Abstract
Cytogenetic and DNA analyses of patients with the Beckwith-Wiedemann syndrome (BWS) enabled us to refine the localization of the syndrome at 11p15.3-pter to two distinct regions. One chromosome region (BWSCR1) is near the insulin (INS) and insulin-like growth factor 2 (IGF2) genes. The other region (BWSCR2) is more proximal near two sequences with zinc-binding finger motifs and a number of known and putative genes. This latter region, at least, seems to be associated with the development of childhood tumors. Our results strongly support the proposed involvement of parental imprinting in the etiology of BWS since all balanced chromosomal abnormalities in these patients were maternally transmitted while the mothers were phenotypically normal. We demonstrate that such an autosomal balanced rearrangement can lead to a specific maternal hypomethylation of the INS/IGF2 genes localized distal to the breakpoint. This underlines the role of these genes in the etiology of the syndrome.
Similar content being viewed by others
Introduction
The Beckwith-Wiedemann syndrome (BWS) was first described independently by Beckwith [1] and Wiedemann [2]. It occurs with an incidence of 1:13,700 births and is characterized by numerous growth abnormalities especially the EMG triad: exomphalos (umbilical hernia), macroglossia (enlarged tongue) and gigantism [3]. These features are variably present and can be found in association with multiple abnormalities including neonatal hypoglycemia (low blood glucose levels), typical ear creases and pits, and a unilateral growth abnormality of parts of the body called hemihypertrophy.
The incidence of different types of tumors found in BWS patients is 7.5% including the following childhood tumors: Wilms’ tumor (59% of all tumors found in this disorder), adrenocortical carcinoma (15%), and a few instances of hepatoblastoma and rhabdomyosarcoma [4]. All of these childhood tumors showed loss of heterozygosity for chromosome 11p15 alleles suggesting a common pathogenetic mechanism [5, 6].
The clinical findings in BWS patients tend to become less distinctive with age and therefore the syndrome can be underdiagnosed in adults [7]. Chitayat et al. [8] suggest that the clinical features of this overgrowth syndrome may be caused by persistent rests of embryonal cells that secrete paracrine and/or endocrine growth factors. These embryonal cells might also be precursor cells of the childhood tumors associated with BWS.
In 30% of the BWS patients, hypoglycemia has been diagnosed, which might be caused by the overproduction of insulin [9]. Children with BWS and children born to mothers with diabetes share certain clinical features [10]. Infants of diabetic mothers also develop high insulin levels to cope with their mothers, high blood glucose levels, sometimes have gigantism and craniofacial and cardiac defects as do children with BWS. Low blood glucose levels have been described in non-BWS patients with mesenchymal tumors including the BWS-associated tumors [reviewed by Macaulay, ref. 11].
In this respect, the assignment of BWS to chromosome region Hp15, near the insulin (INS) and insulin-like growth factor 2 (IGF2) genes, is interesting [12, 13]. Indeed, in some cases of BWS, overproduction of INS and the IGF2 gene products has been noted [ref. 9 and references therein; this study]. Increased expression of IGF2 has also been found in Wilms’ tumors and many other tumors including all those associated with BWS [14].
Overproduction of INS and/or IGF2 could therefore be responsible for the hypoglycemia and gigantism or other growth abnormalities in BWS children. Although this relationship has been found in many BWS patients and families, Henry et al. [15] presented a BWS pedigree in which the disease did not segregate with the insulin marker as studied with linkage analysis. They suggest genetic heterogeneity in the syndrome.
Chromosomal Abnormalities in the Syndrome
A few BWS cases with chromosomal abnormalities have been described. These patients provide evidence for an involvement of 11p15 in the syndrome. Since 1983, 18 cases with duplications of 11p material have been reported. These are of paternal origin in all 11 informative cases (table 1). The smallest duplicated region described is 11p15.4-pter [21, this study]. In addition, 5 patients have been described as having duplications of 11p15 but were not classified as having BWS even though various features of the syndrome were indeed present [reviewed by Turleau and de Grouchy, ref. 27]. In 4 out of 5 cases, the parental origin of the duplication was paternal. The only exception had a complex chromosomal rearrangement resulting in a partial 11p trisomy.
Two cases with a maternally derived balanced chromosomal rearrangement in 11p15 have been described [25, 26]. Two BWS patients had deletions of material from the proximal part of 11p as judged by conventional cytogenetic analysis [28, 29]. In all cases without cytogenetically detectable chromosome abnormalities (the large majority), no duplications or deletions could be detected at the molecular level [3, 15, 30–32, this study].
Apart from trisomy 11p or balanced chromosomal abnormalities involving 11p15, uniparental paternal isodysomy of the region containing IGF2 has been reported [33, 34].
Mode of Inheritance
Pettenati et al. [3] showed that 85% of the BWS cases are sporadic and 15% occur in a familial form. The mode of inheritance is probably autosomal dominant with incomplete penetrance [3, 35]. However, the syndrome is often only transmitted through females [36, 37]. Recent evidence suggests that genomic imprinting may explain this finding [38, 39]. From studies in human and mouse it is well established that the IGF2 gene is maternally imprinted and its receptor, as well as the H19 gene, are paternally imprinted [40–46]. IGF2 and H19, both localized to 11p15, might therefore be candidate genes for the imprinting effects seen in BWS.
So far, 14 cases of monozygotic twins with the Beckwith-Wiedemann syndrome have been reported [30, 35, 47–53]. Interestingly, in 12 out of 14 monozygotic twins only one of the two children had BWS. Lubinsky and Hall [51] suggest that there might be a relation between autosomal imprinting and X inactivation since all reported BWS twins are female.
Methyiation often reflects the active or inactive status of a gene [reviewed in Sapienza et al. 54]. In studies on BWS children of 3 monozygous BWS twins, hypomethylation of IGF2 was only found in the affected children [Weksberg, pers. commun.].
In this study we undertook the molecular and cytogenetic analysis of a large series of BWS patients to determine the critical region of 11p15 involved in the syndrome and associated tumors. Furthermore, we give additional evidence for a possible role of genomic imprinting in the syndrome because, apart from the preferential paternal origin of duplications, the predominantly maternal mode of inheritance, the paternal disomies and the location of the syndrome in a region already associated with genomic imprinting in Wilms’ tumor [55, 56 and references therein] and rhabdomyosarcoma [57], we now demonstrate that the parental origin of 7 out of 7 balanced BWS rearrangements is maternal.
Our results indicate that these translocations causing the BWS phenotype map to two distinct regions of 11p15.3-pter (BWSCR1 and BWSCR2). At least one region (BWSCR2) seems to be associated with the development of childhood tumors. All 7 translocations are maternally transmitted while the mothers were phenotypically normal. In addition, we demonstrated that a balanced BWS translocation of maternal origin in region 11p15.3 led to a specific hypomethylation of the INS/IGF2 genes. These genes map distal to this breakpoint at 11p15.5 and are candidate genes for BWS.
We propose a model in which, apart from INS and IGF2, at least one suppressor gene is involved in the etiology of BWS and associated childhood tumors. In this model, IGF2 and the suppressor gene(s) show opposite parental imprinting.
Materials and Methods
Patients
Blood samples for Epstein-Barr virus (EBV) transformation, cytogenetic analysis or direct DNA isolation from BWS patients and in most cases their parents were obtained from hospitals in The Netherlands (B8.1, B9.1, B10.1, B12.1, B13.1, B15.1, B16.1, B17.1, B18.1, BW6.1, BW7.1), United Kingdom (B1.1, B2.2, B3.1, B4.1, B5.1, B6.1, B7.1, BW1.1, BW2.1), Poland (B11.1), Norway (BW3.1), Denmark [B(9;11)1.1; BW5.1], France (PEL), Canada (1217), Japan (B24.1 and B23.1), and the United States (KS, R645, R646, B001, B002, B901). In addition we studied a patient from Portugal (WH5.1) who had a Wilms’ tumor and hemihypertrophy, but only minimal clinical signs of BWS. Six BWS patients and WH5.1 developed a Wilms’ tumor. A de novo balanced translocation t(1; 11) found in blood samples of a healthy female [code: B(1;11)1.1] was also studied. The following patients have been described elsewhere: R645 and R646 [16, 58]. Patient R645 carried a der(11) with a duplication of chromosome band 11p15. Patient R646 had a recombinant chromosome with a dup(11)(11p13-pter) and a del(11)(11q23-qter) as a result of a paternal pericentric inversion. B24.1 carried a dup(11)(p15.3-pter) of paternal origin [46, −14,+der(14), t(11;14)(p15.3; q23.3)] [23]. PEL [18, 21] carried a balanced reciprocal translocation 46, XY, t(11;18)(p15.4;p11.1). This healthy father had two sons with BWS and dup(11)(p15.4-pter) due to the der(18) chromosome. One child presented with an adrenocortical carcinoma. B901, a BWS patient with a balanced translocation t(11p;22q), has been described by Pueschel and Padre-Mendoza [25]. B001 and B002 [50] are monozygotic BWS twins with a duplication/insertion of chromosome 15(q11.2→q13) which was maternally inherited. The mother had no clinical signs of BWS.
