Abstract
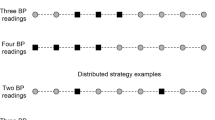
We conducted this study to determine whether ‘office hour’, defined as time period from 0800 to 1800 hours, ambulatory blood pressure monitoring (ABPM) predicts daytime (‘waking-hour’) and 24-h ABPM results, and to examine the impact of sleep disturbance on ABPM and nocturnal dip. Eighty-four patients (mean age 49±18 years, 47 males) were studied. Systolic, diastolic and mean 4-, 6-, 8-, ‘office-hour’ as well as ‘waking-hour’ blood pressures (BPs) were obtained from 24-h ABPM readings. Of these, no statistical differences were found between 8-h and ‘office-hour’ systolic, diastolic and mean BPs compared to ‘waking-hour’ values. There was complete concordance between ‘office-hour’ and ‘waking-hour’ ABPM diagnosis based on British Hypertension Society definitions. Sleep disturbance was found in 22 patients (26%). Although nocturnal dip was not significantly different in either sleep-disturbed or non-disturbed patients, patients who reported sleep disturbance had significantly higher proportion of borderline/abnormal BP diagnosis compared to non-sleep-disturbed counterpart during both ‘waking hour’ and night time. In patients without sleep disturbance, there was complete concordance between ‘office-hour’, ‘waking-hour’ and 24-h ABPM diagnosis based on British Hypertension Society definitions. ‘Office-hour’ ABPM is predictive of ‘waking-hour’ and 24-h ambulatory BP readings. Sleep disturbance is common in patients undergoing the test, and significantly raises the BP readings. We therefore propose ‘office-hour’ ABPM as an accurate, reliable and comfortable method of continual non-invasive BP monitoring, and omitting routine night time BP monitoring.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Owens P, Atkins N, O'Brien E . Diagnosis of white coat hypertension by ambulatory blood pressure monitoring. Hypertension 1999; 34 (2): 267–272.
Staessen JA, O'Brien ET, Thijs L, Fagard RH . Modern approaches to blood pressure measurement. Occup Environ Med 2000; 57 (8): 510–520.
Fagard R, Staessen JA, Thijs L . The relationships between left ventricular mass and daytime and night-time blood pressures: a meta-analysis of comparative studies. J Hypertens 1995; 13 (8): 823–829.
Redon J, Campos C, Narciso ML, Rodicio JL, Pascual JM, Ruilope LM . Prognostic value of ambulatory blood pressure monitoring in refractory hypertension: a prospective study. Hypertension 1998; 31 (2): 712–718.
Imai Y, Ohkubo T, Sakuma M, Tsuji II, Satoh H, Nagai K et al. Predictive power of screening blood pressure, ambulatory blood pressure and blood pressure measured at home for overall and cardiovascular mortality: a prospective observation in a cohort from Ohasama, northern Japan. Blood Press Monit 1996; 1 (3): 251–254.
Beltman FW, Heesen WF, Smit AJ, May JF, Lie KI, Meyboom-de Jong B . Acceptance and side effects of ambulatory blood pressure monitoring: evaluation of a new technology. J Hum Hypertens 1996; 10 (Suppl 3): S39–S42.
Ramsay L, Williams B, Johnston G, MacGregor G, Poston L, Potter J et al. Guidelines for management of hypertension: report of the third working party of the British Hypertension Society. J Hum Hypertens 1999; 13 (9): 569–592.
Ramsay LE, Williams B, Johnston GD, MacGregor GA, Poston L, Potter JF et al. British Hypertension Society guidelines for hypertension management 1999: summary. BMJ 1999; 319 (7210): 630–635.
Clement DL, De Buyzere ML, De Bacquer DA, de Leeuw PW, Duprez DA, Fagard RH et al. Prognostic value of ambulatory blood-pressure recordings in patients with treated hypertension. N Engl J Med 2003; 348 (24): 2407–2415.
Ohkubo T, Hozawa A, Yamaguchi J, Kikuya M, Ohmori K, Michimata M et al. Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens 2002; 20 (11): 2183–2189.
Calvo C, Hermida RC, Ayala DE, Lopez JE, Fernandez JR, Dominguez MJ et al. The ‘ABPM effect’ gradually decreases but does not disappear in successive sessions of ambulatory monitoring. J Hypertens 2003; 21 (12): 2265–2273.
Cuspidi C, Meani S, Salerno M, Valerio C, Fusi V, Severgnini B et al. Reproducibility of nocturnal blood pressure fall in early phases of untreated essential hypertension: a prospective observational study. J Hum Hypertens 2004; 18 (7): 503–509.
Leary AC, Murphy MB . Sleep disturbance during ambulatory blood pressure monitoring of hypertensive patients. Blood Press Monit 1998; 3 (1): 11–15.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wong, RC., Yeo, T. ‘Office-hour’ ambulatory blood pressure monitoring is sufficient for blood pressure diagnosis. J Hum Hypertens 20, 440–443 (2006). https://doi.org/10.1038/sj.jhh.1002022
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1002022