daily rTMS treatment from the age of 4 weeks on.
After one week of daily handling and chronic rTMS, animals adapted well to the procedure, as indicated by the fact that restraint of the rats was unnecessary. The stimulation coil was held in direct physical contact with the animal's head at the stimulation point. To mimic clinical conditions (e.g., Pascual-Leone et al. 1996), the stimulation point was set at the left frontal cortex. As a key part of the study, a series of computer-assisted, MRI-based reconstructions of the current density distributions induced by rTMS in the rat and human brain were performed as has been described previously (Cerri et al. 1995). As the total number of stimuli applied is currently considered to be a crucial point for the clinical effectiveness of rTMS treatment (George et al. 1999), animals received a total of 8250 stimuli what is in the range of clinical studies, e.g., George et al. (1997): 8000 pulses, and Pascual-Leone et al. (1996): 10000 pulses.
Motor Threshold
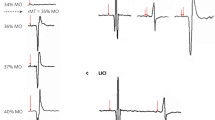
Motor threshold was determined as previously described (Jennum and Klitgaard 1996). Briefly, a standard electromyographic (EMG) machine was used (DANTEC). Sampling frequency was 51.4 kHz, high and low pass filter settings were 10 and 3000 Hz. The muscle activity was recorded by the use of a 0.5 mm bipolar EMG needle (DANTEC) placed in the right hindlimb biceps femoris muscle with a ground electrode 10 mm proximal to the recording electrode. The inter-electrode impedances were less than 3.5 kOhms.
The motor threshold was defined as a reproducible motor evoked potential in five consecutive stimuli with an interstimulus interval > 3s and an amplitude > 50 μV. This study was performed in five rats separately. Rats were investigated under propofol anesthesia as this anesthetic is well known not to interfere with motor evoked potentials either in humans (Kalkman et al. 1992) or in rats (Fishback et al. 1995).
In Situ Hybridization
Animals were killed with an overdose of halothane at the end of the experiments, i.e., 11 weeks after rTMS or sham treatment and 20 h after the last application of rTMS. Thereafter, brains were quickly removed. In all animals, the pituitary and internal organs were visually examined to exclude animals with tumors from the statistical analysis. Brain tissue was frozen in prechilled n-methylbutane on dry ice and stored at −80°C. For subsequent in situ hybridization experiments, brains (rTMS: n = 5; controls: n = 5) were sectioned in a cryostat. All brains were cut in five parallel series (20 μm, coronal sections), with every fifth section being thaw-mounted on the same glass slide. Sections were stored at −20°C until use.
The following oligonucleotide DNA probes were used for in situ hybridization.
CCK(44-mer): 5′-ATCCATCCAGCCCATGTAGTCCCGGTCACTTATCCTGTGGCTAG-3′ according to nucleotides 351–395 of whole rat prepro-cholecystokinin cDNA (Deschenes et al. 1984); BDNF (50-mer): 5′-AGTTCCAGTGCCTTTTGTCTATGCCCCTGCAGCCTTCCTTCGTGTAACCC-3′ according to nucleotides 645–694 of whole rat cDNA (Maisonpierre et al. 1991); and NPY(48-mer) : 5′-ATGAGATGTGGGGGGAAACTAGGAAAAGTCAGGAGAGCAAGTTTCATT-3′ according to nucleotides 3148–3195 of rat NPY sequence (Larhammar et al. 1987).
The specificity of these oligonucleotides has been described in detail elsewhere (Kononen et al. 1995; Schalling et al. 1990). All in situ hybridization experiments were carried out as previously described in detail (Kresse et al. 1995), and all sections were run in the same experiment under identical conditions. Briefly, the synthesized oligonucleotides were labeled at the 3′ end with α-[35S]-dATP (NEN, DuPont, Boston, MA) using terminal dexoynucleotidyl transferase (Boehringer Mannheim, Mannheim, Germany). Radiolabeled probe (106 cpm / 200 μl / slide) was diluted into hybridization buffer consisting of 1 × Denhardt's solution, 0.25 mg/ml yeast tRNA (Sigma, Deisenhofen, Germany), 0.5mg/ml salmon sperm DNA (Sigma), 10% dextran sulfate, 10 mM dithiothreitol and 50% formamide, applied to the slides and incubated for 20 h at 42°C. Following hybridization, the slides were washed in 1 × SSC (55°C), four times for 15 min each, dehydrated in ethanol and air-dried. Finally, the slides were dipped in Kodak NTB2 emulsion diluted 1:1 in distilled water, exposed for five weeks at 4°C and then developed in Kodak D19 solution. The developed slides were lightly counterstained with cresyl violet and examined using a Leica microscope with both bright- and dark-field condensors.
Immunohistochemistry
Serial 20-μm frozen sections were mounted on coated glass slides and stored at −20°C. Tissue was postfixed in absolute acetone for 10 min and air-dried. After blocking of endogenous peroxidase in absolute methanol with 0.01% hydrogen peroxide for 15 min, the sections were transferred to phophate-buffered saline (PBS, pH 7.45). PBS was also used for subsequent washes, and all reagents for immunohistochemistry were diluted in PBS with 1% bovine serum albumin (BSA) unless otherwise specified. After preincubation with 5% normal goat serum for 2 h, incubation with the primary antibody diluted 1:300 (polyclonal rabbit-anti-BDNF antibody [N-20]; Santa Cruz Biotechnology, Santa Cruz, CA) was performed at 4°C overnight. The specificity of this antibody has been tested by the manufacturer.