The following patients were renumbered for this study: R646 (patient 1), R645 (patient 2), B24.1 (patient 3), PEL (patient 4), WH5.1 (patient 5), B10.1 (patient 6), B901 (patient 7), B(9;11)1.1 (patient 8), 1217 (patient 9), B23.1 (patient 10), B(1;11)1.1 (patient 11). The clinical features of the patients are given in table 2.
DNA Isolation, Digestion, Gel Electrophoresis and Hybridization
DNA was isolated, electrophoresed, blotted and hybridized as described earlier [59]. DNA was isolated from lymphocytes or EBV-transformed lymphoblastoid cell lines of the patients.
Dosimetric A nalysis
Autoradiography were scanned and analyzed as described earlier [59]. A nonsyntenic chromosome 2 probe L2.3 (D2S1) was used as a reference probe.
DNA Methylation Studies
The degree of methylation for the HRAS1, INS, IGF2, D11S12 and HBBC alleles was measured using the methylation-sensitive enzyme HpaII and its methylation-insensitive isoschizomere MspI. Double digestions with the above-mentioned enzymes and TaqI enabled identification of the parental origin of the INS, D11S12 and HRAS1 alleles in informative cases since the markers used recognize a TaqI RFLP. To compare the results the same blots were used for all markers. All experiments were repeated in duplicate or triplicate. We studied lymphocytes from blood samples of patient B10.1, his parents and as controls healthy neonates and adults. In addition we studied cells from amniotic fluid, fetal tissue, placental tissue, EBV-transformed cell lines, and Wilms’ tumors.
Probes
The following markers have been used. All single-copy probes are described in detail in the HGM10 and 10.5 proceedings [60, 61]. In all cases the available RFLPs were used in informative individuals to determine the allele copy number.
Single-Copy Probes. Band 11p15.4-pter: HRAS1 (pEJ6.6), INS (pHINS-310 and pgHI3.6), IGF2 (pHins311), D11S12 (pADJ762) and HBBC (pHd3.2); band 11p15.1-p15.2: CALCA (pEMBL36), and PTH (p20.36); band 11p14: HBVS1 (pUCS8-2 and pUCRH-6), FSHB (pFSHB1.1), D11S151 (p56H2.4), and D11S16 (p32-l); band 11p13: D11S324 (p60H1.4), D11S323 (p5S1.6), D11S325 (p8B1.25), and CAT (pCATint1); band 15q11-q12: D15S9 (pML34); band 15q11-q13: D15S18 (pIR39); band 15q12-q24: D15S4 (phage 15); band 15q25-q26: IGF2R (pIGF2-I-R.8). An alphoid probe pLC11A (D11Z1) [62] was used as a chromosome-specific probe for the centromeric region of chromosome 11 and, D15Z1 for detection of centromere 15 [63].
Cosmids/Phage. HRAS1 (cos 536/537) [64]; INS/IGF2 (cosIGF2 and cosInsul-IGF2) [65]; D11S12 (e2313/e2328); HBBC (cosHG50) (gift of R. Fodde); D11S87 (C1.1) [66]; CALCA (coshCT2) [67]; CALCB (cos SG7.1) [68]; CALCP (lambdaTG3) [69]; D11S431 (cCI11-10), D11S466 (cCI11-280), D11S441 (cCI11-38), D11S475 (cCI11-310) [70]; D11S834 (ZnFP65); D11S776 (ZnFP83), D11S777 (ZnFP94), D11S778 (ZnFP04), D11S779 (ZnFP40), D11S780 (ZnFP57), D11S781 (ZnFP17), D11S782 (ZnFP13) [71]. For the following cosmids no D numbers are yet available: L163, L29, L07, L201 [72]; e2624; e3883; e2218; e3198; e2293; ZnFP104; C428; C402; A403; C444a; C444b; C464; A421; A449; B470 [64]; cCIll-289; CCIl1395; CCIl1440; cCIl1421; cCIl1489; cCIl1583 (gift Y. Nakamura). The localization of all cosmids is listed in figure 1. All probes were nick translated as described earlier [59].
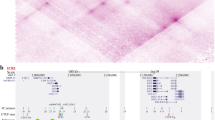
Regional mapping of chromosome 11p cosmids and FISH analysis of BWS patients with 11p abnormalities. D numbers, cosmid names, FLpter values and corresponding 11p bands are given for the markers used. The order is from telomere (top of table) to centromere. Some of the 95% confidence intervals are overlapping but often the order could be established relative to breakpoints. The relative position for HRAS1, INS/IGF22 and D11S12 was taken from the HGM10 proceedings [61]. D11S87 and D11S781 were ordered with CHEF analysis (data not shown). The position of all breakpoints can be deduced from the table. BWS patients 1 (R646), 2 (R645), 3 (B24.1) and 4 (PEL) presented with 11p duplications. BWS patients 5 (WH5.1), 5a (mother WH5.1), 6 (B10.1), 6a (mother B10.1), 7 (B901), 8 [B(9;11)1.1], 8a [mother B(9;11)1.1], 9 (1217) and 10 (B23.1) carried balanced chromosomal abnormalities. Patient 11 [B(1;11)1.1] was a healthy female carrying a de novo balanced translocation. ▩ = DNA marker duplicated; ■ = DNA marker translocated; 0 = DNA marker not duplicated or translocated; − = not done; @ = evolutionarily conserved random cosmid; & = cosmid showing double signal; * = FLpter values adapted from Lichter et al. [73].
Cytogenetic Analysis
Cytogenetic analysis was performed on new patients to establish the presence of cytogenetic abnormalities and on patients with known aberrations for a better definition of the breakpoints. In all cases with chromosomal abnormalities, chromosome slides were prepared for in situ hybridization.
Prometaphase Chromosomes. High-resolution chromosomes from peripheral lymphocytes were obtained according to a double-synchronization technique [78]. EBV transformed lymphoblastoid cell lines were cultured in RPMI 1640, supplemented with 15% fetal calf serum. The cells were synchronized using a thymidine block (final concentration 0.3 mg/ml). After incubation at 37° C for 17 h the medium was replaced with fresh RPMI and cells were incubated for a further 5 h. Colcemid was added to a final concentration of 0.2 µg/ml for 30 min. Cells were harvested according to standard procedures, using methanol: acetic acid (3:1) as a fixative. Slides with well spread metaphases and without cytoplasm were kept at 60°C overnight for hybridization.
In situ Hybridization
Probes were biotin-labeled using a nick translation kit, according to the manufacturer’s specifications (Bethesda Research Laboratories).
Chromosomal in situ Suppression (CISS) Hybridization. This was adapted from Lichter et al. [73, 75] and slightly modified. Prior to hybridization the probe was ethanol-precipitated in the presence of × 500 total human DNA (THD, Boehringer). The probe was then dissolved in a hybridization mixture containing 50% formamide (Merck) in 2 × SSC, 50 mM NaHPO4, 10% dextran sulfate (Pharmacia, pH 7) to give a final concentration of 5 ng/µl. After denaturation of the probe mixture (5 min at 70 °C), preannealing of repetitive DNA sequences was allowed for 1 h at 37° C. Slides were treated with RNase (Sigma, 100 µg/ml in 2 × SSC for 1 h at 37°C), followed by proteinase K (Boehringer) digestion. Slides were preincubated in proteinase K buffer (200 mM Tris-HCl, 20 mM CaCl2, pH 7.4) for 10 min at 37°C, followed by incubation with 5–10 µg proteinase K in 100 ml buffer (10 min at 37°C). Subsequently, slides were washed in PBS + 50 mM MgCl2; and fixed in the same buffer, containing 4% paraformaldehyde (10 min at room temperature). Target DNA was then denaturated separately in 100 µl of a denaturation mixture (70% formamide, 2 × SSC, 40 mM NaHPO4, pH 7), under a sealed coverslip (24 × 50 mm) for 5 min at 80°C, and dehydrated through an ethanol series (2 × 5 min 70%; 1×5 min 96%; 1 × 5 min 100%). Slides were dried at 37 °C and then incubated overnight at 37 °C with 20 µl probe mixture under a coverslip.
CISS Hybridization Combined with Centromere-11- or 15-Specific Probes. When cosmids and the centromere-11- or 15-specific probes were hybridized simultaneously, the cosmid probe was prepared as described above to a final concentration of 10 µg/µl. Centromere-specific probe (5 µg/µl in the same hybridization buffer) was denaturated separately for 5 min at 70 °C. Shortly before hybridization, 10 µl of each was mixed and applied to denaturated target DNA.
Posthybridization Washes. After hybridization, slides were washed (2×1 min) in 50% formamide, 2 × SSC at 42°C (pH 7), followed by 2 × SSC (2 × 5 min) at 42 °C and 4 × SSC/0.05% Tween 20 (Sigma), pH 7.0 (1 × 5 min) at room temperature. FITC-conjugated avidin (Vector) was used for the detection of biotinylated probe (5 µg/ml in 4 x SSC/0.05% Tween 20, 5% nonfat dry milk (NFDM; Elk, Campina), pH 7) for 20 min at room temperature after a 10 min preincubation in the same buffer. To amplify the signal, slides were washed in 4 × SSC/0.05% Tween (3×5 min) and incubated for 20 min in 4 × SSC/Tween 20/NFDM + 5 µg/ml biotinylated goat anti-avidin (Vector). After 3 washes in 4 × SSC/Tween (3× 5 min), the FITC detection procedure was repeated. When necessary for signal detection, the amplification procedure was repeated once more. Finally, slides were washed in 4 × SSC/0.05% Tween 20 (1 × 5 min) and PBS pH 7.4 (2 × 5 min) and dehydrated through an ethanol series. Slides were mounted in 35 µl antifade solution [2% l,4-diazobicyclo(2,2,2)-octane (Merck) in 90% glycerol, 0.02 M Tris/HCl pH 7.5] containing 200 ng/ml propidium iodide (Sigma).
Microscope Examination. Slides were examined under a Zeiss Axioplan epifluorescence microscope, using filterset 09 (BP 450–490, FT 510, LP 520). Pictures were taken on a Kodak EPD color slide film.
Probe Localization with Fluorescence in situ Hybridization (FISH). Probes were localized by measuring the relative position of the probe on the chromosome. For identification of chromosome 11, the centromere-specific probe pLC11A was used. Map positions of the cosmids were expressed as the fractional length of the whole chromosome relative to pter (FLpter) [73]. Measurements were done on slides projected on the wall. For each cosmid, FLpter values were calculated for 10–15 prometaphase chromosomes with a length between 9 and 15 µm, and a 95% confidence interval was determined. We compared the FLpter values with ideograms based on measurements of chromosomes in the same stage of contraction [approximately 750-band stage, ref. 76]. Because measured band positions at a defined band level are very consistent [77], they coincide with FLpter values.
Endocrine Investigations
Following an overnight fast, blood was drawn from the patients via an indwelling venous cannula, separated immediately and assayed for glucose, growth hormone GH), IGF1, insulin, C peptide, 17±-hydroxy-progesterone (17-OHP), dehydroepiandrosterone sulfate (DHAS), and testosterone. A prolonged glucose tolerance test was performed after glucose, 1.4g/kg, had been given orally. Blood was collected at 90, 120, 180, 240, and 300 min for glucose and GH, and at 90 and 180 min for insulin and C peptide.
GH, IGF21, 17-OHP, DHAS, testosterone (Dr. B. Rudd, West Midlands Regional Endocrine Laboratory UK), insulin and C peptide (Dr. D. Teale, Supraregional Endocrine Assay Service, St. Luke’s Hospital, Guildford, UK) were measured using standard radioimmune assay techniques with in-house reagents and double-antibody separation.
Only a few reports on endocrine investigations describe high levels of IGF2 in some BWS children. Therefore we collected the available data on our series of BWS patients. The results show that elevated IGF2 and insulin levels were found in 1 out of 5 BWS children. This particular child also developed a Wilms’ tumor. Although increased expression of these genes after birth can be found, it is not a common feature in the BWS syndrome. This might be explained by a narrow time window of overexpression (for example during fetal development).
Some of the children were tested for 17-OHP, DHAS and testosterone because of a report which referred to adrenal hyperplasia in BWS patients [78]. IGF1, C peptide, insulin and GH were chosen because of the hypoglycemia and growth abnormalities seen in BWS.
The following patients were tested for 17-OHP, DHAS, testosterone, IGF1, insulin, C peptide (for IGF1/IGF2), and GH: B3.1, B4.1, B5.1, B6.1, B7.1 and BW2.1. B1.1 and BW1.1 have been tested for these markers excluding insulin and C-peptide, and B2.1 for GH only.
For patients B2.1, B5.1 and BW2.1 (who developed a Wilms’ tumor) no adequate suppression of GH was seen after glucose stimulation. BW2.1 also showed markedly elevated levels of insulin (155 mU/l after 90 min; normal range <100 mU/l) and C-peptide (2.7 µg/l at 0 min and 15.4 µg/l at 90 min; normal range < 1.0 µg/l at 0 min and < 5µg/l at 90 min) with normal IGF1 levels. Marginally elevated levels of DHAS (8 µmol/l; normal range 1.3–7.4 µmol/l) and testosterone (3.5 nmol/l; normal range 0.8–3.1 nmol/l) were seen in patient B7.1.
Results
Cytogenetic Analysis
We started with a cytogenetic analysis of all 35 BWS patients. Figure 1 shows the breakpoints on chromosome 11p found in the patients with chromosome 11 rearrangements. We could confirm the cytogenetic findings of the patients with 11p duplications (patients 1, 2, 3 and 4). The chromosomal breakpoints in all patients with balanced chromosomal abnormalities mapped to region 11pl15.4-pter at the cytogenetic level, suggesting clustering of these breakpoints. Patient 5 showed an inv(11)(p15.4q22.3). The same inversion was found in his mother and two other members of this family (fig. 2). A t(4;11)(p15.2;p15.4) was found in patient 6 at prenatal diagnosis. A t(11;22)(p15.5;q12) was found in patient 7, a t(9;11)(p11.2;p15.5) in patient 8, a t(11;16)(p15.5;q12) in patient 9 and a t(11;12)(p15.5;q13.1) in patient 10. A de novo t(1;11)(p36.11;p15.5) was found in patient 11, a healthy female. All healthy mothers were carriers of the balanced rearrangements consistent with the involvement of genomic imprinting in this disorder. The presence of extra chromosomal material in 15(q11.2-q13) in the BWS twins [50] was confirmed (data not shown).
Predigree of the family with inv(11) (p15.4q22.3) (patient 5). In this family, expression of the phenotype was only seen after maternal transmission of the inversion. The carriers of the inversion are indicated with half-closed boxes and circles. Only the proband indicated with an arrow developed a Wilms’ tumor and presented with hemihypertrophy. N = Normal karyotype, ? = obligate carrier.
Representative partial karyotypes are given in figure 3. Figure 2 shows the pedigree with an inv(11) and maternal transmission of BWS-associated clinical features. Table 1, summarizes the parental origin of the chromosome 11 abnormalities found in our BWS patients.
Representative karyotypes of chromosomal breakpoints in BWSCR1 and BWSCR2. Idiograms and chromosomes involved in the BWS-associated translocations. Partial karyotypes of a patient (patient 6, fig. 1) with a t(4;11)(p15.2;p15.4)mat and a patient (patient 7, fig. 1) with a t(11;22)(p15.5;q12)mat are shown.
DNA Analysis and FISH
To refine the localization and to determine whether the breakpoints were clustered at the DNA level, FISH and DNA analyses were needed.
For this reason we isolated and mapped a large series of 11p markers. Figure 1 shows the FISH results (cosmid localization and analyses of chromosomal abnormalities). Examples of DNA analyses are given in figure 4. Representative examples of FISH are given in figure 5.