The sections were then incubated with a biotinylated goat-anti-rabbit secondary antibody diluted 1:300 for one hour at room temperature (Vector, Burlingame, CA, USA). This was followed by incubation with avidin biotinylated horseradish peroxidase complex (ABCelite universal kit; Vector) for 45 min at room temperature (1:300). All steps were followed by appropriate washes in PBS. Finally, the sections were developed in a substrate solution of 0.05% diaminobenzidine tetrahydrochloride and 0.01% hydrogen peroxide in 0.05 M Tris-HCl, pH 7.6, washed, lightly counterstained with hematoxylin and mounted. Appropriate negative controls were performed by omission of the primary antibody.
Optical Densitometry
Representative areas of the different brain regions (hippocampal pyramidal cell layer: areas CA1, CA2, CA3, and CA3c [hilus]; granule neurons of the dentate gyrus; parietal cortex; and piriform cortex) were scanned by a digital camera under dark-light conditions. In case of NPY mRNA, the analysis was performed in the area of the hippocampal dentate gyrus/CA3c and the parietal cortex. Care was taken to scan all images under identical light conditions. Levels of mRNA expression were determined by measuring the mean gray value (BDNF and CCK mRNA) or on inverted black-white images (in situ hybridization signal: black) in the region of interest and blind to the treatment conditions on a Macintosh computer using the Macintosh-based public domain image analysis program NIH Image, version 1.6.1. (developed at the US National Institutes of Health and available on the Internet at http://rsb.info.nih.gov/nih-image). As neurons expressing NPY mRNA were scattered throughout the cortex and hippocampal formation, quantitative analysis of NPY mRNA expression was performed as an automatic count of labeled objects (= cells) per mm2 of the parietal cortex and the total region of the dentate gyrus and hilus (CA3c) on automatically thresholded images. In all cases, at least four parallel tissue sections per animal and region were analyzed, and the mean values for each animal and region were calculated.
Statistical Analysis
Statistical analysis was performed using Kruskal-Wallis ANOVA to examine for significant overall group differences. In cases were significant group differences were detected, pairwise comparisons using the Mann-Whitney U-test followed (statistical software: GB Stat™, version 6.5 PPC; Dynamic Microsystems Inc., Silver Spring, MD). As the level of significance p <.05 was accepted.
RESULTS
Long-Term rTMS Increases the Expression of BDNF mRNA in Specific Areas of Rat Brain
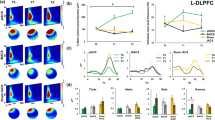
The mean values of BDNF optical density for each region and group + SEM are given in Figure 1. Significant differences between rTMS- and sham-treated animals were found in areas CA3 (rTMS: 48.4 ± 3.8, sham: 36 ± 5, p < .05); and CA3c (hilus) (rTMS: 31.5 ± 3.7, sham: 25.7 ± 3.5, p < .05) of the pyramidal cell layer, the granule cell layer of the dentate gyrus (rTMS: 43.4 ± 3.2, sham: 28 ± 1.6, p < .01) (Figure 2), the parietal cortex (rTMS: 21.2 ± 3.3, sham: 14.1 ± 1, p < .01) (Figure 2), and the piriform cortex (rTMS: 54.2 ± 3.1, sham: 32.3 ± 2.3, p < .01) (Figure 2).
Long-term rTMS increases the expression of BDNF mRNA in specific regions of rat brain. Results of in situ hybridization analysis using an α-[35S]-dATP-labeled oligonucleotide probe are shown. Representative coronal sections of sham-treated (A, C, E, G) and long-term rTMS-treated (B, D, F, H) rat brain. Darkfield photomicrographs reveal a marked rTMS-induced increase in BDNF mRNA expression in hippocampal areas CA3c (CA3c; A, B), the granule cell layer of the dentate gyrus (D, G, A, B), the parietal cortex (C, D), and the piriform cortex (E, F). In contrast, no increase in BDNF mRNA expression can be observed in the CA1 area of the hippocampal pyramidal cell layer (G, H).
No significant difference in BDNF mRNA expression between rTMS and sham-treated animals was detected in the areas CA1 (Figure 2) and CA2 of the hippocampal pyramidal cell layer (rTMS: 46.3 ± 5.8, sham: 39.9 ± 3.9, p = .083 and rTMS: 44.7 ± 5.5, sham: 38.6 ± 6.7, p = .15, respectively).
Long-Term rTMS Increases BDNF-Like Immunoreactivity in Regions of Enhanced BDNF mRNA Expression
In rTMS-treated animals, a marked increase in BDNF-like immunoreactivity was observed in the parietal and piriform cortex (Figure 3). Besides the strong increase in cytoplasmatic BDNF-like immunoreactivity of cortical neurons, several neurons displayed a prominent staining of cell membranes and dendritic processes, something that was not observed in any of the sham-treated animals. In addition, rTMS induced a marked increase in granular-like immunoreactivity in the supragranular zone of the dentate gyrus and an increase in cytoplasmic BDNF-like immunoreactivity in the neurons of the granule cell layer (Figure 3). In the CA3 area, many intensely stained large immunoreactive granules were observed in the stratum lucidum, the terminal zone of the mossy fibers on the proximal dendrites of the CA3 pyramidal neurons (Figure 3).