Representative Southern analysis of trisomy 11p cases and methylation experiments. Molecular weights are indicated. A TaqI digests of DNA from reference (lanes 1 and 3) and patient 1 (lane 2) hybridized to pEJ6.6 (HRAS1). Three different polymorphic alleles can be seen in the patient, demonstrating the duplication. B HindIII digests of reference DNA (lane 1) and DNA from patient 1 hybridized to pFSHB1.1 (FSHB). Neither allele is duplicated compared to the reference RFLP. C PstI/EcoR1 double digests of reference (lane 1) and patient 2 (lane 2) DNA hybridized to p20.36 (PTH). The minor allele of patient R645 is duplicated. D TaqI/HpaII double digests of patient 6 from DNA samples at 3 months (lane 2), 3 years (lane 3), mother (lane 4) and father (lane 5) hybridized to probe pHins311 (IGF2). A representative MspI digest is shown in lane 1. Lane 2 shows the abnormal hypomethylation of IGF2, normally not seen in controls. E The same Southern blot as in D was hybridized to pgHI3.6 (INS) for lanes 1–3. In addition, TaqI digests of child (lane 4), mother (lane 5) and father (lane 6) show the INS RFLPs. Hypomethylation of both alleles is seen in lane 2. In lane 3, only the maternal allele on the translocation chromosome is hypomethylated.
FISH. The probes used give yellow signals (FITC) on red counterstained (propidium iodide) chromosomes. Examples of FISH analyses using 11p cosmids and a centromere-11-specific probe pLC11A hybridized to metaphases from patients with BWS. A Patient 6, t(4;11)(p15.2;p15.4)mat. Probes used are L29 and pLC11A. The signal is proximal to the breakpoint and remains on the der(11). B Patient 6. Probes used are two overlapping cosmids for INS/IGF2. The hybridization signal is distal to the breakpoint and is translocated to the der(4). C Patient 6. Probes used are L7 and pLC11A. The L7 signal is proximal to the breakpoint. D Patient 1 with a duplication 11p due to a paternal pericentric inversion followed by a recombination event. Cosmids used are INS/IGF2. The signal is on the pter and qter regions of the der(11). E Patient 1. Probe ZnFP17 (D11S781) is not duplicated. F Patient 2 with a duplication 11p. INS/IGF2 is duplicated (double signals). G Patient 2. Duplication of ZnFP40 (D11S779).
After Southern blot hybridization, abnormalities of chromosome 11p were only found in the BWS patients with duplications. For patient 1, the breakpoint was found to be between FSHB and HBVS1 at 11p 14.1, for patient 2 between CALCA/PTH and HBVS1 at 11p15.2-p14.1, for patient 3 between CALCA and HBBC, and for patient 4 between HBBC and CALCA/PTH at 11p 15.5-p15.1. No microdeletions/duplications were found in the patients with balanced chromosomal abnormalities. Southern analyses on the BWS twins with extra 15q material, using probes from the relevant 15q region, revealed no duplication of any of the probes used.
The relative positions of the cosmids used on 11p [FLpter; ref. 73] and their band positions are shown in figure 1. The combined application of Southern blotting techniques using single copy probes and FISH using a range of cosmids for 11p allowed an accurate definition of the chromosomal breakpoints in the 11p duplication patients (patients 1, 2, 3, and 4) and those with balanced chromosomal abnormalities (patients 5–11). Patient 1 had a breakpoint at 11p14.1 between FSHB (distal to D11S781) and D11S780; patient 2 a breakpoint at 11p15.1-p14.3 between C402/A403 and D11S834; patient 3 a breakpoint at 11p15.1-p15.3 between D11S475 and D11S777, and patient 4 a breakpoint at 11p15.3-p15.4 between e2624 and D11S776. The balanced rearrangements had breakpoints at 11p15.3-p15.4 between e2624 and D11S776 (patient 5) and between D11S466 and cCI11-583 (patient 6). The breakpoints of patients 4, 5, and 6 fall near four evolutionarily conserved sequences (D11S466, D11S776, D11S431, and cCI11-440), two of which have putative zinc finger protein (ZnFP) sequences (D11S776 and D11S466) [71]. The other balanced rearrangements are clustered at 11p15.5 between INS/IGF2 and cCI11-289/395 (patients 7, 8, 9, 10, and 11). FISH analysis on the BWS twins demonstrated that no contiguous 11p material, large enough to explain the duplication, was inserted in 15q, and therefore it is unlikely that the BWS phenotype was caused by a trisomy 11p. Cosmids tested combined with the centromere-15-specific probe were cosIGF2/InsIGF2 (INS/IGF2), cosHG50 (HBBC), L29, L163, ZnFP4, ZnFP40, ZnFP57, ZnFP17, ZnFP13, and L201.
The results demonstrate that the balanced rearrangements (and one trisomy case, patient 4) cluster in two regions. One (BWSCR1) near INS/IGF2 and one (BWSCR2) proximal to HBBC. Two patients with breakpoints within this latter cluster developed a tumor (patient 4 and 5). The distance between BWSCR1 and BWSCR2 is at least 4,000 kb (data to be published elsewhere).
From our physical map of this region and CHEF analyses of the BWS breakpoints, we could deduce that the breakpoints in BWSCR1 fall within a 450-kb region. The three breakpoints in BWSCR2 are within a 2,000-kb region, breakpoints 4 and 5 being closest to each other (data to be published elsewhere). This confirms the clustering found with FISH analysis. Although the genes for IGF2 and H19 are close to BWSCR1 (at an estimated distance of 400 kb), they are not disrupted by any of the breakpoints in this region (as judged with physical mapping and FISH).
DNA Methylation Studies
To test whether a balanced rearrangement found in a BWS patient could have an effect on the degree of methylation for 11p15 genes distal to the translocation breakpoint, we analyzed the HRAS1, INS, IGF2, HBBC genes and the D11S12 locus.
Figure 4D, E shows the abnormal methylation of INS/IGF2 in a BWS patient with a balanced translocation involving chromosome 11. For practical reasons, this was the only child demonstrating a translocation for whom we could examine DNA isolated from direct blood samples (not EBV cell lines). Although we were unable to study the expression of INS/IGF2 directly, the fact that the child suffered from hypoglycemia makes it likely that one or both of these gene products were overexpressed. In addition, recent studies on the fragile X and Prader-Willi/Angelman syndromes demonstrated that there was a direct correlation between hypomethylation and expression of the gene product involved or the phenotype of the syndrome [79, 80].
The translocation found in BWS patient 6 (B10.1) was first identified at amniocentesis. The presence of the translocation was confirmed after birth at the age of 3 months and was also found in the mother. Figure 4 shows the abnormal methylation pattern found in the child’s blood for the INS/IGF2 alleles at 3 months and 3 years, compared to the methylation pattern seen in the parents’ blood. The INS gene, located 1.4 kb 5′ of IGF2, enabled us to identify the parental alleles. At the age of 3 years, the paternal allele demonstrates the normal methylation pattern and the maternal allele on the der(4) remained hypomethylated. No abnormal methylation patterns at 3 months or 3 years of age were seen for other markers (HBBC, D11S12 and HRAS1) using the same Southern blots.
At the age of 3 years, the methylation status of the IGF2 gene in the patient is comparable to that of the parents. However, it should be noted that we cannot distinguish between the two IGF2 alleles with the probe used; therefore, it is not possible to identify the parental origin of the IGF2 alleles. It should also be noted that hypomethylation or allele-specific methylation for INS/IGF2 in control DNA from amniotic fluid, fetal tissue, neonate or adult blood samples was never seen with the INS and 5′ IGF2 probes used (two samples tested of each control, data not shown) confirming the results of Ghazi et al. [81]. In contrast, we did find hypomethylation of both alleles in control placenta (two samples tested), Wilms’ tumors (3 samples tested including a Wilms’ tumor from a BWS patient) and 3 EBV cell lines tested. In addition, Schneid et al. [82] recently demonstrated allele-specific methylation for IGF2 in lymphocytes in the 3′ region of the gene.
In order to find more patients informative for the INS marker we studied 8 additional BWS patients from our series. None of 8 DNA samples taken from direct blood samples of BWS patients was informative for the insulin TaqI RFLP. All samples were taken after 3 years of age and we could find no altered TaqI/HpaII restriction patterns after hybridization with INS/IGF2 probes.
Uniparental disomy in some cases could explain why 8 out of 8 BWS patients tested in this study were not informative for the INS marker.
Discussion
11p15 Is Imprinted
Several lines of evidence suggest the involvement of parental imprinting of chromosome 11p15 involved in the etiology of BWS and associated childhood tumors. A model involving opposite imprinted genes can be proposed to explain all the available data (fig. 6).
Imprinting model for the Beckwith-Wiedemann syndrome involving IGF2 and a suppressor of IGF2. a Proposed normal situation with inactivation of the maternal IGF2 gene in the target locus. The expression of the IGF2 gene (marked +) is controlled by locus 2 (BWSCR1/2) that contains a maternally expressed suppressor gene (which could also be involved in the development of tumors), b Mutations in familial BWS in locus 1 or 2 can lead to increased expression of the IGF2 gene. Maternal mutations can activate locus 1 or inactivate locus 2 or both (as shown), c Paternal disomy with two paternal and no maternal copies of locus 1 and 2 (as shown) or only two paternal copies of either locus. d Paternally derived duplication with two active copies of IGF2. e Maternally inherited translocation involving 11p15 and another chromosome leading to loss of the existing maternal imprint and consequently two active IGF2 alleles (as shown). The translocation chromosomes are shown to the left, the normal chromosomes to the right. The translocation breakpoint might also fall within locus 2 and thus disrupt the suppressor. A breakpoint proximal to locus 2 might also have an effect on the imprinting status of both loci.
Our results show that the chromosomal abnormalities found in BWS are always maternally inherited in cases with balanced chromosomal rearrangements of 11p. The breakpoints found in patients with balanced chromosomal abnormalities are within two clusters, BWSCR1 and BWSCR2. BWSCR1 is near the INS/IGF2 and H19 genes. BWSCR2 is near putative zinc finger genes and evolutionarily conserved sequences. We found a de novo 11p breakpoint in a healthy female (patient 11) that also falls within one of these regions. We believe that her children might therefore be at risk for the BWS syndrome. In addition, paternal transmission of a balanced 46, XY, t(11;21)(p15;q22) in a child did not result in the BWS phenotype although two brothers with trisomy 11p15 had BWS [Nordenskjöld, pers. commun.].
The duplications are always of paternal origin. We refined the smallest duplicated region to 11p15.3-pter, the breakpoint being within BWSCR2.
Furthermore, the uniparental isodysomies are always of paternal origin.
Finally, region 11p15 is associated with preferential maternal allelic losses in BWS associated childhood tumors [55, 57].
Imprinted Genes: The IGF2 Pathway
Since methylation often reflects the active or inactive status of a gene [reviewed by Sapienza et al., ref. 44], we tested whether the translocations found in BWS have an effect on the methylation of genes distal to the breakpoints. We studied the methylation status of several genes distal to one of the BWS breakpoints and found that the INS and IGF2 alleles on the balanced translocation chromosome t(4;11)(p15.2;p15.4)mat were hypomethylated compared to control samples from father, mother and various adults, neonates, or fetal tissue. Using RFLPs for the insulin gene we could demonstrate that in the patient both alleles were abnormally hypomethylated immediately after birth but that only the maternal allele remained hypomethylated after 3 years. The elevated levels of INS/IGF2 found in BWS patients [ref. 9, and references therein; this study] and associated tumors [14], and the hypomethylation of these genes, point to an involvement of these genes in BWS. This involvement may explain various features of the BWS syndrome such as neonatal hypoglycemia, the clinical similarities of BWS children to children born to mothers with diabetes, the growth abnormalities, and the neoplasia. The finding that between 3 months and 3 years the paternal alleles of the patient tested returned from a hypo- to a normal methylation status may explain why the hypoglycemia and the other clinical symptoms of BWS patients are prominent at a very young age, but are less distinctive at older ages [7].
Expression of IGF2 is found in all components forming the rodent chorioallantoic placenta but not in all embryo tissues and almost never in adult tissues [41]. It is becoming more and more evident that methylation can play a role in gene expression. If the observed hypomethylation in our patient indeed reflects increased expression, it would be in agreement with the hypomethylation (this study, data not shown) and high expression of IGF2 found in placenta, tumors and EBV-transformed lymphoblastoid cell lines [14, 41]. In tumor cells, the increased IGF2 expression could be involved in cell proliferation.
The human chromosome 11p15 region is known to be involved in genomic imprinting and is homologous to an imprinted region of mouse chromosome 7 [83]. Moore and Haig [84] proposed a model in which the paternally expressed IGF2 is able to bind to the IGF1 receptor (as are insulin and IGF1) leading to cell proliferation. IGF2 levels are controlled by the maternally expressed IGF2 receptor (IGF2r, homologous to the cation-independent mannose 6 phosphate receptor, CI-MPR). Binding of IGF2 to this receptor leads to the degradation of IGF2. This model also predicts that decreased levels of IGF2r (two paternal copies or inactivation of the maternal allele) would also promote cell proliferation. At present, no data are available that this receptor, localized to human chromosome region 6q25-q27, is involved in BWS and tumorigenesis. Nonetheless, the paternally derived allele at the murine T-associated maternal effect locus (Tme) is inactivated by genomic imprinting. Tme and IGF2r are closely linked (< 1,000 kb) [42, 85]. Forejt and Gregorova [85] demonstrated that viable hybrid mice with a maternally derived mutation at the Tme locus have no active IGF2r gene. These newborn mice were indeed bigger at birth than their IGF2r-positive sibs.
The IGF1 receptor is localized to 15q25-qter. As discussed, the two children of mono-zygous twins that both had BWS, have a duplication of or an insertion in region 15q11-q13 of maternal origin. In these twins, the duplication/insertion might have altered the existing imprint on 15q and subsequently increased the expression of the more distal IGF1 receptor. It is now known that the IGF1 receptor is imprinted [44] and the duplication/insertion occurred in an imprinted region of 15q associated with the Prader-Willi/Angelman syndromes [83]. It is possible that increased expression of this receptor leads to cell proliferation. This is underlined by the finding that antibodies to the IGF1 receptors have been found to inhibit growth of certain tumour cell lines [14].
From the model of Moore and Haig [84], it follows that both maternal and paternal genomes are necessary to maintain the balance between IGF2 and its receptors. We propose that in BWS patients and associated tumors this balance is disturbed because two active alleles for IGF2 are present at some stage of development through the mechanisms described in figure 6. In addition, at least one 11p suppressor of IGF2 is involved in the etiology of BWS.
The increased expression of IGF2 and insulin found in BWS and/or associated tumors is in agreement with our model. In addition, the experiments of DeChiara et al. [40, 41] demonstrate that an inactivating mutation of IGF2 leads to small mice after paternal inheritance of the mutated IGF2 allele. If it does not lead to lethality, it can be assumed that overproduction of IGF2 leads to increased growth. Indeed, the experiments of Ferguson-Smith et al. [86] demonstrate that the incorporation of cells with a paternal duplication of the mouse chromosomal region containing the IGF2 gene into chimeras, resulted in a striking growth enhancement of the embryos. As discussed, mutation of the maternal IGF2r leads to bigger mice at birth.
A Model to Explain the Observed Parental Effects
In this study we have described the finding of two BWS breakpoint clusters in 11p15, one at 11p15.5 near the INS/IGF2 genes and one more proximal at 11p15.3-p15.4. Because the metylation experiments described in this study show that hypomethylation in BWS occurs only at the INS/IGF2 genes and not at loci between the observed BWS translocation breakpoint and INS/IGF2 or distal to these genes, it is likely that the hypomethylation, and therefore possibly the imprint, in the most distal region is not a result of a general spreading of inactivation from a far more proximal region. It is known that imprinting does not necessarily involve large blocks of genes. Adjacent genes are not always imprinted, and those that are may show opposite parental imprinting. Although there is no evidence for imprinting of the human insulin gene, Kitsberg et al. [87] have demonstrated that IGF2, H19 and INS are localized to the same differentially replicating regions. The altered methylation pattern described in figure 4 might reflect changes in this allele-specific replication. Our investigations show that there are two breakpoint clusters on 11p15 involved in the etiology of BWS. It is therefore possible that multiple genes are involved.
We propose that there are at least two loci on 11p15 that show opposite parental imprinting. The distal locus contains the IGF2 gene that is only paternally expressed, the proximal locus one or more suppressor genes of IGF2 that is/are only maternally expressed. This model would explain not only the parental effects seen in BWS but also the preferential maternal loss of alleles seen in Wilms’ tumor and rhabdomyosarcoma, including the hemizygous loss of maternal 11p15 alleles seen in a Wilms’ tumor from a BWS patient [55]. The model is also in agreement with the tumour suppression seen after introduction of 11p15 into a Wilms’ tumor cell line [88] and the chromosomal breakpoints we found in the proximal region in both BWS patients with tumors. These breakpoints might have led to inactivation of a suppressor gene or to an altered gene product with a negative dominant effect, even if the gene should have been silenced by imprinting (as might be the case in patient 4).