Long-term rTMS increases BDNF-like immunoreactivity in the areas of increased mRNA expression. Photomicrographs of representative immunostained sections of sham-treated (A, B, C, D) and rTMS-treated (E, F, G, H) animals show a strong increase in BDNF-like immunoreactivity in the stratum lucidum of the CA3 pyramidal region (A, E). Many large immunoreactive granules can be observed (arrows). BDNF-like immunoreactivity is increased in the granule neurons of the dentate gyrus (B, F) and the adjacent supragranular layer (arrows). In the parietal cortex (C, G), rTMS treatment induces not only an increase in cytoplasmatic immunoreactivity, but also a prominent staining of cell membranes and dendritic processes (arrows). Long-term rTMS markedly increases BNDF-like immunoreactivity in the piriform cortex (D, H). Scale bars: 80 μm (A, E, C, G, D, H) and 40 μm (B, F).
Long-Term rTMS Induces a Significant Increase in CCK mRNA Expression
The mean values of CCK optical density for each region and group + SEM are presented in Figure 4. Significant differences between rTMS- and sham-treated animals were found throughout the different areas of the pyramidal cell layer, namely CA1 (rTMS: 143 ± 16.4, sham: 107.4 ± 18.2, p < .05); CA2 (rTMS: 52.9 ± 10.1, sham: 30.7 ± 5.3, p < .01); CA3 (rTMS: 73.2 ± 11.3, sham: 51.9 ± 10.4, p < .05); and CA3c (rTMS: 56.9 ± 11.5, sham: 33.2 ± 5.7, p < .01). In addition, there were significant differences between the rTMS- and sham-treated groups in layer II/III of the parietal cortex (rTMS: 47.3 ± 8.0, sham: 35.4 ± 2.8; p < .05); in layer V/VI of the parietal cortex (rTMS: 60.9 ± 5.1, sham: 45.6 ± 4.7, p < .05); and in the piriform cortex (rTMS: 72.7 ± 4.1, sham: 52.1 ± 8.8, p < .01).
NPY mRNA Expression in the Parietal Cortex and Dentate Gyrus is Not Affected by Long-Term rTMS
The mean numbers of NPY mRNA expressing neurons in the parietal cortex (per mm2) and dentate gyrus/CA3c (counted over the total area of the dentate gyrus and hilus region) for each group + SEM are presented in Figure 5. The numbers of NPY mRNA expressing cells did not differ between the groups in either the parietal cortex (rTMS: 7.5 ± 2.5, sham: 7.25 ± 1.25) or the area of the dentate gyrus/CA3c region (rTMS: 17.65 ± 4.85, sham: 20.71 ± 3.29).
Long-term rTMS does not influence the expression of NPY mRNA in cortical and hippocampal areas. Results of in situ hybridization analysis using an α-[35S]-dATP-labeled oligonucleotide probe are shown. Scanned autoradiographs of representative coronal sections of sham-treated (A) and long-term rTMS-treated (B) rat brain. NPY mRNA expressing cells are scattered throughout the cortex and the hippocampal dentate gyrus. No significant differences in the number of NPY mRNA expressing neurons can be observed between sham-treated and long-term rTMS treated animals (C) in either the dentate gyrus (DG) or the parietal cortex (PCtx). n.s., non significant.
DISCUSSION
The present study was performed to investigate the effects of long-term rTMS on the expression of BDNF and the neuropeptides CCK and NPY in rat brain. In spite of the broad clinical use of this technique, the interactions between the magnetic stimuli applied and central nervous system neurons are only poorly understood.
Neuroprotective Effects of rTMS May Be Mediated Via Regulation of BDNF
Recently, first evidence was provided for a neuroprotective effect of rTMS against oxidative cell damage both in vitro and in vivo (Post et al. 1999). The present study demonstrates that long-term rTMS significantly increases the expression of BDNF mRNA and protein in specific areas of the hippocampal formation and cerebral cortex. BDNF belongs to the family of neurotrophins that are characterized by their ability to regulate diverse neuronal responses, including the type and number of afferent synapses, by promoting the survival of discrete neuronal subpopulations (for review see Connor and Dragunow 1998).
Pretreatment of rat cortical and cerebellar cultures with recombinant BDNF has been reported to significantly reduce glutamate-induced neuronal damage (Lindholm et al. 1993; Shimohama et al. 1993). Furthermore, a significant reduction in BNDF mRNA expression was found in the hippocampi of patients afflicted with Alzheimer's disease when compared to age-matched controls, and it was postulated that this decrease might contribute to the progression of neuronal degeneration (Phillips et al. 1991). To date, several findings from both in vitro and in vivo experiments support the proposal that neurotrophic factors might help in the treatment of neurodegenerative disorders by protecting against neuronal cell loss and by increasing the function of surviving neuronal populations (Conner et al. 1997). It therefore seems possible that BDNF could act as a mediator of the neuroprotective effects of rTMS against oxidative cell damage.
Chronic rTMS Treatment Increases BDNF Expression in Specific Areas of Rat Brain: Do Different Antidepressant Treatments Have Similar Effects at the Molecular Level?