Indeed, a locus on 11p15.4-pter has been found to be consistently involved in many human tumors including the BWS-associated tumors i.e. Wilms’ tumor, rhabdomyosarcoma, hepatoblastoma, adrenocortical carcinoma, but also breast, bladder and pancreatic cancers, testicular tumors and germline neoplasms [60]. This locus has been designated the multiple-tumor-associated chromosome region 1 (MTACR1). The smallest regions of overlap for allelic losses found in BWS-associated tumors coincide with both the BWSCR1 and BWSCR2 regions [89].
Whether a gene in these loci would suppress only in the cis and/or trans position, is actually involved in imprinting of other loci, or whether there is a gene dosage effect, is not clear at the moment.
From our model it follows that not only translocations disrupting BWSCR2, but also uniparental paternal disomies, resulting in no active suppressor allele, would increase the tumor risk. Henry et al. [34] demonstrated that indeed the tumor risk in these cases is not 7.5 but 50%. The authors also demonstrated that somatic mosaicism regarding the uniparental disomies can be found in BWS patients. This might explain the hemihypertrophy often seen in this disorder and proves that these latter uniparental disomies occur after fertilization.
Tumor Suppressor Candidate Sequences
There are several tumor suppressor candidate sequences mapped to 11p15.3-pter. We have localized the D11S776 sequence with multiple zinc-binding-finger motifs [P. Little, unpubl. results] to BWSCR2 (fig. 1). The putative DNA-binding properties of this sequence and its location close to the BWS breakpoints make this sequence a tumor suppressor gene candidate. However, it has yet to be determined whether this gene is imprinted. The same holds for D11S431, D11S466, and cCI11-440. WEE1, the human homologue of the weel yeast gene (a mitotic inhibitor), ST5 (a suppressor of tumorigenicity in HeLa cells) and rhombotin, a gene cloned from a leukemia translocation breakpoint, have also been mapped to BWSCR2 [Redeker, submitted].
The human homologue of the mouse H19 gene was recently found to be imprinted with maternal expression only and it is closely linked to IGF2 [45, 46]. Maternal disomy of this gene causes late prenatal lethality. However, this sequence was shown to map distal to D11S12 near INS/IGF2 [90]. We demonstrated with pulsed-field electrophoresis that H19 is very close but distal to IGF2 and still a long way from both BWS clusters [Redeker et al., in preparation]. The breakpoints in BWSCR1 do not disrupt the H19 or IGF2 genes. Nonetheless, these breakpoints are at an estimated distance of 400 kb and might have a position effect on the expression, or alter the imprint, of these genes. So far no other candidate suppressor sequences have been mapped to BWSCR1.
Finally, the WT1 gene localized to 11p13 can also act as an IGF2 suppressor as suggested earlier [55, 91].
At present, we have been able to identify most of the BWS breakpoints at the pulsedfield-electrophoresis level. BWSCR1 falls within a 450-kb fragment. This cluster is at most 400 kb separated from IGF2 (analyzed with interphase FISH and pulsed-field electrophoresis). The second cluster, BWSCR2, falls within an estimated region of 2,000 kb, at least 4,000 kb proximal to BWSCR1. We have cloned two breakpoints in BWSCR1 and one in BWSCR2, and have currently covered most breakpoints with cosmid contigs and YACS (to be published elsewhere).
Characterization of these breakpoints and analysis of mutations in these loci will enable us to study tumor suppressor or any other growth-promoting activity, if any, in the identified loci, and to analyze the contribution of genomic imprinting to the etiology of BWS and associated tumors.
References
Beckwith JP: Extreme cytomegaly of the adrenal fetal cortex, omphalocele hyperplasia of kidneys and pancreas, and Leydig-cell hyperplasia: Another syndrome? Los Angeles, Western Society of Pediatric Research, 1963.
Wiedemann HR: Complexe malformatif familial avec hernie ombilicale et macroglossie — un syndrome nouveau? J Genet Hum 1964;13:223–232
Pettenati MJ. Haines JL. Higgins RR., Wappner RS. Palmer CG, Weaver DD: Wiedemann-Beckwith syndrome: Presentation of clinical and cytogenetic data on 22 new cases and review of the literature. Hum Genet 1986;74:143–154
Wiedemann HR: Tumours and hemihypertrophy associated with Wiedemann-Beckwith syndrome. Eur J Pediatr 1983;141:129.
Koufos A, Hansen MF, Copeland NG, Jenkins NA, Lampkin BC, Cavenee WK: Loss of heterozygosity in three embryonal tumors suggests a common pathogenetic mechanism. Nature 1985;316:330–334
Henry I, Jeanpierre M, Couillin P, Barichard F, Huerre-Jeanpierre C, Glaser T, Lenoir G, Chaussain JL, Junien C: Tumor-specific loss of 11p15.5 alleles in del11p13 Wilms’ tumor and in familial adrenocortical carcinoma. Proc Natl Acad Sci USA 1989;86:3247–3251
Niikawa N, Ishikiriyama S, Takahahi S, Inagawa A, Tonoki H, Ohta Y, Hase N, Kamei T, Kajii T: The Wiedemann-Beckwith syndrome: Pedigree studies on five families with evidence for autosomal dominant inheritance with variable expressivity. Am J Med Genet 1986;24:41–55
Chitayat D, Rothchild A, Ling E, Friedman JM, Couch RM, Yong SL, Baldwin VJ, Hall JG: Apparent postnatal onset of some manifestations of the Wiedemann-Beckwith syndrome. Am J Med Genet 1990;36:434–439
Engström W, Lindham S, Schofield P: Wiedemann-Beckwith syndrome. Eur JPediatr 1988;147:450–457
Gardner LI: Pseudo-Beckwith-Wiedemann syndrome: Interaction with maternal diabetes. Lancet 1973;911–912.
Macaulay VM: Insulin-like growth factors and cancer. Br J Cancer 1992;65:311–320
Ping AJ, Reeve AE, Law DJ, Young MR, Boehnke M, Feinberg AP: Genetic linkage of Beckwith-Wiedemann syndrome to 11p15. Am J Hum Genet 1989;44:720–723
Koufos A, Grundy P, Morgan K, Aleck KA, Hadro T, Lampkin BC, Cavenee WK: Familial Wiedemann-Beckwith syndrome and a second Wilms’ tumor locus both map to 11p15.5. Am J Human Genet 1989;44:711–719
Rechler MM, Nissley SP: Insulinlike growth factors; in Peptide Growth Factors and Their Receptors I, Sporn MB, Roberts AB (eds): Handbook of Experimental Pharmacolocy. Heidelberg, Springer, 1990, vol 95: pp 263–367.