Several lines of evidence indicate that BDNF may be involved in the cellular response to different antidepressant treatment strategies (Altar 1999; Duman et al. 1997). Chronic ECS increases and prolongs the expression of BDNF and its receptor, trkB, in selected areas of rat brain, such as the granule cell layer of the dentate gyrus and the piriform cortex, as do various antidepressant drugs, but not other non-antidepressant psychotropic agents (Nibuya et al. 1995; Smith et al. 1997; Zetterström et al. 1998). In addition, local infusion of high concentrations of BDNF into the midbrain has been reported to exert antidepressant effects in behavioral animal models of depression (Siuciak et al. 1997).
Many antidepressant drugs acutely increase monoamine levels, but the requirement for repeated, chronic administration together with the delayed onset of antidepressant efficacy strongly suggests that long-term adaptive processes are necessary for the therapeutic actions of these treatments. The antidepressant-induced increase in BDNF could result from adaptations of intracellular pathways, and the upregulation of the cyclic AMP response element binding protein (CREB) cascade by chronic antidepressant drug treatment that has been reported (Nibuya et al. 1996; Takahashi et al. 1999) may be the underlying mechanism. CREB has been shown to be an important regulator of BDNF-induced gene expression (Finkbeiner et al. 1997).
The present study shows a significant increase in BDNF mRNA in specific areas of rat brain after chronic rTMS treatment under stimulation conditions comparable to those in clinical use. This increase in BDNF mRNA was detected in areas CA3 and CA3c of the hippocampal pyramidal cell layer, in the granule cell layer and in the parietal and piriform cortex. Our immunohistochemical analysis confirmed these results at the protein level. A strong and granular BDNF-like immmunoreactivity was observed in both the supragranular layer of the dentate gyrus and the stratum lucidum of the CA3 pyramidal area, where the mossy fibers form giant en passant synapses, the characteristic mossy terminals, on the proximal dendrites of the CA3 pyramidal neurons (Freund and Buzsáki 1996). The granule neurons of the dentate gyrus are the target for the majority of entorhinal afferents, and therefore an increase in BDNF expression in these neurons and in their projection sites probably reflects an rTMS-induced stimulation of synaptic activity and input into the hippocampal formation (Schuman 1999). It is noteworthy that after long-term rTMS, BDNF mRNA and protein expression are increased in exactly the same anatomical areas as observed after ECS and antidepressant drug treatment (Nibuya et al. 1995; Zetterström et al. 1998), suggesting that different antidepressant treatments may have similar effects at the molecular and cellular level.
Besides its well-characterized neurotrophic properties, BDNF has also been implicated in neuronal responses to various kinds of injuries: limbic seizures induced by electrolytic lesion or kainic acid strongly increase BDNF mRNA in adult hippocampus and cortex (for review see Castrén et al. 1998). Furthermore, ischemia induces BDNF expression in brain regions outside the ischemic area (Kokaia et al. 1995). Changes in BDNF expression may therefore also reflect secondary events induced by damage to or degeneration of specific neuronal populations. So far, the functional consequences of this increased expression of neurotrophic factors after brain insults are still unclear. However, numerous experimental findings support the hypothesis that the neurotrophic factor response constitutes an intrinsic neuroprotective mechanism.
Therefore, the question arises of whether the increase in BDNF induced by administration of antidepressant drugs, ECS and (as observed in the present investigation) rTMS reflects the ability of these treatments to restore the postulated depression-associated neuronal atrophy (Duman et al. 1997) by stimulating neurotrophin expression, or whether BDNF enhancement reflects a cellular response indicative of neuronal damage or toxicity. In conflict with the latter notion is our previous finding that long-term rTMS did not reduce neuronal viability, but instead actually counteracted the detrimental effects of oxidative stress in hippocampal neurons (Post et al. 1999).
rTMS Differentially Affects the Expression of the Modulatory Neuropeptides CCK and NPY
CCK is the most abundant peptide in the mammalian brain, and it has been found to be co-localized with several neurotransmitters, such as serotonin (van der Kooy et al. 1981), gamma-aminobutyric acid (GABA) (Somogyi et al. 1984), and dopamine (Hökfelt et al. 1980). CCK, acting as a neuromodulator, increases the firing rate of dopaminergic ventral tegmental and substantia nigra neurons, and the ability of CCK to directly affect local dopamine release has been examined in numerous experiments (for review see Crawley and Corwin 1994; Moran and Schwartz 1994).
It has been suggested that the mesolimbic dopamine-containing neurons may be involved in the pathophysiology of depressive disorders and may be a substrate for the therapeutic action of antidepressant drugs (Fibiger 1995), and several lines of evidence indicate that an enhancement of monoamine-mediated neurotransmission accompanies the therapeutic effects of most antidepressant treatments (for review see Blier and de Montigny 1994; Holsboer 1995). rTMS has been suggested to exert therapeutic effects in several different neurological and psychiatric syndromes associated with an altered dopaminergic neurotransmission (Holsboer 1995), e.g., depression, mania, catatonia, and Parkinson's disease (Grisaru et al. 1998a,b; Pascual-Leone and Catala 1995; Pascual-Leone et al. 1994, 1996; Siebner et al. 1999), thus suggesting that it might induce an activation of monoaminergic neuronal pathways. Indeed, electrical stimulation of the medial prefrontal cortex has been reported to increase both CCK and dopamine release in the nucleus accumbens (You et al. 1998). Significant increases in CCK mRNA expression and CCK-like immunoreactivity in different neuroanatomical regions have also been observed after ECS and treatment with antidepressant drugs (Brodin et al. 1989, 1994; Lindefors et al. 1991; Orzi et al. 1990).
Recently, it was found that a single train of rTMS induced significant changes in tissue monoamine levels in selected areas of rat brain, including an increased dopamine concentration in the hippocampal formation that was accompanied by a decrease in the dopamine turnover rate (Ben-Shachar et al. 1997). In addition, a significant increase in hippocampal dopamine release after acute rTMS by in vivo microdialysis was reported (Keck et al. 1998). Antero- and retrograde tracing techniques revealed that the rat hippocampal CA1 area, which provides the major cortical output of the hippocampal formation, projects not only to ipsi- and contralateral cortical regions, to the amygdala and to the hypothalamus, but also to the nucleus accumbens (van Groen and Wyss 1990), a brain region that is known to play a crucial role in reward and incentive motivation (Fibiger 1995). Given the close interaction between CCK and dopamine, it therefore seems possible that the rTMS-induced increase in CCK mRNA expression in several hippocampal and cortical regions observed in the present study is related to a functionally relevant activation of mesolimbic dopaminergic neuronal pathways.
As CCK is found to be co-localized with the inhibitory amino acid GABA in the hippocampus (Freund and Buzsáki 1996), this important neurotransmitter system should be considered as a potential effector of the rTMS-induced changes in CCK expression. The anatomical distribution of CCK-containing neurons in the hippocampus suggests that CCK is involved in both afferent and main efferent hippocampal pathways (Greenwood et al. 1981), and a recent electrophysiological study has shown that CCK increases GABA release by inhibiting a resting K+ conductance in hippocampal interneurons, thus leading to an increased tonic inhibition of pyramidal neurons (Miller et al. 1997).
In contrast to the neuropeptide CCK, NPY mRNA expression in the hippocampus and parietal cortex remains unaffected by long-term rTMS treatment, herewith underlining the specificity of the observed changes in BDNF and CCK expression levels. In contrast, a selective increase in the number of NPY-like immunoreactive and NPY mRNA expressing neurons predominantly in the hippocampal dentate gyrus has been described following repeated electroconvulsive shocks (Wahlestedt et al. 1990; Mikkelsen et al. 1994). Evidence from different animal models of experimental seizures suggests that brief or moderate convulsive stimuli, such as those used in electroconvulsive shock and kindling, strongly upregulate NPY expression in hippocampal GABAergic interneurons. Hippocampal CCK mRNA expression has been also found to be stimulated by repeated, but not single amygdala kindled seizures and ECS, but in contrast to the present results, this effect was only transient in nature and CCK mRNA expression returned to baseline levels already 24 h after the last seizure activity (Zhang et al. 1996). Although ECS and rTMS are similar in applying an electric current to the brain, the biological effects of these two methods might markedly differ: in contrast to ECS, rTMS does not elicit generalized seizure activity, and this fundamental difference indeed may account for the observed discrepancies in both the effects on selected neurotransmitter/neuromodulator systems and the time course of the changes observed.
Taken together, our results provide first evidence that long-term rTMS significantly stimulates the expression of BDNF in distinct areas of rat brain, as has been reported to occur after antidepressant drug treatment and ECS. Hence, these different types of antidepressant treatment may have a common mode of action at the molecular and cellular level. Further studies systematically investigating the influence of varying stimulation parameters (e.g., the duration of treatment, the total number of magnetic stimuli applied, the stimulation frequency, and precise localization of the stimulation coil) are necessary to better characterize the neurobiological effects of TMS responsible for its putative efficacy in the treatment of different neurological and psychiatric disorders. The observed rTMS-induced increase in CCK expression could contribute to the beneficial effects of rTMS in Parkinson's disease and to its therapeutic efficacy in the treatment of depressive disorders by modulating brain monoamine concentrations, probably via a stimulation of dopaminergic neuronal circuitries. Moreover, the idea that rTMS-induced stimulation of BDNF expression might be a novel therapeutic approach in the treatment of neurodegenerative diseases provides an attractive and clinically testable hypothesis.