Henry I, Jeanpierre M, Barichard F, Serre JL, Mallet J, Turleau C, de Grouchy J, Junien C: Duplication of HRAS1, INS and IGF2 is not a common event in Beckwith-Wiedemann syndrome. Ann Genet 1988;31:216–220
Waziri M, Patil SR, Hanson JW, Burtley JA: Abnormality of chromosome 11 in patients with features of BWS. J Pediatr 1983;102:873–876
Turleau C, de Grouchy J, Chavin-Colin F, Martelli H. Voyer M, Charlas R: Trisomy 11 p15 and Beckwith-Wiedemann syndrome: a report of two cases. Hum Genet 1984;67:219–221
Journel A, Lucas I, Allaire C, Le Mee F, Defawe G, Lecornu M, Jouan H, Roussey M, Le Marec B: Trisomy 11p 15 and Beckwith-Wiedemann syndrome. Ann Genet 1985;28:97–101
Okano Y, Osasa Y, Yamamoto H, Hase Y, Tsuruhara T, Fujita H: An Infant with Beckwith-Wiedemann syndrome and chromosomal duplication 11p13-pter: Correlation of symptoms between 11p Trisomy and Beckwith-Wiedemann syndrome. Jpn J Hum Genet 1986;31:365–372
Wales JKH, Walker V, Moore IE, Clayton PT: Bronze baby syndrome, biliary hypoplasia, incomplete Beckwith-Wiedemann syndrome and partial trisomy 11. Eur J Pediatr 1986;145:141–143
Henry I, Jeanpierre M, Couillin P, Barichard F, Serre JL, Journel H, Lamouroux A, Turleau C, de Grouchy J, Junien C: Molecular definition of the 11p15.5 region involved in Beckwith-Wiedemann syndrome and probably in predisposition to adrenocortical carcinoma. Hum Genet 1989;81:273–277
Brown KW, Williams JC, Maitland NJ, Mott MG: Genomic imprinting and the Beckwith-Wiedemann syndrome. Am J Hum Genet 1990;46:1000–1001
Tonoki H, Narahara N, Marsumoto J, Niikawa N: Regional mapping of the parathyroid hormone gene (PTH) by cytogenetic and molecular studies. Cytogenet Cell Genet 1991;56:103–104
Brown KW, Gardner A, Williams JC, Mott MG, McDermott A, Maitland NJ: Paternal origin of 11p15 duplications in the Beckwith-Wiedemann syndrome. Cancer Genet Cytogenet 1992;58:66–70
Pueschel SM, Padre-Mendoza T: Chromosome 11 and Beckwith-Wiedemann syndrome. J Pediatr 1984;104:484–485
Norman AM, Read AP, Clayton-Smith J, Andrews T, Donnai D: Recurrent Wiedemann-Beckwith syndrome with inversion of chromosome (11)(p11.2p15.5). Am J Med Genet 1992;42:638–641
Turleau C, de Grouchy J: Beckwith-Wiedemann syndrome: Clinical comparison between patients with and without 11p15 trisomy. Ann Genet 1985;28:93–96
Haas OA, Zoubek A, Grumayer ER, Gardner H: Constitutional interstitial deletion of 11p11 and pericentric inversion of chromosome 9 in a patient with Wiedemann-Beckwith syndrome and hepatoblastoma. Cancer Genet Cytogenet 1986;23:95–104
Schmutz SM: Deletion of chromosome 11 (p11p13) in a patient with Beckwith-Wiedemann syndrome. Clin Genet 1986;30:154–156
Litz CE, Kimberly AT, Qiu JS, Pescovitz OH, de Martinville B: Absence of detectable chromosomal and molecular abnormalities in monozygotic twins discordant for the Wiedemann-Beckwith syndrome. Am J Med Genet 1988;30:821–833
Schofield PN, Lindham S, Engstrom W: Analysis of gene dosage on chromosome 11 in children suffering from Beckwith-Wiedemann syndrome. Eur J Pediatr 1989,148:320–324.
Spritz RA, Mager D, Pauli RM, Laxova R: Normal dosage of the insulin and insulin-like growth factor II genes in patients with the Beckwith-Wiedemann syndrome. Am J Hum Genet 1986;39:265–273
Henry I, Bonaiti-Pellie C, Chehensse V, Beldjord C, Schwartz C, Utermann G, Junien C: Uniparental paternal disomy in a genetic cancer-predisposing syndrome. Nature 1991;351:665–667
Henry I, Puech A, Riesewijk A, Ahnine L, Mannens M, Beldjord C, Bitoun P, Tournade MF, Landrieu P, Junien C: Somatic mosaicism for partial paternal isodisomy in Wiedemann-Beckwith syndrome: A post-fertilization event. Eur J Hum Genet 1993;1:19–29
Olney AH, Buehler BA, Waziri M: Wiedemann-Beckwith syndrome in apparently discordant monozygotic twins. Am J Med Genet 1988;29:491–499
Lubinski M, Herrman J, Kosseff AL, Opitz JM: Autosomal-dominant sex-dependent transmission of the Wiedemann-Beckwith syndrome. Lancet 1974;i:932.
Aleck KA, Hadro TA: Dominant inheritance of Wiedemann-Beckwith syndrome: Further evidence for transmission of ‘unstable premutation’ through carner women. Am J Med Genet 1988;33:155–160
Viljoen D, Ramesar R: Evidence for paternal imprinting in familial Beckwith-Wiedemann syndrome. J Med Genet 1992;29:221–225
Moutou C, Junien C, Henry I, Bonaiti-Pellie C. Beckwith-Wiedemann syndrome: A demonstration of the mechanisms responsible for the excess of transmitting females. J Med Genet 1992;29:217–220
DeChiara TM, Efstratiadis A, Robertson E: A growth-deficiency phenotype in heterozygous mice carrying an insulin-like growth factor II gene disrupted by targeting. Nature 1990;345:78–80
DeChiara TM, Robertson EJ, Efstratiadis A: Parental imprinting of the mouse insulin-like growth factor II gene. Cell 1991;64:849–859
Barlow DP, Stoger R, Herrman BG, Saito K, Schweifer N: The mouse insulin-like growth factor type-2 receptor is imprinted and closely linked to the TME locus. Nature 1991;349:84–87
Rachmilewitz J, Goshen R, Ariel I, Schneider T, de Groot N, Hochberg A: Parental imprinting of the human H19 gene. FEBS Lett 1992;309:25–28
Rappolee DA, Sturm KS, Behrendtsen O, Schultz GA, Pedersen RA, Werb Z: Insulin-like growth factor II acts through an endogenous growth pathway regulated by imprinting in early mouse embryos. Genes Dev 1992;6:939–952
Bartolomei, M.S., Zemel, S., Tilghman, S.M. Parental imprinting of the mouse H19 gene. Nature 351: 153–155 (1991).
Zhang Y, Tycko B: Monoallelic expression of the human H19 gene. Nature Genet 1992;1:40–44
Benke PJ: Familial BWS. Annu Birth Defects Conf San Francisco, June 1978.
Berry AC, Belton EM, Chantier C: Monozygotic twins discordant for Wiedemann-Beckwith syndrome and the implications for genetic counselling. J Med Genet 1988;17:136–138
Bose B, Wilkie RA, Madlon M, Forsyth JS, Faed MJ: Wiedemann-Beckwith syndrome in one of monozygotic twins. Arch Dis Child 1985;60:1191–1192
Estabrooks LL, Lamb AN, Kirkman HN, Boyer S Wiley JE, Callanan NP, Rao KW: Beckwith-Wiedemann syndrome in twins with a duplication of chromosome 15(q11.2–q13)mat. Am J Hum Genet 1989;45 (suppl) A75.
Lubinski MS, Hall JG: Genomic imprinting, monozygous twinning and X inactivation. Lancet 1991;337: 1288.
Clayton-Smith J, Read AP, Donnai D: Monozygotic twinning and Wiedemann-Beckwith syndrome. Am J Med Genet 1992;42:633–637
Franceschini P, Guala A, Vardeu MP, Franceschini D: Monozygotic twinning and Wiedemann-Beckwith syndrome. Am J Med Genet 1993;46:353–354
Sapienza C, Tran TH, Paquette J, McGowan R, Peterson A: A methylation mosaic model for mammalian genome imprinting. Prog Nucleic Acids Res Mol Biol 1989;1:145–157
Mannens M, Slater RM, Heyting C, Bliek J, de Kraker J, Coad N, De Pagter-Holthuizen P, Pearson PL: Molecular nature of genetic changes resulting in loss of heterozygosity of chromosome 11 in Wilms’ tumors. Hum Genet 1988;81:41–48
Mannens M, Devilee P, Bliek J, Mandjes I, de Kraker J, Heyting C, Slater RM, Westerveld A: Loss of heterozygosity in Wilms’ tumors, studied for six putative tumor-suppressor regions, is limited to chromosome 11. Cancer Research 1990;50:3279–3283
Scrable H, Cavenee W, Ghavimi F, Lovell M, Morgan K, Sapienza C: A model for embryonal rhabdomyosarcoma tumorigenesis that involves imprinting. Proc Natl Acad Sci USA 1989;86:7480–7484
Weksberg R, Glaves M, Teshima I, Waziri M, Patil S, Williams BRG: Molecular characterization of Beckwith-Wiedemann syndrome (BWS) patients with partial duplication of chromosome 11p excludes the gene MYOD1 from the BWS region. Genomics 1990;8:693–698
Mannens M, Slater RM, Heyting C, Geurts van Kessel A, Goedde-Salz E, Frants RR, Van Ommen GJB, Pearson PL: Regional localization of DNA probes on the short arm of chromosome 11 using aniridia-Wilms’ tumor-associated deletions. Hum Genet 1987;75:180–187
Junien C, van Heyningen V: Report of the committee on the genetic constitution of chromosome 11. Cytogenet Cell Genet 1990;55:153–169
Human Gene Mapping 10. 10th Int Workshop on Human Gene Mapping. Cytogenet Cell Genet 1989;51: (1–4).