References
Altar CA . (1999): Neurotrophins and depression. Trends Pharmacol Sci 20: 59–61
Ben-Shachar D, Belmaker RH, Grisaru N, Klein E . (1997): Transcranial magnetic stimulation induces alterations in brain monoamines. J Neural Transm 104: 191–197
Bickford RG, Guidi M, Fortesque P, Swenson M . (1987): Magnetic stimulation of human peripheral nerve and brain: Response enhancement by combined magnetoelectrical technique. Neurosurgery 20: 110–116
Blier P, de Montigny C . (1994): Current advances and trends in the treatment of depression. Trends Pharmacol Sci 15: 220–226
Brodin K, Ögren S-O, Brodin E . (1994): Clomipramine and clonazepam increase cholecystokinin levels in rat ventral tegmental area and limbic regions. Eur J Pharmacol 263: 175–180
Brodin K, Rosén A, Iwarsson K, Ögren S-O, Brodin E . (1989): Increased levels of substance P and cholecystokinin in rat cerebral cortex following repeated electroconvulsive shock and subchronic treatment with a serotonin uptake inhibitor. Acta Physiol Scand 136: 613–614
Castrén E, Berninger B, Leingartner A, Lindholm D . (1998): Regulation of brain-derived neurotrophic factor mRNA levels in hippocampus by neuronal activity. Progr Brain Res 117: 57–64
Cerri G, De Leo R, Moglie F, Schiavoni A . (1995): An accurate 3-D model for magnetic stimulation of the brain cortex. J Med Eng Tech 19: 7–16
Conner JM, Lauterborn JC, Yan Q, Gall CM, Varon S . (1997): Distribution of brain-derived neurotrophic factor (BDNF) protein and mRNA in the normal adult rat CNS: Evidence for anterograde axonal transport. J Neurosci 17: 2295–2313
Connor B, Dragunow M . (1998): The role of neuronal growth factors in neurodegenerative disorders of the human brain. Brain Res Rev 27: 1–39
Crawley JN, Corwin RL . (1994): Biological actions of cholecystokinin. Peptides 15: 731–755
Deschenes RJ, Lorenz LJ, Haun RS, Roos BA, Collier KJ, Dixon JE . (1984): Cloning and sequence analysis of a cDNA encoding rat preprocholecystokinin. Proc Natl Acad Sci USA 81: 726–730
Duman RS, Heninger GR, Nestler EJ . (1997): A molecular and cellular theory of depression. Arch Gen Psychiatry 54: 597–606
Fibiger HC . (1995): Neurobiology of depression: focus on dopamine. In Gessa G, Fratta W, Pani L, Serra G (eds), Depression and Mania: From Neurobiology to Treatment. New York, Raven Press, pp 1–17
Finkbeiner S, Tavazoie SF, Maloratsky A, Jacobs KM, Harris KM, Greenberg ME . (1997): CREB: A major mediator of neuronal neurotrophin responses. Neuron 19: 1031–1047
Fishback AS, Shields CB, Linden RD, Zhang YP, Burke D . (1995): The effects of propofol on rat transcranial magnetic motor evoked potentials. Neurosurgery 37: 969–974
Fleischmann A, Prolov K, Abarbanel J, Belmaker RH . (1995): The effect of transcranial magnetic stimulation of rat brain on behavior: Models of depression. Brain Res 699: 130–132
Freund TF, Buzsáki G . (1996): Interneurons of the hippocampus. Hippocampus 6: 347–470
George MS, Wassermann EM, Kimbrell TA, Little JT, Williams WE, Danielson AL, Greenberg BD, Hallett M, Post RM . (1997): Mood improvement following daily left prefrontal repetitive transcranial magnetic stimulation in patients with depression: A placebo-controlled crossover trial. Am J Psychiatry 154: 1752–1756
George MS, Lisanby SH, Sackheim HA . (1999): Transcranial magnetic stimulation. Arch Gen Psychiatry 56: 300–311
Gjerris A, Widerlov E, Werdelin L, Ekman R . (1992): Cerebrospinal fluid concentrations of neuropeptide Y in depressed patients and in controls. J Psychiatry Neurosci 17: 23–27
Greenwood RS, Godar SE, Reaves TA, Hayward JN . (1981): Cholecystokinin in hippocampal pathways. J Comp Neurol 203: 335–350
Grisaru N, Chudakov B, Yaroslavsky Y, Belmaker RH . (1998a): Catatonia treated with transcranial magnetic stimulation. Am J Psychiatry 155: 1630
Grisaru N, Chudakov B, Yaroslavsky Y, Belmaker RH . (1998b): Transcranial magnetic stimulation in mania: A controlled study. Am J Psychiatry 155: 1608–1610
Heilig M, Wahlestedt C, Ekman R, Widerlov E . (1988): Antidepressant drugs increase the concentration of neuropeptide Y (NPY)-like immunoreactivity in the rat brain. Eur J Pharmacol 147: 465–467
Heilig M, Widerlov E . (1995): Neurobiology and clinical aspects of neuropeptide Y. Crit Rev Neurobiol 9: 115–136
Hökfelt T, Rehfeld JF, Skirboll L, Ivemark B, Goldstein M, Markey K . (1980): Evidence for coexistence of DA and CCK in meso-limbic neurones. Nature 285: 476–478
Holsboer F . (1995): Neuroendocrinology of mood disorders. In Bloom FE, Kupfer DJ (eds), Psychopharmacology: The Fourth Generation of Progress. New York, Raven Press, pp 957–968
Jennum P, Klitgaard H . (1996): Repetitive transcranial magnetic stimulations of the rat. Effect of acute and chronic stimulations on pentylenetetrazole-induced clonic seizures. Epilepsy Res 23: 115–122
Ji R-R, Schlaepfer T, Aizenman CD, Epstein CM, Qiu D, Huang JC, Rupp F . (1998): Repetitive transcranial magnetic stimulation activates specific regions in rat brain. Proc Natl Acad Sci USA 95: 15635–15640
Kalkman CJ, Drummond JC, Ribberink AA, Patel PM, Sano T, Bickford RG . (1992): Effects of propofol, etomidate, midazolam, and fentanyl on motor evoked responses to transcranial electrical or magnetic stimulation in humans. Anesthesiology 76: 502–509
Keck ME, Sillaber I, Ebner K, Welt T, Kaehler ST, Singewald N, Philippu A, Elbel GK, Curt A, Wotjak CT, Landgraf R, Engelmann M . (1998): Neurochemical effects of acute rapid-rate transcranial magnetic stimulation: An intracerebral microdialysis study. Soc Neurosci Abstr 24: 746
Kokaia Z, Zhao Q, Kokaia M, Elmer E, Metsis M, Smith M-L, Siesjö BK, Lindvall O . (1995): Regulation of brain-derived neurotrophic factor gene expression after transient middle cerebral artery occlusion with and without brain damage. Exp Neurol 136: 73–88
Kononen J, Hökfelt T, Pelto-Hiokko M . (1995): Effects of ageing on the expressions of neurotrophins and their receptors in the rat pituitary gland. NeuroReport 6: 2429–2434
Kresse A, Jacobowitz DM, Skofitsch G . (1995): Detailed mapping of CGRP mRNA expression in the rat central nervous system: Comparison with previous immunocytochemical findings. Brain Res Bull 36: 261–274
Larhammar D, Ericsson A, Persson H . (1987): Structure and expression of the rat neuropeptide Y gene. Proc Natl Acad Sci USA 84: 2068–2072
Lindefors N, Brodin K, Stiller CO, Persson H, Brodin E . (1991): Repeated electroconvulsive shock increases tachykinin and cholecystokinin mRNA expression in ventral periaqueductal gray. Neuroscience 45: 73–80
Lindholm D, Dechant G, Heisenberg CP, Thoenen H . (1993): Brain-derived neurotrophic factor is a survival factor for cultured rat cerebellar granule neurons and protects them against glutamate-induced neurotoxicity. Eur J Neurosci 5: 1455–1464
Maisonpierre PC, Le Beau MM, Espinoza R, Ip NY, Belluscio L, de la Monte SM, Squinto S, Furth ME, Yancopoulos GD . (1991): Human and rat brain-derived neurotrophic factor and neurotrophin-3: gene structures, distributions, and chromosomal localizations. Genomics 10: 558–568
Mikkelsen JD, Woldbye D, Kragh J, Larsen PJ, Bolwig TG . (1994): Electroconvulsive shocks increase the expression of neuropeptide Y (NPY) mRNA in the piriform cortex and dentate gyrus. Mol Brain Res 23: 317–322
Miller KK, Hoffer A, Svoboda KR, Lupica CR . (1997): Cholecystokinin increases GABA release by inhibiting a resting K+ conductance in hippocampal interneurons. J Neurosci 17: 4994–5003
Moran TH, Schwartz GJ . (1994): Neurobiology of cholecystokinin. Crit Rev Neurobiol 9: 1–28
Nibuya M, Morinobu S, Duman RS . (1995): Regulation of BDNF and trkB mRNA in rat brain by chronic electroconvulsive seizure and antidepressant drug treatments. J Neurosci 15: 7539–7547
Nibuya M, Nestler E, Duman RS . (1996): Chronic antidepressant administration increases the expression of cAMP response element binding protein (CREB) in rat hippocampus. J Neurosci 16: 2365–2372
Orzi F, Zoli M, Passarelli F, Ferraguti F, Fieschi C, Agnati LF . (1990): Repeated electroconvulsive shock increases glial fibrillary acidic protein, ornithine decarboxylase, somatostatin and cholecystokinin immunoreactivities in the hippocampal formation of the rat. Brain Res 533: 223–231
Pascual-Leone A, Catala MD . (1995): Lasting beneficial effect of rapid rate transcranial magnetic stimulation on slowness in Parkinson's disease. Neurology 45: 550
Pascual-Leone A, Rubio B, Pallardo F, Catala MD . (1996): Rapid-rate transcranial magnetic stimulation of left dorsolateral prefrontal cortex in drug-resistant depression. Lancet 348: 233–237
Pascual-Leone A, Valls-Solé J, Brasil-Neto JP, Cammarota A, Grafman J, Hallett M . (1994): Akinesia in Parkinson's disease. II. Effects of subthreshold repetitive transcranial motor cortex stimulation. Neurology 44: 892–898
Phillips HS, Hains JM, Armanini M, Laramee GR, Johnson SA, Winslow JW . (1991): BDNF mRNA is decreased in the hippocampus of individuals with Alzheimer's disease. Neuron 7: 695–702
Post A, Müller MB, Engelmann M, Keck ME . (1999): Repetitive transcranial magnetic stimulation in rats—evidence for a neuroprotective effect in vitro and in vivo. Eur J Neurosci 11: 3247–3254
Rossini PM, Rossi S . (1998): Clinical applications of motor evoked potentials. Electroencephalogr Clin Neurophysiol 106: 180–194
Schalling M, Friberg K, Seroogy K, Riederer P, Bird E, Schiffmann SN, Mailleux P, Vanderhaeghen JJ, Kuga S, Goldstein M, Kitahama K, Luppi PH, Jouvet M, Hökfelt T . (1990): Analysis of the expression of cholecystokinin in dopamine cells in the ventral mesencephalon of several species and in humans with schizophrenia. Proc Natl Acad Sci USA 87: 8427–8431