Waye JS, Creeper LA, Willard HF: Organization and evolution of alpha satellite DNA from human chromosome 11. Chromosoma 1987;95:182–188
Higgins MJ, Wang H, Shtromas I, Haliotis T, Roder JC, Holden JJA, White BN: Organization of a repetitive human 1.8 kb KpnI sequence localized to the heterochromatin of chromosome 15. Chromosoma 1985;93:77–86
Harrison-Lavoie K, John R, Porteous D, Little PFR A cosmid clone map derived from a small region of human chromosome 11 Genomics 1989;5:501–509.
de Pagter-Holthuizen P, Jansen M, Schaik FMA van der Kammen R, Oosterwijk C, van der Brande JL, Sussenbach JS: The human insulinlike growth factor II gene contains two development-specific promoters. FEBS Lett 1987;214:259–264
Lewis WH, Yeger H, Bonetta L, Chan HSL, Kang J, Junien C, Cowell J, Jones C, Dafoe LA: Homozygous deletion of a DNA marker from chromosome 11p13 in sporadic Wilms’ tumor. Genomics 1988;3:25–31
Steenbergh PH, Höppener JWM, Zandberg J, van de Ven WJM, Jansz HS, Lips CJM: Structure of the human calcitonin gene and its transcripts in medullary thyroid carcinoma; in Pecile A (ed): Calcitonin. Amsterdam, Elsevier, 1985, pp 23–31.
Höppener JWM: The Human Calcitonin/CGRP Genes; thesis University of Utrecht, (1988).
Höppener JWM, Steenbergh PH, Zandberg J, Adema GJ, Geurts van Kessel AHM, Lips CJM, Jansz HS: A third human CALC (pseudo)gene on chromosome 11. FEBS Lett 1988;233:57–63
Tokino T, Takahashi E, Mori M, Tanigami A, Glaser T, Park JW, Jones C, Hori T, Nakamura Y: Isolation and mapping of 62 new RFLP markers on human chromosome 11. Am J Hum Genet 1991;48:258–268
Hoovers JMN, Mannens M, John R, Bliek J, van Heyningen V, Porteous DJ, Leschot NJ, Westerveld A, Little PFR: High resolution localization of 69 potential human zinc finger protein genes: A number are clustered. Genomics 1992;12:254–263
Wadey RB, Little PFR, Pritchard J, Cowell JK: Isolation and regional localization of DNA sequences from a human chromosome 11-specific cos-mid library. Hum Genet 1990:84: 417–423.
Lichter P, Tang CJC, Call K Hermanson G, Evans GA, Housman D, Ward DC: High-resolution mapping of human chromosome 11 by in situ hybridization with cosmid clones. Science 1990;247:64–69
Rønne M: Double synchronization of human lymphocyte cultures: selection for high-resolution banded metaphases in the first and second division. Cytogenet Cell Genet 1985;39:292–295
Lichter P, Cremer T, Borden L, Manuelidis L, Ward DC: Delineation of individual human chromosomes in metaphase and interphase cells by in situ suppression hybridization using recombinant DNA libraries. Hum Genet 1988,80:224–234.
Francke U: High-resolution ideograms of trypsin-Giemsa banded human chromosomes. Cytogenet Cell Genet 1981;31:24–32
Daniel A: The size of prometaphase chromosome segments. Tables using percentages of haploid autosome length (750 band stage). Clin Genet 1985;28:216–224
Barlow GB: Excretion of polyamines by children with Beck-with’s syndrome. Arch Dis Child 1980;55:40–42
Sutchffe JS, Nelson DL, Zhang F, Pieretti M, Caskey CT, Saxe D, Warren ST: DNA methylation represses FMR-1 transcription in fragile X syndrome. Hum Mol Genet 1992;397–400.
Driscoll DJ, Waters MF, Williams CA, Zori RT, Glenn CC, Avidano KM, Nicholls RD: A DNA methylation imprint, determined by the sex of the parent, distinguishes the Angelman and Prader-Willi syndromes. Genomics 1992, 13:917–924.
Ghazi H, Magewu AN, Gonzales F, Jones PA: Changes in the allelic methylation patterns of c-H-ras-1, insulin and retinoblastoma genes in human development. Development Suppl 1990:115–123.
Schneid H, Seurin D, Vazquez MP, Gourmelen M, Cabrol S, Le Bouc Y: Parental allele-specific methylation of the human insulin-like growth factor 2 gene and Beckwith-Wiedemann syndrome. J Med Genet 1993;30:353–362
Reik, W: Genomic imprinting and genetic disorders in man. Trends Genet 1989;5:331–336
Moore T, Haig D: Genomic imprinting in mammalian development: A parental tug of war. Trends Genet 1991;7:45–49
Forejt J, Gregorova S: Genetic analysis of genomic imprinting: An imprintor-1 gene controls inactivation of the paternal copy of the mouse Tme locus. Cell 1992;70:443–450
Ferguson-Smith AC, Cattanach BM, Barton SC, Beechey CV, Surani MA: Embryological and molecular investigations of parental imprinting on mouse chromosome 7. Nature 1991;351:667–670
Kitsberg D, Selig S, Brandeis M, Simon I, Keshet I, Driscoll DJ, Nicholls RD, Cedar H: Allele-specific replication timing of imprinted gene regions. Nature 1993;364:459–463
Dowdy SF, Fasching CL, Araujo D, Lai KM, Livanos E, Weissman BE, Stanbridge EJ: Suppression of tumorigenicity in Wilms tumor by the p15.5-p14 region of chromosome 11. Science 1991;254:293–295
Junien C: Beckwith-Wiedemann syndrome, tumorigenesis and imprinting. Current Opin Genet Dev 1992;2:431–438
Glaser T, Housman D, Lewis WH, Gerhard D, Jones C: A fine-structure deletion map of human chromosome 11p: Analysis of Jl series hybrids. Somat Cell Mol Genet 1989;15:477–501
Madden SL, Cook DM, Morris JF, Gashler A, Sukhatme VP, Rauscher FJ: Transcriptional repression mediated by the WT1 Wilms tumor gene product. Science 1991;253:1550–1553
Acknowledgements
We thank Drs. J.W. Scheres, M. Waziri, C.J. de Groot, A. Midro, H. v.d. Wiel, E.J. Breslau-Siderius, F.A. Beemer, D. Lindhout, B.G. Oppedael, P. Møller, F. Hedborg, A.J.M. Kuppeveit, C. Lundsteen, N. Harada, C. Brandt, and A. Geurts van Kessel for patient material; Drs. J.W.M. Höppener, B. Williams, R. Fodde, P. Holthuizen, P. Devilee, E. Rogler, V. Huff, B. Williams, and P.C Watkins for providing us with some of the probes; W.J. van Est and R. Lutgerhorst for photographic work; K. van der Lip, S.L. Bhola, G.J. Voogd, L. de Galan, R. v.d. Boogaard and M. v.d. Kroonenberg for technical assistance. We would like to express our gratitude to Mrs. P. Thoonen of the Dutch Organization for Parents of Beckwith-Wiedemann Syndrome Patients for her help.
This work has been supported by the Netherlands Cancer Foundation (Koningin Wilhelmina Fonds) grant No. IKA 89-30, the British Leukaemia Research Fund, the UK. Cancer Research Campaign, a special project grant from the Human Genome Mapping Project directed program of the MRC, and a clinical research grant No. 6.551 from the March of Dimes Birth Defects Foundation. The collaboration was facilitated by the commission of the European Communities grant No. SCI*0469-c(EDB), the EEC Concerted Action on Automated Cytogenetics, the Danish Cancer Society and the Danish Program for Human Genome Research.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Mannens, M., Hoovers, J.M.N., Redeker, E. et al. Parental Imprinting of Human Chromosome Region 11p15.3-pter Involved in the Beckwith-Wiedemann Syndrome and Various Human Neoplasia. Eur J Hum Genet 2, 3–23 (1994). https://doi.org/10.1159/000472337
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1159/000472337
Key Words
This article is cited by
-
Clinical and molecular diagnosis, screening and management of Beckwith–Wiedemann syndrome: an international consensus statement
Nature Reviews Endocrinology (2018)
-
Japanese and North American/European patients with Beckwith–Wiedemann syndrome have different frequencies of some epigenetic and genetic alterations
European Journal of Human Genetics (2007)
-
Wilms' tumour: connecting tumorigenesis and organ development in the kidney
Nature Reviews Cancer (2005)
-
DNA methylation, imprinting and cancer
European Journal of Human Genetics (2002)
-
Cloning of breakpoints in and downstream the IGF2 gene that are associated with overexpression of IGF2 transcripts in colorectal tumours
Oncogene (1999)