Schuman EM . (1999): Neurotrophin regulation of synaptic transmission. Curr Opin Neurobiol 9: 105–109
Shimohama S, Tamura Y, Akaike A, Tsukahara T, Ohara O, Watanabe S, Kimura J . (1993): Brain-derived neurotrophic factor pretreatment exerts a partially protective effect against glutamate-induced neurotoxicity in cultured rat cortical neurons. Neurosci Lett 164: 55–58
Siebner HR, Mentschel C, Auer C, Conrad B. . (1999): Repetitive transcranial magnetic stimulation has a beneficial effect on bradykinesia in Parkinson's disease. NeuroReport 10: 589–594
Siuciak JA, Lewis DR, Wiegand SJ, Lindsay RM . (1997): Antidepressant-like effect of brain-derived neurotrophic factor (BDNF). Pharmacol Biochem Behav 56: 131–137
Smith MA, Zhnag L-X, Lyons WE, Mamounas LA . (1997): Anterograde transport of endogenous brain-derived neurotrophic factor in hippocampal mossy fibers. NeuroReport 8: 1829–1834
Somogyi P, Hodgson AJ, Smith AD, Nunzi MG, Gorio A, Wu J-Y . (1984): Different populations of GABAergic neurons in the visual cortex and the hippocampus of cat contain somatostatin or cholecystokinin-immunoreactive material. J Neurosci 14: 2590–2603
Takahashi M, Terwilliger R, Lane C, Mezes PS, Conti M, Duman RS . (1999): Chronic antidepressant administration increases the expression of cAMP-specific phosphodiesterase 4A and 4B isoforms. J Neurosci 19: 610–618
van der Kooy D, Hunt S, Steinbusch HWM, Verhofstad AAJ . (1981): Separate populations of cholecystokinin and 5HT-containing cells in the dorsal raphe and their contribution to its ascending projections. Neurosci Lett 26: 25–30
van Groen T, Wyss JM . (1990): Extrinsic projections from area CA1 of the rat hippocampus: olfactory, cortical, subcortical, and bilateral hippocampal formation projections. J Comp Neurol 302: 515–528
Wahlestedt C, Blendy JA, Kellar KJ, Heilig M, Widerlov E, Ekman R . (1990): Electroconvulsive shocks increase the concentration of neocortical and hippocampal neuropeptide Y (NPY)-like immunoreactivity in the rat. Brain Res 507: 65–68
Widdowson PS, Ordway GA, Halaris AE . (1992): Reduced neuropeptide Y concentrations in suicide brain. J Neurochem 59: 73–80
You Z-B, Tzschentke TM, Brodin E, Wise RA . (1998): Electrical stimulation of the prefrontal cortex increases cholecystokinin, glutamate and dopamine release in the nucleus accumbens: An in vivo microdialysis study in freely moving rats. J Neurosci 18: 6492–6500
Zetterström TS, Pei Q, Grahame-Smith DG . (1998): Repeated electroconvulsive shock extends the duration of enhanced gene expression for BDNF in rat brain compared with a single administration. Brain Res Mol Brain Res 57: 106–110
Zhang LX, Smith MA, Kim SY, Rosen JB, Weiss SR, Post RM . (1996): Changes in cholecystokinin mRNA expression after amygdala kindled seizures: An in situ hybridization study. Mol Brain Res 35: 278–284
Zyss T, Gorka Z, Kowalska M, Vetulani J . (1997): Preliminary comparison of behavioral and biochemical effects of chronic transcranial magnetic stimulation and electroconvulsive shock in the rat. Biol Psychiatry 42: 920–924
Acknowledgements
This study was supported by Kompetenznetzwerk “Depression and Suicidality” (Bundesministerium für Bildung und Forschung, Subproject 4.5). The stimulation device was generously provided by DANTEC, Skovlunde, Denmark.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Müller, M., Toschi, N., Kresse, A. et al. Long-Term Repetitive Transcranial Magnetic Stimulation Increases the Expression of Brain-Derived Neurotrophic Factor and Cholecystokinin mRNA, but not Neuropeptide Tyrosine mRNA in Specific Areas of Rat Brain. Neuropsychopharmacol 23, 205–215 (2000). https://doi.org/10.1016/S0893-133X(00)00099-3
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(00)00099-3
Keywords
This article is cited by
-
Protective Effects of Repetitive Transcranial Magnetic Stimulation Against Streptozotocin-Induced Alzheimer’s Disease
Molecular Neurobiology (2023)
-
Neuromodulation-Based Stem Cell Therapy in Brain Repair: Recent Advances and Future Perspectives
Neuroscience Bulletin (2021)
-
Targeting neuroplasticity in patients with neurodegenerative diseases using brain stimulation techniques
Translational Neurodegeneration (2020)
-
Inhibition of monoamine oxidase activity by repetitive transcranial magnetic stimulation: implications for inter-train interval and frequency
European Archives of Psychiatry and Clinical Neuroscience (2020)
-
Combination of Human Mesenchymal Stem Cells and Repetitive Transcranial Magnetic Stimulation Enhances Neurological Recovery of 6-Hydroxydopamine Model of Parkinsonian’s Disease
Tissue Engineering and Regenerative Medicine (2020)